INTRODUCTION TO AMPUTATION SURGERY
Amputation should never be viewed as a failure of medical or surgical management, but rather as the first critical step in the functional rehabilitation of the patient. The overarching goal of amputation surgery is to remove diseased, ischemic, or severely traumatized tissue while constructing a dynamic, sensate, and pain-free residual limb capable of interfacing seamlessly with a modern prosthesis. Achieving this requires a profound understanding of biomechanics, soft-tissue envelope management, and the physiological demands of prosthetic ambulation.
PREOPERATIVE OPTIMIZATION AND LEVEL DETERMINATION
Determining the appropriate level of amputation requires a nuanced understanding of the tradeoffs between increased functional capacity (associated with a more distal amputation) and a decreased complication and reoperation rate (associated with a more proximal amputation). The patient’s overall physiological reserve, general medical condition, and rehabilitation potential are paramount.
Multidisciplinary Assessment
A vascular surgery consultation is almost universally indicated in dysvascular patients. Even if complete limb salvage is impossible, targeted revascularization may allow for the healing of a partial foot or Syme amputation rather than defaulting to a transtibial (below-knee) amputation. However, surgeons must remain cognizant that peripheral bypass surgery utilizing local tissues or altering hemodynamics may occasionally compromise the wound healing of a future transtibial amputation if the bypass fails.
Nutritional and Immunological Optimization
Medical illness, systemic infection, and major surgical trauma induce a profound hypermetabolic state. Multiple studies have confirmed that malnourished or immunocompromised patients face markedly increased rates of perioperative complications, including wound dehiscence and deep infection.
Clinical Pearl: Simple screening tests for nutritional status are mandatory. Dickhaut et al. demonstrated an 86% healing rate for Syme amputations in patients with a serum albumin level ≥ 3.5 g/dL and a total lymphocyte count (TLC) ≥ 1500 cells/mL. Conversely, only 18% of patients with abnormalities in either parameter achieved successful healing.
Kay et al. further corroborated this, showing that amputations healed uneventfully in 94% of patients with normal nutritional parameters, whereas 44% of malnourished patients suffered severe postoperative complications. The adverse effects of malnutrition are most pronounced in distal amputations; thus, proximal amputations may be considered if nutritional optimization is impossible.
Biomechanics and the Energy Cost of Walking
The preservation of joints, particularly the knee, drastically reduces the energy expenditure required for ambulation. Waters et al. extensively studied the energy cost of walking for amputees. Compared to non-amputee controls, the self-selected walking velocity for dysvascular amputees was:
* Syme level: 66% of normal
* Transtibial level: 59% of normal
* Transfemoral level: 44% of normal
For traumatic amputees (who are generally younger and lack systemic vascular disease), velocities were 87% at the transtibial level and 63% at the transfemoral level.
Amputees naturally decrease their walking velocity as a compensatory mechanism to keep their relative energy costs per minute within normal physiological limits. However, patients with transfemoral amputations secondary to vascular insufficiency are often unable to accomplish this, frequently exceeding 50% of their maximum aerobic capacity even during minimal household ambulation. At this threshold, anaerobic metabolism is triggered, leading to rapid fatigue. Consequently, very few dysvascular transfemoral amputees ever regain functional, community-level ambulatory ability.
Ambulatory vs. Non-Ambulatory Considerations
If ambulation is the primary goal, the amputation must be performed at the most distal level capable of healing. Conversely, if a patient has zero ambulatory potential (e.g., severe dementia, advanced heart failure, bilateral dense hemiplegia), wound healing and the minimization of perioperative morbidity become the chief concerns.
Surgical Warning: A transtibial amputation in a bedbound, non-ambulatory patient is often contraindicated due to the high risk of posterior heel ulceration, wound breakdown, and the inevitable development of severe knee flexion contractures.
For non-ambulators, a knee disarticulation often provides superior outcomes. Compared to a transfemoral amputation, knee disarticulation offers:
1. A longer lever arm with balanced musculature, aiding in bed mobility and wheelchair transfers.
2. Preservation of muscle insertions, preventing the severe atrophy and soft-tissue retraction seen over the transected femur.
3. A broad, end-bearing surface that provides superior sitting stability and comfort.
Objective Assessment of Healing Potential
Determining the most distal level with a reasonable probability of healing is challenging. Clinical assessment of skin color, hair growth, capillary refill, and skin temperature provides valuable baseline data but lacks predictive precision.
- Arteriography: While essential for vascular bypass planning, angiograms offer little predictive value for capillary-level wound healing.
- Ankle-Brachial Indices (ABIs): Segmental systolic blood pressures are frequently falsely elevated (often >1.2) due to medial calcinosis (Mönckeberg's sclerosis) in diabetic and end-stage renal disease patients.
