Introduction to Shoulder Girdle Malunions
The shoulder girdle is a complex, highly integrated biomechanical system. Alterations in the anatomy of any single component—whether the clavicle, the proximal humerus, or the scapula—can profoundly disrupt the kinematics of the entire upper extremity. Midshaft clavicular fractures have historically been treated nonoperatively; however, it is now well-established that fractures healing with significant shortening (greater than 1.5 to 2.0 cm) or severe angular deformity can lead to symptomatic malunion. Patients typically present with chronic pain, weakness, rapid fatigability, and scapular dyskinesia due to the altered resting position of the shoulder girdle.
In cases of symptomatic midshaft clavicular malunion, corrective osteotomy combined with elastic stable intramedullary nailing (ESIN), as popularized by Smekal et al., offers a sophisticated, minimally invasive solution. This technique restores the anatomical length and axis of the clavicle while preserving the periosteal blood supply, thereby optimizing the biological environment for bone healing.
Before detailing the operative steps for clavicular osteotomy, it is imperative to understand the broader biomechanical context of the shoulder girdle, particularly the deforming forces acting on the proximal humerus, as concurrent injuries or malunions in this region frequently complicate patient presentations and surgical decision-making.
Biomechanics and Deforming Forces of the Proximal Humerus
When evaluating a patient for shoulder girdle reconstruction, the surgeon must consider the entire kinetic chain. Bony abnormalities in the proximal humerus—including displacement of the tuberosities, articular surface incongruity, and malalignment of an articular segment—often occur in combination with soft tissue pathological findings such as capsular contracture, tears of the rotator cuff, and neurological injury. These factors collectively limit the range of motion and decrease the strength of the shoulder.
Each of the structures that may be involved in a proximal humeral fracture or malunion has its own tendinous insertions. These insertions pull a free fracture fragment in a predictable direction, resulting in a characteristic deformity. Understanding these forces is critical for both fracture reduction and malunion reconstruction.
Two-Part Fractures of the Surgical Neck
Two-part fractures of the surgical neck frequently heal in varus and anterior angulation.
* Humeral Shaft: Displaces anteromedially due to the powerful pull of the pectoralis major.
* Proximal Fragment: Abducted and externally rotated by the unopposed pull of the rotator cuff (supraspinatus, infraspinatus, and teres minor).
If the resulting deformity is severe enough, the loss of forward flexion and abduction can be clinically significant, mimicking the biomechanical deficits seen in severe clavicular shortening.
Two-Part Fractures of the Greater Tuberosity
With two-part fractures involving the greater tuberosity, the fragment is subjected to distinct posterosuperior forces.
* Deforming Muscles: The tuberosity is displaced posteriorly and superiorly by the forces exerted by the supraspinatus, teres minor, and infraspinatus muscles.
* Clinical Consequence: A malunion of this type causes a mechanical block, leading to a severe limitation of abduction and external rotation. It frequently results in secondary subacromial impingement, requiring surgical takedown and anatomic fixation.
Two-Part Fractures of the Lesser Tuberosity
Isolated fractures of the lesser tuberosity are less common but present unique challenges.
* Deforming Muscle: The fragment displaces medially owing to the pull of the subscapularis.
* Clinical Consequence: While overall shoulder function is usually not significantly impaired, in some patients, the medially displaced fragment can impinge on the coracoid process, severely limiting internal rotation and forward elevation.
Three-Part Fractures
In three-part fractures characterized by displacement of the greater tuberosity and the surgical neck, the biomechanical imbalance is profound.
* Articular Head Fragment: Internally rotated by the unopposed action of the subscapularis inserting on the intact lesser tuberosity.
* Humeral Shaft: Displaces anteromedially due to the pectoralis major.
* Greater Tuberosity: Displaces posterosuperiorly.
Malunions of this complex fracture pattern require extensive reconstructive efforts, often necessitating osteotomy, mobilization of contracted soft tissues, and rigid internal fixation or arthroplasty.
Clinical Pearl: When evaluating a patient with a symptomatic clavicular malunion, always perform a comprehensive assessment of the proximal humerus and rotator cuff. Compensatory kinematics over time can lead to secondary impingement syndromes or unmask subtle, previously asymptomatic proximal humeral malalignments.
Indications for Clavicular Osteotomy and ESIN
Corrective osteotomy of the clavicle is indicated for patients who present with a symptomatic malunion characterized by:
1. Shortening: Greater than 1.5 to 2.0 cm compared to the contralateral side.
2. Pain: Chronic, debilitating pain at the malunion site or in the periscapular musculature.
3. Neurological Symptoms: Thoracic outlet syndrome (TOS) secondary to hypertrophic callus formation or severe inferior angulation compressing the brachial plexus.
4. Functional Deficit: Weakness in overhead activities and rapid fatigability of the shoulder girdle.
The use of Elastic Stable Intramedullary Nailing (ESIN) for the fixation of the osteotomy is particularly advantageous. It requires a smaller incision than traditional plate osteosynthesis, minimizes periosteal stripping, and provides relative stability that promotes robust secondary bone healing via callus formation.
