Acetabular Revision Cupcage: A Challenging Case Solved
Patient Presentation & History
A 68-year-old male presented with a two-year history of worsening left hip pain, instability, and a progressive leg length discrepancy. His past surgical history was significant for a left total hip arthroplasty (THA) performed 15 years prior for osteoarthritis, followed by a revision THA 5 years ago due to aseptic loosening of the acetabular component. The prior revision involved removal of the loose cup and implantation of a larger cementless acetabular component with supplemental screws and bulk femoral head allograft for a superior dome defect.
The patient describes the current pain as deep-seated, constant, and exacerbated by weight-bearing and activity, rating it 8/10 on the Visual Analog Scale (VAS). He requires a walker for ambulation and reports feeling a "clunking" sensation in his hip with certain movements, suggestive of instability. He denies fevers, chills, or night sweats. His medical comorbidities include well-controlled hypertension, type 2 diabetes mellitus managed with oral agents, and obesity (BMI 32 kg/m²). He is an ex-smoker with a 20 pack-year history, having quit 10 years ago. There is no history of prior hip infection.
The mechanism of current failure is insidious, characterized by progressive pain and functional decline, indicating likely mechanical failure and further bone loss around the previously revised acetabular component. Given the history of previous revision and associated bone grafting, a complex acetabular defect requiring significant reconstruction was anticipated.
Clinical Examination
Upon examination, the patient exhibited an antalgic gait, favoring the left lower extremity, with a positive Trendelenburg sign on the left side, indicative of abductor insufficiency or instability. A noticeable left lower extremity shortening of approximately 3 cm was measured clinically. Palpation revealed diffuse tenderness over the left hip joint, particularly along the greater trochanter and anterior capsule. No palpable masses or signs of active inflammation (rubor, calor) were noted.
Passive range of motion (ROM) of the left hip was severely restricted and painful: flexion to 60 degrees, abduction to 10 degrees, adduction to 0 degrees, internal rotation to 5 degrees, and external rotation to 15 degrees. Flexion, abduction, and external rotation were particularly limited and elicited significant pain. An audible and palpable clunk was noted during internal and external rotation, consistent with component instability.
Motor strength testing revealed 4/5 weakness in hip flexion, abduction, and extension on the left, compared to 5/5 on the contralateral side. Sensory examination was intact to light touch in the distribution of the femoral, obturator, and sciatic nerves. Distal pulses (femoral, popliteal, dorsalis pedis, posterior tibial) were all 2+ and symmetrical bilaterally, confirming intact vascular status. No signs of superficial infection were present around the previous surgical scar. The contralateral hip and knee examinations were unremarkable.
Imaging & Diagnostics
Radiographic Evaluation
Initial radiographic assessment commenced with a comprehensive series of standard hip and pelvis views:
*
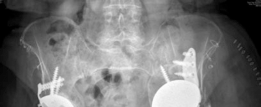
Anteroposterior (AP) pelvis:
Demonstrated significant superior and medial migration of the left acetabular component with evident periacetabular osteolysis. Lucency lines exceeding 2mm were observed at multiple interfaces, particularly zones 1 and 3 of DeLee and Charnley. There was evidence of prior bulk allograft incorporation, but with signs of partial resorption and failure to fully integrate into the host bone in areas of stress shielding. The femoral component appeared well-fixed in comparison.
*
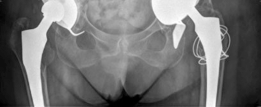
Lateral hip (true lateral or cross-table lateral):
Provided further insight into the anteroposterior extent of component migration and bone loss. The superior migration was particularly pronounced, leading to significant disruption of the acetabular tear drop and potential intrapelvic protrusion if not contained.
*
Judet views (Obturator oblique and Iliac oblique):
These specialized views were crucial for detailed assessment of the anterior and posterior columns and walls of the acetabulum. The obturator oblique view highlighted significant superior and posterior column erosion, while the iliac oblique view showed extensive destruction of the superior acetabular dome and a large contained defect superiorly, consistent with substantial Paprosky type IIIb bone loss, potentially extending to type IV.
