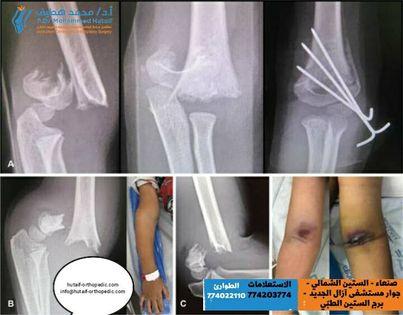
Supracondylar Humerus Fracture: When to Open & How to Treat
Introduction & Epidemiology
Supracondylar humerus fractures (SCHF) are the most common elbow fractures in the pediatric population, accounting for approximately 60% of all elbow fractures and 3% of all pediatric fractures. They typically occur in children between 5 and 8 years of age, often following a fall onto an outstretched hand (FOOSH) with the elbow in hyperextension, resulting in an extension-type fracture (approximately 95-98%). Flexion-type fractures, caused by a direct blow to the posterior aspect of the flexed elbow, are rare (2-5%).
The Gartland classification system (modified) remains the most widely accepted method for categorizing SCHF based on radiographic appearance and displacement:
*
Type I:
Nondisplaced or minimally displaced. The anterior humeral line (AHL) intersects the capitellum.
*
Type II:
Displaced posteriorly with an intact posterior cortex, but with angulation such that the AHL no longer intersects the capitellum. These may be further subdivided into Type IIA (posterior angulation only) and Type IIB (posterior angulation with rotation and/or medial/lateral displacement).
*
Type III:
Completely displaced, with no cortical contact between the proximal and distal fragments. These are highly unstable and carry the greatest risk of neurovascular injury.
*
Type IV (recently added):
Multidirectionally unstable after reduction, characterized by instability in both flexion and extension, often due to significant periosteal tearing around the fracture site.
The critical nature of SCHF stems from the close proximity of the brachial artery and median nerve to the fracture site, as well as the potential for iatrogenic ulnar nerve injury during medial pin placement. Inadequate reduction or fixation can lead to malunion (most commonly cubitus varus) and functional impairment. While closed reduction and percutaneous pinning (CRPP) is the gold standard for displaced fractures, understanding the indications and techniques for open reduction is paramount for optimal outcomes in complex presentations.
Surgical Anatomy & Biomechanics
A thorough understanding of the distal humeral anatomy and surrounding neurovascular structures is critical for safe and effective management of SCHF.
Distal Humerus Anatomy
The distal humerus forms a Y-shaped structure, composed of medial and lateral columns that support the articular surface.
*
Columns:
The medial column includes the medial epicondyle and trochlea. The lateral column includes the lateral epicondyle and capitellum. The supracondylar region is the narrowest part of the bone, rendering it susceptible to fracture.
*
Fossae:
Anteriorly, the coronoid fossa (superior to the trochlea) accommodates the coronoid process during flexion, and the radial fossa (superior to the capitellum) accommodates the radial head. Posteriorly, the olecranon fossa (superior to the trochlea) accommodates the olecranon during extension.
*
Baumann's Angle:
Formed by a line drawn along the lateral epicondylar physis and a line along the shaft of the humerus. This angle (normally 64-81 degrees) is a key radiographic indicator of valgus/varus alignment.
*
Anterior Humeral Line (AHL):
A line drawn along the anterior cortex of the humerus should pass through the middle third of the capitellum on a true lateral radiograph. Displacement or rotation of the distal fragment will alter this relationship.
Neurovascular Bundles
The major neurovascular structures course anterior and medial to the distal humerus, making them highly vulnerable in displaced SCHF.
*
Brachial Artery:
Lies anterior and slightly medial to the humerus, typically bifurcating into the radial and ulnar arteries just distal to the elbow joint. It is tethered proximally by the ligament of Struthers (when present) and distally by the bicipital aponeurosis and recurrent radial artery branches, making it susceptible to stretch, spasm, or laceration with significant displacement.
*
Median Nerve:
Runs in close association with the brachial artery, typically immediately medial to it. It is the most commonly injured nerve in extension-type SCHF.
*
Ulnar Nerve:
Courses posterior to the medial epicondyle in the cubital tunnel. It is particularly vulnerable to iatrogenic injury during medial pin placement in crossed-pin fixation techniques or during surgical approaches to the medial column.
*
Radial Nerve:
Located more laterally and posteriorly, winding around the humerus in the spiral groove. It is less commonly affected by SCHF itself but can be at risk during lateral surgical approaches or with extensive lateral soft tissue injury.
*
Anterior Interosseous Nerve (AIN):
A purely motor branch of the median nerve, innervating the flexor pollicis longus, pronator quadratus, and the radial half of the flexor digitorum profundus. AIN palsy presents with inability to make an "OK" sign (loss of IP joint flexion of thumb and DIP joint flexion of index finger) and can occur with SCHF.