- Transcutaneous Oximetry (TcPO2): This is the gold standard for predicting amputation healing.
TcPO2 Protocol: A probe heated to 45ºC is applied to the skin for 10 minutes to induce maximal local vasodilation, providing an accurate assessment of perfusion reserve.
* A TcPO2 > 40 mm Hg indicates excellent healing potential.
* A TcPO2 < 20 mm Hg indicates a high likelihood of failure.
* The 100% Oxygen Challenge: In the 20–40 mm Hg "gray zone," the patient inhales 100% oxygen. An increase of >10 mm Hg at the target level strongly predicts successful healing.
* The Elevation Test: A decrease of >15 mm Hg after 3 minutes of limb elevation is a poor prognostic indicator.
SURGICAL TECHNIQUE AND PRINCIPLES
Meticulous attention to detail and atraumatic handling of soft tissues are non-negotiable. The tissues in dysvascular limbs are already operating at the absolute limits of their perfusion; iatrogenic trauma will precipitate necrosis.
Hemostasis and Tourniquet Management
Except in severely ischemic limbs, the use of a pneumatic tourniquet is highly desirable to minimize blood loss and improve visualization.
* Standard Application: The limb is exsanguinated using an Esmarch bandage prior to tourniquet inflation.
* Infection or Malignancy: Exsanguination via Esmarch is strictly contraindicated to prevent the systemic seeding of bacteria or tumor cells. Instead, the limb should be elevated at 60 degrees for 5 minutes prior to inflation.
Major blood vessels must be isolated and individually ligated with non-absorbable sutures. Large arteries (e.g., superficial femoral, popliteal) should be doubly ligated or suture-ligated. The tourniquet must be deflated prior to final closure to ensure meticulous hemostasis. A closed-suction drain is recommended for 48 to 72 hours to prevent hematoma formation, which acts as a nidus for infection and increases tension on the suture line.
Skin and Muscle Flaps
Flaps must be kept thick, incorporating skin, subcutaneous fat, and deep fascia as a single, full-thickness unit. Delamination or unnecessary dissection between tissue planes destroys the fragile perforating vessels, leading to marginal necrosis.
The ultimate goal is to cover the distal bone with a robust, mobile soft-tissue envelope. While classic flap designs (e.g., the long posterior flap for transtibial amputations) are standard, atypical flaps are always preferable to sacrificing joint levels. Modern total-contact prosthetic sockets can accommodate scars in almost any location, provided the scar is not adherent to the underlying bone. Adherent scars shear during prosthetic use, leading to chronic ulceration. Redundant soft tissues or large "dog ears" must be excised, as they create pressure points within the prosthetic socket.
Muscle Stabilization: Myodesis vs. Myoplasty
Muscles are typically divided 5 cm distal to the intended level of bone resection to allow for adequate coverage. Unanchored muscles retract, atrophy, and fail to provide a dynamic cushion. Jaegers et al. demonstrated that transected, unfixed muscles atrophy by 40% to 60% within two years.
- Myoplasty: Suturing the fascia of opposing muscles together over the bone end (e.g., anterior compartment fascia to deep posterior compartment fascia).
- Myodesis: Suturing the muscle or tendon directly to the bone via drill holes.
Whenever possible, myodesis is the preferred technique. It provides a rigid insertion point, maximizes residual limb strength, minimizes atrophy, and maintains the physiological resting length of the muscle. This counterbalances antagonist muscles, preventing joint contractures.
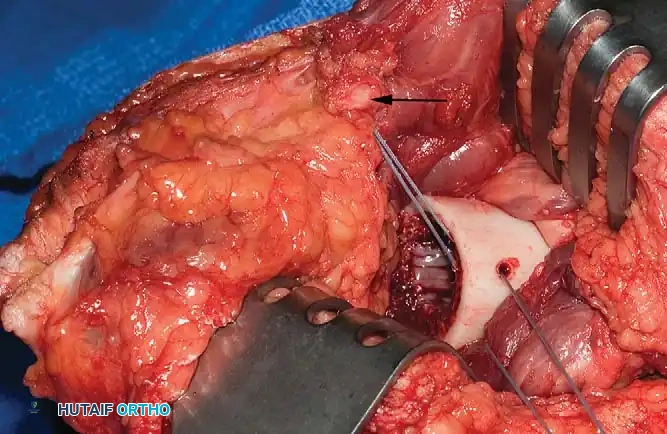
Clinical Pearl: In a transfemoral amputation, myodesis of the adductor magnus to the lateral distal femur is critical. Loss of the adductor insertion leads to an overpowering of the abductors, resulting in a severe abduction contracture. This creates a mechanically inefficient, wide-based Trendelenburg gait.
