Introduction & Epidemiology
Osteoarthritis (OA) of the elbow, while less common than OA of the knee or hip, represents a significant source of pain and functional impairment in affected individuals. It is a degenerative joint disease characterized by progressive loss of articular cartilage, subchondral bone sclerosis, osteophyte formation, and synovial inflammation. Unlike larger weight-bearing joints where primary OA is prevalent, elbow OA often has a identifiable secondary etiology.
Epidemiology:
The prevalence of symptomatic elbow OA is estimated to be lower than other major joints, but its true incidence may be underestimated due to its often insidious onset and the elbow's inherent stability.
*
Primary OA:
Less frequent. More commonly observed in older males, often associated with occupations involving repetitive upper extremity loading, particularly heavy manual labor or sports with overhead activities (e.g., throwing athletes, weightlifters). It typically manifests with osteophyte formation limiting terminal extension and flexion, followed by cartilage loss.
*
Secondary OA:
Accounts for the majority of cases.
*
Post-traumatic Arthritis:
The most common cause, frequently following intra-articular fractures (distal humerus, olecranon, radial head), dislocations, or chronic instability. Malunion, nonunion, and persistent incongruity accelerate degenerative changes.
*
Inflammatory Arthritis:
Conditions such as rheumatoid arthritis, psoriatic arthritis, gout, and seronegative spondyloarthropathies can lead to severe joint destruction and subsequent OA.
*
Occupational/Repetitive Stress:
Long-term, high-impact activities or repetitive forceful motions can lead to microtrauma and accelerate cartilage degeneration. Examples include jackhammer operators, construction workers, and competitive athletes.
*
Crystalline Deposition Disease:
Gout and pseudogout can cause destructive arthropathy.
*
Osteochondritis Dissecans (OCD):
Especially in younger athletes, can lead to focal cartilage damage and eventual OA.
*
Hemophilia:
Recurrent hemarthroses cause chronic synovitis and cartilage destruction.
Clinical presentation typically involves progressive pain, stiffness, loss of motion (especially extension and flexion), mechanical symptoms like clicking or locking, and sometimes ulnar nerve irritation due to osteophyte encroachment. Diagnosis relies on a comprehensive history, physical examination, and radiographic evaluation demonstrating joint space narrowing, osteophytes, subchondral sclerosis, and possibly loose bodies.
Surgical Anatomy & Biomechanics
A thorough understanding of elbow anatomy and biomechanics is paramount for safe and effective surgical intervention in elbow osteoarthritis. The elbow is a complex ginglymoarthrodial joint comprising three distinct articulations within a single capsule: the humeroulnar joint (trochlea and olecranon), the humeroradial joint (capitellum and radial head), and the proximal radioulnar joint (radial head and radial notch of the ulna).
Osseous Anatomy
- Distal Humerus: Characterized by the medial and lateral epicondyles, the trochlea (medial, spool-shaped, articulating with the ulna), and the capitellum (lateral, spherical, articulating with the radial head). The olecranon fossa posteriorly and the coronoid and radial fossae anteriorly accommodate the olecranon, coronoid process, and radial head during extreme flexion and extension, respectively. Osteophytes frequently form at the coronoid and olecranon tips, limiting motion.
- Proximal Ulna: Consists of the olecranon (posterior, forming the tip of the elbow), the coronoid process (anterior), and the trochlear (semilunar) notch, which articulates with the humeral trochlea. The radial notch is located laterally on the coronoid process.
- Proximal Radius: Composed of the radial head (cylindrical, articulating with the capitellum and radial notch of the ulna), the radial neck, and the radial tuberosity (insertion of the biceps tendon).
Ligamentous Stabilizers
The static stability of the elbow is primarily provided by strong collateral ligament complexes.
*
Medial Collateral Ligament (MCL) Complex:
The primary valgus stabilizer.
*
Anterior Bundle:
Strongest, most important component. Originates from the medial epicondyle and inserts on the sublime tubercle of the ulna. Taut throughout flexion.
*
Posterior Bundle:
Thickening of the posterior capsule, taut in extreme flexion.
*
Transverse Ligament (Cooper's Ligament):
Does not contribute to stability.
*
Lateral Collateral Ligament (LCL) Complex:
The primary varus and posterolateral rotatory stabilizer.
*
Radial Collateral Ligament:
Originates from the lateral epicondyle, blends with the annular ligament.
*
Annular Ligament:
Encircles the radial head, maintaining its approximation to the radial notch of the ulna.
*
Accessory Lateral Collateral Ligament:
Reinforces the annular ligament.
*
Lateral Ulnar Collateral Ligament (LUCL):
The critical stabilizer against posterolateral rotatory instability. Originates from the lateral epicondyle and inserts on the supinator crest of the ulna.
Musculature and Neurovascular Structures
-
Muscles:
- Flexors: Biceps brachii, brachialis, brachioradialis.
- Extensors: Triceps brachii, anconeus.
- Pronators: Pronator teres, pronator quadratus.
- Supinators: Supinator, biceps brachii.
-
Nerves:
- Ulnar Nerve: Most vulnerable nerve in elbow surgery. Courses in the cubital tunnel, posterior to the medial epicondyle. At risk during medial approaches, osteophyte resection, and extensive soft tissue release.
- Radial Nerve: Passes anterior to the lateral epicondyle, then divides into superficial (sensory) and deep (posterior interosseous nerve, motor) branches. At risk during lateral approaches, particularly near the radial head and neck.
