Score: 0%
ORTHOPEDIC MCQS ONLINE 013 PEDIATRIC
QUESTION 1
Uric acid
_The laboratory studies listed above are needed to diagnose the disorders listed below. Match theappropriate laboratory studies with each of these disorders._
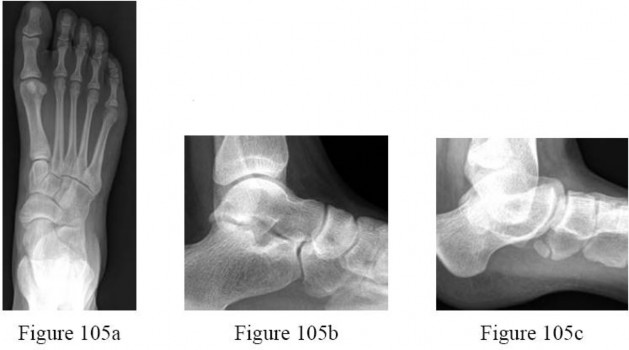
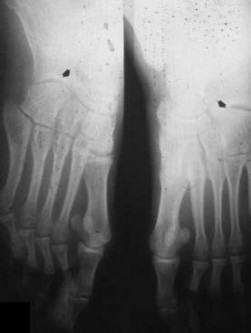
-are the radiographs of a 13-year-old girl with right medial foot pain. The pain has been present for 3 months, is exacerbated by walking and running, and is relieved by rest. She had tried over-the-counter arch supports and nonsteroidal anti-inflammatory drugs for pain relief, but without success. Surgical treatment has been recommended. Which surgical procedure is most likely to relieve the patient’s symptoms?
_The laboratory studies listed above are needed to diagnose the disorders listed below. Match theappropriate laboratory studies with each of these disorders._
-are the radiographs of a 13-year-old girl with right medial foot pain. The pain has been present for 3 months, is exacerbated by walking and running, and is relieved by rest. She had tried over-the-counter arch supports and nonsteroidal anti-inflammatory drugs for pain relief, but without success. Surgical treatment has been recommended. Which surgical procedure is most likely to relieve the patient’s symptoms?













1
Advancement of the posterior tibialis tendon to the inferior portion of the navicular
2
Splitting of the posterior tibialis tendon to excise the bony prominence
3
Performing a hindfoot osteotomy to correct pes planus
4
Performing osteosynthesis of the nonunited bone
-Which gene correlates with severity of disease in spinal muscular atrophy (SMA)?
5
Peripheral myelin protein 22 (PMP22)
-The patient was unable to extend his wrist on preoperative examination. This was caused by injury to the
1) ulnar nerve.
2) radial nerve.
3) recurrent motor branch of the median nerve.
4) anterior interosseous branch of the median nerve.
FOR QUESTIONS 115 THROUGH 117**_
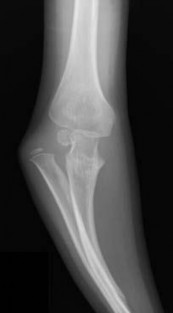
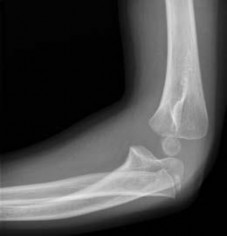
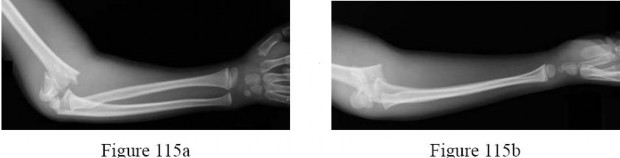
The radiographs show a Gartland type III supracondylar humerus fracture. Although multiple classification systems exist that describe supracondylar humerus fractures, Gartland’s classification is simple and widely used. Type I fractures are nondisplaced according to this classification. Type II
fractures are displaced with a variable amount of angulation, but the posterior cortex of the humerus is intact. Type III fractures are completely displaced with no cortical contact. In flexion-type supracondylar humerus fractures, the distal fragments are anterior to the humeral shaft. The most appropriate treatment method for this fracture is attempted closed reduction and pin fixation. Closed reduction and casting is inappropriate for a Gartland type III supracondylar humerus fracture.
Although open reduction may be required in some cases, most supracondylar humerus fractures, even those that are severely displaced, can be treated with closed reduction and percutaneous pin fixation (and this should be the initial approach).
