Comprehensive Introduction and Patho-Epidemiology
Fractures of the hallucal sesamoids represent a unique, highly nuanced, and frequently mismanaged pathology within foot and ankle orthopaedic surgery. These injuries are most frequently encountered in two distinct clinical scenarios: acute high-energy trauma, often associated with forced hyperextension and dislocations of the first metatarsophalangeal (MTP) joint, and chronic stress fractures. The latter is predominantly seen in high-demand athletic populations, particularly long-distance runners, ballet dancers, gymnasts, and turf-sport athletes where repetitive, high-impact axial loading is concentrated on the forefoot.
The diagnostic complexity of sesamoid fractures lies in the meticulous differentiation of true osseous failure from other confounding pathologies affecting the sesamoid complex. The clinician must routinely distinguish acute fractures from the highly prevalent symptomatic bipartite sesamoid, osteochondritis dissecans, osteonecrosis (avascular necrosis), and soft-tissue derangements of the plantar plate. Misdiagnosis, delayed treatment, or inappropriate conservative management can lead to chronic debilitating pain, altered gait mechanics, transfer metatarsalgia, and progressive, irreversible degenerative joint disease of the first ray.
Epidemiologically, hallucal sesamoid injuries account for approximately 9% of all foot and ankle injuries in the athletic population, yet fractures constitute only a small fraction of these presentations. The tibial (medial) sesamoid is fractured significantly more often than the fibular (lateral) sesamoid, a phenomenon directly related to its anatomical position directly beneath the medial aspect of the first metatarsal head, where it bears the brunt of weight-bearing forces during the terminal stance and push-off phases of the gait cycle. Conversely, fibular sesamoid fractures are comparatively rare and are typically the result of direct crush injuries or violent lateral dislocation events.
The mechanism of injury dictates the fracture morphology and subsequently guides surgical decision-making. Direct trauma, such as a fall from a significant height landing on a plantarflexed forefoot, typically produces a comminuted, multifragmented fracture pattern with associated chondral damage to the metatarsal head. Indirect trauma, which is vastly more common in turf sports, involves a violent tensile force transmitted through the flexor hallucis brevis (FHB) and plantar plate during extreme MTP hyperextension. This mechanism classically results in a transverse fracture or a proximal avulsion-type injury, effectively disrupting the continuity of the flexor apparatus and necessitating precise anatomical restoration to preserve forefoot biomechanics.
Detailed Surgical Anatomy and Biomechanics
To fully grasp the implications of sesamoid fractures and execute their surgical management with precision, a profound understanding of the first MTP joint's biomechanics and microvascular anatomy is mandatory. The hallucal sesamoids are specialized ossicles embedded within the tendinous insertions of the medial and lateral heads of the FHB muscle. They articulate dorsally with the plantar facets of the first metatarsal head, separated by the prominent metatarsal crista, which provides intrinsic osseous stability and prevents subluxation during physiological loading.
The sesamoid complex is a highly integrated biomechanical unit. The sesamoids are firmly interconnected by the robust intersesamoidal ligament and serve as integral, load-bearing components of the plantar plate. The tibial sesamoid is generally larger, longer, and bears a significantly higher load during the stance phase. It is seated more directly beneath the medial facet of the metatarsal head. The fibular sesamoid is smaller, more circular, and slightly more mobile, rendering it highly susceptible to injury during violent hyperextension or lateral MTP dislocation events. Together, these ossicles function as a critical fulcrum, increasing the mechanical advantage of the FHB tendon, much like the patella does for the quadriceps mechanism.
Beyond their mechanical role in flexion, the sesamoids absorb massive weight-bearing forces, reduce frictional wear, and create a protective anatomical tunnel for the flexor hallucis longus (FHL) tendon, which glides smoothly between them. Disruption of the sesamoid complex alters the moment arm of the intrinsic musculature, leading to profound weakness in hallux plantarflexion and subsequent destabilization of the medial longitudinal arch during dynamic propulsion.
