Introduction to Congenital Digital Deformities
The management of congenital hand anomalies requires a profound understanding of embryology, genetic inheritance patterns, and the complex biomechanics of the developing pediatric hand. Among the most frequently encountered anomalies in pediatric orthopedic and hand surgery clinics are postaxial polydactyly and complex phalangeal deformities, such as the longitudinally bracketed epiphysis (delta phalanx) or macrodactyly.
Surgical intervention in these cases is rarely purely cosmetic; it is fundamentally reconstructive, aimed at establishing a stable, sensate, and biomechanically aligned digit that can grow proportionally with the child. This masterclass details the evidence-based evaluation and surgical management of postaxial polydactyly, followed by an exhaustive, step-by-step breakdown of the Peimer reduction osteotomy technique for complex phalangeal deformities.
Postaxial Polydactyly
Postaxial polydactyly, defined as the duplication of digits on the ulnar (postaxial) border of the hand, is one of the most common congenital hand differences. Its presentation ranges from a rudimentary soft-tissue tag to a fully developed, functional supernumerary ray.
Epidemiology and Genetic Pathophysiology
The incidence and genetic underpinnings of postaxial polydactyly vary significantly across different ethnic populations.
In populations of African descent, duplication of the small finger is the most common pattern of polydactyly. It occurs in approximately 1 in 300 live births, demonstrating a relative frequency of 8:1 compared to the duplication of other digits. The true epidemiological incidence is challenging to ascertain definitively, as historically, many rudimentary extra digits (Type 1) were ligated and removed in the neonatal nursery prior to formal documentation.
Genetically, postaxial polydactyly in Black populations is typically an isolated, autosomal dominant trait with marked penetrance. Conversely, the Type 1 pattern is often multifactorial, involving two genes with incomplete penetrance. Individuals presenting with more complex duplications (Types 2 or 3) may produce offspring with any of the three types, whereas those with Type 1 deformities generally produce children exclusively with Type 1 patterns.
Clinical Pearl: A typical Black child presenting with an isolated supernumerary postaxial digit has likely inherited it as an autosomal dominant trait and rarely requires an extensive syndromic workup. However, postaxial polydactyly in a Caucasian child is frequently associated with more serious systemic or chromosomal abnormalities, such as Ellis-van Creveld syndrome (chondroectodermal dysplasia) or McKusick-Kaufman syndrome. Thorough pediatric evaluation is mandatory in these cohorts.
The Stelling Classification System
Surgical decision-making is heavily guided by the morphological classification of the duplication. The Stelling classification categorizes postaxial polydactyly into three distinct types based on the degree of structural duplication:
- Type 1: Duplication of soft parts only. The supernumerary digit is a rudimentary soft-tissue tag devoid of osseous or cartilaginous structures, typically attached by a narrow pedicle.
- Type 2: Partial duplication of the digit, including osseous structures. The extra digit contains phalanges and articulates with the metacarpal head or a bifid metacarpal, often sharing a joint capsule and collateral ligament complex with the dominant small finger.
- Type 3: Complete duplication of the ray, including a fully formed supernumerary metacarpal. This is the rarest variant.
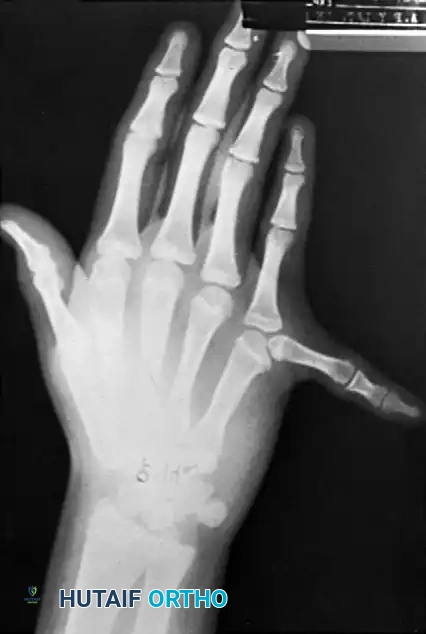
Clinical Evaluation and Surgical Timing
Infants with postaxial polydactyly may present with a well-formed extra digit along the ulnar border (Type 2) or a rudimentary tag (Type 1). In Type 2 and 3 duplications, both the dominant and supernumerary digits are usually hypoplastic to some degree. Angular deformity at the metacarpophalangeal (MCP) or interphalangeal (IP) joints may be present at birth or may manifest progressively during longitudinal growth due to tethering or asymmetric physeal development.