Advanced Imaging
Given the complexity of the defect and the need for meticulous preoperative planning, a
computed tomography (CT) scan with 3D reconstructions
was indispensable.
*
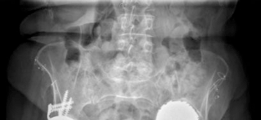
CT findings:
Confirmed severe Paprosky type IIIb acetabular bone loss, characterized by:
* Complete loss of the superior dome.
* Discontinuity of the anterior and posterior columns in segments.
* A large contained cavitary defect with an uncontained segmental defect superiorly.
* The medial wall was largely intact but severely thinned, with evidence of medial protrusion of the polyethylene liner.
* The femoral head allograft used in the previous revision showed patchy integration with areas of non-union and resorption, failing to provide adequate structural support.
* 3D reconstructions clearly delineated the extent of the superior and posterosuperior wall deficiencies, crucial for planning the appropriate cage and bone graft construct. They also helped to identify the remaining host bone available for screw fixation.
Laboratory Diagnostics
- Erythrocyte Sedimentation Rate (ESR) and C-Reactive Protein (CRP): Within normal limits, effectively ruling out acute periprosthetic joint infection (PJI).
- Hip aspiration: Not performed given the low suspicion for infection based on ESR/CRP and clinical presentation. However, in cases with elevated inflammatory markers or atypical presentation, aspiration with synovial fluid analysis (cell count, differential, culture) would be paramount.
Preoperative Templating
Extensive digital templating was performed utilizing the CT scan data and 3D models. The primary goal was to restore the anatomical hip center, which had migrated significantly superiorly and medially.
* Templating indicated the need for a reconstructive cage, specifically an anti-protrusio cage (e.g., Burch-Schneider type or similar custom design), capable of bypassing the large superior and medial defects and fixating to healthier bone in the ilium and ischium/pubis.
* The planned cage size and screw trajectories were determined to maximize purchase into two distinct points of the pelvis: the iliac wing superiorly and the ischial tuberosity/pubic ramus inferiorly.
* Concurrently, the volume and configuration of bulk allograft (e.g., morselized cancellous bone graft mixed with structural grafts) required to fill the cavitary and segmental defects were estimated.
* The final acetabular component (polyethylene liner) size and position within the cage were also templated to achieve appropriate stability and maximize articulation with the well-fixed femoral stem.
Differential Diagnosis
While the overarching diagnosis is a failed revision THA with severe acetabular bone loss, it's crucial to differentiate the primary mode of failure that led to such a complex defect, as this influences surgical planning and prognosis.
| Feature | Aseptic Loosening with Massive Bone Loss (Paprosky IIIb/IV) | Septic Loosening with Bone Destruction | Periprosthetic Acetabular Fracture (Type B3/C) with Contained Bone Defect |
|---|---|---|---|
| Clinical Presentation | Progressive, insidious pain; mechanical symptoms (clunking, instability); leg length discrepancy; no systemic signs of infection. | Acute or chronic pain; systemic signs (fever, chills, fatigue); local signs (redness, warmth, swelling, sinus tract); persistent drainage. | Acute onset of pain after trauma (fall); inability to bear weight; sometimes accompanied by instability symptoms. |
| Imaging Findings | Radiographic evidence of component migration, extensive periacetabular lucency, osteolysis, bone resorption. CT shows detailed morphology of severe contained/uncontained defects. | Similar radiographic findings to aseptic loosening, but often with more aggressive, irregular bone destruction, sometimes periosteal reaction. May show joint effusion. | Fracture lines visible on plain radiographs or CT. Loosening of the component (B3) or fracture extending into supporting columns (C) with associated bone loss. |
| Laboratory Markers | ESR and CRP typically normal or mildly elevated (non-specific). | Elevated ESR and CRP; elevated synovial fluid WBC count (>3,000 cells/µL) and PMN% (>80%); positive synovial fluid cultures. | ESR and CRP typically normal unless associated with infection or other inflammatory process. |
