Introduction and Epidemiology
The Achilles tendon is the strongest tendon in the body and is the primary plantarflexor of the ankle joint. Sudden stretch of the tendon tissue can result in complete or partial rupture, with an estimated incidence of 8 to 18 per 100,000 persons. The demographic distribution is highly skewed, with Achilles rupture being significantly more common in men. Epidemiological studies have demonstrated a male-to-female ratio of up to 12:1, with a peak incidence occurring in the third to fifth decades of life. This demographic is often characterized by the "weekend warrior" phenomenon—individuals who engage in episodic, high-intensity athletic activities without consistent conditioning.
With complete rupture, the ruptured ends of the tendon may pull apart, leading to a significant plantarflexion weakness and to the creation of a gap that is palpated clinically. A common source of confusion is that patients may continue to have active ankle plantarflexion due to the action of other flexors of the ankle, specifically the tibialis posterior, flexor hallucis longus, flexor digitorum longus, and the peroneals. As a result, the diagnosis is initially missed in an estimated 20% to 25% of cases in the primary care or emergency department setting.

Pathogenesis and Natural History
Achilles ruptures are usually caused by noncontact injuries. Common injury mechanisms leading to Achilles rupture are forceful push-off with an extended knee, sudden unexpected ankle dorsiflexion, or violent dorsiflexion of a plantarflexed foot. These mechanisms generate eccentric loading forces that exceed the tensile strength of the tendon, which can endure loads up to ten times body weight during explosive plyometric activities. Achilles rupture can occur high, near the muscle-tendon juncture (9%), at the tendon midportion (72%), or at the calcaneal insertion (19%). Concomitant injuries such as ankle ligament sprains or ankle or tarsal fractures should be ruled out during the initial evaluation.
Most Achilles ruptures do not have any antecedent symptoms. A study of histologic scores comparing ruptured tendons with unruptured tendons, however, showed that there were significant histopathologic changes in the ruptured group that were not present in the older, asymptomatic, and unruptured group. These changes include mucoid degeneration, lipomatosis, and hypoxic degenerative tendinopathy. Therefore, tendinosis may play a role in predisposing the tendon to mechanical failure, but the extent of this role remains a subject of ongoing biomechanical research.

Surgical Anatomy and Biomechanics
Three calf muscles—the medial, lateral gastrocnemius, and soleus—converge together to form the triceps surae or the Achilles tendon. The gastrocnemius provides the power for explosive movements as it crosses both the knee and the ankle joints, whereas the soleus, which crosses only the ankle joint, is primarily responsible for postural control and sustained plantarflexion.
The plantaris muscle originates from the lateral femoral condyle and passes obliquely between the gastrocnemius and soleus to reside medial to the Achilles tendon and inserts into it or the calcaneus. In an anatomic study, the plantaris muscle was absent in 7.3% of specimens. When present, the plantaris can be a useful anatomical landmark during surgical exploration and is occasionally harvested for local autograft augmentation in chronic, neglected ruptures.


The triceps surae is formed by the convergence of the medial, lateral gastrocnemius, and soleus muscles. The Achilles tendon courses distally, rotates 90 degrees internally, the soleus contribution being medial to that of the gastrocnemius, and inserts into the middle third of the flat surface of the posterior calcaneal tuberosity. This 90-degree rotation is biomechanically significant as it produces a spiral configuration of the tendon fibers, which allows for elongation and elastic recoil, storing kinetic energy during the stance phase of gait.
The middle section of the tendon, 2 to 6 cm proximal to its insertion site, is a hypovascular zone. This zone is the narrowest in cross-section and corresponds to the most common site of tendon pathology, including paratenonitis, tendinosis, and tendon rupture. Blood supply to this region is derived from the musculotendinous junction proximally, the osseous insertion distally, and the extrinsic segmental vessels via the mesotenon.
The tendon is surrounded by a paratenon that has a single layer of cells with variable structure, not a true tenosynovium. The paratenon is highly vascularized and serves as the primary source of extrinsic blood supply to the tendon proper. Preservation of the paratenon during surgical intervention is paramount to minimize postoperative adhesions, optimize biologic healing, and reduce the risk of deep space infection.
Neurovascular Considerations
Webb et al documented the highly variable position of the sural nerve in relation to the Achilles tendon. As measured from the calcaneal insertion, the sural nerve crossed the tendon from medial to lateral at a mean distance of 9.8 cm, then coursed distally to lie a mean of 18.8 mm laterally. This anatomical relationship is of critical importance, particularly with the advent of percutaneous and minimally invasive surgical (MIS) techniques. Iatrogenic injury to the sural nerve can result in painful neuromas and lateral foot numbness, representing one of the most common complications of MIS Achilles repair.


