DEFINITION
Simple dislocations of the elbow can most often be treated successfully with closed means: reduction and short-term immobilization followed by early motion. Fracture-dislocations of the elbow are more troublesome in that they often require operative intervention. Fractures associated with elbow dislocations often involve the radial head and coronoid. An elbow dislocation associated with fractures of the radial head and coronoid is termed the
terrible triad.
 ---
---
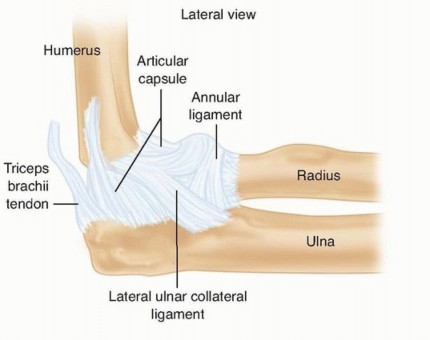
 ### FIG 1 • The MCL and LCL complexes of the elbow. Note their points of attachment on the distal humerus and proximal ulna. The principle of treating fracture-dislocations of the elbow is to provide sufficient stability through reconstruction of bony and ligamentous restraints such that early motion (within 2 weeks postoperatively) can be instituted without recurrent instability. Failure to achieve this will result in either recurrent instability or severe stiffness after prolonged immobilization. ## ANATOMY Posterolateral dislocations of the elbow are associated with disruption of the medial collateral ligament (MCL) and lateral collateral ligament (LCL).
The MCL is the primary stabilizer to valgus stress ( FIG 1).
The LCL is the primary stabilizer to posterolateral rotatory instability. Most often, the LCL disruption is proximally from the lateral epicondyle of the humerus, which creates a characteristic bare spot. Less commonly, the ligament may rupture midsubstance. 7 Secondary restraints on the lateral side that may also be disrupted are the common extensor origin and the posterolateral capsule.
Radial head fractures have been classified by Mason:
Type I: small or marginal fracture with minimal displacement Type II: marginal fracture with displacement
Type III: comminuted fractures of the head and neck 5
Type IV: radial head fracture associated with elbow dislocation (Johnson modification) Coronoid fractures have been classified by Regan and Morrey 11 ( FIG 2):
Type I: tip fractures (not avulsions) Type II: less than 50% of the coronoid
### FIG 1 • The MCL and LCL complexes of the elbow. Note their points of attachment on the distal humerus and proximal ulna. The principle of treating fracture-dislocations of the elbow is to provide sufficient stability through reconstruction of bony and ligamentous restraints such that early motion (within 2 weeks postoperatively) can be instituted without recurrent instability. Failure to achieve this will result in either recurrent instability or severe stiffness after prolonged immobilization. ## ANATOMY Posterolateral dislocations of the elbow are associated with disruption of the medial collateral ligament (MCL) and lateral collateral ligament (LCL).
The MCL is the primary stabilizer to valgus stress ( FIG 1).
The LCL is the primary stabilizer to posterolateral rotatory instability. Most often, the LCL disruption is proximally from the lateral epicondyle of the humerus, which creates a characteristic bare spot. Less commonly, the ligament may rupture midsubstance. 7 Secondary restraints on the lateral side that may also be disrupted are the common extensor origin and the posterolateral capsule.
Radial head fractures have been classified by Mason:
Type I: small or marginal fracture with minimal displacement Type II: marginal fracture with displacement
Type III: comminuted fractures of the head and neck 5
Type IV: radial head fracture associated with elbow dislocation (Johnson modification) Coronoid fractures have been classified by Regan and Morrey 11 ( FIG 2):
Type I: tip fractures (not avulsions) Type II: less than 50% of the coronoid
 ---
---
FIG 2 • Lateral view of the elbow depicting the different types of coronoid fractures. 293 Type III: more than 50% of the coronoid The insertion of the MCL is at the base of the coronoid and it may be involved in type III fractures. 1 Anteromedial facet fractures of the coronoid are a different entity and are caused by a primary varus force. 3 The medial facet is important for varus stability of the elbow, just distal to this is the sublime tubercle, the insertion point of MCL.