Preoperative Planning
Meticulous preoperative planning is mandatory. Standard anteroposterior (AP) and 15-degree cephalad tilt radiographs of both clavicles should be obtained to accurately measure the degree of shortening and angulation.
A computed tomography (CT) scan with 3D reconstruction is highly recommended. The CT scan allows the surgeon to assess the exact plane of the malunion, the presence of a medullary canal (which is often obliterated by sclerotic bone at the malunion site), and the proximity of the hypertrophic callus to the underlying neurovascular structures.
Surgical Technique: Osteotomy and ESIN (Smekal et al.)
The following technique details the corrective osteotomy and elastic intramedullary nailing of a midshaft clavicular malunion, adapted from the principles described by Smekal and colleagues.
1. Patient Positioning and Anesthesia
- Anesthesia: Administer general anesthesia. A regional interscalene block may be utilized as an adjunct for postoperative pain control, provided there is no preoperative neurological deficit that requires postoperative monitoring.
- Positioning: Place the patient in a slightly upright "beach chair" position. Ensure the head and neck are secured in a neutral position to avoid traction on the brachial plexus.
- Preparation: The involved limb and the entire shoulder girdle, extending to the sternum medially, must be draped freely to allow for intraoperative manipulation of the arm and access for the intramedullary nail insertion.
2. Surgical Approach
- Incision: Palpate the bony hump at the malunion site. Make an oblique incision of approximately 5 cm in length, carefully placed above and parallel to the Langer skin lines to optimize cosmetic healing.
- Dissection: Carry the dissection through the subcutaneous tissue and the platysma muscle.
- Nerve Protection: Meticulously identify and protect the branches of the supraclavicular nerve. Retraction or transection of these nerves can lead to painful neuromas or distressing chest wall numbness.
- Exposure: Incise the clavipectoral fascia and expose the malunion site. Perform minimal subperiosteal dissection—only enough to visualize the apex of the deformity and safely perform the osteotomy. Preserve the soft tissue attachments to the clavicle as much as possible to maintain vascularity.
3. Determination of the Osteotomy Plane
The success of the procedure relies heavily on the precise execution of the osteotomy. The goal is to recreate the original fracture plane or create a plane that allows for the restoration of length and alignment without creating massive bone defects.
- Fluoroscopic Guidance: Utilize intraoperative fluoroscopy to determine the optimal osteotomy plane. A K-wire or a drill bit can be placed over the bone to simulate the cut and verified under C-arm imaging.
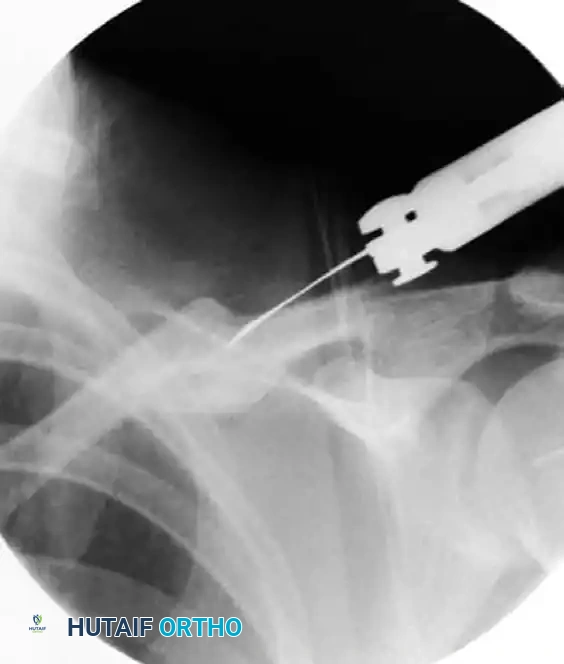
FIGURE 1: Determination of the osteotomy plane using fluoroscopy. A drill bit or K-wire is used to map the trajectory before the definitive cut is made.
- Execution: Once the plane is confirmed, use a fine oscillating saw or an osteotome to carefully divide the malunion. Copious irrigation must be used during sawing to prevent thermal necrosis of the bone.
- Canal Preparation: In chronic malunions, the medullary canal is typically obliterated by dense, sclerotic bone. Use a small drill bit (e.g., 2.0 mm to 3.2 mm, depending on the native canal size) to carefully recanalize both the medial and lateral fragments. Ensure the drill follows the anatomical bow of the clavicle to prevent cortical perforation.
4. Insertion of the Elastic Intramedullary Nail
- Nail Selection: Select a Titanium Elastic Nail (TEN). The diameter is usually between 2.0 mm and 3.0 mm, chosen based on the narrowest isthmus of the recanalized medullary canal.
- Entry Point: While some techniques advocate for a medial entry point at the sternoclavicular junction, others utilize a lateral entry point. For midshaft malunions, a medial entry point is often preferred to allow the nail to be driven laterally across the osteotomy site. Make a small stab incision over the anterior cortex of the medial clavicle, approximately 1.5 cm lateral to the sternoclavicular joint. Use an awl to breach the anterior cortex.
- Nail Advancement: Mount the TEN on a T-handle or a dedicated insertion tool. Advance the nail through the medial fragment until the tip reaches the osteotomy site.