| Definitive Diagnosis | Intraoperative findings of a mobile, uningrown component, extensive granulomatous tissue (without infection), and gross bone loss. Histopathology negative for infection. | Positive intraoperative cultures (min 3-5 samples); positive histopathology for acute inflammation (>5 PMNs per HPF); purulent fluid. | Identification of a fracture line, often associated with a loose or malpositioned component and subsequent bone loss. |
| Typical Onset Post-Op | Years after primary or previous revision. | Variable: early (within weeks to months) or delayed (years). | Can occur at any time, often after minor trauma in osteoporotic patients. |
| Management Implications | Single-stage revision with extensive reconstruction and bone grafting (e.g., cupcage). | Two-stage revision (explantation, debridement, antibiotic spacer, then reimplantation) is standard; single-stage in select cases. | Open reduction and internal fixation (ORIF) and/or revision arthroplasty, often requiring cages or augments for bone defects. |
In this presented case, the patient's normal ESR/CRP, absence of systemic inflammatory signs, and insidious onset of symptoms strongly pointed towards aseptic loosening with massive bone loss (Paprosky IIIb/IV) as the primary etiology for the current hip failure.
Surgical Decision Making & Classification
The decision for surgical intervention was unequivocal, driven by the patient's severe pain, functional impairment, objective instability, and progressive nature of the component migration and bone loss. Non-operative management, including activity modification, analgesics, and assistive devices, had failed to alleviate symptoms and would not address the underlying mechanical instability or halt bone destruction.
Paprosky Classification of Acetabular Defects
The extensive preoperative imaging, particularly the CT scan with 3D reconstructions, allowed for precise classification of the acetabular bone defect according to the Paprosky classification system. This system is critical for guiding surgical strategy in revision total hip arthroplasty:
- Type I: Minimal bone loss, intact rim, minor cavitary defect.
-
Type II:
Varying degrees of cavitary or segmental bone loss with an intact or partially compromised rim.
- IIA: Intact rim, mild superior cavitary defect.
- IIB: Compromised rim, usually superior or superolateral.
- IIC: Medial wall defects.
-
Type III:
Extensive bone loss involving significant portions of the acetabular columns, often with an uncontained defect.
- IIIA: Defect primarily involves the superior dome with intact columns, providing at least 40% host bone contact.
- IIIB: Severe destruction of the superior dome with significant column involvement (usually more than 60% of superior host bone lost), often with ischial osteolysis. This was the primary classification for our patient's defect.
- Type IV: Pelvic discontinuity – complete separation of the acetabulum from the rest of the pelvis, often through the ilioischial line.
Based on the imaging findings (complete superior dome loss, severe involvement of anterior and posterior columns, large uncontained superior segmental defect, and evidence of significant periacetabular osteolysis extending towards the ischium), the defect was classified as Paprosky Type IIIB , bordering on Type IV due to the extensive column involvement and lack of reliable host bone in critical areas for standard cup fixation. The critical feature driving the decision for a cage was the uncontained segmental defect, the complete loss of the superior dome, and the inability to achieve primary stability and coverage with a hemispheric component or even augments alone.
Surgical Goals:
- Restoration of the Hip Center: Re-establishing the anatomical hip center for optimal biomechanics and joint reaction forces.
- Stable Fixation: Achieving durable, multi-point fixation to sound host bone, bypassing the deficient areas.
- Bone Stock Reconstruction: Utilizing bulk and morselized allograft to reconstitute lost bone, aiming for long-term biological integration.
- Implant Durability: Selecting an implant construct (cupcage) known for robust support in massive defects.
- Soft Tissue Tensioning: Optimizing abductor mechanism and overall hip stability.
Operative intervention via an acetabular revision cupcage reconstruction was chosen as the only viable option to address the massive bone loss, restore stability, alleviate pain, and improve functional outcomes for this patient.
