
DEFINITION
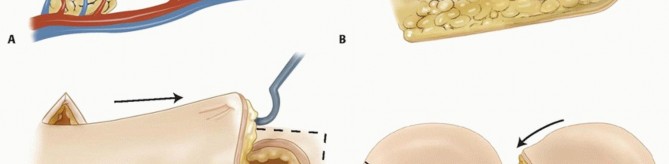
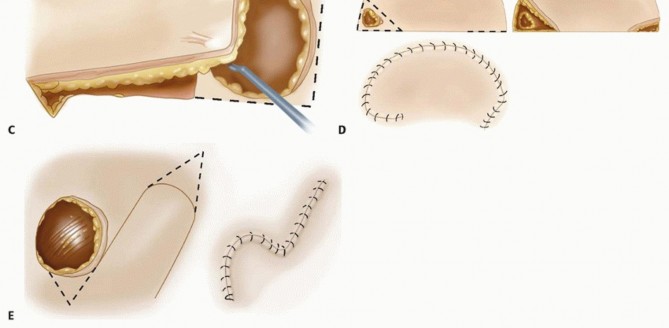
Aflapis a composite of tissue (ie, skin, fascia, muscle, bone, or combination) that is moved from its original location to another location in or on the body.5Several different types of flaps exist, defined by their blood supply.Random flaps(eg, Z-plasty, cross-finger flap) depend on preserving enough of the subcutaneous and dermal vascular plexus for flap survival. There are very few “random flaps.” Because of the extensive research on cutaneous circulation, the knowledge of vascular perforators, and understanding of angiosomes, this term is rarely used (FIG 1A). FIG 1 • A. Random flap. The distal skin flap is not supplied directly by the underlying vessels but relies on circulation from the dermal and subdermal plexus for nutrition. B. Axial flap. The entire flap is carried over an underlying vascular pedicle. C. Advancement flap. This is a direct tissue advancement. This figure also shows Burow triangles, which will decrease the dog-ears at the corners. D. Rotational flap. The flap rotates into the adjacent defect. The radius of the flap decreases with the rotation. A backcut can be used to extend the arc of coverage. E. Transposition flap. This flap is similar to a rotational flap, but the flap is moved across normal tissue to fill the defect. Axial flapsdepend on the blood supply from a single consistent (usually named) blood vessel; examples of this include the radial forearm flap and dorsal metacarpal artery flap (FIG 1B).P.1272Free flaps depend on the division and microsurgical anastomosis of the artery and vein to reestablish blood flow to the flap in a different location.Flaps also can be defined by how the tissue is moved.Advancement flapsare elevated and advanced in a linear direction away from the base of the flap (FIG 1C).Rotational flapsare elevated adjacent to the defect and re-inset within the same bed10 (FIG 1D).Transpositional flapsare elevated and moved across normal tissue to a new defect site (FIG 1E).Island flaps are elevated on their vascular pedicle and moved to a different location; mobility is limited by the pedicle length.Grafts are differentiated from flaps in that there is no native blood supply to the tissue. A skin graft survives initially by osmosis (imbibition) before it obtains vascular ingrowth (inosculation). This process works only for fairly thin tissue grafts.3,4
ANATOMY
A thorough understanding of the anatomy of the area injured and the donor area of the flap is necessary for safe elevation and insetting of these flaps.A full description of the anatomy of the forearm and hand is beyond the scope of this chapter, but the key points of the relevant anatomy will be addressed in the separate sections.The skin and soft tissue covering the forearm and hand vary by location, and this variation must be accounted for when considering coverage.The palm (volar surface) of the hand consists of very thick dermis and epidermis that is structurally anchored to the underlying tissues by numerous vertical fascial connections.The glabrous skin of the palm should be used to cover palmar defects, if possible.The dorsum of the hand has thin dermis and subcutaneous fat covering gliding extensor tendons.Coverage here should be as thin as possible to match the lost tissue.Fingertip sensation and durability should be given consideration when deciding on the type of coverage for fingertip injury.The forearm has thin soft tissue coverage.Proximally there is muscle, which often can be covered with a skin graft.Distally there is tendon on the palmar and dorsal surfaces. Trauma to the soft tissue often disrupts the paratenon and the exposed tendons will subsequently require flap coverage.