The vascular anatomy of the sesamoids is of paramount clinical significance, particularly concerning fracture healing and the risk of osteonecrosis. The blood supply is derived primarily from the medial and lateral plantar arteries, which form a rich anastomotic network. However, the intraosseous vascularity is tenuous. The predominant arterial inflow enters the sesamoids via their proximal poles and plantar surfaces, coursing distally. Consequently, transverse fractures can completely disrupt the blood supply to the distal pole, predisposing the fragment to avascular necrosis and nonunion. This retrograde vascular pattern closely mirrors that of the scaphoid and the talus, necessitating meticulous soft-tissue handling during surgical approaches to preserve the surviving periosteal vessels.
Exhaustive Indications and Contraindications
The decision-making algorithm for surgical intervention in hallucal sesamoid fractures is complex and must be highly individualized, taking into account the patient's athletic demands, chronological age, fracture morphology, and the chronicity of the injury. While many non-displaced or stress fractures can be successfully managed conservatively with strict immobilization, offloading, and extended rest (often requiring 3 to 6 months), surgical intervention becomes necessary when conservative measures are exhausted or when the initial presentation precludes non-operative success.
Surgical management is generally indicated for widely displaced acute fractures, highly comminuted fractures with significant intra-articular step-off, fractures associated with irreducible MTP dislocations, and symptomatic nonunions that have failed rigorous, protracted conservative care. The surgical strategy—whether it be Open Reduction and Internal Fixation (ORIF), bone grafting, or partial/complete sesamoidectomy—depends heavily on the viability of the fracture fragments and the integrity of the articular cartilage.
Conversely, absolute contraindications to surgical intervention include active local infection, severe peripheral vascular disease precluding wound healing, and medically unstable patients unfit for anesthesia. Relative contraindications encompass asymptomatic nonunions, highly non-compliant patients who will not adhere to strict postoperative weight-bearing restrictions, and the presence of advanced, diffuse degenerative joint disease of the first MTP joint, where a primary arthrodesis may be a more appropriate definitive procedure.
| Indication / Contraindication Category | Specific Clinical Scenario | Rationale / Clinical Consequence |
|---|---|---|
| Absolute Surgical Indications | Open sesamoid fractures | High risk of deep space infection and osteomyelitis requiring immediate irrigation and debridement. |
| Absolute Surgical Indications | Fractures with irreducible MTP dislocation | Soft tissue interposition (often the plantar plate or sesamoid complex itself) preventing closed reduction. |
| Relative Surgical Indications | Acute, displaced transverse fractures (>2mm) in high-level athletes | High risk of nonunion and prolonged loss of function; ORIF restores the flexor mechanism rapidly. |
| Relative Surgical Indications | Symptomatic chronic nonunion (failed >6 months conservative care) | Chronic pain and altered gait mechanics; requires bone grafting, ORIF, or partial excision. |
| Absolute Contraindications | Bilateral complete sesamoidectomy | Inevitably results in a severe, rigid claw toe (cock-up) deformity due to complete loss of the intrinsic flexor mechanism. |
| Absolute Contraindications | Active localized soft tissue infection or osteomyelitis | Operating through infected tissue risks catastrophic joint sepsis and hardware failure. |
| Relative Contraindications | Advanced first MTP joint osteoarthritis | Sesamoid-specific surgery will not relieve global joint pain; MTP arthrodesis is the preferred alternative. |
Pre-Operative Planning, Templating, and Patient Positioning
Thorough preoperative planning is the cornerstone of successful sesamoid surgery. The diagnostic workup must begin with a comprehensive, weight-bearing radiographic series. Standard anteroposterior (AP) and lateral views of the foot are obligatory, but specialized views are required to accurately profile the sesamoid complex. The lateral view in slight pronation helps to project the sesamoids away from the overlapping metatarsal head. Medial and lateral oblique views are highly sensitive for isolating the tibial and fibular sesamoids, respectively. The axial sesamoid view is perhaps the most critical, allowing for direct visualization of the sesamoid-metatarsal articulation, revealing joint space narrowing, subchondral sclerosis, or osteochondral defects.
The most significant diagnostic hurdle during preoperative planning is distinguishing an acute fracture from a bipartite sesamoid. The sesamoids are reported to be multipartite in 5% to 30% of asymptomatic individuals, predominantly affecting the tibial sesamoid. The surgeon must scrutinize the radiographs for key distinguishing features: fractured sesamoid bones tend to divide roughly into equally sized sections with irregular, jagged, and uncorticated margins. Conversely, bipartite sesamoids typically present with one dominant, larger fragment and one smaller accessory fragment, exhibiting smooth, well-corticated, and rounded edges.
