Introduction & Epidemiology
Rheumatoid arthritis (RA) is a chronic, systemic inflammatory autoimmune disease predominantly affecting synovial joints, leading to progressive destruction, deformity, and functional impairment. The elbow joint, a diarthrodial hinge joint, is involved in approximately 20-50% of RA patients, often bilaterally and symmetrically. While less frequently affected than the hands, wrists, or feet, advanced RA in the elbow can be profoundly debilitating, severely limiting activities of daily living (ADLs) and impacting overall quality of life.
The pathological cascade in RA begins with synovial inflammation (synovitis), characterized by pannus formation, which invades and erodes articular cartilage and subchondral bone. This process, driven by inflammatory cytokines and proteases, leads to joint space narrowing, subchondral cysts, marginal erosions, and ultimately, osteolysis and capsular laxity. The typical presentation includes pain, swelling, stiffness, and progressive loss of motion, frequently progressing to fixed flexion deformities, valgus instability (due to radial head erosion and lateral collateral ligament attenuation), or less commonly, varus deformity. The ulnar nerve is particularly vulnerable to compression or traction neuropathy due to cubital tunnel involvement, tenosynovitis, or valgus deformity.
Despite significant advancements in medical management, including disease-modifying antirheumatic drugs (DMARDs) and biologic agents, a subset of patients will invariably develop end-stage joint destruction requiring surgical intervention. The goal of surgical management is consistently pain relief, restoration of functional motion, stability, and correction of deformity.
Surgical Anatomy & Biomechanics
A thorough understanding of the intricate anatomy and biomechanics of the elbow is paramount for effective surgical planning and execution in RA. The elbow comprises three distinct articulations within a single capsule:
*
Ulnohumeral joint:
A true hinge joint between the trochlea of the humerus and the trochlear notch of the ulna, primarily responsible for flexion and extension. Its bony congruity provides significant stability.
*
Radiohumeral joint:
A gliding joint between the capitellum of the humerus and the radial head, contributing to flexion/extension and forearm rotation.
*
Proximal radioulnar joint (PRUJ):
A pivot joint between the radial head and the radial notch of the ulna, critical for pronation and supination. The annular ligament encircles the radial head, maintaining its position within the radial notch.
Ligamentous Stabilizers
The primary static stabilizers of the elbow are the medial collateral ligament (MCL) complex and the lateral collateral ligament (LCL) complex.
*
MCL:
Consists of anterior, posterior, and transverse bundles. The anterior bundle is the primary restraint to valgus stress throughout the range of motion.
*
LCL:
Consists of the radial collateral ligament (RCL), lateral ulnar collateral ligament (LUCL), and annular ligament. The LUCL is particularly critical for posterolateral rotatory stability, preventing subluxation of the ulna and radius from the humerus. In RA, chronic synovitis often leads to attenuation and eventual rupture of these ligaments, contributing to instability and progressive deformity.
Musculature
The elbow is surrounded by powerful muscle groups facilitating motion:
*
Flexors:
Biceps brachii, brachialis, brachioradialis.
*
Extensors:
Triceps brachii (medial, lateral, and long heads). The triceps tendon inserts on the olecranon and is often weakened or attenuated in advanced RA, especially following surgical approaches that necessitate triceps management.
*
Forearm rotators:
Supinator, biceps (supination); pronator teres, pronator quadratus (pronation).
Neurovascular Structures
Critical neurovascular structures are in close proximity to the elbow joint and are at risk during surgical dissection:
*
Ulnar nerve:
Posterior to the medial epicondyle, within the cubital tunnel. Highly susceptible to compression, traction, or iatrogenic injury, particularly with valgus deformities or during posterior surgical approaches.
*
Median nerve:
Anterior to the elbow, medial to the brachial artery, typically protected by the pronator teres.
*
Radial nerve:
Divides into superficial (sensory) and deep (motor, posterior interosseous nerve) branches anterior to the lateral epicondyle, deep to the brachioradialis and supinator.
*
Brachial artery:
Anterior to the elbow, typically medial to the biceps tendon.
In RA, the synovial hypertrophy and effusion can directly impinge on nerves. Furthermore, bony erosions and progressive deformity can alter normal anatomical relationships, making surgical dissection more challenging. The radial head is frequently involved, leading to erosions and osteolysis, often resulting in radial head subluxation or dislocation and contributing to valgus instability. The olecranon and coronoid fossae can also undergo significant erosion, leading to bone loss.
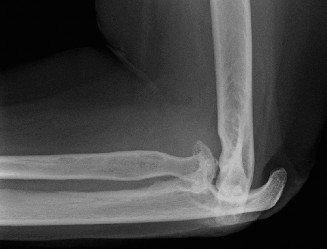
Indications & Contraindications
The decision-making process for surgical intervention in the RA elbow is multifaceted, considering disease activity, systemic comorbidities, functional deficit, pain severity, and patient expectations. Non-operative management, including optimizing DMARDs and biologics, physical therapy, and judicious use of corticosteroid injections, remains the first-line treatment. Surgical options range from arthroscopic or open synovectomy to total elbow arthroplasty (TEA) or, in rare cases, arthrodesis.
Operative Indications
Surgical intervention is generally considered when non-operative measures have failed to adequately address pain, improve function, or halt disease progression.
- Persistent severe pain: Unresponsive to medical management, significantly impacting quality of life.
- Progressive joint destruction and deformity: Evidenced by radiographs showing significant joint space narrowing, erosions, osteolysis, subluxation, or dislocation. This includes fixed flexion deformities >30-45 degrees, severe valgus/varus instability, or ankylosis.
- Loss of functional range of motion: Impairing activities of daily living, such as feeding, dressing, or perineal care. A functional arc of motion for the elbow is generally considered to be 30-130 degrees of flexion/extension and 50 degrees of pronation/supination.
- Mechanical symptoms: Locking, catching, or palpable crepitus, often due to loose bodies or severe cartilage loss.
- Neurological compromise: Ulnar nerve compression neuropathy unresponsive to conservative management.
- Failed previous surgery: Such as failed synovectomy or excision arthroplasty, leading to persistent symptoms.
Contraindications
Absolute contraindications are few but critical, whereas relative contraindications require careful risk-benefit analysis.
-
Absolute Contraindications:
- Active infection (local or systemic): Must be aggressively treated and resolved prior to elective surgery.
- Inadequate bone stock: For implant fixation, particularly for TEA.
- Neuropathic joint (Charcot arthropathy): Poor outcomes with arthroplasty.
- Non-compliance: With post-operative rehabilitation protocols.
-
Relative Contraindications:
- Extensor mechanism insufficiency: Severe triceps weakness or rupture, potentially compromising rehabilitation outcomes and increasing implant loosening risk.