PATHOGENESIS
The mechanism of injury has a considerable effect on the need for flap coverage.Sharp injuries can usually be closed primarily without the need for flap coverage.Abrasive injuries commonly occur as a result of motor vehicle accidents. These usually involve one surface of the hand, and the extent of injury is usually relatively apparent. However, the level of contamination often is high, and extensive débridement of contaminated and devitalized tissue is necessary.Crush injuries can lead to necrosis of skin, tendon, bone, and muscle. The zone of injury often is large and can be underestimated on initial inspection.Other systemic injuries may delay treatment of extremity injuries. However, treatment for compartment syndrome and gross contamination must not be delayed any longer than necessary.
NATURAL HISTORY
The natural history of a wound depends greatly on the type of injury. The degree of original injury is the primary factor contributing to the prognosis for function of the hand.A large wound involving the bones, tendons, or joints often has a profound negative effect on future function of the hand.Early coverage can decrease total inflammation of the injured area and can limit the detrimental effect of the injury on the return to function.Many wounds will heal by second intention without the need for coverage. Secondary healing can lead to acceptable results in some locations but also may lead to very poor results in others. These factors must be taken into account when deciding type of coverage.Small wounds (<1 cm) on the fingertips, without exposed bone or tendon, will likely heal well on their own. This secondary healing often gives the strongest soft tissue coverage with the best sensibility and is the preferred treatment for most wounds of this type.If dorsal hand wounds secondarily heal or “granulate” over tendons, the tendons tend to scar, which limits gliding and impairs finger motion.Exposed bones, tendons, nerves, or vessels usually should be covered with a flap. Secondary healing or skin grafts will result in more scarring or unstable coverage.Skin grafts are best for wounds that have no exposure of tendons, nerves, or vessels. However, in certain circumstances, a skin graft can provide temporary coverage over most viable tissue. Skin grafts will not survive on bone or tendon when the periosteum or paratenon is absent.A well-performed flap will provide stable, durable coverage over any viable wound bed. This will allow earlier therapy and motion.
PATIENT HISTORY AND PHYSICAL FINDINGS
After a traumatic injury, a complete history and physical examination are performed.The mechanism of the injury is important. Contaminated or crush injuries often require more than one procedure for adequate irrigation and débridement.Any past medical history of diabetes, smoking, heart disease, peripheral vascular disease, or hypercoagulability will impact the healing of any flap, but none of these is an absolute contraindication to coverage procedures.Examination of the wound and extremity should be comprehensive:Assessment of vascular status Imaging for fractureMotor and sensory examination to evaluate for nerve, tendon, or muscle injury Examination for compartment syndrome in severe injuriesP.1273
IMAGING AND OTHER DIAGNOSTIC STUDIES
Radiographs of the hand should be obtained to evaluate for bony injury.Advanced imaging, such as computed tomography (CT) scan or magnetic resonance imaging (MRI), may be warranted for fracture pattern delineation, but these studies rarely are needed to assess the indications for flap coverage.Questionable blood flow or limb perfusion warrants further evaluation, such as angiography.Adequate blood flow to the extremity must be restored before considering flap coverage.
TYPES OF FLAPS
RADIAL FOREARM FLAP
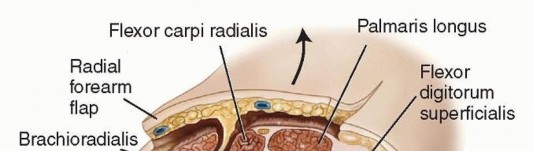
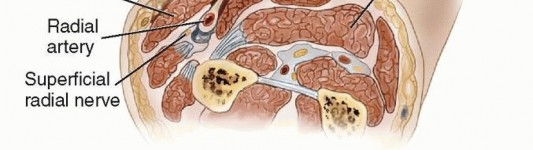
FIG 2 • Cross-section showing the relevant forearm anatomy for a radial forearm flap. The septum lies between the BR and FCR. The skin and subcutaneous tissue and fascia above the volar forearm musculature are elevated as a unit with the radial artery and septum with perforating vessels. There is a loose tissue septum between the FCR and BR. Within this septum, there are perforating branches of the radial artery to the skin that provide blood supply to the overlying skin. These are meticulously preserved to perfuse the flap (FIG 2).