- Median Nerve: Courses anterior to the elbow joint, protected by the biceps aponeurosis. Less commonly injured but at risk during anterior capsular releases or extensive anterior debridement.
- Vessels: Brachial artery bifurcates into radial and ulnar arteries distal to the joint. Numerous recurrent branches (radial recurrent, ulnar recurrent interosseous recurrent) supply the joint and are at risk during capsular dissection.
Biomechanics
The elbow joint functions primarily as a hinge joint, allowing flexion and extension from approximately 0° to 150°. However, it also permits pronation and supination (80° each way) through the combined humeroradial and proximal radioulnar articulations.
*
Carrying Angle:
The normal valgus angulation of the forearm relative to the humerus in extension (typically 10-15° in males, 15-20° in females) results from the obliquity of the trochlear groove.
*
Stability Arcs:
The elbow exhibits inherent bony stability, particularly the humeroulnar joint. During the arc of motion, the MCL and LCL complexes maintain stability. Degenerative changes, especially osteophyte formation at the coronoid and olecranon, progressively limit terminal flexion and extension, leading to a restricted arc of motion. Loose bodies can cause intermittent locking.
*
Articular Pressure:
The humeroulnar joint bears the majority of load in flexion and extension. The radiocapitellar joint is primarily involved in axial loading and forearm rotation. OA can lead to increased stress concentrations and progressive cartilage loss in these specific areas.
Indications & Contraindications
Surgical management of elbow osteoarthritis is considered when non-operative measures have failed to provide adequate pain relief or functional improvement. The decision for operative intervention is multifactorial, considering the patient's age, activity level, medical comorbidities, specific functional demands, and the extent and distribution of arthritic changes.
Non-Operative Indications (Conservative Management)
Initial management for elbow OA is typically non-operative and aims to alleviate pain, reduce inflammation, and improve function.
*
Early/Mild OA:
Symptoms are intermittent, tolerable, or do not significantly interfere with daily activities.
*
Failed Conservative Trials:
Patients should have trialed these for at least 3-6 months.
*
Activity Modification:
Avoidance of provocative activities, especially repetitive lifting, carrying, or sports-specific movements.
*
Pharmacotherapy:
Non-steroidal anti-inflammatory drugs (NSAIDs) orally or topically. Acetaminophen.
*
Physical Therapy:
Focus on maintaining range of motion, gentle stretching, strengthening periarticular musculature (biceps, triceps, forearm flexors/extensors) without aggravating pain. Modalities such as heat, ice, ultrasound.
*
Intra-articular Injections:
*
Corticosteroids:
Provide temporary pain relief by reducing inflammation, but do not alter disease progression. Repeated injections should be approached cautiously due to potential cartilage degradation and infection risk.
*
Viscosupplementation (Hyaluronic Acid):
Efficacy in the elbow is less well-established than in the knee, but may be considered for symptomatic relief in selected cases.
*
Platelet-Rich Plasma (PRP) / Other Biologics:
Emerging therapies with limited high-level evidence for elbow OA, considered experimental in many settings.
Operative Indications
Surgery is considered for patients with persistent, debilitating pain and/or significant functional limitation despite adequate non-operative management.
*
Pain Refractory to Conservative Treatment:
The primary indication for most surgical interventions.
*
Limited Range of Motion (ROM):
Significant loss of flexion and/or extension interfering with activities of daily living (e.g., inability to feed oneself, perform hygiene). A functional arc of motion is generally considered to be 30-130° flexion/extension and 50° pronation/supination.
*
Mechanical Symptoms:
Locking, catching, or giving way due to loose bodies, severe osteophytes, or articular incongruity.
*
Neurological Symptoms:
Ulnar nerve compression neuropathy (cubital tunnel syndrome) directly attributable to osteophytes or structural deformity associated with OA.
*
Progressive Joint Destruction:
Radiographic evidence of severe joint space narrowing, large osteophytes, or bone-on-bone articulation in younger, active patients where alternative solutions are sought.
Contraindications
General medical contraindications apply to all surgical procedures. Specific contraindications for elbow OA surgery vary by procedure type.
*
Absolute Contraindications:
*
Active Infection:
Local (e.g., cellulitis, septic arthritis) or systemic. Requires eradication prior to elective surgery.
*
Severe Systemic Medical Comorbidities:
Uncontrolled cardiac disease, diabetes, coagulopathy, or other conditions that significantly increase surgical risk and preclude safe anesthesia or recovery.
*
Non-compliance:
Unrealistic patient expectations or inability to adhere to demanding post-operative rehabilitation protocols.
*
Severe Neuropathic Arthropathy (Charcot Joint):
Difficult to manage surgically due to bone fragility and poor healing potential.
*
Relative Contraindications:
*
Osteoporosis:
Particularly for arthroplasty, may compromise implant fixation.
*
Extensive Soft Tissue Loss/Poor Skin Quality:
May impede wound healing or increase infection risk.
*
Prior Surgery with Significant Scarring:
Can complicate subsequent dissection and increase risk of neurovascular injury.
*
Young, Highly Active Patients:
For total elbow arthroplasty (TEA), as implant longevity and ability to withstand high loads are concerns. Interposition arthroplasty or arthroscopic debridement may be considered first.