When plain radiographs are equivocal, advanced imaging is absolutely warranted. High-resolution Computed Tomography (CT) is excellent for delineating subtle fracture lines, assessing the degree of comminution, and evaluating the articular surface for step-offs that would necessitate ORIF over excision. Magnetic Resonance Imaging (MRI) is increasingly utilized to assess bone marrow edema, osteonecrosis of the fracture fragments, and concomitant soft tissue injuries, such as plantar plate ruptures or FHL tenosynovitis, which may dictate a change in the surgical approach.
In the operating room, meticulous patient positioning is critical for adequate exposure and intraoperative fluoroscopy. The patient is placed in the supine position on a radiolucent operating table. A bump is placed under the ipsilateral hip to internally rotate the leg, bringing the medial aspect of the foot into a neutral, easily accessible position (particularly important for tibial sesamoid approaches). A well-padded thigh tourniquet is applied to ensure a bloodless surgical field, which is essential for identifying the delicate plantar digital nerves. The fluoroscopy unit (C-arm) is brought in from the contralateral side, ensuring unobstructed AP, lateral, and axial imaging of the first MTP joint throughout the procedure.
Step-by-Step Surgical Approach and Fixation Technique
The surgical management of hallucal sesamoid fractures demands meticulous soft-tissue handling and precise osseous fixation. The primary surgical options include Open Reduction and Internal Fixation (ORIF), autologous bone grafting, partial sesamoidectomy, and complete sesamoidectomy. Regardless of the chosen method, the overriding principle is the anatomical restoration and secure repair of the flexor mechanism.
Open Reduction and Internal Fixation (ORIF)
ORIF is considered the gold standard for acute, displaced transverse fractures of the sesamoid, particularly in young, high-demand athletic patients where the preservation of the sesamoid's biomechanical function is paramount.
For the tibial sesamoid, a medial longitudinal incision is utilized. The incision is centered over the medial eminence but kept slightly plantar to avoid the medial dorsal cutaneous nerve. Deep dissection must carefully identify and protect the medial plantar proper digital nerve, which frequently courses perilously close to the inferior border of the sesamoid. The fracture site is exposed by longitudinally incising the medial capsule and the FHB tendinous expansion. The fracture hematoma is evacuated, and the jagged edges of the fracture are meticulously debrided with a curette to expose bleeding, viable cancellous bone.
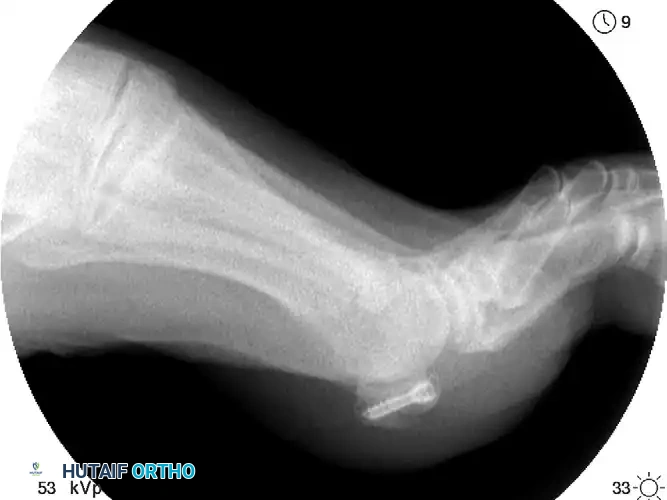
Reduction of the fracture is achieved using a specialized pointed reduction clamp, ensuring that the articular surface is perfectly congruent to prevent post-traumatic arthritis. Fixation is typically achieved using a mini-fragment screw system. A 1.5 mm to 2.0 mm cannulated or solid headless compression screw is directed from proximal to distal (or distal to proximal, depending on fragment size and vascular considerations) to achieve rigid interfragmentary compression. The surgeon must confirm via intraoperative axial fluoroscopy that the screw does not violate the dorsal articular surface.