 ---
---


 ### FIG 3 • Anteromedial facet fracture of the coronoid. A. Radiographs demonstrating fracture of the anteromedial facet of the coronoid as well as the coronoid ti Varus instability can be appreciated on the AP radiograph. B. CT scan depicting the anteromedial facet fragment (
black arrow
) and coronoid tip fragment (
white arrow
). C. Intraoperative picture, the anteromedial facet has been reduced and fixed with a buttress plate and screws. The coronoid tip is held reduced with a Kirschner wire and ready for plate fixation. D. Postoperative radiograph demonstrating plate fixation of the coronoid tip as well as anteromedial facet with two separate plates. E. Clinical picture revealing medial-based incision and good postoperative range of motion. Anteromedial facet fractures may lead to varus posteromedial instability, and disruption of the LCL (from the varus force) is often seen. However, there is also potential for valgus instability if the fractured fragment is large enough to include the MCL insertion. These fractures are unstable and in general are best treated with open reduction internal fixation with use of a medial plate in a buttress fashion ( FIG 3). 294
### FIG 3 • Anteromedial facet fracture of the coronoid. A. Radiographs demonstrating fracture of the anteromedial facet of the coronoid as well as the coronoid ti Varus instability can be appreciated on the AP radiograph. B. CT scan depicting the anteromedial facet fragment (
black arrow
) and coronoid tip fragment (
white arrow
). C. Intraoperative picture, the anteromedial facet has been reduced and fixed with a buttress plate and screws. The coronoid tip is held reduced with a Kirschner wire and ready for plate fixation. D. Postoperative radiograph demonstrating plate fixation of the coronoid tip as well as anteromedial facet with two separate plates. E. Clinical picture revealing medial-based incision and good postoperative range of motion. Anteromedial facet fractures may lead to varus posteromedial instability, and disruption of the LCL (from the varus force) is often seen. However, there is also potential for valgus instability if the fractured fragment is large enough to include the MCL insertion. These fractures are unstable and in general are best treated with open reduction internal fixation with use of a medial plate in a buttress fashion ( FIG 3). 294
 ---
---
 ### FIG 4 • Typical mechanism of elbow fracture-dislocation. Note the forces at play on the elbow.
### FIG 4 • Typical mechanism of elbow fracture-dislocation. Note the forces at play on the elbow.
PATHOGENESIS Fracture-dislocations of the elbow occur during falls onto an outstretched hand, falls from a height, motor vehicle accidents, or other high-energy trauma ( FIG 4). Typically, there is a hyperextension and valgus or varus stress applied to the pronated arm. ## NATURAL HISTORY Elbow dislocations with associated coronoid or radial head fractures have a poor natural history. These injuries are commonly treated with open reduction and surgical fixation, as redislocation or subluxation is likely with closed treatment. Treatment of the radial head fracture by excision alone in the context of an elbow dislocation has a high rate of failure due to recurrent instability and should be avoided. Problems of recurrent instability, arthrosis, and severe stiffness lead to poor functional results. 12 ## PATIENT HISTORY AND PHYSICAL FINDINGS Fracture-dislocations of the elbow are acute and traumatic, so the history should be straightforward. It is not unusual for these injuries to occur with high-energy trauma, so a diligent search for other musculoskeletal and systemic injuries must accompany evaluation of the elbow. The ipsilateral shoulder and wrist should be evaluated. The evaluation and documentation of peripheral nerve and vascular function in the injured extremity is critical and should be performed before and after reduction maneuvers. ## IMAGING AND OTHER DIAGNOSTIC STUDIES High-quality plain radiographs in the anteroposterior (AP) and lateral plane should be obtained before and after closed reduction. Cast material can obscure bony detail after closed reduction. If there is any evidence of forearm or wrist pain associated with the elbow injury, these should be imaged as well. Computed tomography (CT) scans with reformatted images and three-dimensional (3-D) reconstructions are helpful in understanding the configuration of bony injuries (especially of the radial head and coronoid) and are helpful in treatment planning ( FIG 5). ## DIFFERENTIAL DIAGNOSIS Radial head or neck fractures without associated dislocation Coronoid fracture associated with posteromedial instability. The radial head is not fractured, making diagnosis more difficult. ## NONOPERATIVE MANAGEMENT Initial treatment involves closed reduction and splinting with radiographs to confirm reduction ( FIG 6). If reduction cannot be maintained because of bone or soft tissue injury, repeated attempts at closed reduction should not be attempted. This is thought to contribute to the formation of heterotopic ossification. In the setting of fracture-dislocation of the elbow with instability, the ability of nonoperative management to meet treatment goals is rare and surgery is indicated in almost all cases.