GROIN FLAP
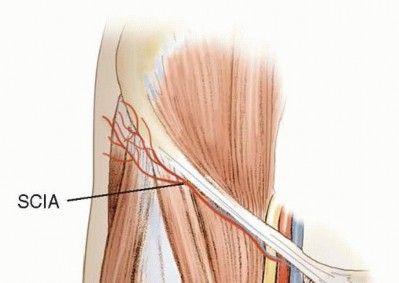
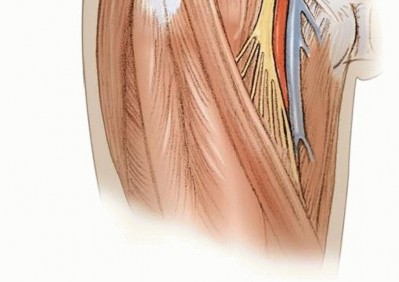
FIG 3 • Relevant groin flap anatomy. The SCIA arises from the femoral artery 3 cm distal to the inguinal ligament. It then travels laterally, anterior to the thigh musculature, parallel and inferior to the inguinal ligament.
KITE FLAP
The kite flap, or first dorsal metacarpal artery flap, is a reliable flap taken from the dorsum of the index finger over the proximal phalanx.Its most common use is for reconstruction of palmar thumb defects. Both soft tissue coverage and sensibility can be provided if the dorsal branches of the radial nerve are moved with the flap.1It also can be used for web space reconstruction or covering smaller defects on the dorsum of the hand or wrist. The flap can be 2 × 4 cm in size.Relevant anatomyThe radial artery travels through the anatomic “snuffbox,” then onto the dorsum of the thumb, before diving between the two heads of the first dorsal interosseous muscle. This artery has three main branches:The dorsal carpal archThe princeps pollicis artery to the thumb The first dorsal metacarpal arteryThe first dorsal metacarpal artery extends dorsally out along the surface of the first dorsal interosseous muscle to the dorsum on the index finger (FIG 4).The venous drainage of the flap is from the dorsal venous system of the finger.The radial nerve provides sensation to the dorsum of the radial hand and fingers distally. These small branches can be preserved and included with the flap, if desired.
POSTERIOR INTEROSSEOUS FLAP
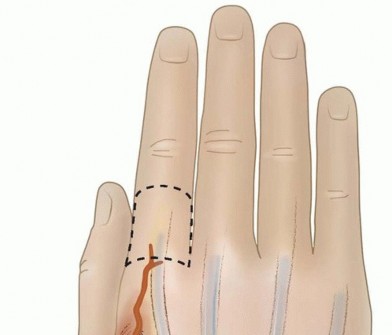
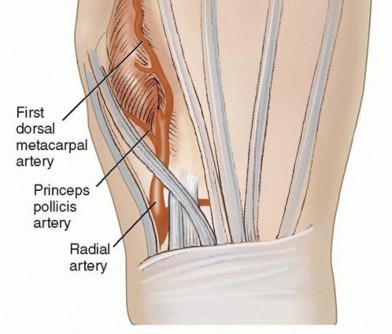
FIG 4 • Anatomy of the dorsal metacarpal artery.
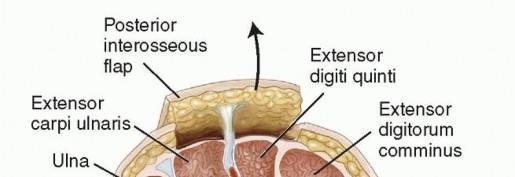
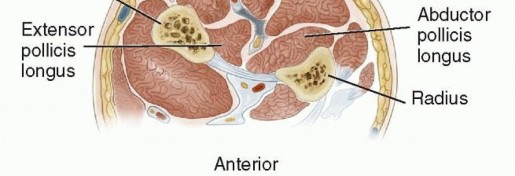
FIG 5 • The posterior interosseous flap is elevated with the posterior interosseous artery in a retrograde fashion. Perforating vessels are present within a septum that lies between the EDQ and ECU. The skin, subcutaneous tissue, fascia, and septum are all elevated with the artery. DisadvantagesTechnically difficult dissection due to the proximity of the posterior interosseous nerveThe anatomy does not always allow safe dissection of the flap, and the surgeon should have a plan for an alternate flap if necessary.Flap repair is contraindicated with wrist trauma due to disruption of the dorsal wrist vascular arcade.