Partial and Complete Sesamoidectomy
Excision of the fractured pole (partial sesamoidectomy) is indicated when the fragment is too small, comminuted, or avascular to support rigid fixation. The offending fragment is carefully shelled out of the FHB tendon using sharp dissection, taking extreme care not to violate the FHL tendon sheath. The most critical step of this procedure is the meticulous repair of the resulting defect in the FHB tendon. The tendon must be reapproximated using heavy non-absorbable sutures (e.g., #2-0 FiberWire) to restore the tension and continuity of the flexor apparatus. Failure to perform a robust repair will inevitably result in weakness and potential angular deformity.
Complete excision of the sesamoid is reserved strictly as a salvage procedure for highly comminuted fractures with no reconstructable fragments, severe osteonecrosis, or profound loss of articulating cartilage. The entire sesamoid is enucleated from its tendinous envelope. The surgeon must meticulously repair the capsulotendinous defect, often imbricating the tissue to maintain appropriate tension. As previously stated, complete excision of both the tibial and fibular sesamoids is strongly contraindicated due to the catastrophic resultant claw toe deformity.
Complications, Incidence Rates, and Salvage Management
While outcomes following sesamoid surgery are generally favorable, complications can be severe, debilitating, and exceedingly difficult to salvage if strict surgical principles are violated. The orthopaedic surgeon must be acutely aware of the potential pitfalls and possess the technical repertoire to manage them effectively.
The most feared complications relate to biomechanical imbalance following sesamoid excision. Excision of the tibial sesamoid weakens the medial head of the FHB, allowing the unresisted lateral structures (adductor hallucis and lateral FHB) to pull the hallux into a progressive hallux valgus deformity. Conversely, excision of the fibular sesamoid can result in an unresisted pull of the medial structures (abductor hallucis), leading to an iatrogenic hallux varus. The prevention of these deformities relies entirely on the careful, robust soft-tissue repair of the tendinous defect left after excision.
Neurological complications are also prevalent. Postoperative scarring and iatrogenic transection or traction injury to the plantar proper digital nerves can result in excruciatingly painful neuroma formation. This is particularly noted after plantar approaches to the fibular sesamoid, which is why a dorsal approach through the first web space is often advocated by experienced foot and ankle surgeons. Additionally, altered weight-bearing mechanics following excision or malunion can lead to intractable plantar keratosis (transfer metatarsalgia) under the remaining sesamoid or adjacent lesser metatarsal heads.
| Complication | Estimated Incidence | Pathophysiology / Cause | Salvage Management Strategy |
|---|---|---|---|
| Iatrogenic Hallux Valgus | 10% - 15% (Post-tibial excision) | Loss of medial FHB integrity; unresisted pull of adductor hallucis. | Medial capsulorrhaphy, abductor hallucis advancement, or first MTP arthrodesis in severe cases. |
| Iatrogenic Hallux Varus | 5% - 10% (Post-fibular excision) | Loss of lateral FHB/adductor integrity; unresisted pull of abductor hallucis. | Extensor hallucis brevis transfer, lateral capsule release, or first MTP arthrodesis. |
| Plantar Digital Neuroma | 5% - 8% | Iatrogenic nerve injury or entrapment in scar tissue, common with plantar incisions. | Conservative measures (injections, orthotics); surgical neurolysis or neurectomy with proximal burying. |
| Transfer Metatarsalgia | 15% - 20% | Altered load distribution following sesamoid excision or altered first ray mechanics. | Custom accommodative orthotics with relief padding; rarely requires corrective metatarsal osteotomies. |
| Nonunion / Hardware Failure | 5% - 10% (Post-ORIF) | Avascularity of the fragment, inadequate compression, or premature weight-bearing. | Revision ORIF with autologous bone grafting, or conversion to partial/complete sesamoidectomy. |
Phased Post-Operative Rehabilitation Protocols
Postoperative rehabilitation following hallucal sesamoid surgery is a critical determinant of the final functional outcome. The protocol must be meticulously phased and tailored to the specific surgical procedure performed, balancing the need for tissue healing with the prevention of capsular scarring and joint stiffness.