Indications and Contraindications
The management of acute Achilles tendon ruptures remains one of the most debated topics in orthopedic surgery. The paradigm has shifted significantly over the last decade, moving away from a strict operative imperative toward a nuanced, shared decision-making model based on patient physiology, functional demands, and compliance with rigorous rehabilitation protocols.
Operative management is generally favored for younger, highly active individuals, elite athletes, and patients presenting with delayed diagnoses (greater than 2 to 4 weeks) where tendon retraction precludes successful conservative management. Non-operative management, combined with early functional rehabilitation, has shown equivalent functional outcomes and re-rupture rates in appropriately selected patients, while entirely avoiding surgical complications such as wound necrosis and iatrogenic nerve injury.
| Clinical Scenario | Operative Management | Non Operative Management |
|---|---|---|
| Patient Age and Activity | Young, high-demand athletes, manual laborers | Older, sedentary individuals, low functional demands |
| Timing of Presentation | Delayed presentation (> 3 weeks), chronic ruptures | Acute presentation (< 2 weeks) |
| Gap Size on Ultrasound | > 1 cm gap in resting equinus | Apposition of tendon ends in 20° of plantarflexion |
| Comorbidities | Healthy, non-smokers, no microvascular disease | Diabetes mellitus, peripheral vascular disease, active smoking |
| Compliance | Reliable for post-operative restrictions | Non-compliant or unable to manage functional bracing |
| Skin and Soft Tissue | Intact, healthy posterior ankle skin | Compromised soft tissue envelope, active local infection |
Absolute contraindications to surgical intervention include active systemic or local infection, severe peripheral arterial disease compromising the posterior tibial or peroneal angiosomes, and profound medical comorbidities precluding anesthesia. Relative contraindications include heavy tobacco use, poorly controlled diabetes mellitus, and advanced age with low functional demands.


Pre Operative Planning and Patient Positioning
Thorough preoperative planning begins with a meticulous clinical examination. The diagnosis of an acute Achilles tendon rupture is primarily clinical. The Thompson test (calf squeeze test) is the most reliable clinical sign; a lack of passive plantarflexion upon squeezing the gastrocnemius muscle belly indicates disruption of the musculotendinous unit. Additionally, the Matles test (increased resting dorsiflexion of the affected foot when the patient is prone with knees flexed to 90 degrees) and the presence of a palpable defect in the tendon substance are highly sensitive and specific.
Imaging Modalities
While the diagnosis is clinical, imaging can be utilized in equivocal cases or for preoperative planning. Dynamic musculoskeletal ultrasound is highly cost-effective and allows for real-time assessment of the tendon gap during passive range of motion. It is particularly useful in determining if the tendon ends appose in resting equinus, which may dictate the feasibility of non-operative management. Magnetic Resonance Imaging (MRI) is rarely indicated for acute ruptures but is invaluable for chronic, neglected ruptures to assess the degree of tendinosis, the extent of the gap, and the degree of fatty infiltration in the triceps surae muscle bellies.