Z-PLASTY
Although Z-plasty is not often used during immediate reconstruction, it is a useful adjunct for secondary reconstruction due to scar contracture.This method lengthens or redirects a scar by transposing two triangular flaps to bring normal tissue within a scarred area.A prerequisite is good tissue on either side of the area to be lengthened because this tissue is interposed in the place of the original scar.
NONOPERATIVE MANAGEMENT
As with all reconstructive procedures, if nonoperative management is possible, it should be considered and may be preferred.Small wounds often will heal secondarily with good results.Fingertip injuries that do not expose bone or tendon usually heal with good results and with good sensibility. These wounds should be débrided and cleaned, then dressed appropriately and allowed to heal over 2 to 3 weeks.Wounds on the distal forearm and hand often have exposure of tendon, bone, nerve, or vessel. Except in rare circumstances, these should all be covered with good tissue.Primary closure is the ideal, but with tissue loss, this may not be possible.Skin grafts provide good coverage for muscle or clean wounds of the hand but often do not offer the best coverage for future function of the hand.A skin graft will heal on bone or tendon if the periosteum or paratenon is intact, but this may create a thin, unstable wound. Skin grafting over tendons is prone to scarring and may decrease tendon excursion.Skin grafts will heal over nerves or vessels but can result in hypersensitivity with nerves or thin coverage over vessels increasing the chance of bleeding.In many cases, early flap closure with a good gliding surface (for tendon movement) may be better than delayed healing with increased scar tissue.
SURGICAL MANAGEMENT
The wound should be débrided back to viable tissue before it is covered.If there is gross contamination, the débridement often can be done in several stages to obtain a clean wound. The wound depth and size must be taken into consideration.
PREOPERATIVE PLANNING
If there is tendon or bone involvement of the injury site, the selected reconstruction should consider these factors.The affected area should be well perfused when the patient is brought to the operating room for flap coverage. Only rarely should flaps be performed on an emergent basis in an unhealthy patient.Flap coverage should be performed over a stable skeleton, and devitalized or contaminated tissue should not becovered.
POSITIONING
The arm usually is placed on an arm board at a 90-degree angle. The operating table is positioned to allow the surgeon and the assistant to sit on either side of the arm.This positioning gives excellent access to the palmar and dorsal forearm, arm, and hand.If a skin graft is considered, the ipsilateral groin or thigh is prepped to allow for full- or split-thickness grafting, respectively.Small full-thickness grafts can be obtained from the antecubital fossa, the ulnar forearm, or the ulnar side of the palm (for thick glabrous skin).
APPROACH
For all procedures, a padded tourniquet is used on the patient’s arm and inflated for the duration of the débridement of the wound and for flap elevation.At the end of the flap elevation, the tourniquet is released and bleeding controlled with bipolar electrocautery. Easily visible vessels are divided with clips or ties while the tourniquet is inflated.The wound site is always well débrided back to good tissue. Any foreign material is removed, and the wound irrigated with saline. Pulse lavage irrigation is used for heavily contaminated wounds.Careful handling of the tissue is imperative. Avoid handling the skin edges with pickups because the corners of flaps are particularly susceptible to trauma. Use retention sutures and skin hooks as much as possible.P.1276
TECHNIQUE
RADIAL FOREARM FLAP
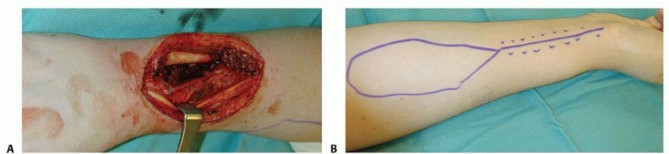
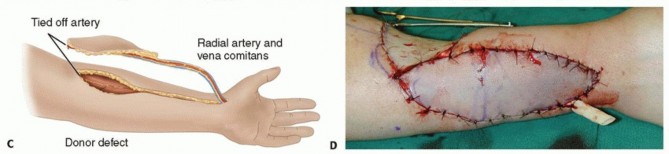
TECH FIG 1 • A. After resection of a recurrent sarcoma, this patient had a large dorsal defect with exposure of bone and tendon. B. The radial forearm flap is planned on the proximal forearm overlying the radial artery. Distal to the flap, the incision is drawn over the radial artery to extend the pedicle length. C. The flap is elevated from the proximal forearm, and once freed from its bed, the pedicle dissection is completed to the wrist. D. After the flap is elevated, it is inset in the excised wound. The flap defect is covered with a split-thickness skin graft.