Surgical Technique / Intervention
The surgery was performed under general anesthesia combined with epidural analgesia.
1. Patient Positioning and Surgical Approach:
The patient was positioned in the lateral decubitus position on a fracture table, allowing for optimal access to the acetabulum while providing stable lower extremity traction if needed. A standard Hardinge (direct lateral) approach was utilized, extending proximally to allow for adequate exposure of the iliac wing and distally for potential trochanteric osteotomy if necessary for femoral stem revision (which was not required in this case). The previous surgical scar was incised, and meticulous dissection through the scarred tissue was performed.
2. Explantation of Failed Components and Debridement:
The existing cementless acetabular component was found to be grossly loose and easily explanted. Significant amounts of polyethylene wear debris and granulomatous tissue were encountered, consistent with aseptic loosening and osteolysis. The previously grafted femoral head allograft fragments were non-integrated, loose, and partially resorbed, contributing to the structural instability. All wear debris, granulomatous tissue, and non-viable graft material were meticulously debrided to expose healthy bleeding host bone and define the true extent of the acetabular defect. This step is critical for infection prevention and future graft incorporation.
3. Assessment of Bone Defect and Host Bone Preparation:
The resulting acetabular defect was indeed Paprosky Type IIIB, confirming preoperative templating. There was a complete loss of the superior and postero-superior acetabular dome, with extensive cavitary and segmental defects. The anterior and posterior columns were severely attenuated. The medial wall was extremely thin but largely intact, precluding intrapelvic protrusion of the reconstruction plate itself, but requiring reinforcement.
The remaining host bone in the ilium, ischium, and pubis was prepared by curettage and burring to create a bleeding, receptive bed for bone graft.
4. Bone Grafting:
To address the extensive bone loss and facilitate long-term biological reconstruction, a combination of structural and morselized allograft was employed.
*
Structural Allograft:
A large femoral head allograft was shaped to fill the large superior segmental defect, providing initial structural support and helping to reconstitute the superior dome. This graft was initially held in place with temporary K-wires.
*
Morselized Cancellous Allograft:
Mixed with bone marrow aspirate (BMA) from the greater trochanter, this cancellous graft was packed tightly into all remaining cavitary defects to promote osteoconduction and eventual incorporation.
This image depicts a stage of the surgery where the defect has been debrided, and possibly initial bone grafting or reaming is underway, showing the exposed bone deficiency.
5. Cupcage Implantation (Burch-Schneider Cage):
A
Burch-Schneider anti-protrusio cage
(also known as a roof-reinforcement ring with an anti-protrusio flange) was selected due to its robust design and ability to bypass large defects, achieving fixation in healthier bone remote from the defect.
*
Cage Placement:
The cage was carefully positioned to restore the anatomical hip center, ensuring maximal contact with the superior structural allograft and the remaining host bone. The anti-protrusio flange was seated against the inferior margin of the acetabulum.
*
Fixation:
Multiple 3.5mm and 4.5mm cortical screws were then strategically inserted through the cage and into the host pelvis.
* Superiorly: Screws were directed into the iliac wing, gaining strong purchase.
* Inferiorly: Screws were directed into the ischium and superior pubic ramus, providing the crucial inferior buttress.
* Medially: Screws secured the cage to the thinned medial wall.
* All screws were meticulously placed under fluoroscopic guidance to ensure proper depth, direction, and to avoid neurovascular structures (sciatic nerve, obturator nerve/vessels). The cage was compressed against the bone graft and tightened incrementally until a rigid construct was achieved.
6. Acetabular Component Insertion:
Once the cage was rigidly fixed, a conventional cemented polyethylene acetabular liner was implanted within the cage. The liner was carefully cemented into the inner surface of the cage, ensuring optimal orientation (typically 40-45 degrees of abduction and 15-20 degrees of anteversion) for stability and wear characteristics. A trial reduction was performed to confirm stability through a full range of motion.