Patient Positioning and Setup
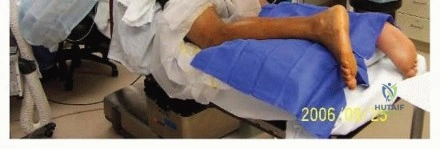
The patient is typically placed in the prone position on the operating table. General anesthesia or regional anesthesia (spinal or popliteal block) may be utilized. A thigh tourniquet is placed to provide a bloodless surgical field, though it should be inflated only after exsanguination and used judiciously to minimize ischemic time.
The feet must be allowed to hang freely over the edge of the operating table. This positioning is critical as it allows the surgeon to assess the resting tension of the uninjured contralateral limb (if prepped and draped) and match it during the repair of the injured tendon. Maintaining appropriate resting tension is the most critical biomechanical step in the procedure to prevent post-operative elongation and subsequent push-off weakness.
Detailed Surgical Approach and Technique
The surgical management of Achilles tendon ruptures can be broadly categorized into open, minimally invasive (MIS), and percutaneous techniques. The choice of technique depends on the surgeon's experience, the location of the rupture, and the chronicity of the injury.
Open Repair Technique
An open repair remains the gold standard, particularly for ruptures with significant mop-end fraying or those presenting with a delay. A longitudinal posteromedial incision is typically utilized. The incision is placed just medial to the palpable medial border of the Achilles tendon. This placement avoids the sural nerve laterally and prevents direct irritation of the surgical scar from shoe wear posteriorly.
Dissection is carried sharply through the skin and subcutaneous tissues. Meticulous hemostasis is achieved. The paratenon is identified and incised longitudinally. It is critical to elevate the paratenon as a distinct layer and preserve it for robust closure. Once the paratenon is opened, the hematoma is evacuated, and the ruptured tendon ends are exposed.


The degenerative, necrotic "mop-ends" of the tendon are conservatively debrided to healthy, organized collagen bundles. A core suture technique is then employed to reapproximate the tendon ends. The Krackow locking stitch is the most biomechanically sound and widely utilized configuration. Using heavy, non-absorbable, braided multi-filament suture (e.g., #2 or #5 FiberWire or Ethibond), two to three locking loops are placed in the proximal stump and similarly in the distal stump.
The ankle is placed in approximately 15 to 20 degrees of plantarflexion to match the resting tension of the contralateral side. The core sutures are tied securely. Following the core repair, an epitendinous running suture (e.g., 2-0 or 3-0 absorbable monofilament) is placed circumferentially around the repair site. This step smooths the repair, tucks in any protruding tendon fibrils, and enhances the overall biomechanical construct by reducing gap formation under cyclic loading.
Minimally Invasive and Percutaneous Techniques
Minimally invasive techniques, such as the Percutaneous Achilles Repair System (PARS) or the Achillon device, have gained significant popularity. These techniques utilize a small transverse or longitudinal incision directly over the rupture site. A specialized jig is introduced deep to the paratenon and superficial to the tendon. Needles are passed transversely through the jig, capturing the tendon proximally and distally.
The primary advantage of MIS techniques is the preservation of the soft tissue envelope and the hematoma, which contains osteoinductive and tenogenic factors crucial for biologic healing. The risk of major wound complications is significantly reduced. However, the surgeon must be acutely aware of the sural nerve anatomy. To mitigate the risk of sural nerve entrapment, the lateral tines of the jig and the lateral needle passes must be executed with the nerve's trajectory in mind, and sweeping the nerve laterally before needle passage is recommended.


