INTRODUCTION TO TIBIAL AND MALLEOLAR NONUNIONS
The management of nonunions in the lower extremity, particularly involving the medial malleolus and the tibial shaft, presents a complex biomechanical and biological challenge for the orthopedic surgeon. Because the tibia is the primary weight-bearing bone of the lower leg, its length, alignment, and rotational orientation are paramount to the proper kinematic function of both the knee and the ankle joints. Simply achieving osseous union is insufficient; the ultimate goal is the restoration of a functionally aligned, pain-free extremity.
Nonunions in these regions are broadly categorized by their biological capacity—specifically, whether they are hypervascular (hypertrophic) or avascular (atrophic/oligotrophic). The surgical technique selected must be meticulously tailored to address the specific deficiency, whether it be a lack of mechanical stability, a compromised biological envelope, or the presence of deep infection. This comprehensive guide details the operative techniques for addressing recalcitrant nonunions of the medial malleolus and the tibial shaft, ranging from fragment resection and sliding grafts to advanced internal fixation strategies.
MANAGEMENT OF MEDIAL MALLEOLUS NONUNIONS
Nonunion of the medial malleolus typically occurs due to inadequate initial reduction, soft tissue interposition (often the periosteum or the posterior tibial tendon), or premature weight-bearing. Depending on the size of the ununited fragment and its contribution to the stability of the ankle mortise, surgical intervention may involve either simple excision of the fragment or a reconstructive sliding bone graft.
Technique 1: Resection of the Distal Fragment of the Medial Malleolus
Resection is generally indicated for small, avascular distal fragments that do not compromise the structural integrity of the deltoid ligament complex or the stability of the ankle mortise. Attempting to internally fix a small, sclerotic fragment often leads to hardware prominence, fragmentation, and persistent pain.
Surgical Approach and Dissection
* Incision: Make a precise medial longitudinal incision, approximately 5 cm in length, centered over the medial malleolus.
* Deep Dissection: Divide the periosteum and the superficial fibers of the deltoid ligament strictly in line with the skin incision.
* Fragment Isolation: Employ a combination of sharp and blunt subperiosteal dissection to isolate the ununited distal fragment.
🔪 Surgical Warning: It is critical to avoid cutting the periosteum in a transverse direction. Furthermore, meticulous care must be taken to identify and protect the posterior tibial tendon, which lies immediately posterior to the medial malleolus in the retromalleolar groove. Iatrogenic injury to this tendon will result in significant postoperative morbidity and acquired flatfoot deformity.
- Resection: Once isolated, carefully excise the distal fragment of the malleolus. Ensure that the remaining bony bed is smooth and free of sharp prominences that could irritate the overlying soft tissues.
- Closure: Irrigate the wound thoroughly and close the periosteal sleeve, subcutaneous tissue, and skin in a layered fashion.
Postoperative Protocol
Following resection, the ankle is immobilized in a bulky Jones dressing or a short-leg splint to allow for soft tissue healing. Weight-bearing in a functional ankle corset or controlled ankle motion (CAM) boot can typically be initiated at 3 weeks postoperatively, advancing as tolerated by the patient's pain levels.
Technique 2: Sliding Bone Graft for Medial Malleolus Nonunion
When the ununited medial malleolar fragment is large and its absence would compromise the deltoid ligament's stabilizing effect on the talus, reconstruction is mandatory. A sliding bone graft provides both osteoconductive scaffolding and rigid mechanical stability across the nonunion site.
Surgical Approach and Preparation
* Incision: Expose the nonunion site through an anteromedial curved incision, approximately 10 cm in length, to provide adequate exposure of both the nonunion and the proximal tibial metaphysis.
* Periosteal Reflection: Carefully reflect the periosteum anteriorly and posteriorly.
* Nonunion Takedown: Excise all intervening fibrous tissue from the nonunion site. Freshen the ends of the proximal and distal fragments using a curette or a high-speed burr to expose bleeding, punctate cortical bone (the "paprika sign").
* Fragment Preservation: Crucially, remove no bone from the deeper, articular edges of the fragments to prevent narrowing of the ankle mortise or iatrogenic chondral injury.
* Distal Preparation: With a small curette, carefully hollow out the cancellous bed of the distal fragment to create a receptive socket for the advancing graft.