- Extremely poor skin quality: Due to chronic steroid use or previous surgeries, increasing wound complication risk.
- Significant systemic comorbidities: Uncontrolled diabetes, severe cardiovascular disease, renal failure, or pulmonary disease, increasing anesthetic and surgical risks.
- Young, high-demand patient: Though rare in advanced RA, younger patients with high physical demands may have higher rates of implant loosening or failure, requiring careful consideration of alternative salvage procedures.
- Psychiatric illness: Affecting patient cooperation with post-operative care.
Summary of Operative vs. Non-Operative Indications
| Indication Type | Non-Operative Management | Operative Management |
|---|---|---|
| Pain | Mild-to-moderate, responsive to analgesics/DMARDs | Severe, persistent, debilitating; refractory to medical therapy |
| Joint Status | Early synovitis without significant cartilage/bone erosion | Progressive joint space narrowing, erosions, osteolysis, subluxation |
| Deformity | Minimal or non-progressive; functional arc of motion maintained | Fixed flexion deformity (>30-45°), severe instability, ankylosis |
| Function | ADLs largely preserved; minimal functional limitation | Significant impairment of ADLs; functional arc lost |
| Neuropathy | Mild, intermittent ulnar nerve symptoms; responsive to rest/bracing | Persistent ulnar nerve compression/traction; progressive neurological deficit |
| Comorbidities | Significant systemic illness; poor surgical candidate | Medically optimized; reasonable surgical risk |
| Patient Factors | Low functional demand; preference for conservative approach | High functional demand (relative); desire for pain relief/function |
| Failure of prior | N/A | Failed synovectomy or excision arthroplasty |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is crucial for optimizing outcomes in RA elbow surgery. This involves a comprehensive patient assessment, appropriate imaging, and detailed surgical strategy.
Patient Assessment
- History: Detail pain characteristics (severity, aggravating/alleviating factors), functional limitations, previous medical and surgical treatments for RA, current medications (especially immunosuppressants, biologics, corticosteroids), and any history of infection.
- Physical Examination: Assess range of motion (active and passive), stability (valgus/varus, anteroposterior), triceps strength, presence of neurological deficits (especially ulnar nerve), skin quality, and overall limb alignment. Evaluate for other involved joints that may impact post-operative rehabilitation or compensatory movements.
- Laboratory Investigations: Complete blood count, electrolytes, renal and liver function tests, coagulation profile. Inflammatory markers (ESR, CRP) can provide insight into disease activity. Pre-operative screening for infection is paramount, especially if the patient is on immunosuppressants.
Imaging
-
Plain Radiographs:
Anteroposterior (AP) and lateral views are essential. Obtain views of the entire humerus and forearm to assess overall alignment, bone stock, and presence of previous hardware. Look for characteristic RA changes: joint space narrowing, erosions (particularly radial head, capitellum, olecranon, trochlear notch), subchondral cysts, osteopenia, and subluxation/dislocation. Stress views may reveal instability.
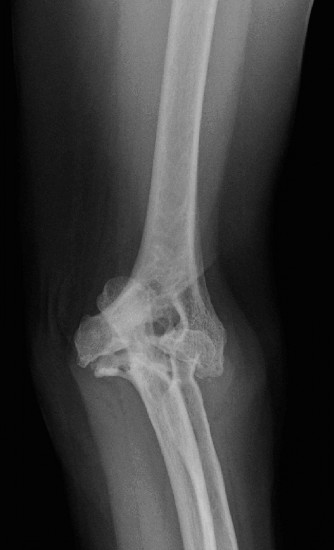
- Computed Tomography (CT) Scan: Highly recommended, especially for advanced cases involving significant bone loss, complex deformities, or revision surgery. CT provides detailed information on bone stock, joint congruity, and the extent of erosions, aiding in templating for implant size and position.
- Magnetic Resonance Imaging (MRI): Useful for assessing soft tissue involvement (synovitis, pannus, ligamentous integrity, nerve compression) if the surgical plan includes soft tissue procedures or nerve decompression. Not typically required for routine TEA.
Templating
Pre-operative templating using radiographs and CT scans is essential for Total Elbow Arthroplasty (TEA). Determine the appropriate implant size (humeral and ulnar components), assess the need for augments or bone grafting to address bone loss, and anticipate potential challenges with fixation.
Patient Positioning
For most elbow procedures in RA, particularly total elbow arthroplasty, the
lateral decubitus position
is preferred.
* The patient is positioned on their unaffected side with appropriate padding.
* The operative arm is draped free over a bolster or arm holder, allowing full access to the posterior aspect of the elbow and unimpeded flexion/extension.
* Ensure the shoulder is abducted and externally rotated to avoid brachial plexus traction.
* The head and neck are neutral to avoid iatrogenic neurological injury.
* Careful padding of bony prominences (e.g., fibular head of the contralateral leg, iliac crest) is crucial.
* A tourniquet is applied to the upper arm.
Alternatively, the prone position can be used, particularly for bilateral cases or if shoulder issues prevent lateral decubitus. However, it can make ulnar nerve management more challenging. The supine position with an arm board is generally reserved for anterior or medial approaches (e.g., ulnar nerve decompression or MCL repair), which are less common for advanced RA elbow reconstruction.
Detailed Surgical Approach / Technique
The choice of surgical technique depends on the extent of RA pathology and the specific goals. For advanced RA with significant joint destruction, Total Elbow Arthroplasty (TEA) is the gold standard.
Total Elbow Arthroplasty (TEA) - Posterior Approach
The posterior approach offers excellent exposure to both the ulnohumeral and radiohumeral joints and allows for management of the ulnar nerve.
1. Incision and Initial Dissection
- A posterior midline skin incision is made, centered over the olecranon, extending proximally about 8-10 cm over the distal humerus and distally 5-7 cm over the proximal ulna.
- Dissect through the subcutaneous tissue to expose the triceps tendon and fascia.
-
Ulnar Nerve Identification and Transposition:
Crucially, the ulnar nerve must be identified and protected. It is typically found posterior to the medial epicondyle. Carefully dissect it free from its cubital tunnel retinaculum, tracing it proximally and distally. The nerve is usually transposed anteriorly, submuscularly, beneath the flexor-pronator mass to prevent post-operative impingement or injury, especially given the common valgus deformity in RA.
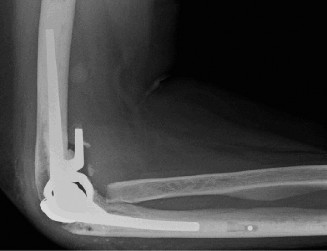
2. Triceps Management
Several techniques exist for gaining access to the joint through the triceps:
*
Triceps-splitting approach (Bryan-Morrey modification):
A longitudinal incision is made through the triceps tendon, starting proximally at the intramuscular septum and extending distally to the olecranon. This preserves the triceps insertion on the ulna.