Surgical Warning: Surgical reconstruction should ideally be performed by the time the child is 6 months old. Delaying surgery beyond this window increases the risk of progressive angular deformity, joint contracture, and cortical remodeling that can permanently compromise the function of the retained digit.
Principles of Surgical Management
Management of Type 1 Deformities
Historically, the use of suture ligatures around the base of Type 1 postaxial duplications in the nursery was commonplace. This practice relies on ischemic necrosis and auto-amputation.
Pitfall: Nursery ligation is increasingly discouraged in modern practice. It carries a significant risk of incomplete necrosis, leaving a residual cartilaginous nubbin, or causing a painful traumatic neuroma at the base of the ulnar border of the hand. Formal surgical excision in the operating room under local or brief general anesthesia, with careful identification and proximal resection of the digital nerve, is the gold standard.
Management of Type 2 and Type 3 Deformities
For Type 2 and Type 3 duplications, simple amputation is insufficient. The procedure must be approached as a formal reconstruction.
1. Incision: An elliptical incision is made at the base of the duplicated digit.
2. Neuroma Prevention: The digital nerve to the duplicated digit is identified, tractioned distally, and transected sharply to allow it to retract deep into the soft tissues.
3. Ligamentous Reconstruction: In Type 2 duplications sharing a metacarpal head, the ulnar collateral ligament (UCL) and the abductor digiti minimi (ADM) insertion are often attached to the supernumerary digit. These must be meticulously detached with a periosteal sleeve and reattached to the base of the proximal phalanx of the retained small finger to prevent postoperative ulnar deviation and instability.
4. Articular Contouring: If the metacarpal head is bifid or excessively broad, a longitudinal shaving osteotomy of the articular cartilage and subchondral bone is performed to narrow the joint and allow for concentric reduction of the retained phalanx.
Reduction Osteotomy for Complex Phalangeal Deformities
Complex phalangeal deformities, such as macrodactyly or the presence of a longitudinally bracketed epiphysis (delta phalanx), require sophisticated osseous remodeling. The delta phalanx is characterized by a C-shaped epiphysis that brackets the diaphysis longitudinally, tethering growth on one side and resulting in a progressive, severe clinodactyly.
The Peimer reduction osteotomy is a highly effective, albeit technically demanding, procedure designed to excise the abnormal epiphyseal bracket, shorten the digit, and realign the mechanical axis.
Preoperative Planning
Meticulous preoperative planning is the cornerstone of a successful reduction osteotomy.
* Radiographic Templating: Obtain high-quality, true anteroposterior (AP) and lateral radiographs of the affected digit.
* Surgical Mapping: Mark the preoperative radiographs or create a detailed sketch of the phalangeal and epiphyseal deformities. Calculate the exact location of the osteotomies and the precise wedge of bone to be resected to achieve a neutral mechanical axis.
* Skin Marking: Prior to exsanguination, use a sterile skin-marking pen to delineate the curved dorsal incision. This incision must often include the nail and germinal matrix that are slated for removal to appropriately narrow the digit.
Step-by-Step Surgical Technique (Peimer)
The following technique details the reduction osteotomy for a complex middle phalangeal deformity with a C-shaped epiphysis.
- Incision and Exposure:
- Exsanguinate the limb and inflate the pneumatic tourniquet.
- Make a curved dorsal incision through the nail, matrix, and skin, carrying the dissection down to the level of the paratenon.