Although olecranon traction is an option in managing these fractures, it involves repeated radiographs and prolonged hospitalization and is not widely used in North America. The preoperative examination is consistent with a radial nerve injury. Neuropraxias are common in supracondylar humerus fractures, with anterior interosseous nerve injury being the most common, followed by radial nerve. Ulnar nerve injuries occur in flexion-type supracondylar fractures and occasionally as the result of medial pin placement during surgery. The recurrent motor branch of the median nerve supplies the thenar muscles.
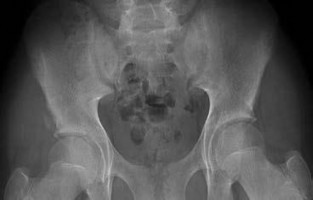
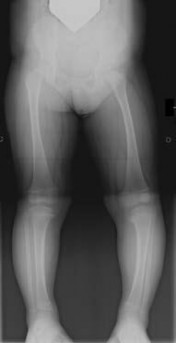
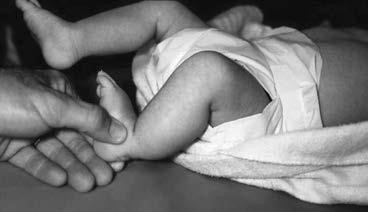
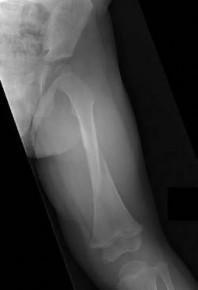
-is the radiograph of a 2-year-old boy who had an isolated injury. An immediate hip spica cast was chosen as the method of treatment. Which of the following techniques increases risk for compartment syndrome in the left leg following cast placement?
1) Using a single-leg spica instead of a double-leg spica
2) Wrapping the left short-leg portion of the cast first, then pulling traction through the fracture site
3) Placing the cast in an emergency department setting under sedation
4) Placing the cast within 24 hours of the injury
108 • American Academy of Orthopaedic Surgeons
A 12-year-old boy from Maine has an atraumatic knee effusion. He has no fever, mild tenderness, and lacks 10 degrees of flexion and extension. He continues to play basketball. He had flu-like symptoms 3 months ago. Radiographs and white blood cell count (WBC) findings are normal. His erythrocyte sedimentation rate is 53 mm/h (reference range, 0-20 mm/h) and C-reactive protein is 3.2 mg/L (reference range, 0.08-3.1 mg/L). The knee aspiration WBC count is 55000 leukocytes/mL (a synovial fluid count
1) Administer Lyme titer and oral doxycycline
2) Operative lavage of the knee and start intravenous cephalosporin
3) Start nonsteroidal anti-inflammatory drugs (NSAIDs) and refer to rheumatology
4) Hospitalization for intravenous cephalosporin
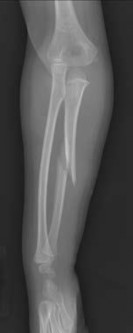
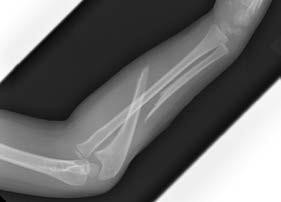
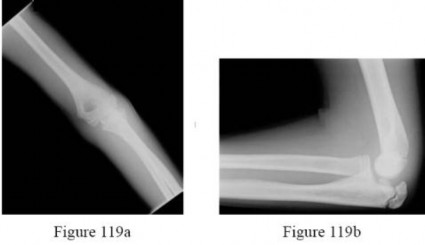
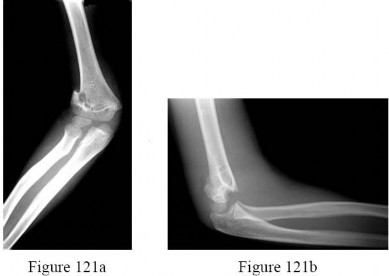
-are the anteroposterior (AP) and lateral radiographs of the right elbow of a 7-yearold boy who fell off the monkey bars onto his outstretched right hand. Immediate pain and swelling were noted around his elbow; there were no other injuries. His hand was neurovascularly intact. What is the best treatment for this fracture?