*
Triceps-sparing approach:
A medial or lateral paratricipital incision. This can limit exposure, especially for complex cases.
*
Triceps-reflecting approach (e.g., Campbell):
The triceps is elevated subperiosteally from the olecranon and reflected proximally. This offers excellent exposure but can risk triceps avulsion post-operatively.
*
Olecranon osteotomy:
A chevron or transverse osteotomy of the olecranon provides the widest exposure, particularly useful in revision surgery or cases with severe bone loss. The osteotomy is typically fixed with tension band wiring or plates post-implantation. This method offers excellent exposure but has additional risks of non-union or hardware prominence.
*
For RA, due to potentially fragile bone and concerns about triceps integrity, an olecranon osteotomy might be favored by some surgeons for primary TEA in cases of severe deformity or limited exposure, provided the bone stock allows stable fixation.
3. Joint Exposure and Synovectomy
- Once the triceps is managed, incise the posterior capsule to expose the elbow joint.
- Perform a thorough synovectomy, removing all hypertrophied synovium and pannus from the olecranon fossa, coronoid fossa, radial head, and around the collateral ligaments. This reduces inflammatory burden and improves visualization.
- Excise the radial head if severely involved and interfering with implant placement or rotation.
4. Humeral Preparation
- Identify the intramedullary canal of the distal humerus.
- Use sequential reamers and broaches to prepare the humeral canal to accept the chosen humeral component. Ensure appropriate anteversion/retroversion.
- Address any significant bone loss in the distal humerus with bone graft (allograft or autograft) or custom augments, especially if using a non-constrained implant.
- For linked prostheses, the humerus is typically reamed to accept a specific stem length and size. For unlinked prostheses, the humeral component is a smaller capitellar or resurfacing component.
5. Ulnar Preparation
- Identify the intramedullary canal of the ulna.
- Use sequential reamers and broaches to prepare the ulnar canal for the ulnar component. Ensure alignment with the long axis of the ulna.
- The olecranon tip is often removed or trimmed to improve exposure and allow for implant seating.
- Similarly, address any bone loss in the proximal ulna with grafting or augments.
6. Implant Insertion
-
Linked vs. Unlinked Prostheses:
- Linked (constrained) prostheses: The humeral and ulnar components are mechanically connected, providing inherent stability. These are generally favored for RA due to significant ligamentous laxity, bone loss, and the need for immediate stability. They allow for controlled flexion/extension but limit varus/valgus motion.
- Unlinked (anatomic or resurfacing) prostheses: Relies on intact collateral ligaments for stability. These are rarely used in advanced RA due to the high incidence of ligamentous attenuation and bone loss, leading to high rates of instability.
- Apply bone cement (polymethylmethacrylate) to both the humeral and ulnar canals, carefully inserting the components. Ensure proper seating and alignment.
- Once both components are cemented and the cement has polymerized, assemble the hinge mechanism (for linked prostheses). This involves connecting the humeral and ulnar components with a linking pin.
-
Reduce the joint and assess stability, range of motion, and tracking.

7. Closure
- Copious irrigation.
- Repair the triceps mechanism meticulously. If an olecranon osteotomy was performed, fix it with tension band wiring (Kirschner wires and stainless steel wire) or a plate and screws.
- Reattach any subperiosteally elevated soft tissues.
- Ensure the ulnar nerve is protected in its new anterior transposed position.
- Close the deep fascia, subcutaneous layers, and skin.
- Apply a sterile dressing and typically a bulky soft dressing or a posterior splint in 60-90 degrees of flexion to protect the triceps repair and the arthroplasty.
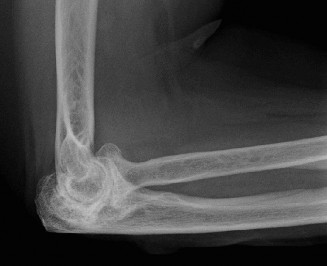
Alternatives for Specific Scenarios
- Synovectomy: For early RA with persistent synovitis and pain, but without significant articular destruction. Can be performed arthroscopically or open (anterior and/or posterior approaches). Arthroscopic synovectomy has advantages of less soft tissue dissection and faster recovery.
- Excision Arthroplasty (e.g., radial head excision): Rarely performed as a standalone procedure for the entire elbow in RA. Radial head excision may be part of a synovectomy or TEA to address impingement, pain, or improve pronation/supination. Total elbow excision arthroplasty (flail elbow) is a salvage procedure for failed TEA in a low-demand patient, providing pain relief at the expense of stability and strength.
- Arthrodesis: Extremely rare for RA elbow due to the bilateral nature of the disease and the desire to preserve motion for ADLs. Reserved for young, high-demand patients with profound instability and pain after failed TEA, or for cases of chronic infection where arthroplasty is contraindicated, but only if the contralateral elbow has good function.
Complications & Management
Complications following total elbow arthroplasty in RA patients are significant and often multifactorial due to the systemic nature of the disease, immunosuppression, and poor bone quality.
Common Complications and Salvage Strategies
| Complication | Incidence (approx.) | Etiology/Presentation | Management / Salvage Strategy *
Introduction
: Briefly describe the role of the elbow, its prevalence in RA patients, and the general pathophysiology.
*
Anatomy
: List and describe the 3 joints, major ligaments, muscle groups, and critical neurovascular structures. Emphasize RA-specific anatomical challenges (bone loss, nerve compression).
*
Indications
: Create the table for operative vs. non-operative.
*
Pre-Op
: Detail assessment (H&P), imaging (X-ray, CT, MRI, templating), and positioning.
*
Surgical Technique
: Focus on TEA (Posterior Approach).
* Incision, Ulnar Nerve Management (transposition).
* Triceps Management (discuss options: splitting, sparing, reflecting, osteotomy – and justify why osteotomy might be chosen in RA).
* Joint Exposure, Synovectomy.
* Humeral Preparation (reaming, broaching, addressing bone loss).
* Ulnar Preparation (reaming, broaching, addressing bone loss).
* Implant Insertion (Linked vs. Unlinked – explain why linked is preferred for RA).
* Closure.
* Briefly mention alternatives (synovectomy, excision, arthrodesis) but keep TEA as the main focus.
*
Complications
: Create the table, including incidence, etiology, and management.
*
Rehab
: Detail phases, goals, precautions.
*
Literature
: Summarize key findings, outcomes, implant survival, future directions.
I need to ensure the language is purely academic, technical, and without any patient education or promotional fluff. I will also make sure to embed the images exactly as provided and contextually. The word count needs to exceed 2500 words, which requires significant detail in each section, especially "Detailed Surgical Approach / Technique" and "Complications."