 ---
---
FIG 5 • 3-D CT reconstruction of “terrible triad” injury. The
arrow
represents the large coronoid fragment anterior to the elbow. (From Pugh DM, Wild LM, Schemitsch EH, et al. Standard surgical protocol to treat elbow dislocations with radial head and coronoid fractures. J Bone Joint Surg Am 2004;86A:1122-1130.) 295
 ---
---
FIG 6 • Radiograph revealing nonconcentric reduction after closed reduction. The small arrows highlight the nonconcentric reduction of the ulnohumeral joint. (From Pugh DM, Wild LM, Schemitsch EH, et al. Standard surgical protocol to treat elbow dislocations with radial head and coronoid fractures. J Bone Joint Surg Am 2004;86A:1122-1130.)
SURGICAL MANAGEMENT The goals of surgery are to obtain and maintain a concentric and stable reduction of the ulnohumeral and radiocapitellar joint such that early motion within a flexion-extension arc of 30 to 130 degrees can be initiated. Early motion is key (within 2 weeks postoperatively) to avoid elbow stiffness and resultant poor function. Management of elbow dislocations with associated radial head and coronoid fractures should follow an established protocol ( Table 1) that has produced reliable results.10 The radial head is an important secondary stabilizer of the elbow to valgus stress and posterior instability. 9 It is also a longitudinal stabilizer of the forearm to proximal translation. If fractured in this setting, it must be fixed or replaced, as radial head excision leads to recurrent instability and unacceptable results. 12 ## Preoperative Planning Before surgery, the surgeon must ensure that the proper equipment and implants are available. Coronoid tip fractures are fixed with small fragment or cannulated screws of appropriate size. In the setting of small fragments (ie, type 1) that are not amendable to screw fixation, sutures through the anterior capsule around the fragment can be used instead. Large coronoid fragments such as anteromedial facet fragments should be fixed with a minifragment plate and screws in buttress fashion. ## Table 1 Treatment Protocol for Elbow Dislocation with Associated Radial Head and Coronoid Fractures
Step Action
1 Fix the coronoid fracture. ### 2 Fix or replace the radial head. ### 3 Repair the LCL. ### 4 Assess elbow stability within 30-130 degrees of flexion-extension with the forearm in full pronation. ### 5 If the elbow remains unstable, consider fixing the MCL. ### 6 Failing this, apply a hinged external fixator to maintain concentric reduction and allow for early motion. Radial head and neck fracture fixation is accomplished with screws alone or small fragment plates and screws. We often use countersunk Herbert screws or countersunk minifragment screws to fix articular head fragments. If the radial head fragment is comminuted with more than three fragments, the surgeon must be prepared for radial head replacement. A metallic, modular radial head implant system should be available if primary osteosynthesis cannot be achieved. An image intensifier is helpful during surgery. Films confirming concentric reduction and the proper positioning of implanted hardware should always be obtained before leaving the operating room. In rare instances in which bony and ligamentous repair fails to restore sufficient elbow stability, dynamic hinged external fixation is used. This is a highly specialized technique that may not be appropriate for all surgeons. In the event that a dynamic fixator is not an option, a static external fixation should be applied and patient must be referred to an upper extremity surgeon for further management. ## Positioning Most commonly, the patient is positioned supine on the operating table under general anesthesia. The operative limb is supported on a hand table, and a tourniquet is applied to the upper arm before preparation and draping ( FIG 7). Alternatively, the lateral decubitus position can be used with the operative limb supported by a padded bolster. This position is used if hinged fixation is deemed likely. A posterior skin incision can also be used in this position, with creation of full-thickness flaps to access both medial and lateral sides. ## Approach The lateral approach is the workhorse for treatment of these injuries where the coronoid, radial head, and LCL can 296 be addressed. A direct lateral incision with the patient supine and the arm on a hand table is used.