Note: Myodesis may be contraindicated in cases of severe ischemia, as the tension placed on the muscle can strangulate its remaining blood supply, leading to deep tissue necrosis.
Nerve Management
A neuroma is the inevitable physiological result of nerve transection. The surgical goal is not to prevent a neuroma, but to ensure it forms in a deep, well-cushioned soft-tissue bed, away from the incision line, bony prominences, and areas of prosthetic contact.
Despite historical attempts at perineural closure, Silastic capping, or chemical cauterization, the most reliable method remains traction neurectomy.
1. The nerve is isolated and gently drawn distally into the wound.
2. It is divided cleanly with a sharp scalpel (never electrocautery or scissors, which crush the fascicles).
3. The nerve is allowed to retract deep into the proximal soft tissues.
Surgical Warning: Avoid excessive tension when pulling the nerve distally. Over-stretching can cause proximal axonal tearing, leading to a severe, intractable neuropathic pain syndrome that persists even after the wound heals.
Large nerves, particularly the sciatic nerve, contain substantial intrinsic arteries (the vasa nervorum or the companion artery of the sciatic nerve) and must be formally ligated to prevent postoperative hematoma.
Bone Preparation
Excessive periosteal stripping is strictly contraindicated. Stripping devascularizes the distal cortex, leading to the formation of ring sequestra or painful bony overgrowth (spurs).
Bony prominences that will not be adequately padded by soft tissue must be resected and meticulously rasped to a smooth contour. Critical areas requiring beveling include:
* The anterior cortex of the distal tibia.
* The lateral aspect of the distal femur.
* The radial styloid in wrist disarticulations.
OPEN AMPUTATIONS AND CONTAMINATED WOUNDS
An open amputation is indicated in the presence of fulminant infection (e.g., wet gangrene, necrotizing fasciitis) or severe traumatic wounds with extensive tissue destruction and gross contamination. The primary objective is source control and the elimination of infection.
An open amputation is never a definitive procedure; it is the first stage of a reconstructive process requiring secondary closure, formal revision, or plastic repair.
Vacuum-Assisted Closure (NPWT)
While historical techniques relied on inverted skin flaps or circular open amputations with postoperative skin traction, modern management heavily utilizes Negative Pressure Wound Therapy (NPWT/VAC).
Following the initial radical debridement, a wound VAC is applied directly to the open stump. This provides continuous drainage, reduces interstitial edema, promotes robust granulation tissue formation, and physically retracts the soft tissues distally, preventing skin retraction. Subsequent serial debridements are scheduled at 48- to 72-hour intervals until the bioburden is cleared and the wound bed is optimized for delayed primary closure.
POSTOPERATIVE CARE AND REHABILITATION
The postoperative management of an amputee requires a highly coordinated multidisciplinary team, including the orthopedic surgeon, physiatrist, prosthetist, physical therapist, occupational therapist, and medical internist.
Pain Management
Effective perioperative pain control is critical to prevent the centralization of pain and the development of chronic phantom limb pain. Management typically begins with a brief course of intravenous narcotics, rapidly transitioned to multimodal oral analgesia (gabapentinoids, acetaminophen, NSAIDs).
Recent advancements emphasize the use of continuous postoperative perineural infusional anesthesia. Placing an indwelling catheter adjacent to the major nerve trunks (e.g., sciatic or femoral nerve) for 3 to 5 days significantly decreases opioid consumption, blunts the acute neuropathic pain response, and facilitates earlier participation in physical therapy.
Stump Dressings and Edema Control
The treatment of the residual limb from the moment of closure until definitive prosthetic fitting dictates the ultimate functional outcome. Since the 1970s, the standard of care in high-volume amputation centers has shifted from conventional soft dressings to rigid dressings.
The Rigid Dressing (Plaster of Paris Cast):
Applied immediately in the operating room, the rigid dressing offers profound advantages:
1. Edema Control: It physically prevents postoperative swelling, accelerating wound healing.
2. Trauma Protection: It shields the fragile surgical site from inadvertent bed trauma.
3. Contracture Prevention: For transtibial amputations, a cast extending above the knee physically prevents the development of knee flexion contractures, which can otherwise render a patient un-fittable for a prosthesis.
4. Pain Reduction: By immobilizing the soft tissues and preventing shear across the incision, rigid dressings significantly reduce postoperative pain.
Immediate Postoperative Prosthesis (IPOP):
If early weight-bearing is deemed safe and appropriate, a certified prosthetist may apply a specialized rigid cast incorporating stump socks, contoured felt padding over bony prominences, and a distal attachment plate. A metal pylon and prosthetic foot are attached, allowing for immediate, protected touch-down weight-bearing.