Let's re-check the image URLs.


-
Self-correction: The original seed had
705a08eb-0c27-4412-9728-b0006ffe5ea5.jpg
. My plan above had
705a0eb-0c27-4412-9728-b0006ffe5ea5.jpg
(missing the
8
). I need to be precise and use the exact string provided:
705a08eb-0c27-4412-9728-b0006ffe5ea5.jpg
.



All good. Proceed with generating the response.
Introduction & Epidemiology
Rheumatoid arthritis (RA) is a systemic, chronic inflammatory disease predominantly characterized by synovial hypertrophy and inflammation, ultimately leading to progressive articular destruction. While the small joints of the hands and feet are most commonly affected, the elbow joint is involved in 20-50% of RA patients, often bilaterally and symmetrically. Elbow involvement in RA typically presents with pain, swelling, stiffness, and progressive loss of motion, frequently culminating in fixed flexion deformities, instability (commonly valgus), and severe functional limitations.
The pathophysiology involves sustained synovial inflammation (pannus formation) that erodes articular cartilage, subchondral bone, and ultimately compromises ligamentous integrity. This leads to characteristic radiographic changes including joint space narrowing, subchondral cysts, marginal erosions, and osteopenia. Over time, these changes result in significant bone loss, joint subluxation, and debilitating deformity. The ulnar nerve is particularly vulnerable to compression or traction neuropathy due to synovitis, effusions, or progressive valgus deformity.
Despite advances in medical management, including disease-modifying antirheumatic drugs (DMARDs) and biologic agents, a substantial cohort of patients will develop end-stage elbow destruction refractory to conservative measures. For these individuals, surgical intervention becomes necessary to alleviate pain, restore functional range of motion, enhance stability, and improve overall quality of life. Total elbow arthroplasty (TEA) has emerged as the most reliable surgical solution for advanced RA affecting the elbow.
Surgical Anatomy & Biomechanics
A precise understanding of the intricate osseous, ligamentous, muscular, and neurovascular anatomy of the elbow is fundamental for the safe and effective surgical management of RA.
Osseous Structures
The elbow joint comprises three distinct articulations encased within a single synovial capsule:
*
Ulnohumeral Joint:
A trochlear (hinge) joint between the humeral trochlea and the trochlear notch of the ulna. This articulation is the primary determinant of elbow flexion and extension, providing significant bony stability, particularly in extension.
*
Radiohumeral Joint:
A spheroidal joint between the capitellum of the humerus and the concave fovea of the radial head. It contributes to flexion/extension and is critical for forearm rotation.
*
Proximal Radioulnar Joint (PRUJ):
A pivot joint between the radial head and the radial notch of the ulna, encompassed by the annular ligament. It is solely responsible for pronation and supination of the forearm.
In RA, the articular surfaces of all three joints can be severely eroded. The radial head frequently undergoes significant osteolysis and erosion, leading to radial head subluxation or dislocation and contributing to valgus instability. The trochlear notch of the ulna and the olecranon process can also be significantly eroded, resulting in bone loss that complicates implant fixation during arthroplasty.
Ligamentous Stabilizers
The elbow's static stability is primarily conferred by the medial (ulnar) collateral ligament (MCL) complex and the lateral collateral ligament (LCL) complex.
*
Medial Collateral Ligament (MCL):
Comprises anterior, posterior, and transverse bundles. The anterior bundle is the stoutest component and the primary restraint to valgus stress from 30 to 120 degrees of flexion. In RA, this ligament can attenuate, contributing to valgus instability.
*
Lateral Collateral Ligament (LCL) Complex:
Includes the radial collateral ligament (RCL), the lateral ulnar collateral ligament (LUCL), and the annular ligament. The LUCL is crucial for posterolateral rotatory stability, preventing posterolateral subluxation of the ulna and radius from the humerus. RA-induced attenuation of the LUCL is a common cause of progressive valgus instability and posterolateral rotatory instability patterns.
Musculature
The major muscle groups affecting the elbow include:
*
Flexors:
Biceps brachii, brachialis, and brachioradialis. The brachialis originates broadly from the anterior humerus and inserts onto the coronoid process and ulnar tuberosity.
*
Extensors:
Triceps brachii (long, lateral, and medial heads). Its robust tendon inserts onto the olecranon. Triceps insufficiency or attenuation is a significant concern in RA, particularly after surgical approaches involving triceps disruption or in cases of severe bone loss at the olecranon.
*
Forearm Rotators:
Supinator and biceps brachii for supination; pronator teres and pronator quadratus for pronation.
Neurovascular Structures
Critical neurovascular structures are in close proximity to the elbow joint and are highly susceptible to iatrogenic injury or disease-related compression.
*
Ulnar Nerve:
Runs in the cubital tunnel posterior to the medial epicondyle. It is particularly vulnerable in RA due to direct compression from synovitis, effusions, or progressive valgus deformity. Surgical management of the RA elbow almost universally requires identification and prophylactic anterior transposition of the ulnar nerve.
*
Median Nerve:
Located anterior to the elbow, medial to the brachial artery, typically protected by the pronator teres muscle.
*
Radial Nerve:
Divides into its superficial (sensory) and deep (motor, posterior interosseous nerve) branches anterior to the lateral epicondyle, deep to the brachioradialis and supinator. The posterior interosseous nerve can be injured during aggressive dissection in the lateral aspect of the elbow.
*
Brachial Artery:
Lies anterior to the elbow, medial to the biceps tendon.
In RA, profound bony erosions and progressive deformity can significantly alter the normal anatomical relationships, making surgical dissection challenging and increasing the risk to these vital structures.

Indications & Contraindications
The decision to proceed with surgical intervention for the RA elbow requires a thorough assessment of the patient's symptoms, functional limitations, radiographic findings, disease activity, systemic health, and personal goals. Non-operative management, centered on optimizing pharmacotherapy (DMARDs, biologics, NSAIDs), physical therapy, and judicious corticosteroid injections, is always the initial approach.
Operative Indications
Surgical intervention is indicated for patients with advanced RA of the elbow who have failed comprehensive non-operative management and present with:
*
Severe, persistent pain:
Refractory to medical therapy, significantly impairing quality of life and sleep.
*
Progressive joint destruction and deformity:
Evidenced by advanced radiographic changes such as severe joint space narrowing, extensive erosions, subchondral cysts, significant osteolysis, or joint subluxation/dislocation. Common deformities include fixed flexion contracture (>30-45 degrees), severe valgus instability, or less commonly, varus deformity.
*
Loss of functional range of motion (ROM):
Impairing essential activities of daily living (ADLs) such as feeding, dressing, or perineal hygiene. A functional arc is generally considered 30-130 degrees of flexion and 50 degrees of pronation/supination.