7. Femoral Stem Assessment and Reduction:
The existing femoral stem was assessed and found to be well-fixed, stable, and appropriately positioned. Therefore, no revision of the femoral component was deemed necessary. The femoral head was placed onto the stem trunnion, and the hip was reduced into the newly constructed acetabulum.
8. Final Stability Assessment and Closure:
A final assessment of hip stability was performed. Full range of motion was demonstrated without impingement or dislocation. Leg lengths were re-evaluated and corrected to within 0.5 cm of the contralateral side. The surgical wound was irrigated extensively, a drain was placed, and the deep fascia, abductor muscles, and subcutaneous layers were meticulously closed in layers.
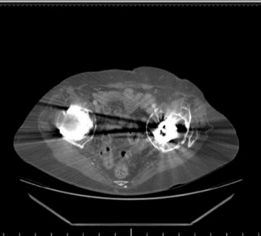
This image likely represents the immediate post-operative radiograph, clearly demonstrating the Burch-Schneider cage in situ, the cemented polyethylene liner, and the well-positioned femoral stem, with initial bone graft material visible.
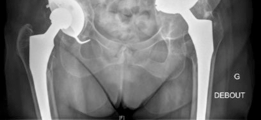
This image likely depicts a follow-up radiograph, showing continued good position of the components and signs of early bone graft incorporation, or potentially a different projection to confirm cage integrity.
Post-Operative Protocol & Rehabilitation
Immediate Post-Operative (Day 0-7):
- Pain Management: Multimodal analgesia including epidural/regional blocks, oral opioids, NSAIDs (if not contraindicated), and acetaminophen.
- DVT Prophylaxis: Low molecular weight heparin (LMWH) or direct oral anticoagulants (DOACs) initiated on post-operative day 1, continued for 4-6 weeks.
- Antibiotics: Prophylactic intravenous antibiotics for 24-48 hours.
- Drain Management: Surgical drain removed when output is minimal (<50 ml/24 hours).
- Weight-Bearing Status: Strict toe-touch weight-bearing (TTWB) on the operated limb for the first 6-8 weeks, to protect the bone graft and allow for initial cage osteointegration and graft healing. Crutches or a walker were utilized.
-
Physical Therapy:
- Early mobilization out of bed to a chair with assistance.
- Gentle, protected hip range of motion exercises within a safe arc (avoiding extremes of flexion, adduction, and internal rotation that could lead to impingement or dislocation).
- Ankle pumps, quadriceps sets, gluteal sets to maintain muscle tone and reduce swelling.
- Instruction on hip precautions (avoiding flexion >90 degrees, adduction past midline, internal rotation) to prevent dislocation.
Early Rehabilitation (Weeks 2-12):
-
Weight-Bearing Progression:
- Gradual progression to partial weight-bearing (PWB) at 6-8 weeks, contingent on radiographic evidence of early bone graft incorporation and stability.
- Progression to weight-bearing as tolerated (WBAT) by 12 weeks, as bone healing progresses.
-
Physical Therapy:
- Focus on increasing hip ROM, strengthening hip abductors, extensors, and flexors (e.g., resisted abduction, straight leg raises within precautions).
- Gait training with gradual reduction in assistive device use.
- Proprioceptive and balance exercises.
- Follow-up: Clinical and radiographic follow-up at 2 weeks, 6 weeks, and 3 months. Radiographs (AP pelvis, lateral hip) assessed for component position, signs of loosening, and bone graft integration.
Late Rehabilitation (Months 3-6 and Beyond):
- Weight-Bearing: Full weight-bearing without restrictions as tolerated.
-
Physical Therapy:
- Advanced strengthening program targeting hip and core musculature.
- Functional exercises: stairs, walking on uneven surfaces.
- Return to light recreational activities.
- Follow-up: Clinical and radiographic follow-up at 6 months, 1 year, and annually thereafter to monitor for late complications, osteointegration, and long-term implant survival.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls:
-
Meticulous Preoperative Planning:
- CT with 3D Reconstructions is Mandatory: Provides an invaluable roadmap for assessing the true extent of bone loss (cavity vs. segmental vs. column defects), remaining host bone for screw purchase, and templating cage size and screw trajectories. Judet views are also essential.