- Reduction and Passage: Manipulate the arm and use reduction forceps (e.g., pointed Weber clamps) at the osteotomy site to anatomically align the medial and lateral fragments. Once reduced, advance the nail across the osteotomy and into the lateral fragment under continuous fluoroscopic control.
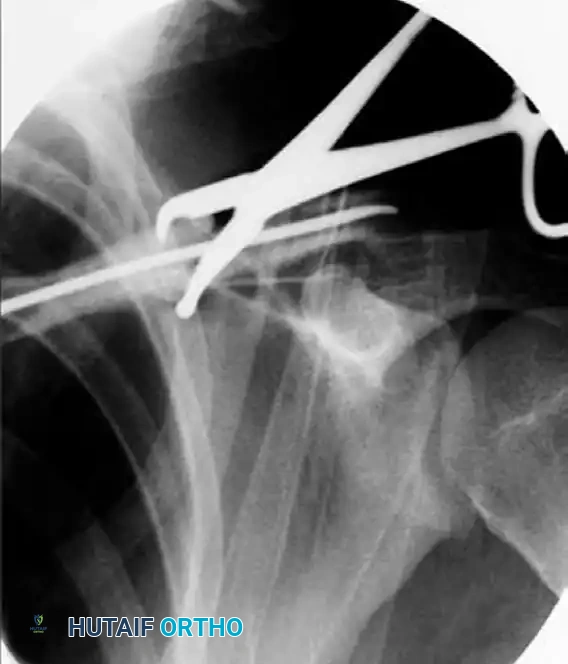
FIGURE 2: Insertion of the elastic nail under fluoroscopic control. Note the use of reduction forceps to maintain alignment while the nail is advanced across the osteotomy site.
Surgical Warning: Do not force the nail if significant resistance is encountered. Forcing the nail can lead to iatrogenic comminution or perforation of the posterior cortex, placing the subclavian vessels and brachial plexus at catastrophic risk. If resistance is met, withdraw the nail slightly, re-verify the reduction, and ensure the canal is adequately prepared.
5. Final Seating and Closure
- Seating the Nail: Advance the nail until the tip is securely embedded in the dense cancellous bone of the lateral clavicle, taking care not to penetrate the acromioclavicular joint.
- Cutting the Nail: Cut the medial end of the nail, leaving approximately 5 to 10 mm protruding from the entry cortex to facilitate future removal. Bend the protruding end slightly toward the bone to minimize soft tissue irritation.
- Bone Grafting (Optional): If the osteotomy results in a structural gap after length restoration, autologous bone graft (harvested from the iliac crest) or demineralized bone matrix (DBM) may be packed into the defect to stimulate osteogenesis.
- Closure: Close the clavipectoral fascia and platysma over the osteotomy site with absorbable sutures. Close the subcutaneous tissue and skin in a layered fashion.
Postoperative Protocol and Rehabilitation
The postoperative rehabilitation protocol must balance the need for early mobilization to prevent shoulder stiffness with the requirement for mechanical stability to allow the osteotomy to heal.
- Phase I (Weeks 0-2): The operative arm is placed in a broad arm sling. Immediate postoperative pendulum exercises are initiated. Active range of motion (ROM) of the elbow, wrist, and hand is encouraged to prevent distal edema and stiffness.
- Phase II (Weeks 2-6): Passive and active-assisted ROM of the shoulder is commenced, limited to 90 degrees of forward flexion and abduction. External rotation is permitted to neutral. The sling is gradually weaned for activities of daily living.
- Phase III (Weeks 6-12): Radiographs are obtained at 6 weeks to assess callus formation. Once clinical and radiographic signs of early union are present, active ROM is progressed without restriction. Isotonic strengthening exercises for the rotator cuff and periscapular stabilizers are initiated.
- Phase IV (Months 3-6): Return to heavy manual labor and contact sports is typically permitted only after complete radiographic consolidation of the osteotomy, which usually occurs between 3 and 6 months postoperatively.
- Hardware Removal: The elastic nail is routinely removed after complete bony union, typically between 6 and 12 months postoperatively, to prevent long-term medial skin irritation or hardware migration.
Complications and Pitfalls
While highly effective, osteotomy and ESIN of the clavicle carry specific risks:
* Hardware Migration: The most common complication of ESIN is medial or lateral migration of the nail. Leaving the medial tip too long can cause skin breakdown, while leaving it too short makes removal difficult.
* Nonunion: Failure to adequately recanalize the sclerotic bone, excessive periosteal stripping, or failure to achieve stable fixation can result in nonunion, necessitating revision surgery with plate osteosynthesis and bone grafting.
* Neurovascular Injury: The subclavian artery, subclavian vein, and brachial plexus lie immediately posterior and inferior to the middle third of the clavicle. Plunging with the drill, saw, or intramedullary nail can cause life-threatening hemorrhage or permanent neurological deficit.
By adhering to strict biomechanical principles, meticulous preoperative planning, and precise surgical execution, the orthopedic surgeon can successfully manage complex clavicular malunions, restoring both anatomy and function to the compromised shoulder girdle.