1) Closed reduction and casting in the emergency department
2) Closed reduction and percutaneous pinning of the fracture
3) Open reduction and plate fixation of the fracture in the operating room with early mobilization and no cast
4) Cast immobilization in the emergency department with the expectation that this injury will heal and remodel uneventfully
-is the radiograph of an 11-year-old gymnast who was evaluated for lateral foot pain that has been increasing during the past 6 months. She had 3 ankle sprains during the last 6 months. She was prescribed proprioceptive ankle exercises, orthotics, and a trial of a cast immobilization, but experienced no relief. She has foot pain with daily activity and is now unable to participate in gymnastics. What is the most appropriate course of action?
1) Discontinue gymnastics
2) Cast immobilization
3) Surgical treatment
4) Continued physical therapy
.v4b{border:2px solid #0984e3;background:#fff;color:#0984e3;padding:8px 20px;border-radius:25px;cursor:pointer;margin-right:10px;font-weight:bold;transition:0.3s;}
.v4b.active{background:#0984e3;color:#fff;}
.v4b:hover:not(.active){background:#e3f2fd;}
.mcq-v4-card{background:#fff;border-radius:15px;padding:35px;margin-bottom:40px;border:1px solid #e1e8ed;box-shadow:0 5px 15px rgba(0,0,0,0.04);}
.card-meta{color:#0984e3;font-weight:800;margin-bottom:20px;letter-spacing:1.5px;font-size:0.95rem;}
.q-stem{font-size:1.25rem;margin-bottom:30px;font-weight:500;line-height:1.7;color:#2d3436;}
.q-opt{display:flex;align-items:center;padding:15px;border:2px solid #f1f2f6;border-radius:12px;margin-bottom:15px;cursor:pointer;transition:all 0.2s ease-in-out;background:#fff;}
.q-opt:hover{border-color:#0984e3;background:#f0f7ff;transform:translateX(5px);}
.q-opt-circle{width:35px;height:35px;border:2px solid #ddd;border-radius:50%;display:flex;align-items:center;justify-content:center;margin-right:20px;font-weight:bold;background:#fafafa;flex-shrink:0;color:#636e72;}
.q-opt.correct{background:#e3fcef;border-color:#00b894;}
.q-opt.correct .q-opt-circle{background:#00b894;color:#fff;border-color:#00b894;}
.q-opt.wrong{background:#fff5f5;border-color:#ff7675;}
.q-opt.wrong .q-opt-circle{background:#ff7675;color:#fff;border-color:#ff7675;}
.q-opt.selected{border-color:#0984e3;background:#e3f2fd;}
.q-opt.selected .q-opt-circle{background:#0984e3;color:#fff;border-color:#0984e3;}
.q-feedback{margin-top:30px;padding:25px;background:#f8f9fa;border-left:6px solid #0984e3;border-radius:8px;}
.feedback-label{font-weight:bold;margin-bottom:15px;font-size:1.2rem;}
.explanation-text{line-height:1.7;color:#444;font-size:1.05rem;}
var v4E={
m:'study',r:new Map(),
setMode:function(m){this.m=m;document.getElementById('v4s').classList.toggle('active',m=='study');document.getElementById('v4e').classList.toggle('active',m=='exam');document.getElementById('v4xa').style.display=m=='exam'?'block':'none';this.reset();},
reset:function(){document.querySelectorAll('.q-opt').forEach(e=>{e.className='q-opt';e.style.pointerEvents='auto';});document.querySelectorAll('.q-feedback').forEach(e=>e.style.display='none');this.r.clear();this.up();},
up:function(){let s=0;this.r.forEach(v=>{if(v===true||v.s==v.c)s++;});const t=document.querySelectorAll('.mcq-v4-card').length;document.getElementById('v4sc').innerText=Math.round((s/t)*100)||0;},
reveal:function(c,s,k){const o=c.querySelectorAll('.q-opt');if(o[k-1])o[k-1].classList.add('correct');if(s!=k && o[s-1])o[s-1].classList.add('wrong');c.querySelector('.q-feedback').style.display='block';const fl=c.querySelector('.feedback-label');fl.innerHTML=s==k?' Correct Answer':' Incorrect';},
finish:function(){this.r.forEach((v,k)=>{this.reveal(document.getElementById('card-'+k),v.s,v.c);});document.querySelectorAll('.q-opt').forEach(e=>e.style.pointerEvents='none');window.scrollTo({top:0,behavior:'smooth'});}
};
document.querySelectorAll('.q-opt').forEach(el=>{
el.onclick=function(){
const q=this.dataset.q,k=this.dataset.correct,s=this.dataset.idx,p=this.closest('.mcq-v4-card');
if(v4E.m=='study') { if(v4E.r.has(q))return; v4E.r.set(q,s==k); p.querySelectorAll('.q-opt').forEach(o=>o.style.pointerEvents='none'); v4E.reveal(p,s,k); }
else { p.querySelectorAll('.q-opt').forEach(o=>o.classList.remove('selected')); this.classList.add('selected'); v4E.r.set(q,{s:s,c:k}); }
v4E.up();
};
});
1) ulnar nerve.