Table: Operative vs. Non-Operative Indications for Elbow Osteoarthritis
| Feature / Category | Non-Operative Indications | Operative Indications |
|---|---|---|
| Pain | Mild to moderate, intermittent, tolerable, or responsive to activity modification. | Severe, chronic, debilitating pain refractory to at least 3-6 months of comprehensive non-operative management. |
| Functional Limitation | Minimal impact on daily activities; functional ROM maintained (e.g., 30-130° flexion/extension). | Significant loss of range of motion (e.g., <100° arc of motion), inability to perform essential ADLs (feeding, hygiene, dressing), or occupational tasks. |
| Mechanical Symptoms | Absent or infrequent, mild clicking without true locking/catching. | Persistent locking, catching, or giving way suggestive of large loose bodies, significant osteophytes, or severe articular incongruity. |
| Nerve Involvement | Absent or mild, transient paresthesias responsive to conservative measures. | Persistent ulnar neuropathy (cubital tunnel syndrome) directly attributable to osteophyte impingement or deformity associated with OA, unresponsive to conservative care. |
| Radiographic Changes | Early OA: mild joint space narrowing, minimal osteophyte formation, no loose bodies. | Moderate to severe OA: significant joint space narrowing, large osteophytes (anterior/posterior), subchondral sclerosis, loose bodies, gross articular incongruity, subchondral cysts. |
| Patient Profile | Any age, patient preference for conservative approach, medical comorbidities precluding surgery. | Age and activity level dictate procedure choice (e.g., arthroscopy/debridement for younger active patients; TEA for older, lower demand; interposition for intermediate). Patient willingness to undergo rehabilitation. |
| Previous Treatment | No prior surgical intervention or minimal success with previous minor procedures. | Documented failure of comprehensive non-operative treatment including NSAIDs, activity modification, physical therapy, and appropriate injections over an adequate period (typically 3-6 months). Failed previous conservative surgery. |
Pre-Operative Planning & Patient Positioning
Careful pre-operative planning is essential to anticipate potential challenges and optimize surgical outcomes for elbow osteoarthritis. This phase encompasses detailed patient evaluation, advanced imaging, and meticulous consideration of the surgical approach and patient positioning.
Pre-Operative Evaluation
- Clinical Assessment: Comprehensive history focusing on pain characteristics, functional limitations, mechanical symptoms, and any neurological complaints. Physical examination includes assessment of skin integrity, active and passive range of motion (flexion, extension, pronation, supination), joint stability (valgus/varus stress), and neurological status (ulnar, median, radial nerve function).
-
Radiographic Imaging:
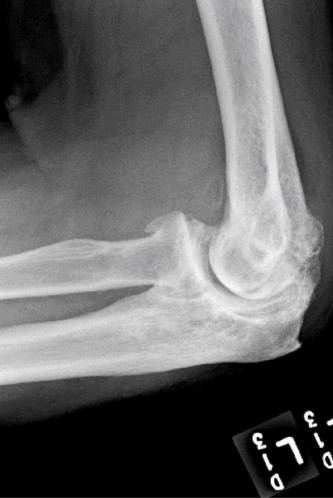
- Standard Radiographs: AP, lateral, and oblique views are crucial for assessing joint space narrowing, osteophyte burden (anterior coronoid, posterior olecranon, radial head), subchondral sclerosis, and the presence of loose bodies. Weight-bearing views are not typically used for the elbow.
- Computed Tomography (CT) Scan: Highly valuable for complex OA, especially post-traumatic cases. Provides detailed information on bone morphology, the size and location of osteophytes, quantification of loose bodies, and assessment of bone stock for potential arthroplasty. 3D reconstructions are extremely helpful for visualizing complex deformities and planning osteophyte excision or implant placement.
- Magnetic Resonance Imaging (MRI): Less commonly indicated for isolated OA unless soft tissue pathology (e.g., ligamentous injury, chondral defects, synovitis) is suspected. Can help assess articular cartilage integrity and visualize inflamed synovium or effusions.
- Neurophysiological Studies: Electromyography (EMG) and nerve conduction studies (NCS) are indicated if ulnar nerve entrapment is suspected, to confirm the diagnosis and quantify the severity of compression. This guides decisions regarding concurrent ulnar nerve release or transposition.
Surgical Decision-Making
Based on the pre-operative evaluation, the surgeon determines the most appropriate surgical intervention:
*
Arthroscopic Debridement:
Indicated for early to moderate OA with predominant symptoms of mechanical locking/catching, loose bodies, or isolated osteophyte impingement without extensive joint destruction or instability.
*
Open Debridement / Ulnohumeral Arthroplasty (Outerbridge-Kashiwagi Procedure):
For more extensive osteophyte formation, significant loss of motion, or complex loose body removal not amenable to arthroscopy. Often involves ulnar nerve protection/transposition.
*
Interposition Arthroplasty:
Considered in younger, active patients with diffuse OA but good bone stock, aiming to preserve motion and function while avoiding total joint replacement. Materials include fascia lata, Achilles tendon allograft, or capsular interposition.
*
Total Elbow Arthroplasty (TEA):
Reserved for end-stage OA with severe pain, gross articular destruction, or failed previous surgeries, particularly in older, lower-demand patients or those with inflammatory arthritis.
*
Radial Head Excision/Replacement:
For isolated symptomatic radiocapitellar OA or as part of a more comprehensive debridement.
*
Osteotomy:
Rarely indicated for primary OA, primarily for post-traumatic malunion with significant deformity.
Patient Positioning and Surgical Preparation
Proper positioning is critical for optimal exposure, surgeon comfort, and prevention of iatrogenic injury.
*
General Anesthesia:
Regional nerve blocks (e.g., interscalene block) can be used as an adjunct for post-operative pain control.
*
Tourniquet:
Essential for a bloodless field, typically applied high on the arm.
*
Positions:
*
Lateral Decubitus:
*
Advantages:
Excellent access to medial and lateral aspects of the elbow, easy assessment of motion, ability to "drop" the arm for gravity-assisted exposure.
*
Setup:
Patient positioned on their side, operative arm draped free. A padded arm holder or commercially available elbow positioner is used to support the arm, allowing flexion and extension. The shoulder is abducted, and the elbow is typically flexed to 90 degrees.
*
Prone:
*
Advantages:
Excellent posterior exposure for triceps-sparing or triceps-reflecting approaches, good for ulnar nerve management.
*
Setup:
Patient is prone with the operative arm abducted on an arm board. Head turned away from the operative side. Careful padding of pressure points.
*
Supine with Arm Across Chest:
*
Advantages:
Good for anterior approaches or less extensive procedures. Can be easily converted to lateral decubitus.
*
Setup:
Patient supine, operative arm placed across the chest on a sterile Mayo stand or arm rest.
*
Padding:
Meticulous padding of all pressure points, especially the contralateral elbow, axilla, and bony prominences, is crucial to prevent nerve compression or skin breakdown.
*
Draping:
Sterile draping should allow full range of motion of the elbow during the procedure for assessment of debridement adequacy or implant fit.
Detailed Surgical Approach / Technique
Surgical management of elbow osteoarthritis is tailored to the severity of disease, patient demands, and specific pathology. The goal is to reduce pain, improve range of motion, and restore function.
I. Arthroscopic Debridement
Indications: Early to moderate OA, mechanical symptoms (locking/catching), loose bodies, isolated osteophytes, and synovitis. Less effective for diffuse cartilage loss or severe stiffness.
Patient Positioning:
Lateral decubitus or prone with the arm draped free.
Portals:
Typically 6 standard portals are used. Careful planning is essential to avoid neurovascular structures (ulnar, radial, median nerves, brachial artery).
*
Proximal Anteromedial & Anterolateral:
(~2 cm proximal to epicondyles, anterior to intermuscular septa) for viewing and instrumentation of the anterior compartment.
*
Distal Anteromedial & Anterolateral:
(~1 cm distal to epicondyles, anterior to intermuscular septa) for anterior compartment work.
*
Direct Posterior:
(~2 cm proximal to olecranon tip) for posterior viewing/instrumentation.
*
Posterolateral:
(~2 cm proximal to olecranon, lateral to triceps tendon) for posterior compartment.
*
Mid-medial:
For specific pathology or Ulnar Nerve Release.
Technique:
1.
Distention:
Initial joint distention with saline via a needle placed in the soft spot or anterolateral portal.
2.
Anterior Compartment:
* Systematic evaluation for synovitis, cartilage damage, loose bodies, and osteophytes.
*
Loose Body Removal:
Grasping forceps or suction shaver.
*
Capsular Release:
Anterior capsular contracture limiting extension can be released.
*
Coronoid Osteophyte Excision:
Using a shaver or osteotome, carefully resect anterior osteophytes from the coronoid fossa and tip, ensuring not to compromise the coronoid itself or underlying cartilage.
3.
Posterior Compartment:
* Systematic evaluation for synovitis, cartilage damage, loose bodies, and osteophytes.
*
Olecranon Osteophyte Excision:
Resect posterior osteophytes from the olecranon fossa and tip to improve terminal extension.
*
Ulnar Nerve Decompression:
If osteophytes encroach on the cubital tunnel, arthroscopic or open release may be performed.
4.
Humeroradial Joint:
Assess for osteophytes on the radial head and capitellum, which can be debrided.
5.
Closure:
Portal sites are closed with sterile strips or sutures.
II. Open Debridement / Ulnohumeral Arthroplasty (Outerbridge-Kashiwagi Procedure)
Indications:
Significant motion loss (especially extension), large osteophytes not amenable to arthroscopy, or extensive loose bodies.
Approach:
Posterior approach, typically with an initial ulnar nerve release.
Technique (Key Steps):
1.
Ulnar Nerve Identification and Protection:
Essential for all posterior elbow approaches. An incision is made over the olecranon, extending proximally along the triceps and distally along the ulna. The ulnar nerve is identified proximal to the cubital tunnel, dissected free, and protected throughout the procedure. Subcutaneous or submuscular anterior transposition may be performed if the nerve is highly mobile, subluxating, or if significant cubital valgus is present.
2.
Triceps Management:
*
Triceps-Sparing:
The triceps tendon is retracted, not incised. Offers faster rehabilitation but more limited exposure.
*
Triceps-Splitting:
Longitudinal incision through the triceps aponeurosis and muscle. Offers better exposure but potentially slower recovery.
*
Triceps Reflection (Olecranon Osteotomy):
Provides the widest exposure but involves osteotomy of the olecranon, requiring fixation (tension band wiring or plate/screws) and longer protection. Rarely necessary for primary OA debridement.
3.
Capsule and Synovectomy:
The posterior capsule is incised longitudinally. Synovectomy can be performed if significant synovitis is present.
4.
Osteophyte Excision:
*
Olecranon Fossa Debridement:
The olecranon fossa is cleared of osteophytes and soft tissue impinging on the olecranon tip during extension. This is critical for restoring extension.
*
Olecranon Tip Resection:
A small portion of the olecranon tip (up to 5mm) can be resected to further improve extension, particularly in cases of impingement.
*
Coronoid Osteophyte Excision:
The anterior compartment is accessed by carefully distracting the joint. Osteophytes from the coronoid fossa and tip are removed to improve flexion. This often requires careful dissection to protect the anterior capsule and median nerve.
5.
Loose Body Removal:
All identified loose bodies are meticulously removed.
6.
Humeroradial Debridement:
Osteophytes from the radial head and capitellum are removed, and the radial head can be debrided. Isolated radial head excision may be considered for severe radiocapitellar OA.
7.
Closure:
The capsule and triceps (if incised) are repaired. Skin closure in layers.
III. Interposition Arthroplasty
Indications:
Younger, active patients with diffuse end-stage OA who are not candidates for TEA, but have failed less invasive debridement. Aims to provide a biological spacer between articulating surfaces.
Materials:
Fascia lata autograft (most common), Achilles tendon allograft, dermal allograft, capsular interposition.
Approach:
Similar to open debridement, often a posterior approach with ulnar nerve transposition.
Technique:
1.
Exposure and Debridement:
Extensive debridement of osteophytes and loose bodies, similar to ulnohumeral arthroplasty. The joint is prepared by removing remaining articular cartilage down to bleeding subchondral bone.
2.
Graft Harvest:
If fascia lata is used, it is harvested from the lateral thigh (typically 15x20 cm).
3.
Graft Placement:
The graft is typically sewn into the resected areas. For total interposition, the graft is draped over the entire articular surface of the distal humerus, secured with absorbable sutures or bone anchors at the epicondyles. The radial head may be resected or resurfaced with the graft.
4.
Closure:
Standard layered closure.
IV. Total Elbow Arthroplasty (TEA)
Indications:
End-stage OA with severe pain, gross articular destruction, instability, or failed previous surgeries, particularly in older, lower-demand patients or those with inflammatory arthritis.
Contraindications:
Active infection, insufficient bone stock, severe skin compromise, non-compliance, high-demand lifestyle in younger patients.
Implant Types:
*
Linked (Constrained/Semi-constrained):
Most common. Components are physically linked (hinged) to provide stability, compensating for deficient soft tissue stabilizers. Semi-constrained designs allow some rotation and varus/valgus motion.
*
Unlinked (Resurfacing):
Separate humeral and ulnar components. Relies on intact collateral ligaments for stability. Less common for OA due to high rates of instability.
*
Custom Implants:
For severe bone loss or unique anatomies.
Approach (Posterior, often Triceps-Sparing or Triceps-Reflecting):
1.
Incision:
Posterior midline incision centered over the olecranon.
2.
Ulnar Nerve:
Identify and protect the ulnar nerve throughout, often performing an anterior transposition.
3.
Triceps Management:
*
Triceps-Sparing:
A longitudinal incision is made in the deep fascia to the medial and lateral sides of the triceps tendon, which is then elevated from the humerus and capsule. The triceps tendon is retracted to allow exposure.
*
Triceps-Reflecting:
A V-Y lengthening of the triceps or a triceps-splitting approach can be used. Some surgeons prefer an olecranon osteotomy for maximum exposure, especially in revision cases, but this adds morbidity.
4.
Capsular Incision and Exposure:
The posterior capsule and anconeus muscle are carefully incised and elevated.
5.
Humeral and Ulnar Preparation:
*
Humeral Component:
The distal humerus is resected precisely using cutting guides to create the appropriate bone cuts (distal, anterior, posterior). The intramedullary canal is reamed for the humeral stem.
*
Ulnar Component:
The proximal ulna is resected, and the intramedullary canal is reamed for the ulnar stem.
*
Image showing the bone cuts for a total elbow arthroplasty:
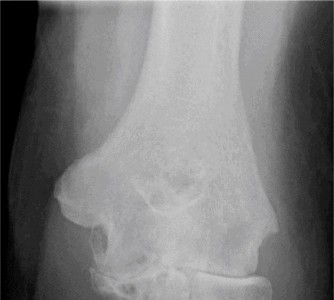
6.
Trial Reduction:
Trial implants are inserted, and range of motion and stability are assessed. Adjustments to bone cuts or soft tissue releases may be necessary.
7.
Cementation:
The definitive humeral and ulnar components are cemented into place using standard bone cement techniques. The linkage pin is inserted.
8.
Irrigation and Hemostasis:
Thorough irrigation and careful hemostasis are performed.
9.
Closure:
The capsule is repaired. The triceps mechanism is meticulously repaired (if incised/detached). Subcutaneous and skin closure in layers. A drain may be placed.
*
Image showing an implanted total elbow arthroplasty:
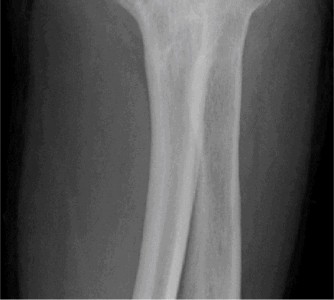
V. Radial Head Excision / Replacement
Indications:
Isolated symptomatic radiocapitellar OA, painful rheumatoid arthritis, or as part of a more extensive debridement in post-traumatic OA.
Approach:
Lateral Kocher approach.
Technique:
1.
Incision:
Lateral incision between the anconeus and extensor carpi ulnaris (ECU) muscles.
2.
Identification:
Identification and protection of the posterior interosseous nerve (PIN), which enters the supinator distally.
3.
Resection:
The radial head is resected using an oscillating saw. Care is taken to avoid over-resection, which can lead to proximal migration of the radius and wrist pain.
4.
Replacement (Arthroplasty):
A modular radial head prosthesis may be implanted if stability is a concern or if significant proximal migration is anticipated. This is particularly relevant in cases of associated medial collateral ligament insufficiency.
5.
Closure:
Standard layered closure.
Complications & Management
Elbow osteoarthritis surgery, regardless of the technique employed, carries potential risks and complications. Proactive recognition and appropriate management are crucial for mitigating adverse outcomes.
Table: Common Complications of Elbow OA Surgery
| Complication | Incidence | Salvage Strategy / Management |
|---|---|---|
| Infection | 1-5% (higher for TEA) | Acute: Debridement, irrigation, retention of implants (if stable), IV antibiotics (6+ weeks). Chronic/TEA: Two-stage revision arthroplasty (explant, spacer, IV antibiotics, re-implantation), or permanent implant removal with resection arthroplasty/arthrodesis. |
| Ulnar Nerve Neuropathy | 5-15% (transient), 1-5% (persistent) | Mild/Transient: Observation, rest, NSAIDs. Persistent/Progressive: Ulnar nerve neurolysis, +/- anterior transposition, if not performed initially. |
| Radial Nerve (PIN) Injury | <1% (rare but devastating) | Exploration, neurolysis, or nerve graft depending on injury severity. Wrist extension orthosis. |
| Stiffness / Loss of Motion | Up to 20-30% after debridement | Early: Aggressive physical therapy, dynamic splinting. Persistent: Manipulation under anesthesia (MUA), arthroscopic or open capsular release. |
| Heterotopic Ossification (HO) | 10-50% (radiographic), 5-10% (symptomatic) | Prophylaxis: Indomethacin (pre- and post-op), single-dose radiation. Symptomatic: Excision of HO (after maturation, ~6-12 months post-op) with post-op prophylaxis. |
| Instability (Post-TEA) | 2-5% | Bracing, activity modification. Revision with more constrained implant, ligament repair/reconstruction if applicable. |
| Implant Loosening/Failure (TEA) | 5-10% at 5-10 years | Revision arthroplasty (component exchange, bone grafting if needed), or resection arthroplasty. |
| Fracture (Intra-op/Periprosthetic) | 1-2% | Internal fixation with plates/screws (if good bone quality), revision of components, conversion to resection arthroplasty. |
| Complex Regional Pain Syndrome (CRPS) | <1% | Early recognition, aggressive pain management (nerve blocks, gabapentin), physical therapy. |
| Vascular Injury | Rare (brachial artery) | Immediate surgical exploration, repair, or bypass grafting. |
Detailed Management Strategies
1. Infection
- Acute Post-operative Infection (<4-6 weeks): Typically managed with aggressive surgical debridement and lavage, with retention of implants if they are stable and not obviously contaminated. Intravenous antibiotics, guided by culture sensitivities, are administered for 4-6 weeks, often followed by oral suppression.
- Chronic Infection (>4-6 weeks) or Infected TEA: Management is more challenging. For TEA, a two-stage revision is often necessary: explantation of components, thorough debridement, placement of an antibiotic-loaded cement spacer, and 6-12 weeks of culture-specific intravenous antibiotics. After infection markers normalize and bone quality is acceptable, reimplantation of new components is performed. In cases where reimplantation is not feasible due to bone loss or patient factors, permanent resection arthroplasty (flail elbow) or arthrodesis (rarely done for elbow) may be considered.
2. Neurological Injury
-
Ulnar Nerve:
The most commonly injured nerve.
- Transient Neuropraxia: Often resolves spontaneously. Observation, rest, and NSAIDs.
- Persistent Symptoms/Compression: If symptoms persist or worsen, formal open neurolysis of the ulnar nerve and anterior transposition (if not already done) is indicated to decompress the nerve.
-
Radial/Median Nerves:
Less common but more debilitating.
- Intraoperative Laceration: Requires immediate microsurgical repair.
- Postoperative Palsy/Paresis: Observation for neuropraxia. EMG/NCS at 6-12 weeks if no improvement. Exploration and neurolysis if indicated.
3. Stiffness / Loss of Motion
- Early Post-operative: Aggressive but controlled physical therapy, continuous passive motion (CPM) machines, and dynamic splinting.
- Established Contracture: If conservative measures fail, manipulation under anesthesia (MUA) may be considered after 3-6 months. For recalcitrant stiffness, arthroscopic or open capsular release (anterior, posterior, or both) may be necessary, often with removal of heterotopic ossification.
4. Heterotopic Ossification (HO)
- Prophylaxis: In high-risk patients (e.g., post-traumatic, extensive surgical dissection, burns, head injury), prophylactic measures include non-steroidal anti-inflammatory drugs (NSAIDs) such as Indomethacin for 3-6 weeks post-operatively, or a single dose of post-operative radiation therapy (700-800 cGy within 72 hours of surgery).
- Treatment of Symptomatic HO: Surgical excision is performed once the HO has matured (typically 6-12 months post-surgery, confirmed by alkaline phosphatase levels and radiographs). Excision should be followed by post-operative prophylaxis.
5. Instability (Post-Total Elbow Arthroplasty)
- Ligamentous Insufficiency: In linked designs, instability can manifest as linkage pin failure or excessive play. In unlinked designs, collateral ligamentous repair or reconstruction may be required.
- Component Malposition: Revision of poorly positioned components.
- Recurrent Instability: May necessitate revision to a more constrained implant or, in severe cases, conversion to a resection arthroplasty.
6. Implant Loosening/Failure (Total Elbow Arthroplasty)
- Aseptic Loosening: Managed by revision arthroplasty, involving exchange of loose components, potentially with bone grafting for cavitary defects.
- Periprosthetic Fracture: Managed with open reduction internal fixation (ORIF) for stable constructs or revision arthroplasty if the fracture compromises implant stability or bone stock significantly.
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is a critical determinant of functional outcomes following elbow surgery for osteoarthritis. Protocols vary significantly depending on the specific surgical procedure, intraoperative findings, and implant stability. A multidisciplinary approach involving the surgeon, physical therapist, and patient is essential.
General Principles
- Pain Management: Adequate pain control is paramount to facilitate early motion. This includes multimodal analgesia, regional blocks, and oral medications.
- Protection: Protecting surgical repairs (e.g., triceps, collateral ligaments, ulnar nerve transposition) from excessive stress.
- Early Motion: Initiating range of motion as soon as safely possible to prevent stiffness and optimize articular cartilage health (if retained).
- Gradual Progression: Systematically increasing intensity of exercises, resistance, and functional demands.
- Patient Education: Ensuring the patient understands the limitations, goals, and commitment required for rehabilitation.
Specific Protocols by Procedure
I. Arthroscopic Debridement / Open Debridement / Ulnohumeral Arthroplasty
These procedures are generally less restrictive regarding post-operative motion.
*
Phase 1: Immediate Post-operative (Weeks 0-2)
*
Protection:
Sling for comfort and protection, usually for 1-7 days. Avoid aggressive weight-bearing.
*
Motion:
Early initiation of active-assisted and passive range of motion (AAROM/PROM) exercises for flexion, extension, pronation, and supination within pain limits. Goal is to achieve maximal safe ROM as quickly as possible.
*
Soft Tissue Care:
Wound care, edema management (ice, elevation).
*
Ulnar Nerve (if transposed):
Avoid excessive elbow flexion and direct pressure on the nerve for the first few weeks.
*
Phase 2: Intermediate (Weeks 2-6)
*
Motion:
Progress to active range of motion (AROM). Continue working on gaining full, pain-free ROM.
*
Strengthening:
Begin gentle isometric exercises for biceps, triceps, and forearm musculature. Progress to light resistance with elastic bands or low weights.
*
Functional Activities:
Gradual return to light activities of daily living (ADLs).
*
Phase 3: Advanced Strengthening & Return to Activity (Weeks 6-12+)
*
Strengthening:
Progressive resisted exercises, focusing on muscular endurance and strength.
*
Functional Training:
Sport-specific or work-specific drills, emphasizing controlled movements and proper body mechanics.
*
Return to Activity:
Gradual return to full activities, typically by 3-4 months, depending on symptoms and functional goals. Avoid heavy lifting or impact activities for several months.
II. Interposition Arthroplasty
Rehabilitation is similar to debridement but often more prolonged due to the extensive joint resurfacing and graft healing.
*
Phase 1: Protection & Early Motion (Weeks 0-6)
*
Splinting:
Often placed in a static or dynamic splint, with initial protective range of motion (e.g., 30-100 degrees of flexion/extension) to protect the graft. This may vary based on surgeon preference and graft security.
*
Motion:
Gentle AAROM/PROM within protected arc. Focus on minimizing stress on the graft while preventing stiffness.
*
Phase 2: Progressive Motion & Gentle Strengthening (Weeks 6-12)
*
Motion:
Gradually increase ROM as tolerated.
*
Strengthening:
Light isometric exercises, progressing to very light resistance.
*
Phase 3: Strengthening & Functional Return (Weeks 12-24+)
* Progressive strengthening and functional activities, with a more cautious return to heavy lifting or impact activities, typically 6-12 months post-operatively.
III. Total Elbow Arthroplasty (TEA)
Rehabilitation protocols for TEA are highly structured and typically more restrictive due to the need to protect the implant-bone interface and soft tissue repairs (especially the triceps).
*
Phase 1: Protection & Controlled Motion (Weeks 0-6)
*
Splinting:
A posterior splint is typically applied post-operatively, often at 90 degrees of flexion, for 1-2 weeks. Some surgeons advocate for immediate motion in a dynamic splint.
*
Motion:
Strict limitations on active range of motion initially, especially against gravity, to protect the triceps repair and implant fixation. Passive and active-assisted ROM, often in a supine position or with assistance from a therapist, is initiated within a specific arc (e.g., 30-90 degrees, gradually increasing to 0-130 degrees).
*
Weight-Bearing Restrictions:
Absolutely NO active elbow flexion against gravity for 4-6 weeks (if triceps reflected/incised). No pushing, pulling, or lifting anything heavier than a coffee cup.
*
Ulnar Nerve:
Continue nerve gliding exercises if transposition was performed.
*
Phase 2: Gradual Strengthening & Increased ROM (Weeks 6-12)
*
Motion:
Gradually increase active ROM, aiming for a functional arc.
*
Strengthening:
Begin gentle isometric exercises for biceps and triceps. Progress to very light, controlled resistance (e.g., 1-2 lbs). Active elbow extension against gravity may begin around 6 weeks if triceps repair is solid.
*
Functional Activities:
Light ADLs. Continue to educate on strict weight-bearing restrictions.
*
Phase 3: Advanced Strengthening & Functional Integration (Weeks 12+)
*
Strengthening:
Progressive resistance exercises, but with continued adherence to
LIFELONG WEIGHT-BEARING RESTRICTIONS
.
*
Lifelong Restrictions:
Patients are strictly limited to lifting no more than 10-15 lbs (4.5-6.8 kg) with the operative arm. Avoid repetitive impact, pushing/pulling, or activities that place high torsional stresses on the implant. No racquet sports, heavy gardening, or demanding manual labor.
*
Return to Light Activities:
Gradual return to appropriate recreational and occupational activities within these restrictions.
IV. Radial Head Excision/Replacement
-
Phase 1: Early Motion (Weeks 0-2)
- Sling for comfort. Immediate AAROM and PROM for flexion/extension, pronation/supination.
-
Phase 2: Strengthening (Weeks 2-6)
- Progressive strengthening, starting with isometrics and advancing to light resistance.
-
Phase 3: Functional Return (Weeks 6+)
- Full activities as tolerated. If radial head replacement, follow similar, but less restrictive, weight-bearing precautions as TEA, based on surgeon preference and implant fixation.
Summary of Key Literature / Guidelines
The management of elbow osteoarthritis has evolved significantly with advancements in arthroscopic techniques, implant design, and rehabilitation protocols. Current literature emphasizes a stepwise approach, starting with conservative management and progressing to surgical intervention only after failure of non-operative measures.
Key Themes in Current Literature:
- Arthroscopy vs. Open Debridement: Numerous studies support arthroscopic debridement as an effective treatment for early to moderate elbow OA, particularly for mechanical symptoms and limited motion due to osteophytes and loose bodies. Outcomes are generally favorable in terms of pain relief and motion improvement, with lower morbidity than open procedures. However, open debridement remains a viable option for extensive disease, large osteophytes, or cases where arthroscopic visualization is challenging. Long-term results of arthroscopic debridement, especially for diffuse cartilage loss, remain mixed, with recurrence of symptoms or progression of OA being potential concerns.
- Ulnar Nerve Management: Prophylactic ulnar nerve release or transposition is a common consideration during extensive posterior elbow surgery for OA, given the high incidence of pre-existing or post-operative ulnar neuropathy. While the necessity of routine transposition in the absence of pre-operative symptoms is debated, most surgeons advocate for careful identification and protection, with transposition reserved for symptomatic nerve, subluxating nerve, or extensive bony resection.
- Interposition Arthroplasty: Literature suggests interposition arthroplasty, particularly with fascia lata, can provide satisfactory pain relief and improved motion in select younger, active patients with diffuse OA, where TEA is deemed inappropriate due to high functional demands. However, results are often less predictable than TEA, with potential for continued pain, graft failure, or progressive stiffness. Long-term durability and consistent outcomes remain areas of ongoing research.
- Total Elbow Arthroplasty (TEA): TEA is considered the gold standard for end-stage elbow OA, especially in older, lower-demand patients or those with inflammatory arthritis. Modern semi-constrained designs have shown reliable pain relief and functional improvement with reasonable long-term survival rates (e.g., 85-95% at 5-10 years). However, the procedure is not without significant complications, including infection, aseptic loosening, and periprosthetic fracture. Patient selection and adherence to lifelong activity restrictions are paramount for implant longevity and success. The impact of activity restrictions on patient quality of life is a continuous discussion.
- Prophylaxis for Heterotopic Ossification (HO): The incidence of HO following elbow surgery, especially for post-traumatic OA, is well-documented. Numerous studies advocate for prophylactic measures, typically with NSAIDs (e.g., indomethacin for 3-6 weeks) or a single dose of post-operative radiation therapy, to reduce symptomatic HO and improve motion outcomes.
- Radial Head Excision/Replacement: For isolated radiocapitellar OA, radial head excision can effectively relieve pain and restore motion, but care must be taken to avoid proximal migration of the radius, particularly in cases of concomitant medial collateral ligament deficiency. Radial head replacement is often favored in these scenarios to maintain radiocapitellar stability and prevent wrist pain (e.g., DRUJ disruption).
- Rehabilitation: Evidence consistently highlights the crucial role of early, controlled range of motion in preventing stiffness after elbow surgery. Protocols for TEA are particularly stringent, emphasizing protection of the triceps mechanism and strict adherence to weight-bearing limitations to prevent early failure and maximize implant survival.
- Emerging Concepts: Ongoing research focuses on biologics (PRP, stem cells) for early cartilage repair, although definitive evidence for their widespread use in elbow OA is still developing. Advances in implant materials and surgical techniques continue to refine outcomes and potentially expand indications for arthroplasty.
Guidelines and Consensus:
While specific, universally adopted guidelines for elbow OA are less codified than for knee or hip OA, orthopedic societies and consensus statements generally advocate for:
1. Initial conservative management for all patients.
2. Surgical debridement/arthroscopy for mechanical symptoms, loose bodies, and isolated osteophytes.
3. Interposition arthroplasty for select younger, active patients with diffuse disease where TEA is unsuitable.
4. Total Elbow Arthroplasty for end-stage disease with severe pain and functional loss, particularly in older, lower-demand individuals.
Long-term follow-up studies and registries continue to provide valuable data on the durability of various interventions and inform evidence-based treatment algorithms for this challenging joint.