Regardless of the technique, meticulous closure of the paratenon is mandatory. The paratenon is closed with a fine absorbable suture (e.g., 3-0 Vicryl). The subcutaneous tissue is closed in layers, and the skin is approximated with non-absorbable nylon or a subcuticular Monocryl stitch. The limb is subsequently placed in a well-padded short leg splint in 20 degrees of plantarflexion.
Complications and Management
Complications following Achilles tendon repair can be devastating and require prompt, aggressive management. The posterior ankle has a tenuous blood supply, and the thin soft tissue envelope makes wound complications a primary concern.
| Complication | Estimated Incidence | Etiology and Risk Factors | Salvage and Management Strategy |
|---|---|---|---|
| Infection / Wound Necrosis | 2% - 5% (Open) < 1% (MIS) | Smoking, diabetes, excessive retraction, poor paratenon closure | Aggressive serial debridement, negative pressure wound therapy, local rotational flaps or free tissue transfer. |
| Sural Nerve Injury | 5% - 10% (MIS) < 2% (Open) | Blind percutaneous passage of lateral sutures, variant anatomy | Initial observation for neuropraxia. Persistent symptomatic neuroma may require exploration, excision, and burying of the proximal stump into muscle. |
| Re-rupture | 2% - 4% | Non-compliance with rehab, premature return to sport, inadequate initial fixation | Revision surgery utilizing V-Y advancement, turn-down flaps, or Flexor Hallucis Longus (FHL) tendon transfer. |
| Tendon Elongation | 5% - 10% | Failure to tension appropriately during surgery, aggressive early stretching | Conservative management with orthotics. Severe cases with profound push-off weakness may require shortening osteotomy or FHL transfer. |
| Deep Vein Thrombosis (DVT) | 1% - 5% | Prolonged immobilization, hypercoagulable states | Chemical prophylaxis (LMWH or DOACs) based on risk stratification. Therapeutic anticoagulation if DVT is confirmed. |
Wound breakdown and deep infection are the most feared complications. Superficial necrosis may be managed with local wound care and oral antibiotics, but deep infection involving the tendon repair necessitates immediate surgical debridement. If a significant tendon defect is created post-debridement, reconstruction with an FHL transfer or allograft may be required once the infection is cleared.


Post Operative Rehabilitation Protocols
The postoperative rehabilitation of Achilles tendon ruptures has undergone a radical transformation. Historically, patients were casted in equinus for up to 8 weeks, leading to profound calf atrophy, joint stiffness, and poor functional outcomes. Contemporary evidence overwhelmingly supports early functional rehabilitation, which stimulates collagen synthesis, improves fiber alignment, and accelerates the return to pre-injury activity levels.
Phase 1 (0 to 2 weeks) focuses on wound healing and edema control. The patient is strictly non-weight-bearing in a plantarflexed splint. Elevation and strict adherence to non-weight-bearing status are critical to prevent early catastrophic failure of the repair.
Phase 2 (2 to 6 weeks) marks the transition to early functional mobilization. The splint is transitioned to a controlled ankle motion (CAM) boot equipped with heel wedges (typically three wedges, elevating the heel approximately 20 to 30 degrees). Patients are allowed progressive weight-bearing as tolerated in the boot. Active plantarflexion out of the boot is initiated to stimulate the musculotendinous unit, but active dorsiflexion past neutral is strictly prohibited to protect the healing repair from excessive tensile loads.
Phase 3 (6 to 12 weeks) involves progressive weaning from the heel wedges, typically removing one wedge every 1 to 2 weeks until the foot reaches neutral. The patient transitions to standard shoe wear with a small heel lift. Physical therapy focuses on concentric strengthening of the triceps surae, proprioceptive training, and gait normalization.
Phase 4 (3 to 6 months and beyond) focuses on eccentric strengthening, plyometrics, and sport-specific training. Return to competitive sports is generally not recommended until at least 6 months post-operatively, and only when the patient demonstrates symmetric calf strength, full range of motion, and the ability to perform single-leg heel raises without pain or fatigue.
Summary of Key Literature and Guidelines
The evolution of Achilles tendon management is heavily driven by high-quality prospective randomized controlled trials and meta-analyses. The landmark study by Willits et al. (JBJS, 2010) profoundly impacted the field by demonstrating that when an accelerated functional rehabilitation protocol is employed, there is no clinically important difference in re-rupture rates between
Clinical & Radiographic Imaging