Patient Presentation & History
We present the case of a 78-year-old female who sustained a periprosthetic femoral fracture following a low-energy fall from standing height at her home. She presented to the emergency department with acute onset of severe left hip pain and an inability to bear weight on the affected limb.
Her medical history includes:
* Total hip arthroplasty (THA) on the left side approximately 10 years prior for severe osteoarthritis, involving a cementless femoral stem and acetabular component.
* Osteoporosis, for which she was on weekly alendronate.
* Controlled hypertension.
* Type 2 Diabetes Mellitus, managed with oral hypoglycemics.
* Prior surgical history: Appendectomy, cholecystectomy, right knee arthroscopy.
* No known drug allergies.
* Social history: Non-smoker, occasional alcohol use, lives independently with minimal assistance. She was functionally active prior to the injury, ambulating with a single-point cane for long distances.
On initial assessment, the patient was hemodynamically stable. She reported immediate, excruciating pain in her left hip and thigh, exacerbated by any attempt at movement. There was no history of prodromal pain, mechanical symptoms, or recent fevers/chills that might suggest a periprosthetic infection or aseptic loosening prior to the fall.
Clinical Examination
Upon examination in the emergency department, the following findings were noted:
Inspection
- The left lower extremity was visibly shortened, abducted, and externally rotated compared to the contralateral limb.
- Significant swelling and ecchymosis were observed around the left greater trochanter and extending distally along the proximal thigh.
- No open wounds or signs of skin compromise were present. The incision from the prior THA appeared well-healed, without erythema or discharge.
Palpation
- Marked tenderness was elicited over the lateral aspect of the left proximal femur and greater trochanter.
- Palpable crepitus was noted with gentle manipulation of the limb, consistent with a bony fracture.
- The pelvis was stable to stress.
Range of Motion
- Active and passive range of motion of the left hip was severely limited due to pain. Any attempt at movement caused significant distress.
- Knee and ankle range of motion were grossly intact, but the patient was unable to actively move the hip.
Neurological and Vascular Assessment
- Neurological: Distal neurovascular status was intact. Sensation to light touch was normal in the distribution of the femoral, obturator, sciatic, peroneal, and tibial nerves. Motor function of ankle dorsiflexion, plantarflexion, great toe extension, and knee extension/flexion was preserved, though limited by pain proximally. Specifically, the sciatic nerve function (dorsiflexion and plantarflexion of the ankle) was assessed and found to be intact.
- Vascular: Capillary refill in the toes was brisk (<2 seconds). Dorsalis pedis and posterior tibial pulses were strong and palpable bilaterally. No signs of distal ischemia were present.
Imaging & Diagnostics
X-ray Findings
Initial radiographs included an AP pelvis view, and dedicated AP and lateral views of the left hip and entire femur, ensuring visualization of the femoral stem and distal femur.
The radiographs revealed:
* A spiral fracture of the proximal femur originating distal to the lesser trochanter and extending distally for approximately 8 cm, surrounding the previously implanted femoral stem.
* The fracture involved cortical breach and significant displacement.
* Crucially, there were signs suggestive of femoral stem loosening. Specifically, complete lucency was observed at the bone-implant interface, along with evidence of subsidence of the femoral component compared to prior radiographs (obtained one year prior, available for comparison). There was also evidence of gross motion of the stem within the canal when comparing AP and lateral views with the fracture reduced, though this was difficult to ascertain precisely given the fracture displacement.
* The acetabular component appeared well-fixed without overt signs of loosening or migration.
* There was no evidence of prior stress shielding or significant cortical thinning that might suggest an impending atypical femoral fracture, though her bisphosphonate use was noted.
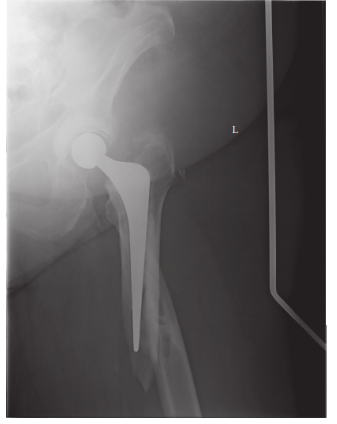
Initial AP hip X-ray demonstrating the periprosthetic femoral fracture and signs of stem loosening:

CT Scan Indications
A Computed Tomography (CT) scan of the left hip and femur was obtained to further characterize the fracture pattern, more accurately assess femoral stem stability, and evaluate the extent of bone loss.
*
CT Findings:
The CT scan confirmed a comminuted spiral fracture of the proximal femur, extending from the lesser trochanter distally. It unequivocally demonstrated circumferential lucency around the femoral stem, confirming aseptic loosening of the implant. The cortex was intact proximally but significantly disrupted at the fracture site. Minimal bone loss was noted at the fracture site itself, but the surrounding osteoporotic bone quality was evident. No significant trochanteric or calcar defects were observed. Three-dimensional reconstructions were invaluable for appreciating the complex fracture morphology and planning reduction strategies.
Templating
Pre-operative templating was performed meticulously using calibrated radiographs and CT reconstructions.
* The existing femoral stem was identified as a cementless, tapered, proximally-coated component.
* Templating focused on selecting a revision femoral stem that would bypass the distal extent of the fracture by at least two cortical diameters, ideally achieving diaphyseal fixation in healthy bone.
* Potential revision stem options (e.g., modular, fluted, tapered, or cylindrical stems) were considered based on available bone stock and planned bypass length.
* Plate selection (e.g., locking compression plate, LISS plate) and cerclage wire/cable placement were also templated to ensure adequate implant availability and construct length for stable fixation. The length of the plate would need to extend proximally to the greater trochanter and distally well beyond the fracture, overlapping with the diaphyseal engagement of the new stem.
Differential Diagnosis
The primary differential diagnosis for an acute periprosthetic fracture revolves around the stability of the existing femoral stem, bone quality, and the location of the fracture relative to the implant.
| Feature | Vancouver B1 (Stable Stem) | Vancouver B2 (Loose Stem) | Vancouver B3 (Bone Loss & Loose Stem) | Atypical Femoral Fracture (AFF) |
|---|---|---|---|---|
| Pathophysiology | Traumatic fracture around a well-fixed stem | Traumatic fracture around an aseptically loose stem | Traumatic fracture around a loose stem with significant bone loss/poor host bone | Stress fracture, often spontaneous or low-energy trauma, associated with bisphosphonate use |
| Stem Stability | Stable (radiographically and clinically) | Loose (radiographic lucency, subsidence, clinical symptoms prior to fracture) | Loose with substantial bone defect or poor quality bone | N/A (fracture in native bone) |
| Fracture Location | Around or distal to the stem tip | Around or distal to the stem tip | Around or distal to the stem tip | Subtrochanteric or diaphyseal region, often transverse with medial spike |
| Radiographic Signs | Fracture lines clearly separate from stem-bone interface. No stem migration/lucency. | Clear signs of stem loosening (e.g., circumferential lucency >2mm, subsidence, endosteal erosion). | Loose stem with segmental bone loss, cavitation, or severe osteoporosis. | Transverse fracture, often with a unicortical "beak" or "flare," localized periosteal thickening. |
| Treatment Strategy | Open Reduction Internal Fixation (ORIF) with plates and cerclage wires. Stem not revised. | Revision Arthroplasty (Stem) with ORIF (long stem, plates, cerclage wires). | Revision Arthroplasty (Stem) with significant bone grafting (allograft/autograft), tumor prosthesis, or custom implant. | ORIF with intramedullary nail (e.g., cephalo-medullary nail). Stopping bisphosphonates. |
| Prognosis | Generally good, focused on fracture union. | More complex, higher complication rates (nonunion, re-loosening). | Poorer prognosis due to reconstructive challenges, high failure rates. | Good with appropriate surgical stabilization and cessation of bisphosphonates. |
Based on the clinical and radiographic findings, particularly the unequivocal signs of femoral stem loosening and displacement of the fracture around the stem, the patient's injury was classified as a Vancouver B2 periprosthetic femoral fracture . This classification is critical as it dictates the primary surgical strategy.
Surgical Decision Making & Classification
Operative vs. Non-Operative Management
For periprosthetic femoral fractures, operative management is almost universally indicated for displaced fractures due to:
1.
Instability:
Most periprosthetic fractures involving the prosthesis are inherently unstable.
2.
Pain Management:
Operative fixation allows for stable constructs that facilitate pain control and early mobilization.
3.
Restoration of Function:
Non-operative management typically involves prolonged immobilization and non-weight-bearing, which is poorly tolerated in elderly patients and carries significant risks (DVT, pneumonia, deconditioning, pressure ulcers).
4.
Implant Status:
When the implant is loose (as in a B2 fracture), non-operative management is contraindicated as the source of instability (the loose stem) remains unaddressed, precluding any hope of satisfactory fracture healing or functional recovery.
Non-operative management is reserved for highly selected cases, such as very stable, non-displaced fractures (e.g., some Vancouver A fractures), or in non-ambulatory patients with severe comorbidities where the risks of surgery outweigh the benefits. This patient's fracture was displaced and involved a loose stem, mandating surgical intervention.
Classification (Vancouver B2)
The Vancouver Classification system is the most widely accepted system for periprosthetic femoral fractures. It categorizes fractures based on:
*
Location:
(A: trochanteric, B: around or just below stem, C: well below stem)
*
Stem Stability:
(1: stable, 2: loose)
*
Bone Stock:
(3: poor quality/significant loss)
Our patient's fracture, a spiral pattern extending around a demonstrably loose femoral stem, directly fits the criteria for a Vancouver B2 fracture .
The implications of a Vancouver B2 classification are profound:
*
Mandatory Stem Revision:
Unlike Vancouver B1 fractures where the stable stem allows for ORIF of the fracture alone, a Vancouver B2 fracture necessitates
revision of the loose femoral stem
in addition to fracture fixation. The loose stem is the primary pathology contributing to instability and must be addressed.
*
Reconstructive Challenges:
Stem revision adds significant complexity to the surgery, requiring careful removal of the existing stem, reaming the canal, and implanting a new, longer stem that achieves stable diaphyseal fixation.
*
Bone Stock Assessment:
While not B3, the underlying osteoporotic bone quality is a significant consideration, influencing implant choice and fixation strength.
Surgical Planning
Our surgical plan focused on addressing both the fracture and the loose femoral stem:
1.
Femoral Stem Revision:
The primary goal was to remove the existing loose stem atraumatically, preserving as much existing bone stock as possible. This would be followed by reaming and insertion of a new, longer, cementless revision stem designed to bypass the fracture site by at least two cortical diameters, achieving stable diaphyseal fixation.
2.
Fracture Fixation:
Once the new stem was securely placed, the fracture fragments would be anatomically reduced and fixed using a combination of cerclage cables and a locking plate. The plate would span the fracture and overlap with the diaphyseal engagement zone of the new stem.
3.
Ancillary Techniques:
Consideration of bone grafting (autograft or allograft) for any significant bone defects created during stem removal or present at the fracture site.
Surgical Technique / Intervention
The patient was optimized pre-operatively, including medical clearance, Type & Screen/Crossmatch for blood products, and discussion of the surgical plan with the family.
Patient Positioning
The patient was placed in the lateral decubitus position on a fracture table, allowing for full access to the lateral aspect of the femur and controlled manipulation of the limb for reduction maneuvers. Adequate padding was used to protect pressure points.
Approach
The previous posterolateral approach incision was utilized and extended proximally and distally to ensure adequate exposure of the greater trochanter and the entire fracture extent, as well as the anticipated distal extent of the new revision stem. Dissection was carried down through scarred tissues. The abductor musculature was released from the greater trochanter, allowing for anterior subluxation of the hip joint if needed for exposure. The sciatic nerve was identified posteriorly and protected throughout the procedure.
Exposure and Fracture Reduction
- The fracture hematoma was evacuated, and the fracture fragments were carefully debrided.
- The fracture pattern (spiral) was identified. Initial provisional reduction of the main fracture fragments was achieved using broad periosteal elevators and bone clamps, taking care to minimize further soft tissue stripping.
- The previous femoral stem was identified. Given its looseness, its removal was anticipated to be relatively straightforward.
Femoral Stem Removal
- The existing femoral head was removed.
- The loose femoral stem was carefully disimpacted using specific extractors. Due to the circumferential lucency and subsidence, the stem was removed without requiring extended trochanteric osteotomy or creation of a cortical window. Care was taken to avoid further iatrogenic fracture during extraction. Any remaining cement mantle (if present in the original implant, which was cementless in this case) or fibrous tissue was meticulously debrided from the femoral canal.
- The femoral canal was sequentially reamed to prepare for the new revision stem, taking care to maintain the central axis and avoid cortical perforation.
New Stem Insertion
- Templating Review: The pre-operative templating was re-confirmed. A modular, tapered, fluted, cementless revision stem (e.g., a Wagner cone or similar diaphyseal engaging stem) was selected. This type of stem offers good rotational stability and allows for length adjustment.
- Trial Reduction & Stem Sizing: Trial components were used to determine the optimal stem size and length, ensuring stable diaphyseal fixation and bypass of the fracture by at least 2 cortical diameters distal to the most distal fracture line. The goal was 6-8 cm of bypass.
- Definitive Stem Implantation: The definitive revision stem was implanted with firm press-fit. Rotational alignment was carefully controlled. Once seated, the stem demonstrated excellent stability within the femoral canal. The femoral head was then re-attached, and the hip was reduced. Stability was assessed dynamically.
Fracture Fixation
- Cerclage Wires/Cables: With the new stem in place, the fracture fragments were anatomically reduced around the new stem. Multiple non-absorbable cerclage cables (e.g., Dall-Miles cables) were placed circumferentially around the femur, securing the fracture fragments to the new stem and achieving provisional compression. Typically, 3-4 cables were used proximally and distally to the main fracture line. Monocortical wires/cables were used where the plate would be placed.
-
Locking Plate Application:
A long, pre-contoured locking compression plate (LCP) was chosen, ensuring sufficient length to span the fracture and overlap with the new stem. The plate was provisionally secured to the lateral aspect of the femur.
- Proximal Fixation: The plate was fixed proximally to the greater trochanteric region with locking screws, avoiding compromise of the new stem.
- Distal Fixation: Distal to the fracture, locking screws were inserted bicortically into the healthy femoral shaft, ensuring adequate fixation into the bone distal to the new stem's diaphyseal engagement.
- Fracture Zone Fixation: Around the revision stem and across the fracture, monocortical locking screws were utilized where the screws might impinge on the stem. The locking plate construct provides angular stability and maintains reduction while promoting fracture healing. A gap between the plate and the bone can sometimes be left to allow for callus formation (biological plating principles).
- Final Assessment: The hip joint was taken through a full range of motion under fluoroscopic guidance to confirm stability of the implant and fracture fixation, ensure no impingement, and rule out dislocation.
Closure
A drain was placed deep to the vastus lateralis. The abductor musculature was reattached to the greater trochanter if detached. Fascia, subcutaneous layers, and skin were closed in layers.
Post-Operative Protocol & Rehabilitation
The post-operative protocol was designed to protect the construct, promote fracture healing, and facilitate early mobilization while considering the patient's age and comorbidities.
Immediate Post-Operative Period (Days 0-7)
- Pain Management: Multimodal analgesia including regional blocks, oral opioids, and NSAIDs (if not contraindicated).
- DVT Prophylaxis: Low molecular weight heparin (LMWH) or fondaparinux initiated immediately and continued for 4-6 weeks. Mechanical prophylaxis (TED stockings, SCDs) also utilized.
- Antibiotics: Prophylactic antibiotics continued for 24-48 hours.
- Neurovascular Monitoring: Regular checks of distal neurovascular status.
- Wound Care: Daily wound inspections. Drain removal when output is minimal (<30-50 mL/24h).
- Mobility: Out of bed on post-operative Day 1, with assistance. Education on hip precautions (avoiding extreme flexion, adduction, internal rotation to prevent dislocation) was reinforced.
- Weight-Bearing Status: Protected weight-bearing (toe-touch or 20-lb partial weight-bearing) on the operated limb was permitted immediately, using a walker or crutches. This was crucial to allow early mobilization and prevent deconditioning, but strict adherence to weight-bearing limits was emphasized to prevent stress on the healing fracture and new construct.
Early Rehabilitation (Weeks 1-6)
-
Physiotherapy:
Daily sessions focused on:
- Gradual increase in hip range of motion within hip precautions.
- Gentle isometric strengthening of hip abductors, adductors, and extensors.
- Ankle pump exercises, knee flexion/extension.
- Bed mobility, transfer training, and gait training with protected weight-bearing.
- Occupational Therapy: Assessment for adaptive equipment and home safety recommendations.
- Radiographic Follow-up: Initial post-operative radiographs to confirm implant position and fracture reduction. Follow-up radiographs at 4-6 weeks to assess early callus formation and exclude hardware failure or stem subsidence.
Mid-Term Rehabilitation (Weeks 6-12)
- Progression of Weight-Bearing: Based on clinical progress, pain levels, and radiographic evidence of early fracture healing (e.g., bridging callus, stable construct), weight-bearing was gradually advanced to partial weight-bearing (50%) and then weight-bearing as tolerated . This decision was individualized.