Graft Harvesting and Fixation
* Harvesting: Beginning immediately proximal to the nonunion site, use a cooled oscillating motor saw to harvest a cortical bone graft approximately 4 cm long and 1 cm wide from the anterior aspect of the proximal fragment.
* Displacement: Displace the harvested graft distally across the nonunion site, impacting it firmly into the previously hollowed-out distal fragment.
* Fixation: Hold the distal fragment in its exact anatomic position, restoring the articular congruity of the mortise. Transfix the proximal fragment, the sliding graft, and the distal fragment with a fully threaded cortical screw or a partially threaded cancellous lag screw to provide rigid interfragmentary compression.
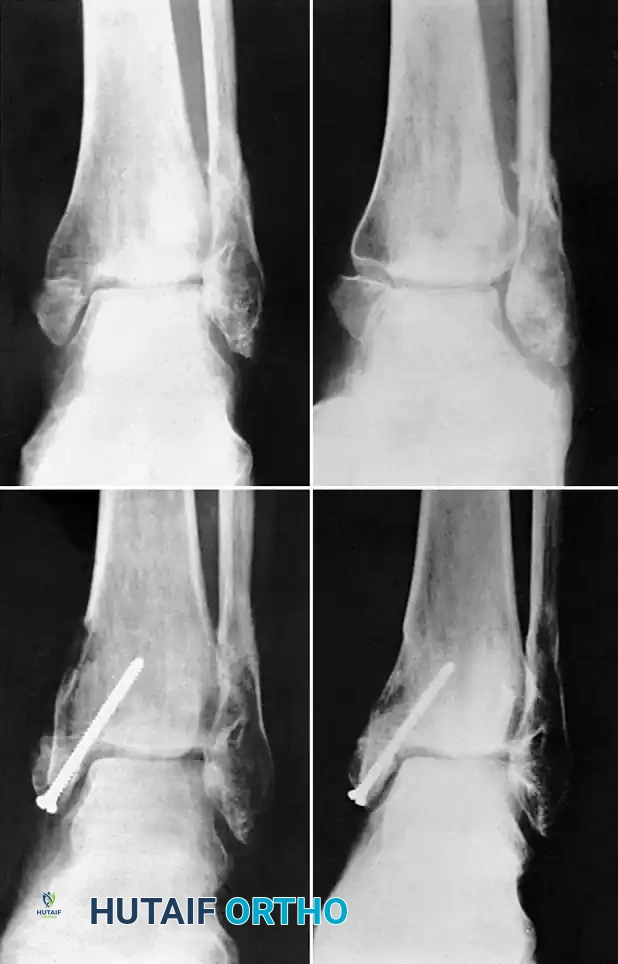
- Radiographic Confirmation: Intraoperative fluoroscopy is mandatory. Check the position of the graft, the trajectory and length of the screw, and the anatomic alignment of the malleolar fragments.
- Biological Augmentation: Place autologous cancellous bone chips (harvested locally or from the proximal tibia) around the graft site to enhance osteogenesis.
- Closure: Close the wound in standard layered fashion.
💡 Clinical Pearl: When using a motor saw to harvest the sliding graft, continuous saline irrigation is essential to prevent thermal necrosis of the bone, which would severely compromise the graft's incorporation and lead to failure of the procedure.
Postoperative Protocol
* Initial Phase (0-2 Weeks): A non-weight-bearing cast is applied from the toes to just distal to the knee.
* Intermediate Phase (2-4 Weeks): At 2 weeks, sutures are removed, and a walking cast or rigid CAM boot is applied. Partial weight-bearing is initiated.
* Late Phase (4+ Weeks): Full weight-bearing is permitted after 4 weeks. The cast or boot is entirely discarded when serial radiographs demonstrate definitive osseous healing of the nonunion, which typically occurs at 8 to 10 weeks postoperatively.
MANAGEMENT OF TIBIAL SHAFT NONUNIONS
Tibial shaft nonunions are notoriously challenging due to the bone's precarious subcutaneous anteromedial blood supply and its susceptibility to high-energy trauma. However, modern treatment methods have been highly successful in obtaining union.
Epidemiology and Union Rates
The literature demonstrates robust success rates depending on the modality chosen:
* Closed Bone Grafting: In hypertrophic aseptic nonunions, union rates of 72.1% to 87.8% have been reported.