 ---
---
 ### FIG 7 • Patient positioned supine with hand table. Landmarks and skin incision are shown in FIG 8A. The typical approach uses the Kocher interval between the anconeus and external carpi ulnaris. However, the surgeon should use the traumatic dissection that has occurred at the time of injury to gain exposure of the elbow. Typically, the LCL has been avulsed from the lateral distal humerus, leaving a bare spot ( FIG 8B).10 Some cases require a medial approach as well for either medial ligament reconstruction or plating of a coronoid fracture. This can be accomplished through a second medial incision.
### FIG 7 • Patient positioned supine with hand table. Landmarks and skin incision are shown in FIG 8A. The typical approach uses the Kocher interval between the anconeus and external carpi ulnaris. However, the surgeon should use the traumatic dissection that has occurred at the time of injury to gain exposure of the elbow. Typically, the LCL has been avulsed from the lateral distal humerus, leaving a bare spot ( FIG 8B).10 Some cases require a medial approach as well for either medial ligament reconstruction or plating of a coronoid fracture. This can be accomplished through a second medial incision.
 ---
---
 ### FIG 8 • A. Landmarks and skin incision. The underlying bones have been represented and the position of the lateral skin incision is marked with the
hashed line.
B. Avulsion of LCL. The
arrow
is pointing to the bare spot on the distal lateral humerus where the LCL complex has been avulsed. The ulnar nerve is at risk in this approach and should be identified and protected. The common flexor origin is split distal to the medial epicondyle to expose the coronoid medially. Alternatively, a posterior skin incision can be used with elevation of full-thickness flaps at the fascial level to approach both laterally and medially. The patient can be placed in the lateral decubitus position or supine with the arm across the chest for this approach. ## TECHNIQUES
### FIG 8 • A. Landmarks and skin incision. The underlying bones have been represented and the position of the lateral skin incision is marked with the
hashed line.
B. Avulsion of LCL. The
arrow
is pointing to the bare spot on the distal lateral humerus where the LCL complex has been avulsed. The ulnar nerve is at risk in this approach and should be identified and protected. The common flexor origin is split distal to the medial epicondyle to expose the coronoid medially. Alternatively, a posterior skin incision can be used with elevation of full-thickness flaps at the fascial level to approach both laterally and medially. The patient can be placed in the lateral decubitus position or supine with the arm across the chest for this approach. ## TECHNIQUES
POSTOPERATIVE CARE Indications 1. Elbow dislocations with associated fractures of the coronoid or radial head must be recognized as complex dislocations. They usually require surgical treatment. Goals of treatment 1. The goals are to obtain a concentric reduction with sufficient elbow stability such that early range of motion is possible and to avoid persistent instability, elbow stiffness, and arthritis. Coronoid fractures 1. Repair of coronoid fractures is technically demanding but necessary for successful treatment. Radial head 1. The surgeon should be prepared to replace the radial head if necessary with a metal, modular prosthesis. 2. Excision alone is not an option. Lateral ligaments 1. Repair of the lateral ligaments is important to impart the necessary stability for early motion and to avoid late posterolateral rotatory instability. Physiotherapy ▪ It is important to emphasize to the patient the need to be diligent with rehabilitation and exercises, as this will have a great effect on the end result. 1. Immobilization beyond 2 weeks should be avoided. The injured elbow is placed in a well-padded plaster splint at 90 degrees of flexion and full pronation. The patient is given a sling for comfort. AP and lateral radiographs are obtained in the operating room to ensure congruent reduction and verify hardware placement. The patient may be discharged home on the same day after receiving adequate analgesia and prophylactic antibiotics. We do not routinely give prophylaxis for heterotopic ossification unless the patient has a concomitant head injury: In this case, indomethacin 25 mg three times a day is prescribed with a cytoprotective agent for 3 weeks. The patient returns to our clinic at 7 to 10 days postoperatively for staple removal. The splint is typically removed at this point. Range-of-motion exercises are initiated at this time under the supervision of a physiotherapist. Active and active-assisted flexion-extension between 30 and 130 degrees and forearm rotation with the