- Strengthening: Progressive resistive exercises for hip musculature, core strengthening.
- Gait Training: Progression from walker to crutches, then a single point cane as stability and strength improve. Emphasis on normalized gait pattern.
- Bisphosphonate Management: Re-evaluation of bisphosphonate use. Often, a "holiday" from bisphosphonates is considered to facilitate bone healing, with re-initiation considered based on bone density and fracture risk after union.
Long-Term Rehabilitation (Months 3-12+)
- Full Weight-Bearing: Typically achieved by 3-6 months post-operatively, once definitive radiographic union is evident.
- Advanced Strengthening: Return to functional activities, balance training, and sport-specific rehabilitation if applicable.
- Radiographic Follow-up: Every 3-6 months for the first year, then annually, to monitor for late complications such as nonunion, malunion, implant loosening, or heterotopic ossification.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls
- Pre-operative Templating is Paramount: Essential for predicting stem size, length, and potential challenges. Have a contingency plan (e.g., different revision stems, allograft options).
- Adequate Exposure: Utilize prior incisions, but extend sufficiently to visualize the entire fracture and the full length of the femoral canal needed for revision. Be prepared for extensive scar tissue.
- Preservation of Bone Stock: During stem removal, meticulous technique is vital to avoid iatrogenic fracture or further bone loss, especially in osteoporotic bone. Flexible osteotomes, burrs, and careful extraction are key.
- Achieve Diaphyseal Fixation: For B2/B3 fractures, the revision stem must bypass the fracture by at least two cortical diameters (ideally 6-8 cm) to achieve stable fixation in healthy bone distal to the fracture.
- Stable Fracture Fixation: Employ a robust construct: multiple cerclage cables for provisional reduction and compression, combined with a long locking plate for angular stability.
- Monocortical Screws Around Stem: When placing screws into the plate adjacent to the revision stem, use monocortical locking screws to avoid hitting the stem and creating stress risers.
- Biological Plating Principles: Consider a gap between the plate and the bone (indirect reduction) to promote periosteal healing, especially in comminuted fractures.
- Neurovascular Protection: The sciatic nerve is particularly vulnerable in posterolateral approaches, especially with extensive soft tissue dissection and limb manipulation. Proactive identification and protection are critical.
- Multidisciplinary Approach: Collaboration with arthroplasty surgeons, geriatricians (for medical optimization), and rehabilitation specialists improves outcomes.
- Realistic Expectations & Patient Education: Counsel patients and families about the prolonged recovery, potential for complications, and the protected weight-bearing protocol.
Pitfalls
- Inadequate Pre-operative Planning: Lack of appropriate implant sizes or types can lead to intraoperative delays or suboptimal fixation.
- Inadequate Exposure: Rushing or insufficient exposure leads to poor visualization, increased risk of iatrogenic injury, and suboptimal reduction/fixation.
- Iatrogenic Fracture During Stem Removal: Aggressive or uncontrolled stem removal can extend the fracture or create new fractures, significantly complicating the revision.
- Ignoring Stem Instability (Treating B2 as B1): This is a critical error. Attempting to fix a fracture around a loose stem without revising the stem invariably leads to construct failure, nonunion, and early reoperation.
- Insufficient Bypass of Fracture: If the new revision stem does not extend far enough distally beyond the fracture, it will not achieve stable diaphyseal fixation, leading to early failure or re-fracture.
- Neurovascular Injury: Direct trauma or stretch injury to the sciatic nerve can result in devastating functional deficits.
- Infection: Any periprosthetic procedure carries a risk of infection, which is often challenging to treat and can necessitate further complex surgery. Strict aseptic technique is paramount.
- Nonunion/Malunion: Can occur due to poor biology, inadequate fixation, or non-compliance with post-operative instructions.
- Hardware Failure: Plate or screw breakage can occur due to excessive stress on the construct before biologic union is achieved.
- Dislocation: Inadequate soft tissue repair, improper component alignment, or non-compliance with hip precautions can lead to post-operative dislocation.
- Overly Aggressive Weight-Bearing: Premature or uncontrolled weight-bearing can compromise the healing fracture and lead to hardware failure or loss of reduction. Strict adherence to protocols is vital.
Clinical & Radiographic Imaging