* Internal Fixation: Rigid internal fixation yields an exceptional union rate of up to 98%.
* Electrical Stimulation: Non-invasive electrical stimulation has shown a 78.8% success rate in appropriately selected cases.
* Infected Nonunions: Historically difficult, infected nonunions have seen 100% union reported with staged closed bone grafting, 81% with open bone grafting, and 83% with combined bone grafting and internal fixation following eradication of infection.
Biological Classification: Hypervascular vs. Avascular
The surgical technique selected depends fundamentally on whether the nonunion is hypervascular (hypertrophic) or avascular (atrophic), as well as whether the alignment of the fragments is satisfactory.
Hypervascular (Hypertrophic) Nonunions
In hypervascular nonunions, the bone ends possess excellent biological capacity and are actively attempting to unite, as evidenced by abundant callus formation ("elephant foot" appearance). The failure to unite is purely mechanical—a lack of adequate stability.
* Treatment Strategy: Rigid internal fixation is usually all that is necessary. This can be achieved via a dynamic compression plate (DCP), a locked intramedullary (IM) nail, or a rigid external fixator.
* Grafting: Because the biological drive is already present, supplemental bone grafting is rarely necessary for hypervascular nonunions. The application of Perren's strain theory dictates that absolute or relative stability will allow the existing fibrocartilage to ossify.
Avascular (Atrophic or Oligotrophic) Nonunions
Avascular nonunions lack both mechanical stability and biological viability. The bone ends are typically sclerotic, tapered, and devoid of callus.
* Treatment Strategy: Rigid internal fixation must be supplemented by aggressive biological stimulation. This requires decortication of the sclerotic bone ends (shingling) to expose bleeding Haversian canals, combined with the application of autogenous bone grafting (cancellous or cortical).
* Fixation Modalities: Excellent results have been obtained using heavy-duty plates and screws or reamed intramedullary nailing, always in conjunction with robust bone grafting to provide osteoinductive and osteoconductive elements.
Surgical Strategies and Techniques
The Role of Fibulectomy
For many tibial nonunions, particularly those with an intact or healed fibula, the fibula acts as a mechanical strut that holds the tibial fragments apart, preventing compressive forces from stimulating bone healing. In these cases, a simple partial fibulectomy (resection of a 1-2 cm segment of the fibula) can allow the tibia to dynamically compress during weight-bearing, frequently resulting in union without the need for direct tibial intervention.
Extensive Procedures for Complex Nonunions
For nonunions complicated by significant bony defects, active infection, or severe angular deformity, more extensive procedures are necessary.
* Onlay Bone Grafting: In the past, most nonunions of the tibial shaft were treated with a massive cortical onlay bone graft. While this method rarely is used today due to the advent of locked plating and IM nailing, it remains a useful salvage technique for nonunions located in the extreme proximal or distal fourth of the tibia, or in cases involving severely sclerotic or avascular fragments where intramedullary devices are contraindicated.
* Management of Recalcitrant and Infected Cases: In recalcitrant cases, particularly those complicated by osteomyelitis, debate still exists on the optimal fracture care. The two-stage technique (often utilizing the Masquelet induced-membrane technique or Ilizarov bone transport) has become the gold standard. The first stage involves radical debridement of all infected and necrotic bone, placement of an antibiotic-impregnated cement spacer, and stabilization (usually via external fixation). The second stage, performed weeks later once infection is eradicated, involves removal of the spacer and massive autologous cancellous bone grafting into the biologically active induced membrane.
💡 Clinical Pearl: Because the tibia is a primary weight-bearing bone, simply obtaining union is not the sole objective. The surgeon must meticulously restore length, mechanical axis alignment, and rotation. Malunion in the coronal or sagittal plane will inevitably lead to altered kinematics and early-onset osteoarthritis of the knee and ankle joints.
Conclusion
The successful management of medial malleolus and tibial shaft nonunions demands a rigorous assessment of the mechanical and biological environment of the fracture site. Whether performing a delicate sliding graft for a malleolar defect or executing a complex reconstruction for an atrophic tibial shaft nonunion, the principles remain constant: eradicate infection, restore anatomic alignment, provide rigid mechanical stability, and optimize the biological envelope. By adhering to these evidence-based tenets, orthopedic surgeons can reliably achieve osseous union and restore full function to the lower extremity.