- Elevate full-thickness skin flaps to preserve the delicate vascularity of the dorsal skin.
- Tendon Management:
- Expose the middle and distal phalanges by identifying the extensor mechanism.
- Divide and reflect the extensor tendon (e.g., extensor pollicis longus in the thumb, or the terminal extensor slip in the fingers) just proximal to its insertion on the base of the distal phalanx. Tag the tendon with a non-absorbable suture for later repair.
- Distal Phalanx Contouring:
- Utilize a #15 scalpel or fine bone-cutting forceps to narrow the distal phalanx to the desired width, matching the planned dimensions of the reconstructed digit.
- Surgical Warning: Exercise extreme caution to avoid fragmenting the tuft of the distal phalanx, which serves as the critical anchor for the digital pulp.
- First Osteotomy (Epiphyseal Excision):
- Expose the distal phalangeal epiphysis with a precise longitudinal cut.
- Using a scalpel (in young children with largely cartilaginous structures) or a fine oscillating saw, make a transverse osteotomy to completely excise the abnormal epiphysis.
- Second Osteotomy (Middle Phalanx):
- Make a second transverse osteotomy in the middle of the middle phalanx, distal to the normal horizontal portion of the epiphysis.
- Clinical Pearl: To ensure the second osteotomy is perfectly parallel with the proximal interphalangeal (PIP) joint, insert a thin hypodermic needle (e.g., 25-gauge) into the PIP joint space. Use this needle as a visual guide to determine the true joint line and parallel your osteotomy cut accordingly.
- Excision of the Bracketed Epiphysis:
- With the second transverse osteotomy complete, expose the abnormal longitudinal portion of the C-shaped middle phalangeal epiphysis.
- Completely excise the distal portion of the middle phalanx along with the abnormal bracketed epiphysis.
- Critical Step: Perform this excision meticulously to avoid inadvertently cutting or compromising the collateral ligaments of the adjacent joints, which would lead to catastrophic postoperative instability.
- Realignment and Fixation:
- After removing the pathological bone fragments, place the remaining osseous structures in a closing-wedge position. This maneuver simultaneously realigns the angular deformity and shortens the digit to a physiological length.
- If necessary, use fine bone-cutting forceps or a small diamond rasp to contour the bony surfaces for maximum cortical contact.
- Align the bone ends and achieve osteosynthesis using one or two smooth 0.028-inch or 0.035-inch Kirschner wires (K-wires).
- If the retained interphalangeal joint exhibits instability, advance the K-wire across the joint to transfix it temporarily.
- Intraoperative Verification:
- Obtain intraoperative fluoroscopy (C-arm) to check the adequacy of the osseous resection, the correction of the mechanical axis, and the precise placement of the K-wires.
- Closure and Tendon Repair:
- Shorten the previously tagged extensor tendon to match the new skeletal length. Repair it using fine, non-absorbable horizontal mattress sutures (e.g., 4-0 or 5-0 Ethibond).
- Deflate the tourniquet, achieve meticulous hemostasis using bipolar electrocautery, and excise any redundant skin flaps to ensure a contoured, tension-free closure.
- Close the skin with interrupted fine sutures.
- Cut and bend the K-wires outside the skin, leaving them protruding to facilitate easy removal in the clinic.
Management of Central Polysyndactyly
While postaxial polydactyly is the most common, central polysyndactyly (duplication of the index, long, or ring fingers, often hidden within a complex syndactyly web) presents a unique reconstructive challenge.
In the central polysyndactyly pattern, the osseous anatomy is highly variable, often involving cross-bones, synostoses, and shared flexor/extensor mechanisms. Surgical options include complex syndactyly reconstruction combined with the excision of the most hypoplastic extra digit, or, in severe cases where functional reconstruction of four fingers is impossible, the creation of a highly functional three-fingered hand.