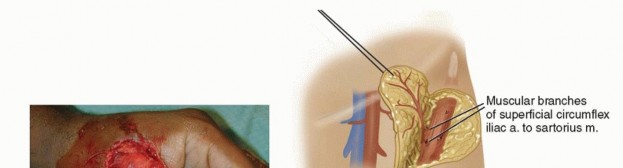
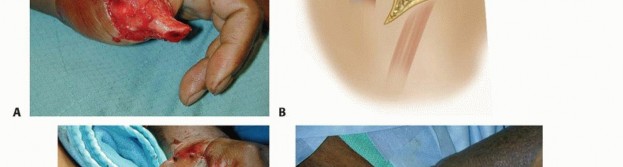
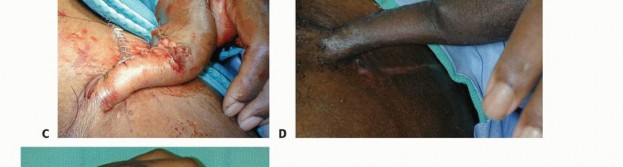
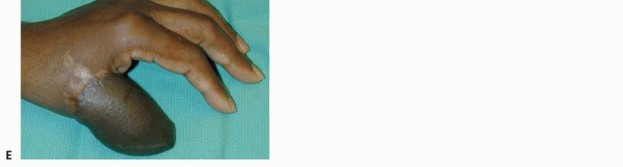
TECH FIG 2 • A. This patient had a traumatic amputation of his thumb, leaving reasonable bony length, but no soft tissue coverage. B. The groin flap is elevated from lateral to medial. Lateral to the sartorius, the superficial fascia is elevated with the flap. At the lateral border of the sartorius, the deep fascia is elevated and the perforating branches are ligated. Elevation stops at the medial border. C. After elevation and inset of the flap, the thumb is well covered. D. After 3 weeks, the flap had matured well in place. The pedicle is divided in the operating room. E. Three months after pedicle division, the flap is doing well. The preserved
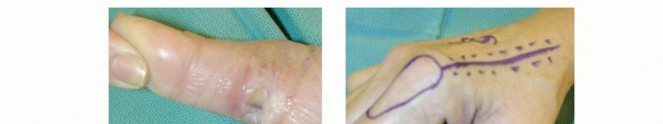
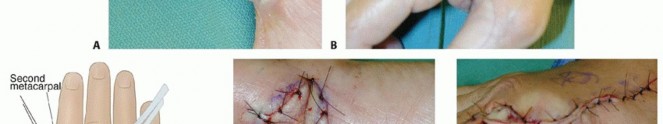
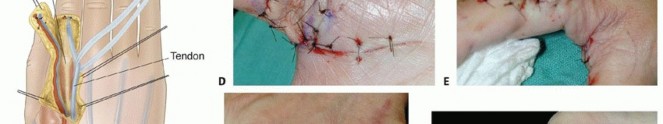
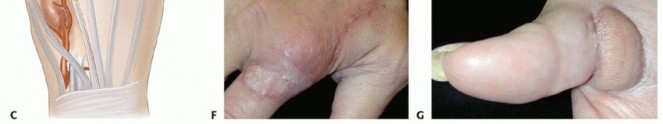
TECH FIG 3 • A. This wound of the volar thumb has exposed tendon and will not heal without a vascularized skin flap. B. The flap is planned on the dorsoradial aspect of the index finger. The proximal incision is for pedicle dissection. C. The first dorsal metacarpal artery flap is a vascularized skin flap from the dorsum of the index finger over the proximal phalanx. The dissection will give a flap that is good for small dorsal defects of the volar thumb. D. The flap is inset on the wound. E. The defect is closed. A small skin graft is needed to assist in closure. F. At 3 weeks postoperatively, the donor defect is healed. G. At 6 months postoperatively, the flap is well healed and allows for full tendon excursion.