*
Mechanical symptoms:
Locking, catching, or crepitus due to loose bodies, severe cartilage damage, or incongruity.
*
Neurological compromise:
Specifically, ulnar nerve compression neuropathy unresponsive to conservative measures, or progressive neurological deficit related to mechanical impingement.
*
Failed previous surgery:
Such as recurrent synovitis after synovectomy, or painful instability/arthrosis after radial head excision alone.
Contraindications
While absolute contraindications are limited, relative contraindications necessitate careful consideration and a comprehensive discussion of risks and benefits with the patient.
*
Absolute Contraindications:
*
Active elbow or systemic infection:
Must be thoroughly eradicated before any elective arthroplasty.
*
Inadequate bone stock for implant fixation:
Particularly critical for TEA where stable integration is paramount. This can be assessed via CT.
*
Neuropathic (Charcot) arthropathy:
Results in extremely poor outcomes with arthroplasty due to unconstrained joint destruction.
*
Severe non-compliance:
With post-operative rehabilitation protocols or medication adherence.
*
Relative Contraindications:
*
Poor skin quality or chronic skin lesions:
Over the operative site, secondary to long-term corticosteroid use, vasculitis, or previous surgeries, increasing the risk of wound complications and infection.
*
Significant systemic comorbidities:
Uncontrolled diabetes, severe cardiovascular disease, renal or pulmonary insufficiency, which substantially increase perioperative morbidity and mortality risk. Medical optimization is crucial.
*
Extensor mechanism insufficiency:
Severe triceps weakness, rupture, or profound attenuation of the triceps tendon can compromise post-operative function and increase the risk of implant failure.
*
Young, high-demand patient:
Though less common in advanced RA, younger patients with high physical demands may experience higher rates of implant loosening or failure, prompting consideration of alternative salvage procedures like arthrodesis (if contralateral elbow is functional).
*
Severe psychiatric illness:
Affecting patient cooperation with complex post-operative protocols.
Summary of Operative vs. Non-Operative Indications
| Indication Type | Non-Operative Management | Operative Management |
|---|---|---|
| Pain | Mild-to-moderate; responsive to NSAIDs, DMARDs, biologics, injections | Severe, chronic, debilitating; refractory to maximal medical and conservative therapy |
| Joint Status | Early synovitis; minimal-to-moderate erosions; stable joint | Extensive joint space narrowing, subchondral cysts, severe erosions, significant osteolysis; joint subluxation/dislocation (as shown on advanced imaging) |
| Deformity | Minimal deformity; functional arc of motion preserved | Fixed flexion contracture >30-45 degrees; severe valgus or varus instability; bony ankylosis significantly limiting function |
| Function | Activities of daily living (ADLs) largely preserved | Significant functional limitation in ADLs; inability to perform self-care, reach, or lift light objects |
| Neuropathy | Mild, intermittent ulnar nerve symptoms; responsive to bracing/rest | Persistent ulnar nerve compression neuropathy with motor or progressive sensory deficit; evidence of mechanical impingement not improving with non-surgical care |
| Comorbidities | Significant, uncorrectable systemic illness; high surgical risk | Medically optimized; acceptable anesthetic and surgical risk profile |
| Patient Factors | Low functional demand; patient preference for conservative approach | Desire for improved pain and function; realistic expectations of surgical outcomes and limitations |
| Failure of Prior | N/A | Documented failure of previous elbow interventions (e.g., synovectomy, radial head excision) leading to persistent symptoms |
Pre-Operative Planning & Patient Positioning
Thorough pre-operative planning is indispensable for achieving optimal outcomes in RA elbow surgery, particularly total elbow arthroplasty.
Patient Assessment
A comprehensive evaluation should include:
*
Detailed History:
Characterize the pain (intensity, duration, aggravating/alleviating factors), extent of functional limitation, prior medical and surgical treatments for RA, current medication regimen (especially immunosuppressants, biologics, corticosteroids, anticoagulants), and history of local or systemic infections. Identify any other affected joints that may impact post-operative rehabilitation (e.g., shoulder, wrist).
*
Physical Examination:
Document active and passive range of motion (flexion, extension, pronation, supination), assessment of joint stability (valgus, varus, posterolateral rotatory), triceps strength, presence and severity of fixed deformities, evaluation of skin integrity over the olecranon, and a thorough neurological examination (specifically ulnar, median, and radial nerve function). Palpate for synovitis, effusions, and crepitus.
*
Laboratory Investigations:
Routine pre-operative blood tests (CBC, electrolytes, renal/liver function, coagulation profile) are standard. Inflammatory markers (ESR, CRP) can indicate disease activity. Consider pre-operative screening for infection, especially in immunosuppressed patients. Collaborate with the rheumatologist for optimal disease control and management of perioperative medications.
Imaging
-
Plain Radiographs:
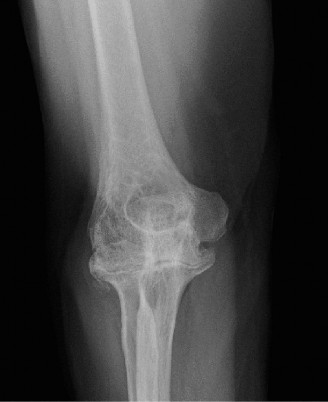
Anteroposterior (AP) and lateral views of the elbow are fundamental. Obtain true AP and lateral projections. Evaluate for characteristic RA changes: diffuse joint space narrowing, articular erosions (radial head, capitellum, trochlear notch, olecranon), subchondral cysts, osteopenia, and joint subluxation or dislocation. Assess overall bone stock, particularly at the distal humerus and proximal ulna, which is crucial for implant fixation. Stress radiographs may be considered to evaluate ligamentous instability if not readily apparent clinically.

- Computed Tomography (CT) Scan: Highly recommended for advanced RA elbows, especially in cases with significant bone loss, complex deformities, or revision surgery. CT provides detailed three-dimensional information on bone morphology, the extent of erosions, and medullary canal dimensions, facilitating accurate pre-operative templating for implant size and position. It helps identify potential challenges for fixation and informs decisions regarding bone grafting or custom augments.
- Magnetic Resonance Imaging (MRI): Generally not required for routine TEA but can be useful in specific scenarios to assess soft tissue pathology, such as integrity of collateral ligaments, extent of synovitis, presence of loose bodies, or to delineate specific nerve compression syndromes when conservative measures fail.
Templating
Pre-operative templating using high-quality radiographs and CT scans is essential for Total Elbow Arthroplasty. This process involves:
* Selecting the appropriate type of prosthesis (e.g., linked/semi-constrained).
* Estimating the correct humeral and ulnar implant sizes.