2) radial nerve.
3) recurrent motor branch of the median nerve.
4) anterior interosseous branch of the median nerve.
FOR QUESTIONS 115 THROUGH 117**_
The radiographs show a Gartland type III supracondylar humerus fracture. Although multiple classification systems exist that describe supracondylar humerus fractures, Gartland’s classification is simple and widely used. Type I fractures are nondisplaced according to this classification. Type II
fractures are displaced with a variable amount of angulation, but the posterior cortex of the humerus is intact. Type III fractures are completely displaced with no cortical contact. In flexion-type supracondylar humerus fractures, the distal fragments are anterior to the humeral shaft. The most appropriate treatment method for this fracture is attempted closed reduction and pin fixation. Closed reduction and casting is inappropriate for a Gartland type III supracondylar humerus fracture.
Although open reduction may be required in some cases, most supracondylar humerus fractures, even those that are severely displaced, can be treated with closed reduction and percutaneous pin fixation (and this should be the initial approach).
Although olecranon traction is an option in managing these fractures, it involves repeated radiographs and prolonged hospitalization and is not widely used in North America. The preoperative examination is consistent with a radial nerve injury. Neuropraxias are common in supracondylar humerus fractures, with anterior interosseous nerve injury being the most common, followed by radial nerve. Ulnar nerve injuries occur in flexion-type supracondylar fractures and occasionally as the result of medial pin placement during surgery. The recurrent motor branch of the median nerve supplies the thenar muscles.
-is the radiograph of a 2-year-old boy who had an isolated injury. An immediate hip spica cast was chosen as the method of treatment. Which of the following techniques increases risk for compartment syndrome in the left leg following cast placement?
1) Using a single-leg spica instead of a double-leg spica
2) Wrapping the left short-leg portion of the cast first, then pulling traction through the fracture site
3) Placing the cast in an emergency department setting under sedation
4) Placing the cast within 24 hours of the injury
108 • American Academy of Orthopaedic Surgeons
A 12-year-old boy from Maine has an atraumatic knee effusion. He has no fever, mild tenderness, and lacks 10 degrees of flexion and extension. He continues to play basketball. He had flu-like symptoms 3 months ago. Radiographs and white blood cell count (WBC) findings are normal. His erythrocyte sedimentation rate is 53 mm/h (reference range, 0-20 mm/h) and C-reactive protein is 3.2 mg/L (reference range, 0.08-3.1 mg/L). The knee aspiration WBC count is 55000 leukocytes/mL (a synovial fluid count
1) Administer Lyme titer and oral doxycycline
2) Operative lavage of the knee and start intravenous cephalosporin
3) Start nonsteroidal anti-inflammatory drugs (NSAIDs) and refer to rheumatology
4) Hospitalization for intravenous cephalosporin
-are the anteroposterior (AP) and lateral radiographs of the right elbow of a 7-yearold boy who fell off the monkey bars onto his outstretched right hand. Immediate pain and swelling were noted around his elbow; there were no other injuries. His hand was neurovascularly intact. What is the best treatment for this fracture?
1) Closed reduction and casting in the emergency department
2) Closed reduction and percutaneous pinning of the fracture
3) Open reduction and plate fixation of the fracture in the operating room with early mobilization and no cast
4) Cast immobilization in the emergency department with the expectation that this injury will heal and remodel uneventfully
-is the radiograph of an 11-year-old gymnast who was evaluated for lateral foot pain that has been increasing during the past 6 months. She had 3 ankle sprains during the last 6 months. She was prescribed proprioceptive ankle exercises, orthotics, and a trial of a cast immobilization, but experienced no relief. She has foot pain with daily activity and is now unable to participate in gymnastics. What is the most appropriate course of action?