The complexity of these deformities requires astute surgical judgment, advanced preoperative imaging (often including MRI or 3D CT reconstructions), and a highly individualized approach. As a general rule, as many normal-appearing, independently functioning fingers as possible should be reconstructed. Amputation of a stiff, functionless, or severely deviated digit may be performed as a secondary procedure later in childhood if it interferes with global hand mechanics.
Postoperative Protocol and Rehabilitation
The success of a reduction osteotomy or a complex polydactyly reconstruction relies heavily on strict adherence to postoperative protocols.
- Immobilization: Immediately postoperatively, apply a bulky, non-compressive soft dressing reinforced with a long-arm plaster opponens gauntlet splint that extends above the elbow. Extending the splint above the elbow is critical in pediatric patients to prevent the child from slipping out of the cast.
- Wound Care: If necessary, the splint can be bivalved or removed for wound inspection during the first 2 to 3 weeks after surgery. However, the hand must be kept strictly and continuously splinted for a total of 6 to 8 weeks to protect the osteotomies and ligamentous reconstructions.
- Hardware Removal: The protruding Kirschner wires are removed in the outpatient clinic after 6 to 8 weeks, contingent upon radiographic evidence of bridging callus and clinical stability.
- Rehabilitation: Splinting is usually discontinued after pin removal. While infants and toddlers naturally integrate the reconstructed digit into play, formal physical therapy and occupational therapy may be highly beneficial in older patients to regain full active range of motion, overcome tendon adhesions, and optimize grip strength.
Complications and Avoidance
- Nonunion/Delayed Union: Minimized by ensuring broad cancellous bone contact at the osteotomy site and avoiding thermal necrosis during saw cuts.
- Recurrent Deformity: Often results from incomplete excision of the C-shaped epiphysis in delta phalanx cases. Complete resection of the longitudinal bracket is mandatory.
- Joint Instability: Caused by failure to reconstruct the collateral ligaments (especially the UCL in postaxial polydactyly) or iatrogenic injury during epiphyseal resection.
- Nail Bed Deformities: Careful management of the germinal matrix during the dorsal incision and narrowing of the distal phalanx is required to prevent split or hooked nails.
📚 Medical References
- reduction osteotomy as a treatment for refractory trochanteric bursitis, J Bone Joint Surg 85B:199, 2003.
- Haggart GE: Synovial cysts of the popliteal space: clinical signifi cance and treatment, Ann Surg 118:438, 1943.
- Harper MC, Schaberg JE, Allen WC: Primary iliopsoas bursography in the diagnosis of disorders of the hip, Clin Orthop Relat Res 221:238, 1987.
- Hench PK, Reid RT, Reames PM: Dissecting popliteal cysts simulating thrombophlebitis, Ann Intern Med 64:1259, 1966.
- Hendryson IE: Bursitis in the region of the fi bular collateral ligament, J Bone Joint Surg 28:446, 1946.
- Hitchcock HH, Bechtol CD: Painful shoulder: observations on the role of the tendon of the long head of the biceps brachii in its causation, J Bone Joint Surg 30A:263, 1948.
- Jerosch J, Strauss JM, Schmiel S: Arthroscopic treatment of calcifi c tendonitis of the shoulder, J Shoulder Elbow Surg 7:30, 1998.
- Johnston CA, Wiley JP, Lindsay DM, et al: Iliopsoas bursitis and tendonitis: a review, Sports Med 25:271, 1998.
- Kerlan RK, Glousman RE: Tibial collateral ligament bursitis, Am J Sports Med 16:344, 1988.
- Ko SH, Ahn JH: Popliteal cystoscopic excisional débridement and removal of capsular fold of valvular mechanism of large recurrent popliteal cyst, Arthroscopy 20:37, 2004.
- Krasny C, Enenkel M, Aigner N, et al: Ultrasound-guided needling combined with shock-wave therapy for the treatment of calcifying tendonitis of the shoulder, J Bone Joint Surg 87B:501, 2005.
- Krome J, deAraujo W, Webb LX:
