ACUTE DISLOCATIONS OF THE PATELLA
Acute dislocation of the patella is a significant traumatic event that primarily affects young, active patients. The patella almost exclusively dislocates laterally, driven by the inherent biomechanical vectors of the extensor mechanism, the Q-angle, and the lateral pull of the vastus lateralis. Understanding the pathoanatomy, particularly the disruption of the medial soft-tissue restraints, is paramount for both conservative and operative management.
While the majority of primary acute dislocations can be managed successfully with closed reduction and structured rehabilitation, the high incidence of associated osteochondral shear fractures and profound medial patellofemoral ligament (MPFL) tearing necessitates a high index of suspicion and rigorous diagnostic evaluation.
Pathoanatomy and Biomechanics
The stability of the patellofemoral joint relies on a complex interplay between active muscular restraints, passive ligamentous structures, and the osseous geometry of the trochlear groove.
The Medial Patellofemoral Ligament (MPFL) is the primary passive restraint to lateral patellar translation, providing approximately 50% to 60% of the restraining force from 0 to 30 degrees of knee flexion. During an acute lateral dislocation, the MPFL is almost universally injured.
An extensive MRI study by Balcarek et al. elucidated the specific injury patterns associated with acute lateral patellar dislocations. They identified either a complete or partial tear of the MPFL in the vast majority of patients (98%). The anatomical distribution of these tears is highly variable but follows distinct patterns:
* Femoral Origin: Most frequently affected (50%).
* Midsubstance: Accounted for 10% of isolated tears.
* Patellofemoral Origin (Insertion): Accounted for 10% of isolated tears.
* Multifocal Injuries: More than one site of injury was found in 22% of patients, indicating massive retinacular failure.
Furthermore, subgroup analyses have demonstrated that underlying anatomical variants strongly predispose individuals to dislocation. Specifically, patellar height (patella alta) and trochlear facet asymmetry (trochlear dysplasia) are significantly different on MRI in patients who experience acute dislocations compared to healthy controls. Patella alta delays the engagement of the patella into the stabilizing bony confines of the trochlea during early flexion, leaving the joint entirely dependent on the MPFL.
Clinical Pearl: The classic "kissing contusion" pattern seen on MRI—bone bruising on the medial patellar facet and the lateral femoral condyle—is the hallmark of a transient lateral patellar dislocation and subsequent relocation. This impaction is the primary mechanism for osteochondral shear fractures.
Clinical Evaluation and Closed Reduction
Patients typically present with an acutely painful, swollen knee, often locked in a flexed position with a visible lateral deformity. If the patella has not spontaneously reduced prior to arrival, urgent closed reduction is indicated.
Closed Reduction Technique
Acute dislocations of the patella are usually managed initially by closed methods. The reduction maneuver is straightforward and relies on relaxing the extensor mechanism:
1. Positioning: The patient is placed supine. Adequate analgesia or intra-articular local anesthetic may be administered if muscle spasm is severe.
2. Maneuver: The clinician gently and progressively extends the flexed knee.
3. Reduction: Simultaneous, gentle, medially directed pressure is applied to the lateral margin of the patella. As the knee approaches full extension, the patella typically clunks back into the trochlear groove.
Post-Reduction Immobilization
Following successful reduction, the limb is immobilized in a knee immobilizer or a hinged knee brace locked in extension for 3 to 6 weeks.
* Rationale: Immobilization allows the torn medial structures (MPFL and medial retinaculum) to heal in an anatomically reduced position.
* Early Motion: After the initial strict immobilization phase, controlled range of motion (ROM) is begun. This is critical to prevent arthrofibrosis and to promote the formation of strong, organized collagen along the lines of mechanical stress.
Radiographic Evaluation and Advanced Imaging
Following reduction, a comprehensive radiographic series is mandatory to confirm concentric reduction and, more importantly, to rule out osteochondral fractures.
Standard Radiographs
A standard trauma knee series should include:
* Anteroposterior (AP) View: Evaluates overall alignment and may show large osteochondral fragments or avulsion fractures from the medial patella (MPFL insertion).
* Lateral View: Essential for assessing patellar height (Insall-Salvati ratio) and identifying trochlear dysplasia (crossing sign, supratrochlear spur).
* Sunrise / Merchant View: Evaluates patellofemoral congruence, tilt, and the presence of intra-articular fragments within the dependent portions of the joint.
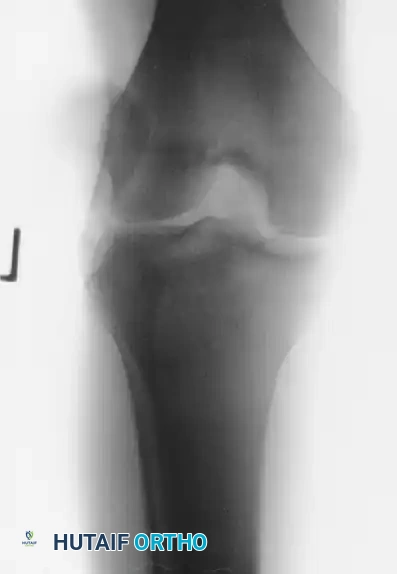
FIGURE 60-1A: Anteroposterior (AP) view demonstrating an acute lateral patellar dislocation prior to reduction.

FIGURE 60-1B: Sunrise view clearly illustrating the lateral displacement of the patella relative to the trochlear groove, highlighting the vulnerability of the medial patellar facet to shear injury against the lateral femoral condyle.
Magnetic Resonance Imaging (MRI)
Radiographs must be evaluated carefully to ensure that no osteochondral fragments are displaced within the joint. However, plain films have low sensitivity for purely cartilaginous or small osteochondral shear injuries.
If a hemarthrosis is present, MRI is strictly warranted. A tense hemarthrosis in the setting of a patellar dislocation is highly predictive of intra-articular pathology.
* One landmark study demonstrated articular cartilage injury in 94% of patients following acute dislocation.
* 72% of these patients had a distinct osteochondral or chondral fracture.
* 23% exhibited patellar microfractures.
MRI not only identifies these fragments but also maps the exact location of the MPFL tear, which is critical if surgical repair or reconstruction is being considered.
Treatment Algorithm for Acute Primary Patellar Dislocation
The management of acute primary patellar dislocation is dictated by the presence of intra-articular damage and the patient's anatomical risk factors. The following algorithm guides evidence-based decision-making:
- Initial Event: Acute Primary Patellar Dislocation.
- First Step: Obtain standard X-rays (AP, Lateral, Sunrise).
- Assess for Hemarthrosis:
- If Hemarthrosis is Present: Proceed immediately to MRI to evaluate the articular surfaces and the integrity of the medial restraints.
- If Hemarthrosis is Absent: Proceed to conservative management. Immobilization in extension for 3–6 weeks, followed by structured knee rehabilitation.
- Evaluate MRI for Displaced Osteochondral Fragment:
- If Fragment is Present (Yes): Surgical intervention is indicated. Proceed to Operative fixation of the fragment (or removal if non-fixable) +/- MPFL repair or reconstruction.
- If Fragment is Absent (No): Proceed to conservative management (Immobilization in extension for 3–6 weeks followed by knee rehabilitation).
- Long-Term Follow-Up:
- Conduct history and physical examinations at future follow-up visits to evaluate for the development of loose body symptoms or recurrent instability.
- If symptoms of a loose body develop: Re-evaluate with imaging and consider arthroscopic removal of the fragment.
- If no symptoms develop: Continue knee rehabilitation and allow return to activity as appropriate.
Surgical Warning: Failure to identify and address a large osteochondral fragment from the weight-bearing surface of the lateral femoral condyle or the patella can lead to rapid, early-onset patellofemoral osteoarthritis and chronic mechanical symptoms.
🔪 Surgical Technique 60-1: Open Exploration and Repair
When surgical intervention is mandated—typically due to a displaced osteochondral fragment, a massive avulsion of the vastus medialis obliquus (VMO), or an irreducible dislocation (often due to interposition of the medial retinaculum)—a formal open exploration and repair is performed.
While modern techniques often utilize arthroscopically assisted methods for fragment fixation, the classic open approach remains a foundational technique for comprehensive joint exploration and direct anatomical repair of the medial structures.
1. Preoperative Preparation and Positioning
- Anesthesia: General or regional anesthesia is administered. A femoral nerve block or adductor canal block is highly recommended for postoperative pain control.
- Positioning: The patient is placed supine on the operating table. A tourniquet is applied to the proximal thigh. The operative leg is prepped and draped free to allow full range of motion during the procedure.
- Examination Under Anesthesia (EUA): Prior to incision, assess patellar tracking, the degree of lateral translation (in quadrants), and the competence of the medial restraints compared to the contralateral knee.
2. Surgical Approach
- Incision: Make a longitudinal medial parapatellar incision. The incision should be centered over the medial border of the patella, extending from the distal pole of the patella to the VMO insertion.
- Dissection: Deepen the incision through the subcutaneous tissues to expose the medial patellar retinaculum and the joint capsule.
- Exploration of the Tear: Carefully explore the tear in the medial patellar retinaculum. The tear may be located at the patellar insertion, midsubstance, or at the femoral origin (Schöttle's point). Note the extent of the disruption, particularly if it extends proximally into the vastus medialis muscle belly.
3. Intra-articular Exploration and Fragment Management
- Arthrotomy: Extend the traumatic rent in the retinaculum to perform a formal medial arthrotomy.
- Irrigation: Copiously irrigate the knee joint with sterile saline to evacuate the hemarthrosis and wash out small cartilaginous debris.
- Joint Inspection: Make a thorough, systematic search for any loose fragments or intra-articular damage. Inspect the medial patellar facet and the lateral femoral condyle specifically for osteochondral shear fractures.
- Fragment Management:
- Removal: If the osteochondral fragments are small, purely cartilaginous, highly comminuted, or located in non-weight-bearing zones, they should be excised. Debride the donor crater to stable, vertical margins.
- Fixation: If a fragment is large (>1-1.5 cm) and contains sufficient subchondral bone to hold hardware, it should be anatomically reduced and fixed. Fixation can be achieved using headless compression screws, bioabsorbable pins, or chondral darts. Ensure all hardware is countersunk below the articular cartilage surface to prevent opposing surface abrasion.
4. Retinacular and VMO Repair
- Anatomical Reduction: Once the joint is cleared of debris and fractures are addressed, focus on the medial soft-tissue repair.
- Repairing the Disruption: Repair any disruption in the vastus medialis muscle belly or in the medial patellar retinaculum.
- If the MPFL is avulsed from the patella, it can be repaired using suture anchors placed along the medial articular margin of the upper two-thirds of the patella.
- If the tear is midsubstance, a direct end-to-end repair using heavy non-absorbable or slowly absorbing sutures (e.g., #2 FiberWire or PDS) is performed using a Krackow or locking whipstitch technique.
- If the avulsion is from the femoral origin, suture anchors at the anatomic footprint (between the adductor tubercle and medial epicondyle) are utilized.
- Tensioning: The repair must be tensioned with the knee flexed to approximately 30 to 45 degrees. Do not over-tension the medial structures, as this will cause iatrogenic medial patellar subluxation and severe patellofemoral pain. The patella should be able to be translated laterally by 1 to 2 quadrants post-repair.
5. Closure
- Thoroughly irrigate the wound one final time.
- Deflate the tourniquet and achieve meticulous hemostasis to prevent postoperative hematoma, which can compromise the repair and increase the risk of arthrofibrosis.
- Close the subcutaneous tissue and skin in a standard layered fashion.
- Apply a sterile compressive dressing and place the limb in a hinged knee brace locked in full extension.
Postoperative Protocol and Rehabilitation
Whether managed conservatively or operatively, rehabilitation is phased to protect the healing medial structures while restoring function.
- Phase I (Weeks 0-3): Protection and Activation. The knee is locked in extension for ambulation. Weight-bearing is typically allowed as tolerated in the locked brace (unless osteochondral fixation dictates restricted weight-bearing). Isometric quadriceps activation (quad sets) and straight leg raises are initiated immediately to prevent VMO atrophy.
- Phase II (Weeks 3-6): Controlled Motion. The brace is unlocked to allow progressive passive and active-assisted range of motion. The goal is to achieve 90 degrees of flexion by week 4 and full ROM by week 6.
- Phase III (Weeks 6-12): Strengthening. The brace is discontinued. Focus shifts to closed-kinetic-chain exercises (e.g., mini-squats, leg presses) to strengthen the quadriceps, gluteals, and core, which are vital for dynamic lower extremity alignment.
- Phase IV (Months 3-6): Return to Sport. Plyometrics, agility drills, and sport-specific training are introduced. Return to play is permitted when the patient demonstrates symmetrical strength (>90% of the contralateral limb), full pain-free ROM, and no apprehension during dynamic valgus stress.