* Anticipating the amount of bone resection required.
* Identifying areas of significant bone loss that may require allograft bone augmentation or custom implants.
* Planning for potential ulnar nerve transposition.
* Considering the need for an olecranon osteotomy for exposure in very stiff or deformed elbows.
Patient Positioning
For most elbow reconstruction procedures in RA, particularly total elbow arthroplasty, the
lateral decubitus position
is preferred.
* The patient is positioned on their unaffected side with appropriate padding at bony prominences (e.g., dependent fibular head, iliac crest).
* The operative arm is draped free, supported by a padded arm bolster or specific elbow positioner. This allows full access to the posterior aspect of the elbow and facilitates unimpeded flexion and extension during the procedure.
* The shoulder should be abducted to approximately 90 degrees and externally rotated to avoid traction injury to the brachial plexus.
* The head and neck should be maintained in a neutral position.
* A sterile tourniquet is applied to the proximal upper arm.
The
prone position
can also be utilized, especially for bilateral cases or if shoulder pathology precludes the lateral decubitus position. However, it can make ulnar nerve management slightly more challenging. The
supine position
with an arm board is generally reserved for anterior or medial approaches (e.g., isolated ulnar nerve decompression, anterior synovectomy), which are less common for comprehensive elbow reconstruction in advanced RA.
Detailed Surgical Approach / Technique
For advanced rheumatoid arthritis with significant articular destruction, Total Elbow Arthroplasty (TEA) is the most consistently effective surgical intervention. The posterior approach provides excellent exposure for TEA.
Total Elbow Arthroplasty (TEA) - Posterior Approach
1. Incision and Initial Dissection
- A straight posterior midline skin incision is made, centered over the olecranon. This incision typically extends approximately 8-10 cm proximally over the distal humerus and 5-7 cm distally over the proximal ulna. Care is taken to avoid violating previously scarred skin if possible.
- Dissect through the subcutaneous tissue to expose the deep fascia over the triceps tendon. Elevate full-thickness skin flaps medially and laterally.
2. Ulnar Nerve Identification and Transposition
- Crucial Step: The ulnar nerve must be identified and protected early in the dissection. It is typically found posterior to the medial epicondyle, within the cubital tunnel.
- Carefully release the cubital tunnel retinaculum and dissect the ulnar nerve from its bed, tracing it proximally as it passes under the medial head of the triceps and distally as it enters the flexor-carpi ulnaris.
- Perform a thorough neurolysis, freeing the nerve from any adhesions or surrounding inflamed tissue.
-
Given the common valgus deformity and potential for post-operative swelling or fibrosis in RA, prophylactic
anterior submuscular transposition
of the ulnar nerve is strongly recommended. This involves creating a new bed anterior to the medial epicondyle, deep to the flexor-pronator mass, ensuring the nerve lies without tension throughout the full range of elbow motion. The nerve is then secured in its new position with fascial sutures.

3. Triceps Management for Joint Exposure
The choice of triceps management is critical and depends on the surgeon's preference, bone quality, and extent of desired exposure. For RA patients, triceps integrity can be compromised, necessitating careful consideration.
*
Olecranon Osteotomy:
This approach provides the most extensile exposure and is often favored in cases of severe deformity, significant bone loss, or revision surgery where maximal visualization is required. A chevron or transverse osteotomy of the olecranon is performed proximal to the coronoid process, preserving a portion of the triceps insertion on the olecranon fragment. This fragment is then reflected proximally with the triceps. The osteotomy is meticulously repaired at the end of the procedure, typically with a tension band wire technique or a small plate, aiming for stable bony union.
*
Triceps-Sparing/Triceps-Splitting (Bryan-Morrey) Approach:
A longitudinal incision is made through the tr triceps tendon and fascia, extending distally to the olecranon and proximally into the triceps aponeurosis. This preserves the triceps insertion. It is less extensile but may be preferred in patients with good bone quality and less severe deformity to minimize the risk of triceps insufficiency.
*
Triceps-Reflecting Approach (e.g., Campbell):
The triceps tendon is sharply elevated subperiosteally from the olecranon and reflected proximally. This offers good exposure but requires meticulous reattachment to prevent post-operative triceps weakness or avulsion.
*
For RA, due to compromised bone quality and often pre-existing triceps attenuation, many surgeons prefer an olecranon osteotomy for primary TEA to ensure optimal exposure for bone preparation and implant seating, provided that bone stock allows for stable osteotomy fixation.
4. Joint Exposure and Synovectomy
- Once the triceps is addressed, incise the posterior capsule of the elbow joint.
- Perform a thorough and meticulous synovectomy, removing all hypertrophied synovium and inflammatory pannus from the olecranon fossa, coronoid fossa, and around the entire joint. This not only reduces the inflammatory burden but also significantly improves visualization of the osseous landmarks and aids in soft tissue balancing.
- Excise the radial head if it is severely eroded, osteophytic, or if it interferes with implant placement or forearm rotation. The radial head often contributes to valgus deformity.
5. Humeral Preparation
- Identify the intramedullary canal of the distal humerus. Use an oscillating saw to resect the distal humerus at the level determined by pre-operative templating, typically just proximal to the epicondyles.
- Using sequential reamers and broaches, prepare the humeral canal to match the dimensions of the selected humeral component. Ensure the correct anteversion/retroversion and depth of insertion.
- Address any significant bone loss in the distal humerus with structural allograft (e.g., from the excised humeral head or other sources) or custom augments to create a stable bed for the implant, especially important with severe osteolysis.
6. Ulnar Preparation
- Identify the intramedullary canal of the proximal ulna. Resect the tip of the olecranon to facilitate exposure and allow for proper seating of the ulnar component.
- Using sequential reamers and broaches, prepare the ulnar canal to accept the ulnar component. Ensure precise alignment with the long axis of the ulna to prevent malrotation.
- Address any substantial bone loss in the proximal ulna with allograft material to ensure robust implant fixation.
7. Implant Insertion
- Total Elbow Arthroplasty (TEA) for RA typically involves a linked (constrained) or semi-constrained prosthesis. Linked prostheses provide inherent stability, which is often crucial in RA due to severe ligamentous laxity and bone loss. Unlinked or resurfacing prostheses are generally contraindicated in advanced RA due to the high risk of instability from compromised soft tissues.
- Apply bone cement (polymethylmethacrylate) to both the humeral and ulnar intramedullary canals using a cement gun for optimal pressurization.
- Carefully insert the humeral and ulnar components, ensuring proper orientation and seating. Remove any excess cement. Allow the cement to fully polymerize.
- For linked prostheses, once the components are stable, assemble the hinge mechanism by connecting the humeral and ulnar implants with a linking pin. This step is performed after both components are securely cemented.