1) Discontinue gymnastics
2) Cast immobilization
3) Surgical treatment
4) Continued physical therapy
.v4b{border:2px solid #0984e3;background:#fff;color:#0984e3;padding:8px 20px;border-radius:25px;cursor:pointer;margin-right:10px;font-weight:bold;transition:0.3s;}
.v4b.active{background:#0984e3;color:#fff;}
.v4b:hover:not(.active){background:#e3f2fd;}
.mcq-v4-card{background:#fff;border-radius:15px;padding:35px;margin-bottom:40px;border:1px solid #e1e8ed;box-shadow:0 5px 15px rgba(0,0,0,0.04);}
.card-meta{color:#0984e3;font-weight:800;margin-bottom:20px;letter-spacing:1.5px;font-size:0.95rem;}
.q-stem{font-size:1.25rem;margin-bottom:30px;font-weight:500;line-height:1.7;color:#2d3436;}
.q-opt{display:flex;align-items:center;padding:15px;border:2px solid #f1f2f6;border-radius:12px;margin-bottom:15px;cursor:pointer;transition:all 0.2s ease-in-out;background:#fff;}
.q-opt:hover{border-color:#0984e3;background:#f0f7ff;transform:translateX(5px);}
.q-opt-circle{width:35px;height:35px;border:2px solid #ddd;border-radius:50%;display:flex;align-items:center;justify-content:center;margin-right:20px;font-weight:bold;background:#fafafa;flex-shrink:0;color:#636e72;}
.q-opt.correct{background:#e3fcef;border-color:#00b894;}
.q-opt.correct .q-opt-circle{background:#00b894;color:#fff;border-color:#00b894;}
.q-opt.wrong{background:#fff5f5;border-color:#ff7675;}
.q-opt.wrong .q-opt-circle{background:#ff7675;color:#fff;border-color:#ff7675;}
.q-opt.selected{border-color:#0984e3;background:#e3f2fd;}
.q-opt.selected .q-opt-circle{background:#0984e3;color:#fff;border-color:#0984e3;}
.q-feedback{margin-top:30px;padding:25px;background:#f8f9fa;border-left:6px solid #0984e3;border-radius:8px;}
.feedback-label{font-weight:bold;margin-bottom:15px;font-size:1.2rem;}
.explanation-text{line-height:1.7;color:#444;font-size:1.05rem;}
var v4E={
m:'study',r:new Map(),
setMode:function(m){this.m=m;document.getElementById('v4s').classList.toggle('active',m=='study');document.getElementById('v4e').classList.toggle('active',m=='exam');document.getElementById('v4xa').style.display=m=='exam'?'block':'none';this.reset();},
reset:function(){document.querySelectorAll('.q-opt').forEach(e=>{e.className='q-opt';e.style.pointerEvents='auto';});document.querySelectorAll('.q-feedback').forEach(e=>e.style.display='none');this.r.clear();this.up();},
up:function(){let s=0;this.r.forEach(v=>{if(v===true||v.s==v.c)s++;});const t=document.querySelectorAll('.mcq-v4-card').length;document.getElementById('v4sc').innerText=Math.round((s/t)*100)||0;},
reveal:function(c,s,k){const o=c.querySelectorAll('.q-opt');if(o[k-1])o[k-1].classList.add('correct');if(s!=k && o[s-1])o[s-1].classList.add('wrong');c.querySelector('.q-feedback').style.display='block';const fl=c.querySelector('.feedback-label');fl.innerHTML=s==k?' Correct Answer':' Incorrect';},
finish:function(){this.r.forEach((v,k)=>{this.reveal(document.getElementById('card-'+k),v.s,v.c);});document.querySelectorAll('.q-opt').forEach(e=>e.style.pointerEvents='none');window.scrollTo({top:0,behavior:'smooth'});}
};
document.querySelectorAll('.q-opt').forEach(el=>{
el.onclick=function(){
const q=this.dataset.q,k=this.dataset.correct,s=this.dataset.idx,p=this.closest('.mcq-v4-card');
if(v4E.m=='study') { if(v4E.r.has(q))return; v4E.r.set(q,s==k); p.querySelectorAll('.q-opt').forEach(o=>o.style.pointerEvents='none'); v4E.reveal(p,s,k); }
else { p.querySelectorAll('.q-opt').forEach(o=>o.classList.remove('selected')); this.classList.add('selected'); v4E.r.set(q,{s:s,c:k}); }
v4E.up();
};
});