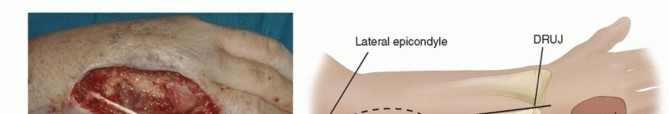
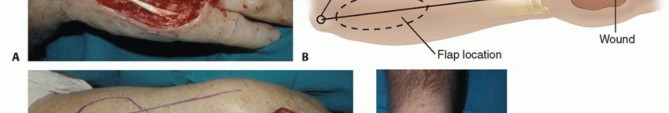
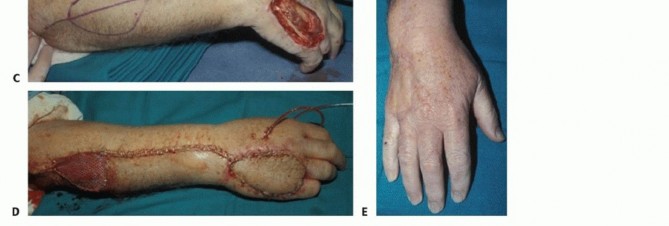
TECH FIG 4 • A. This traumatic wound has exposure of the extensor tendons. B,C. The posterior interosseous flap is located proximally over the posterior interosseous artery. The flap is centered over a line from the lateral epicondyle to the DRUJ. D. After elevation, the flap is inset on the wound. E. The wound is well healed.
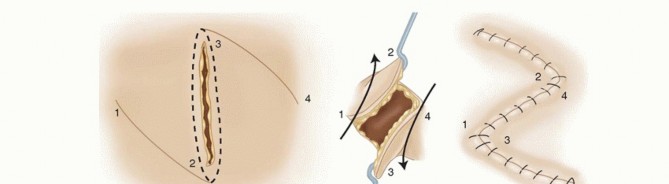
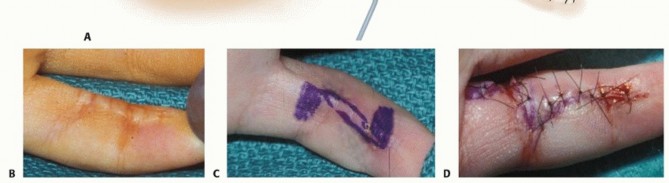
TECH FIG 5 • A. With a Z-plasty, two triangular flaps are elevated and transposed to interpose normal tissue into a contracted scar. The angle of the flaps usually is 60 degrees. B. This small finger has a contracted scar on the volar radial border. As it crosses both interphalangeal joints, the scar decreases the finger’s ability to extend fully. C. The Z-plasty is designed. D. After the flaps are elevated and transposed, the scar is lengthened, allowing full extension of the finger. The flaps created are then elevated at a subcutaneous level. Then, the two triangular flaps are transposed and sutured into place.Once the two flaps are elevated, they often “fall” into the correct position and are easily sutured in place.This usually gives an obvious and considerable lengthening immediately after flap transposition and insetting (TECH FIG 5D).PEARLS AND PITFALLS
|Indications ▪ A thorough physical examination must be completed before reconstruction of any defect.Flap ▪ Flap elevation must be done with care and precision, with attention to preservation elevation of the feeding blood vessels. The small vessels perfusing the flaps are vital to flapsurvival.|1. The choice of reconstruction is guided by the reconstructive ladder. Less invasive operations should be considered before more invasive procedures, but, ultimately, the expected outcome of the type of operation will direct the choice.2. Before any wound is covered, it must be clean, with no foreign material or dead tissue. Delaying reconstruction a few days until these goals are met is worthwhile.3. Frequent use of Doppler ultrasound facilitates vessel identification.Radial forearm flap5. The dissection is safest when the fascia is elevated first from the ulnar side. The septum rises obliquely under the BR.6. Preservation of the paired venae comitantes and the septal perforators is critical to survival of the flap.7. The reversed flap needs a patent palmar vascular arch.Groin flap ▪ The patient must be prepared to have the hand connected to the groin and must understand that a second operation is mandatory.1. This flap and the radial forearm flap are the workhorse flaps for large soft tissue flaps of the hand.First dorsal metacarpal artery flap8. Reliable coverage for volar thumb or small dorsal hand defects9. Sensation can also be preserved with this flap through branches of the superficial radial nerve.10. The dissection is somewhat complex due to the small caliber of the vessels.Posterior interosseous flap1. This flap is not typically a first choice.2. It is used when there is not a patent palmar arch (ie, when a radial forearm flap is contraindicated) and when there is a reason not to use a groin flap.
POSTOPERATIVE CARE
The postoperative care largely depends on the flap that has been used. For all of the operations, some of the same principles are followed.P.1281Postoperative antibiotics often are indicated because the wounds have been open for some time, have been contaminated, or have associated open fractures. The choice of antibiotic is individualized for each patient.The operative site usually is splinted to allow for healing of the flap without movement. If there is no bony injury, this is usually for 7 to 10 days, but the length of time may vary.The arm should be elevated above the level of the heart as much as possible. This will help decrease both edema within the flap and patient discomfort.The radial forearm flap should be monitored in the hospital for 2 or 3 days.When distally based, this flap may be susceptible to venous congestion.Care should be taken during the operation to meticulously preserve the vena comitans.If the cephalic vein has been preserved with the flap, it can be anastomosed to a vein in the field of the flap, but this is rarely necessary with the reversed flap.Care should be taken not to make the splint or dressing too tight.If a skin graft is placed during the operation, the bolster dressing is removed at 5 to 7 days and the skin graft is dressed daily with petrolatum-infused gauze or a nonadhering dressing until fully healed.Sutures around the flap are removed at 10 to 14 days.Early active motion of the fingers is encouraged to promote tendon gliding and lessen edema, unless contraindicated after coverage.Hand therapy is initiated in most patients at 1 to 2 weeks following surgery.
COMPLICATIONS
Short-term complications include those related to flap survival and healing of the wound.Long-term complications result from undesirable scarring relating to both the primary injury and the method of closure.Complete flap loss due to flap ischemia is uncommon. More often, a small area of the flap margin may not heal to the native skin margin due to inadequate débridement of the skin edges or rough handling of the flap skin.As the flaps heal, the function of the hand depends on subsequent scarring, which, if it occurs, leads to poor tendon gliding. Persistent tendon scarring requires later tenolysis. After 3 months, loss of the flap by inadvertent pedicle division is rare, but late flap loss has been reported.If scarring from the flap margin creates a contracture across a joint, a Z-plasty may be necessary.Overall, the complications related to flap closure are less than complications related to secondary healing. The long-term outcome will be better with flap coverage compared to secondary healing because secondary intention creates an abundance of scar tissue, which can impair function of the hand.
REFERENCES
- Foucher G, Baun JB. A new island flap transfer from the dorsum of the index to the thumb. Plast Reconstr Surg 1979;63:344-349.
- Foucher G, van Genechten N, Merle M, et al. A compound radial artery flap in hand surgery: an original modification of the Chinese forearm flap. Br J Plast Surg 1984;37:139-148.
- Mathes SJ, Nahai F. Introduction: a systematic approach. In: Mathes SJ, Nahai F, eds. Reconstructive Surgery: Principles, Anatomy, and Technique. New York: Churchill Livingstone, 1997:3-15.
- Pederson WC, Lister GD. Skin flaps. In: Green DP, Hotchkiss RN, Pederson WC, et al, eds. Green's Operative Hand Surgery, ed 5. Philadelphia: Elsevier Churchill Livingstone, 2005:1648-1703.
- Place MJ, Herber SC, Hardesty RA. Basic techniques and principles in plastic surgery. In: Aston SJ, Beasley RW, Thorne CH, eds. Grabb and Smith's Textbook of Plastic Surgery. Philadelphia: Lippincott Williams & Wilkins, 1997:13-16.
- Serafin D. The groin flap. In: Serafin D, ed. Atlas of Microsurgical Composite Tissue Transplantation. Philadelphia: WB Saunders, 1996:57-65.
- Sherif MM. First dorsal metacarpal artery flap in hand reconstruction: I. Anatomical study. J Hand Surg Am 1994;19:26-31.
- Smith PJ, Foley B, Mcgreggor IA, et al. The anatomic basis of the groin flap. Plast Reconstr Surg 1972;49:41-47.
- Song R, Gao Y, Song Y, et al. The forearm flap. Clin Plast Surg 1982;9:21-26.
- Spector JA, Levine JP. Cutaneous defects: flaps, grafts, and expansion. In: McCarthy JG, Galiano RD, Boutros SG, eds. Current Therapy in Plastic Surgery. Philadelphia: WB Saunders, 2006:11-21.
- Zancoli EA, Angrigiani C. Posterior interosseous island flap. J Hand Surg Br 1988;13:130-135.