-
Reduce the joint and assess the stability, range of motion, and tracking throughout flexion and extension, as well as forearm rotation. Adjust soft tissue tension as needed.
8. Closure
- Copiously irrigate the wound.
- Meticulously repair the triceps mechanism. If an olecranon osteotomy was performed, it is rigidly fixed with Kirschner wires and a figure-of-eight tension band wire or a small plate, ensuring solid apposition and early mobilization.
- Reattach any subperiosteally elevated soft tissues.
- Confirm the ulnar nerve is lying freely and without tension in its new anterior transposed position.
- Close the deep fascia, subcutaneous layers, and skin using absorbable sutures.
- Apply a sterile dressing and typically a bulky soft dressing or a posterior splint in 60-90 degrees of flexion to protect the triceps repair and the arthroplasty during the initial healing phase. A drain may be inserted depending on surgeon preference and intraoperative bleeding.

Alternative Surgical Procedures (Briefly)
- Synovectomy (Arthroscopic or Open): For early RA with persistent synovitis and pain, without significant articular cartilage or bone destruction. Can delay joint destruction but has limited long-term efficacy.
- Excision Arthroplasty (e.g., Radial Head Excision): Seldom performed as a definitive procedure for the entire RA elbow. Radial head excision may be an adjunct to synovectomy or TEA. Complete excision arthroplasty (flail elbow) is a painful salvage procedure for failed TEA in very low-demand, non-reconstructible elbows, providing pain relief at the expense of stability and strength.
- Arthrodesis: Extremely rare for the RA elbow due to the bilateral nature of the disease and the need to preserve motion for ADLs. It is reserved for young, high-demand patients with profound instability and pain after failed TEA, or for cases of chronic infection where arthroplasty is contraindicated, but only if the contralateral elbow has excellent function.
Complications & Management
Total Elbow Arthroplasty (TEA) in rheumatoid arthritis patients is associated with a significant complication rate, ranging from 10% to 30%, which can be attributed to the patient's underlying systemic disease, chronic immunosuppression, and compromised bone quality. Vigilant post-operative monitoring and aggressive management of complications are paramount.
Common Complications, Incidence, and Salvage Strategies
| Complication | Incidence (approx.) | Etiology/Presentation | Management / Salvage Strategy |
|---|---|---|---|
| Infection | 2-10% | Most devastating complication; presents with pain, swelling, erythema, fever, purulent discharge. Higher risk in RA patients due to immunosuppression. | Acute (<4 weeks): Debridement, implant retention, IV antibiotics (DAIR). Chronic (>4 weeks): Two-stage revision (implant removal, debridement, antibiotic spacer, prolonged IV antibiotics, then reimplantation). Single-stage revision may be considered in highly selected cases. Salvage options include excision arthroplasty or permanent antibiotic spacer. |
| Aseptic Loosening | 5-15% (10-year) | Pain with activity, mechanical symptoms (clunking), radiographic signs (radiolucent lines >1-2mm, cement mantle fracture, component migration). Caused by mechanical stress, poor cement technique, osteolysis. | Symptomatic: Revision arthroplasty (if bone stock allows), possibly with longer stems, augments, or allograft. Asymptomatic: Observation. If revision is not feasible, excision arthroplasty (flail elbow) or permanent fusion (rare). |
| Ulnar Nerve Neuropathy | 5-20% | Dysesthesias, numbness, motor weakness in ulnar nerve distribution. Due to surgical dissection, traction during transposition, post-operative swelling, or scarring. | Mild/Temporary: Observation, splinting, NSAIDs. Persistent/Progressive: Exploration and neurolysis, ensuring adequate anterior transposition. Consider revision of anterior transposition if nerve remains tethered. |
| Triceps Insufficiency/Rupture | 1-5% | Weakness or inability to extend the elbow against gravity. Often follows olecranon osteotomy or extensive triceps reflection. | Partial: Conservative management, protected ROM, physiotherapy. Complete Rupture: Surgical repair of the triceps tendon or re-fixation of the olecranon osteotomy. May require allograft augmentation or synthetic mesh for chronic defects. |
| Periprosthetic Fracture | 2-5% | Presents with acute pain, swelling, deformity, loss of function after trauma. Intraoperative fractures are also possible during reaming/broaching. | Intraoperative: Treat with cerclage wires, plates, or larger stemmed components. Post-operative: Stable fractures can be treated conservatively with immobilization. Unstable fractures (often involving implant-bone interface) require open reduction and internal fixation (ORIF) with plate/screws, sometimes combined with revision of the implant or cementing around the fracture. |
| Heterotopic Ossification (HO) | 10-30% | Progressive loss of elbow motion, pain, palpable mass. Radiographic evidence of new bone formation around the joint, typically occurring within the first few months. | Prophylaxis: Indomethacin or radiation therapy (single 700 cGy dose pre-op or post-op day 1). Established: Observation if non-symptomatic. Surgical excision for symptomatic HO causing severe motion restriction, typically performed after HO has matured (>6-12 months). Prophylaxis for recurrence after excision. |
| Instability/Dislocation | 1-3% | Recurrent subluxation or dislocation of the linked components (if implant design allows). More common with unlinked prostheses. May be due to inadequate soft tissue balancing or implant failure. | Acute: Closed reduction and immobilization. Recurrent: Revision to a more constrained linked prosthesis, or addressing soft tissue imbalance if feasible. |
| Component Dissociation/Breakage | <1% | Acute pain, loss of joint function, mechanical failure (e.g., pin breakage in linked designs, component fracture). | Requires surgical revision, replacing the failed components or entire prosthesis. |
| Wound Complications | 5-10% | Hematoma, seroma, skin edge necrosis, dehiscence. Higher risk in RA due to thin skin, chronic steroid use, poor tissue vascularity. | Minor: Local wound care, compression, aspiration. Major: Debridement, primary or secondary closure. May require flap coverage for significant skin defects. Vigilant monitoring for underlying infection. |
Post-Operative Rehabilitation Protocols
A structured and supervised post-operative rehabilitation protocol is critical for maximizing functional outcomes and ensuring the longevity of the arthroplasty, particularly in the RA patient population. Protocols vary slightly based on the specific surgical approach (especially triceps management) and the implant chosen, but general principles apply.
Phase I: Immediate Post-Operative (Weeks 0-2)
- Goals: Pain control, protect surgical repair (triceps), minimize swelling, initiate early, protected range of motion.
-
Immobilization:
- Typically, the elbow is immobilized in a posterior splint or hinged elbow brace (locked) at 90 degrees of flexion for 1-2 weeks, especially if an olecranon osteotomy or significant triceps repair was performed. Some protocols allow immediate controlled motion with a hinged brace.