Biomechanics of Injury
- Extension-Type (Hyperextension): The most common type. A FOOSH injury forces the elbow into hyperextension, driving the olecranon into the olecranon fossa, creating a fulcrum. The distal humerus fails in tension anteriorly and compression posteriorly. The periosteum on the posterior aspect often remains intact, forming a hinge, which can aid in closed reduction.
- Flexion-Type: Occurs with a direct impact on the posterior elbow while it is in flexion. The distal fragment displaces anteriorly. The anterior periosteum may remain intact. These are often more unstable and difficult to reduce closed.
- Rotational Malalignment: Often accompanies posterior displacement in Type IIB and III fractures. Failure to correct rotational malalignment is a common cause of failed reduction and can lead to cosmetic deformity (cubitus varus) despite apparently good AP/lateral alignment.
Indications & Contraindications
The management of supracondylar humerus fractures primarily revolves around achieving and maintaining an anatomical or near-anatomical reduction to prevent malunion, particularly cubitus varus, and to minimize neurovascular complications.
Non-Operative Indications
- Gartland Type I: Nondisplaced or minimally displaced fractures. These are managed with a long arm cast or splint, typically in 90 degrees of flexion with the forearm in pronation, for 3-4 weeks. Close follow-up with radiographs is crucial to monitor for secondary displacement.
Operative Indications (Closed Reduction and Percutaneous Pinning - CRPP)
- Gartland Type II (Displaced): Significant posterior angulation, AHL does not intersect the capitellum. These often require reduction to restore proper alignment and avoid malunion.
- Gartland Type III: Complete displacement, no cortical contact. These are inherently unstable and require surgical stabilization.
- Gartland Type IV: Multidirectionally unstable fractures that cannot be held in reduction. While often initially attempted with closed reduction, the inherent instability frequently necessitates percutaneous pinning.
Operative Indications (Open Reduction)
Open reduction is reserved for specific scenarios where closed reduction and percutaneous pinning are not feasible or fail to achieve optimal outcomes. These indications directly address the core question of "When to Open":
*
Failed Closed Reduction:
After two to three attempts by an experienced surgeon, if acceptable reduction cannot be achieved or maintained. This is the most common indication for open reduction. Causes include irreducible periosteal interposition, soft tissue interposition (e.g., brachialis muscle, median nerve, brachial artery), buttonholing of the olecranon through the brachialis, or severe comminution preventing stable reduction.
*
Open Fracture:
Any Gustilo-Anderson classification open fracture requires debridement and often open reduction with internal fixation to prevent infection and facilitate soft tissue management.
*
Associated Neurovascular Injury Requiring Direct Exploration:
*
"White, Pulseless Hand" (Ischemic Hand):
This is a limb-threatening emergency. After a single gentle attempt at closed reduction (which may restore perfusion), if the hand remains white, cold, and pulseless, immediate surgical exploration of the brachial artery via an anterior approach is indicated, irrespective of the fracture reduction quality. Vascular repair (often with vein graft interposition) takes precedence.
*
Expanding Hematoma:
Suggests active arterial bleeding and necessitates exploration.
*
Neurological Deficit with Compromised Perfusion:
If a pre-existing neurological deficit (especially median nerve or AIN) is accompanied by poor perfusion, direct exploration may be warranted to assess for nerve entrapment or direct injury if vascular compromise also requires intervention.
*
Severe Skin Compromise:
Impending open fracture, skin puckering (indicates distal fragment has buttonholed through muscle and skin), or skin blanching/tenting that cannot be relieved by reduction and may lead to necrosis.
*
Compartment Syndrome:
Clinical signs of acute compartment syndrome necessitate emergent fasciotomy, which often accompanies open reduction of the fracture.
*
Flexion-Type Fractures:
These are sometimes more difficult to reduce closed due to different deforming forces and periosteal hinge. Open reduction may be considered if closed attempts fail.
*
Type IV Fractures with Persistent Instability:
While often initially attempted closed, if the multidirectional instability precludes stable pinning, direct visualization may be required to clear intervening soft tissues and achieve a stable construct.
Contraindications for Open Reduction
There are no absolute contraindications to open reduction for SCHF when indicated to prevent severe complications or achieve reduction. Relative contraindications relate more to the patient's overall health (e.g., severe comorbidities precluding anesthesia) or to selecting the least invasive method possible. The goal is always to minimize iatrogenic harm while achieving the best functional outcome.
Table: Operative vs. Non-Operative Indications for Supracondylar Humerus Fractures
| Treatment Modality | Indications | Non-Operative | Gartland Type I (non-displaced or minimally displaced). | | |
|
Non-Operative (Observation)
| Type I fracture (non-displaced or minimally displaced, AHL intersects capitellum). Stable. | |
|
CRPP (Closed Reduction, Pinning)
| Type IIB (displaced with rotation/displacement), Type III, Type IV (sometimes difficult to reduce fully, requires stable pinning). Also used for Type II fractures with significant angulation/displacement. | | | | | | | | | | | | | | |