- Paprosky Classification: Accurately classify the defect (e.g., Paprosky Type IIIB/IV) to guide implant choice (cage vs. augments vs. custom).
- Contingency Planning: Always have backup options (e.g., different cage sizes, alternative bone graft sources) readily available.
-
Adequate Exposure:
- An extensile approach (e.g., modified Hardinge, extended trochanteric osteotomy) may be necessary to fully visualize and reconstruct complex defects. Be prepared to perform an osteotomy if required.
-
Thorough Debridement:
- Remove all soft tissue interposition, granulomatous tissue, cement remnants, and loose bone fragments to ensure a clean bed for graft incorporation and cage seating. Bleeding host bone is key.
-
Strategic Bone Grafting:
- Structural Grafts: Essential for restoring large segmental defects and the hip center (e.g., femoral head allograft).
- Morselized Grafts: Packed tightly into cavitary defects to promote long-term bone ingrowth and fill voids. Consider mixing with BMA or DBM for enhanced osteoinductivity.
-
Robust Cage Fixation:
- Bypass Fixation: The primary principle of cages is to bypass deficient bone and gain bicortical screw purchase into distant, healthy host bone (e.g., ilium superiorly, ischium/pubis inferiorly).
- Screw Length and Direction: Carefully select screw lengths and angles under fluoroscopic guidance to maximize purchase and avoid neurovascular injury (sciatic nerve, obturator nerve/vessels).
- Contour to the Pelvis: Ensure the cage contours well to the remaining host bone for maximal contact and load distribution.
-
Restoration of Hip Biomechanics:
- Restore the anatomical hip center to optimize abductor lever arm, minimize joint reaction forces, and reduce polyethylene wear.
- Achieve appropriate acetabular abduction and anteversion for stability and reduced impingement.
-
Multidisciplinary Approach:
- Involve infectious disease specialists if infection is suspected.
- Early engagement with physiotherapy for tailored rehabilitation.
Pitfalls:
- Inadequate Preoperative Assessment: Failing to fully appreciate the extent of bone loss or remaining host bone can lead to intraoperative surprises and compromise the reconstruction.
- Incomplete Debridement: Residual wear debris or granulomatous tissue can lead to recurrent osteolysis and early failure.
-
Poor Cage Seating/Fixation:
- Malpositioning: Improper cage placement can lead to malalignment, impingement, or inadequate fixation.
- Insufficient Screws/Poor Purchase: Inadequate number or suboptimal placement of screws can result in early cage migration or loosening.
- Over-contouring/Under-contouring: If the cage does not conform well to the bone, it can create stress risers or gaps.
- Neurovascular Injury: Aggressive reaming, drilling, or screw placement, especially in the inferior aspect of the acetabulum, carries a risk of injury to the sciatic nerve or obturator vessels/nerve. Careful fluoroscopic control is paramount.
- Infection: Despite meticulous technique, complex revision cases, especially those with extensive bone loss and allograft, have a higher risk of periprosthetic joint infection.
- Dislocation: Risk is increased due to altered soft tissue tension, abductor weakness, and potentially suboptimal component orientation in challenging reconstructions. Adherence to hip precautions is crucial.
- Non-Union/Resorption of Bone Graft: Inadequate graft incorporation can lead to continued bone loss, cage loosening, and eventual failure of the construct.
- Heterotopic Ossification: A common complication after extensive hip surgery, especially with bone grafting. Prophylaxis (NSAIDs or radiation) should be considered.
- Early Weight-Bearing: Premature weight-bearing can jeopardize bone graft incorporation and lead to failure of the cage fixation. Strict adherence to a protected weight-bearing protocol is critical.
- Chronic Pain: Even with successful reconstruction, patients may experience residual pain due to extensive soft tissue scarring, abductor insufficiency, or persistent nerve irritation.