Phase 1: Immediate Post-Operative Period (Weeks 0-2)
Following ORIF or bone grafting, the primary goal is the protection of the fragile osseous fixation. Patients are typically placed in a well-padded, non-weight-bearing short leg cast or a rigid controlled ankle motion (CAM) boot. Strict non-weight-bearing status is enforced using crutches or a knee scooter. Elevation and strict adherence to cryotherapy protocols are mandated to control edema and minimize wound complications. Following partial or complete sesamoidectomy, the protocol may be slightly accelerated, allowing for protected heel-weight-bearing in a specialized postoperative stiff-soled shoe, provided the soft-tissue repair is deemed robust by the operating surgeon.
Phase 2: Intermediate Healing and Mobilization (Weeks 2-6)
At the two-week mark, sutures are removed. For ORIF patients, non-weight-bearing in a CAM boot is continued until radiographic evidence of early callus formation is observed, typically around 4 to 6 weeks. For sesamoidectomy patients, active and passive MTP joint mobilization is initiated aggressively. Gentle plantarflexion and dorsiflexion exercises are critical to prevent capsular adhesions and preserve the gliding mechanism of the FHL tendon. Weight-bearing is gradually advanced to full weight-bearing in a stiff-soled shoe or CAM boot, guided by the patient's pain tolerance.
Phase 3: Strengthening and Return to Function (Weeks 6-12)
Once osseous union is confirmed in ORIF patients, or soft-tissue healing is complete in excision patients, the focus shifts to restoring intrinsic foot strength and normalizing gait mechanics. Physical therapy incorporates progressive resistance exercises for the FHB, FHL, and extrinsic lower leg musculature. Proprioceptive training and balance exercises are introduced. Transition to standard athletic footwear is permitted, often augmented with a custom orthotic featuring a Morton's extension or a specific sesamoid relief pad to offload the surgical site during the final stages of healing.
Phase 4: Return to Play (Weeks 12+)
Return to competitive sports is a highly individualized milestone. Criteria for return to play include entirely pain-free full weight-bearing, restoration of at least 80% of contralateral MTP joint range of motion, and the ability to perform sport-specific dynamic movements (e.g., sprinting, cutting, jumping) without apprehension or biomechanical compensation. Literature indicates that following successful partial sesamoidectomy, athletes frequently return to competitive sports at a mean time of 7.5 to 10 weeks, whereas recovery following ORIF may require 12 to 16 weeks to ensure absolute osseous consolidation prior to subjecting the joint to maximum athletic loads.
Summary of Landmark Literature and Clinical Guidelines
The surgical management of hallucal sesamoid fractures has evolved significantly over the past three decades, guided by landmark clinical studies and biomechanical analyses. Historically, complete sesamoidectomy was viewed as a benign, definitive solution for sesamoid pathology. However, early literature, notably the seminal biomechanical studies by Aper et al., definitively demonstrated the profound loss of push-off power and the high incidence of iatrogenic deformities associated with complete excision. This catalyzed a paradigm shift toward joint-preserving procedures.
The current consensus, strongly supported by the American Orthopaedic Foot & Ankle Society (AOFAS) guidelines, prioritizes ORIF for acute, displaced fractures in high-demand patients. Studies by Anderson and colleagues have consistently demonstrated that successful ORIF restores nearly normal first MTP joint kinematics and yields superior long-term functional scores compared to excision. Furthermore, their research highlighted the critical importance of utilizing headless compression screws to avoid dorsal articular impingement.
In the realm of chronic nonunions, the work of Blundell et al. established autologous bone grafting as a highly viable, joint-preserving alternative to excision, reporting union rates exceeding 85% in carefully selected, compliant patients. When excision is unavoidable, the literature unequivocally stresses the necessity of meticulous soft-tissue reconstruction. Biedert's comprehensive review of sesamoidectomies in athletically active patients confirmed that while partial excision yields excellent pain relief and a rapid return to sport (mean 7.5 weeks), the complication rate skyrockets if the FHB tendinous defect is not robustly repaired.
Ultimately, the contemporary orthopaedic surgeon must approach hallucal sesamoid fractures with a high index of suspicion, precise radiographic interpretation, and a nuanced, evidence-based approach to surgical intervention. Whether undertaking internal fixation, grafting, or excision, the paramount objective remains the anatomical restoration of the first ray's complex soft-tissue envelope to ensure optimal functional recovery and the prevention of long-term debilitating sequelae.
