Score: 0%
Orthopedics Online MCQs
observation.



.04 4
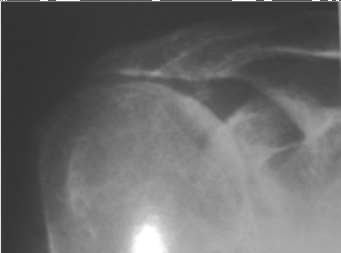
The key to this question is the simply having the knowledge that there are recognized anatomic variants in the anterosuperior aspect of the glenoid labrum (this knowledge won't guarantee that you answer the question right but will keep option "4" open for consideration). The cited
The key to this question is the simply having the knowledge that there are recognized anatomic variants in the anterosuperior aspect of the glenoid labrum (this knowledge won't guarantee that you answer the question right but will keep option "4" open for consideration). The cited
Scientific References
- discuss the described anatomic variants at the anterosuperior aspect of the glenoid labrum but do not discuss how one specifically identifies such a variant (I guess that just comes with experience; both having been shown them and having seen and identified them yourself). Three variants are mostly described:
.04 1
Crush injuries to the foot are bad injuries. In the cited article less than half of the patients had a good functional outcome. The patients that did the best were the ones who strictly adhered to the treatment protocol (no surprise). But, even some of these had poor outcomes. Poor results usually resulted after delayed treatment, delayed soft tissue coverage, development of _neuritis or RSD_ , or those involved in workers' comp/litigation (no surprise again). Recommended treatment includes prompt recognition and treatment of compartment syndrome, early soft tissue coverage and rigid skeletal stabilization.
Reference(s)
Myerson M, McGarvey WC: Crush injuries and compartment syndromes, in Myerson M (ed): Current Therapy in Foot and Ankle Surgery. St Louis, MO, Mosby-Year Book, 1993, pp 264-273.
Answer
Myerson MS, McGarvey WC, Henderson MR, Hakim J: Morbidity after crush injuries to the foot. J Orthop Trauma 1994; 8:343-349.
44.04
A patient sustained a Hawkins type II talar neck fracture and underwent open reduction and internal fixation. The patient now has residual decreased subtalar motion without pain and stands on the lateral border of the foot. What is the most likely cause of these findings?
Crush injuries to the foot are bad injuries. In the cited article less than half of the patients had a good functional outcome. The patients that did the best were the ones who strictly adhered to the treatment protocol (no surprise). But, even some of these had poor outcomes. Poor results usually resulted after delayed treatment, delayed soft tissue coverage, development of _neuritis or RSD_ , or those involved in workers' comp/litigation (no surprise again). Recommended treatment includes prompt recognition and treatment of compartment syndrome, early soft tissue coverage and rigid skeletal stabilization.
Reference(s)
Myerson M, McGarvey WC: Crush injuries and compartment syndromes, in Myerson M (ed): Current Therapy in Foot and Ankle Surgery. St Louis, MO, Mosby-Year Book, 1993, pp 264-273.
Answer
Myerson MS, McGarvey WC, Henderson MR, Hakim J: Morbidity after crush injuries to the foot. J Orthop Trauma 1994; 8:343-349.
44.04
A patient sustained a Hawkins type II talar neck fracture and underwent open reduction and internal fixation. The patient now has residual decreased subtalar motion without pain and stands on the lateral border of the foot. What is the most likely cause of these findings?

Keywords