elbow at 90 degrees of flexion is initiated. A lightweight resting splint is made for the injured elbow that is removed for hygiene and physiotherapy. The patient returns at 4, 8, and 12 weeks after surgery for clinical review with plain radiographs. Thereafter, the interval of clinic visits is widened, but we follow our patients out to 2 years. At 4 weeks, we allow unrestricted range of motion and at 8 weeks, unrestricted strengthening. Evidence of fracture union is usually present between 6 and 8 weeks. Progress with range of motion can be slow and frustrating for the patient but does not plateau until 1 year of follow-u ## OUTCOMES Following the protocol outlined for fracture-dislocations of the elbow should yield satisfactory functional results. Pugh et al 10 reported the results of this treatment protocol for 36 elbows at 34 months. The flexion-extension arc averaged 112 degrees and rotation 136 degrees. Fifteen patients had excellent results, 13 good, 7 fair, and 1 poor as measured by the Mayo Elbow Performance Score. Eight patients had a complication requiring reoperation. ## COMPLICATIONS The most likely complication after treatment is unacceptable elbow stiffness with a resultant nonfunctional range of motion. An acceptable range is 30 to 130 degrees of flexion. At about 1 year after surgery, once motion has plateaued, patients are candidates for release with hardware removal if they are not happy with their range of motion and the flexion-extension arc is less than 100 degrees. This is done through the lateral approach with an anterior and posterior capsulectomy plus manipulation under anesthesia. A radial head implant in place can be downsized to improve motion, but it should not be simply removed. The lateral ligament complex is preserved. In our series, this was necessary in 11% of cases. 10 Synostosis around the elbow is another possible cause of rotational forearm stiffness. A resection can be planned to improve motion. CT scanning preoperatively helps to define the extent of the lesion. Resection is technically demanding. Superficial and deep wound infection is possible after repair. Immediate and aggressive treatment is recommended with antibiotics initially and irrigation with débridement if rapid improvement is not seen. Persistent instability is rare but may occur despite best efforts at repair. Formal ligament reconstruction can be helpful in this setting. Posttraumatic arthritis may be a long-term problem. ## REFERENCES
- Cage DJ, Abrams RA, Callahan JJ, et al. Soft tissue attachments of the ulnar coronoid process. An anatomic study with radiographic correlation. Clin Orthop Relat Res 1995;(320):154-158. 2. Doornberg JN, Linzel DS, Zurakowski D, et al. Reference points for radial head prosthesis size. J Hand Surg 2006;31(1):53-57. 3. Doornberg JN, Ring DC. Fracture of the anteromedial facet of the coronoid process. J Bone Joint Surg Am 2006;88(10):2216-2224. 301 4. Frank SG, Grewal R, Johnson J, et al. Determination of correct implant size in radial head arthroplasty to avoid overlengthening. J Bone Joint Surg Am 2009;91:1738-1746. 5. Mason ML. Some observations on fractures of the head of the radius with a review of one hundred cases. Br J Surg 1954;42:123-132. 6. McKee MD, Bowden SH, King GJ, et al. Management of recurrent, complex instability of the elbow with a hinged external fixator. J Bone Joint Surg Br 1998;80(6):1031-1036. 7. McKee MD, Schemitsch EH, Sala MJ, et al. The pathoanatomy of lateral ligamentous disruption in complex elbow instability. J Shoulder Elbow Surg 2003;12:391-396. 8. Moro JK, Werier J, MacDermid JC, et al. Arthroplasty with a metal radial head for unreconstructable fractures of the radial head. J Bon Joint Surg Am 2001;83-A(8):1201-1211. 9. Morrey BF, Tanaka S, An KN. Valgus stability of the elbow. A definition of primary and secondary constraints. Clin Orthop Relat Res 1991;(265):187-195. 10. Pugh DM, Wild LM, Schemitsch EH, et al. Standard surgical protocol to treat elbow dislocations with radial head and coronoid fractures. J Bone Joint Surg Am 2004;86A:1122-1130. 11. Regan W, Morrey B. Fractures of the coronoid process of the ulna. J Bone Joint Surg Am 1989;71:1248-1254.
- Ring D, Jupiter JB, Zilberfarb J. Posterior dislocation of the elbow with fractures of the radial head and coronoid. J Bone Joint Surg Am 2002;84-A(4):547-551.
 ---
---
 **### TECH FIG 1 • Lateral approach. In this case, the radial neck was fractured and the head has been removed. An excellent view of the coronoid is achieved. Here, a type I coronoid fracture is present.
**### TECH FIG 1 • Lateral approach. In this case, the radial neck was fractured and the head has been removed. An excellent view of the coronoid is achieved. Here, a type I coronoid fracture is present.