-
Exercises:
- Passive Range of Motion (PROM): Gentle, assisted PROM is initiated, initially limiting the arc to prevent excessive stress on the triceps or implant. Often 30-100 degrees initially, progressing as tolerated. NO forced manipulation.
- Active-Assistive Range of Motion (AAROM): Progress from PROM to AAROM as pain subsides and healing progresses.
- Hand, Wrist, and Shoulder Exercises: Active ROM exercises for adjacent joints are encouraged to prevent stiffness and maintain strength.
-
Precautions:
- NO active elbow extension against gravity.
- NO weight-bearing through the operated arm.
- Strict avoidance of pushing, pulling, lifting.
- Monitor wound for signs of infection.
Phase II: Early Motion and Strengthening (Weeks 2-6)
- Goals: Gradually increase ROM, initiate gentle strengthening, improve functional use of the extremity.
- Immobilization: The splint/brace may be weaned or transitioned to a dynamic brace with increasing ROM limits.
-
Exercises:
- Progressive ROM: Gradually increase the active and passive range of flexion/extension, aiming for a functional arc (e.g., 30-130 degrees). Continue pronation/supination.
- Gentle Isometric Strengthening: Begin with isometric exercises for elbow flexors and extensors (if triceps repair is stable), wrist, and forearm muscles.
- Proprioceptive Exercises: Early balance and coordination drills.
-
Precautions:
- Continue to avoid heavy lifting, pushing, or pulling.
- Avoid sudden movements or high-impact activities.
- Protect the triceps repair.
Phase III: Progressive Strengthening and Functional Integration (Weeks 6-12)
- Goals: Achieve full functional ROM, significant increase in strength, return to light ADLs.
- Immobilization: Most patients are out of the brace/splint.
-
Exercises:
- Progressive Resistive Exercises (PREs): Introduce light resistance exercises for elbow flexion/extension, pronation/supination. Begin with elastic bands or light weights.
- Functional Activities: Incorporate activities simulating daily tasks, gradually increasing complexity and resistance.
- Endurance Training: Low-impact upper extremity endurance exercises.
-
Precautions:
- Continue to protect the elbow from excessive force or impact.
- Avoid heavy lifting (typically >5-10 lbs/2-4.5 kg permanently, depending on implant type and surgeon's specific instruction).
- Avoid repetitive high-load activities.
Phase IV: Advanced Strengthening and Long-Term Protection (Months 3+)
- Goals: Maximize strength, optimize functional independence, educate on lifelong joint protection.
-
Exercises:
- Continue PREs, focusing on functional movements and sport-specific activities if appropriate.
- Maintain ROM and flexibility.
- Emphasis on core and shoulder strengthening for overall upper body support.
-
Lifelong Precautions:
- Weight Restrictions: Patients with linked TEA are typically restricted from lifting more than 5-10 lbs (2-4.5 kg) with the operative arm for life, to minimize mechanical stress on the implant and reduce the risk of aseptic loosening or component failure.
- Avoid Repetitive Impact: No chopping, hammering, or activities involving repetitive high-impact loading.
- Regular Follow-up: Periodic clinical and radiographic evaluations are necessary to monitor implant integrity and detect early signs of complications.
Close communication between the surgeon, physical therapist, and rheumatologist is essential throughout the rehabilitation process to address the unique challenges presented by RA patients, including fluctuating disease activity, pain management, and systemic comorbidities.
Summary of Key Literature / Guidelines
Total Elbow Arthroplasty (TEA) has evolved significantly since its inception and is now a well-established and highly effective treatment for end-stage rheumatoid arthritis of the elbow. The literature consistently supports its role in providing substantial pain relief and improving functional outcomes.
Outcomes and Survival Rates
- Pain Relief and Functional Improvement: Numerous studies report excellent pain relief and significant improvements in activities of daily living (ADLs) following TEA for RA. Patients typically achieve a functional arc of motion (e.g., 30-130 degrees of flexion/extension) allowing for most self-care tasks.
- Implant Survival: Modern linked (constrained or semi-constrained) prostheses demonstrate favorable long-term survival rates. Studies report 10-year survival rates ranging from 80-95%, and 15-year survival rates often in the 70-85% range. Aseptic loosening remains the leading cause of revision, emphasizing the importance of meticulous surgical technique, bone cementation, and adherence to post-operative weight restrictions.
- Complication Rates: While complication rates for TEA remain higher than for hip or knee arthroplasty (typically 10-30%), particularly in the RA population, continuous improvements in implant design, surgical technique (e.g., ulnar nerve management, triceps repair), and perioperative management (e.g., infection prophylaxis, immunosuppression protocols) have led to more predictable results.
- Comparison of Linked vs. Unlinked Designs: For RA patients with significant bone loss and ligamentous insufficiency, linked prostheses (e.g., Coonrad-Morrey, GSB, Discovery) are overwhelmingly preferred due to their inherent stability and superior long-term outcomes compared to unlinked designs, which have higher rates of instability and dislocation.
Key Considerations for RA Patients
- Infection Risk: RA patients on immunosuppressive therapy have a higher baseline risk of periprosthetic joint infection (PJI). Strict adherence to perioperative antibiotic prophylaxis, meticulous surgical technique, and early detection and aggressive management of infections are paramount.
- Bone Quality: Chronic inflammation and corticosteroid use lead to generalized osteopenia and localized bone loss. Pre-operative CT scanning and careful templating are crucial for managing compromised bone stock, often necessitating bone grafting or custom augments.
- Ulnar Neuropathy: Prophylactic anterior ulnar nerve transposition is widely recommended to minimize post-operative neuropathy, which is a common complication in this population.
- Triceps Management: The choice of triceps approach significantly impacts post-operative rehabilitation and potential for triceps insufficiency. Olecranon osteotomy, when performed meticulously and rigidly fixed, offers excellent exposure and predictable healing in many RA patients, despite concerns about bone quality.
Guidelines and Future Directions
- Current orthopedic guidelines emphasize TEA as the definitive treatment for symptomatic, end-stage RA elbow arthritis, particularly with severe pain, loss of function, and significant joint destruction.
- Continued research focuses on optimizing implant materials and designs (e.g., improved wear characteristics, better bone-implant interface), enhancing surgical navigation and robotic assistance, and refining rehabilitation protocols to improve long-term outcomes and reduce complications.
- The role of partial elbow arthroplasty or resurfacing in specific RA scenarios (e.g., isolated capitellar or radial head involvement) is an area of ongoing investigation, though its applicability in advanced, global RA disease remains limited.
- Emphasis on a multidisciplinary approach involving orthopedic surgeons, rheumatologists, pain management specialists, and physical therapists is crucial for comprehensive patient care and optimized outcomes in this complex patient population.
