INTRODUCTION TO SYNOVIAL AND SYSTEMIC ARTHROPATHIES OF THE HAND
The management of inflammatory conditions of the hand requires a profound understanding of tendon biomechanics, synovial pathophysiology, and the systemic nature of connective tissue disorders. Conditions ranging from isolated flexor tenosynovitis to complex systemic arthropathies—such as progressive systemic sclerosis (scleroderma), calcium pyrophosphate deposition (CPPD) disease, and tophaceous gout—present unique challenges to the orthopedic hand surgeon.
While initial management is frequently nonoperative, relying on targeted pharmacotherapy and corticosteroid injections, the progressive nature of these diseases often mandates precise surgical intervention. This masterclass delineates the evidence-based protocols for both the conservative and operative management of persistent synovitis, tenosynovitis, and the severe hand deformities associated with systemic arthropathies.
NONOPERATIVE TREATMENT OF SYNOVITIS AND TENOSYNOVITIS
Persistent tenosynovitis or arthritis characterized by obvious, recalcitrant swelling that persists for several weeks despite an adequate trial of nonsteroidal anti-inflammatory drugs (NSAIDs) warrants localized intervention. The cornerstone of nonoperative management in these refractory cases is the local injection of a corticosteroid preparation combined with a local anesthetic.
Indications and Biomechanical Considerations
Corticosteroid injections are highly efficacious in reducing synovial hypertrophy, thereby restoring the normal gliding mechanism of tendons within their retinacular sheaths. This treatment modality is especially applicable to:
* Stenosing Tenosynovitis (Trigger Finger): Reduces volume at the A1 pulley, alleviating the mechanical block to tendon excursion.
* Carpal Tunnel Syndrome (CTS): Decreases flexor tenosynovial volume within the rigid confines of the carpal canal, thereby reducing interstitial pressure on the median nerve.
* Trapeziometacarpal (CMC) Joint Osteoarthritis: Mitigates capsular inflammation and synovitis at the base of the thumb.
* Distal Interphalangeal (DIP) Joint Osteoarthritis: Provides symptomatic relief for acute inflammatory flares associated with Heberden's nodes.
* Proximal Interphalangeal (PIP) Joint Rheumatoid Arthritis: Offers temporary cessation of synovial proliferation, delaying the need for surgical synovectomy.
Clinical Pearl: While single or dual injections often yield dramatic relief, the response to repeated injections typically diminishes over time. Furthermore, repeated corticosteroid administration carries a documented risk of tendon attenuation, perilymphatic atrophy, and dermal depigmentation.
Transition to Surgical Intervention
If clinically significant synovitis and tenosynovitis persist after 4 to 6 months of adequate medical therapy and localized injections, surgical intervention is strongly indicated. Prolonged synovial proliferation leads to enzymatic degradation of the articular cartilage, attenuation of collateral ligaments, and eventual tendon rupture.
SURGICAL MANAGEMENT: SYNOVECTOMY AND TENOSYNOVECTOMY
When nonoperative measures fail, synovectomy or tenosynovectomy becomes necessary to halt disease progression and prevent structural failure.
Flexor Tenosynovectomy
Indications: Refractory flexor tenosynovitis, often seen in rheumatoid arthritis or CPPD, presenting with a "boggy" swelling in the palm or digits, restricted active flexion, and secondary carpal tunnel syndrome.
Patient Positioning and Preparation:
* The patient is positioned supine with the operative arm extended on a radiolucent hand table.
* A well-padded pneumatic tourniquet is applied to the proximal arm.
* Regional anesthesia (axillary or supraclavicular block) is preferred to allow for intraoperative assessment of the tenodesis effect, though general anesthesia may be utilized.
Surgical Approach (Step-by-Step):
1. Incision: Utilize a palmar zigzag (Brunner) incision over the affected digit, extending proximally into the palm if necessary. For carpal tunnel involvement, a standard longitudinal palmar incision in line with the radial border of the ring finger is utilized.
2. Exposure: Elevate full-thickness fasciocutaneous flaps. Identify and protect the neurovascular bundles bilaterally.
3. Sheath Access: Expose the flexor tendon sheath. The hypertrophic tenosynovium will often bulge through the thin cruciform pulleys.
4. Pulley Preservation: It is critical to preserve the A2 and A4 pulleys to prevent bowstringing. The A1, A3, and A5 pulleys may be vented or excised to facilitate access.
5. Excision: Meticulously excise the diseased tenosynovium from around the flexor digitorum superficialis (FDS) and flexor digitorum profundus (FDP) tendons. Use tenotomy scissors or a blunt dissector to strip the synovium while preserving the vincula (blood supply to the tendons).
6. Closure and Postoperative Protocol: Deflate the tourniquet, achieve meticulous hemostasis, and close the skin. Initiate early active range of motion (ROM) within 24 to 48 hours postoperatively to prevent tendon adhesions.
Surgical Warning: Aggressive tenosynovectomy that compromises the vincula brevia or longa can lead to avascular necrosis of the flexor tendons and subsequent spontaneous rupture. Always maintain a healthy respect for the dorsal aspect of the tendons where the vascular supply enters.
CRYSTAL DEPOSITION ARTHROPATHIES
Calcium Pyrophosphate Deposition (CPPD) Disease / Pseudogout
CPPD disease is characterized by the accumulation of calcium pyrophosphate crystals within articular and periarticular tissues. Clinically, it presents as intermittent acute attacks that closely resemble acute gouty arthritis.
Clinical Manifestations in the Hand:
* Flexor Tenosynovitis: CPPD can cause severe, acute flexor tenosynovitis, rapidly leading to acute carpal tunnel syndrome due to volume expansion within the carpal canal.
* Radiographic Findings: Routine radiographs frequently reveal chondrocalcinosis—visible as opaque, stippled areas in the articular cartilage or, classically, within the fibrocartilaginous disc of the triangular fibrocartilage complex (TFCC) at the distal radioulnar joint.
Diagnosis and Management:
Definitive diagnosis is established by the identification of weakly positively birefringent, rhomboid-shaped calcium pyrophosphate crystals in the joint aspirate under polarized light microscopy. The primary treatment of pseudogout is medical (NSAIDs, colchicine, intra-articular corticosteroids). Surgical intervention is reserved for acute compressive neuropathies (e.g., urgent carpal tunnel release) or advanced joint destruction requiring arthrodesis or arthroplasty.
Gouty Arthritis
Gout results from the deposition of monosodium urate crystals in joints and soft tissues, leading to intense inflammatory responses. In chronic tophaceous gout, heavy calcium urate deposits can cause severe, grotesque deformities of the digits, destroying subchondral bone and attenuating extensor mechanisms.
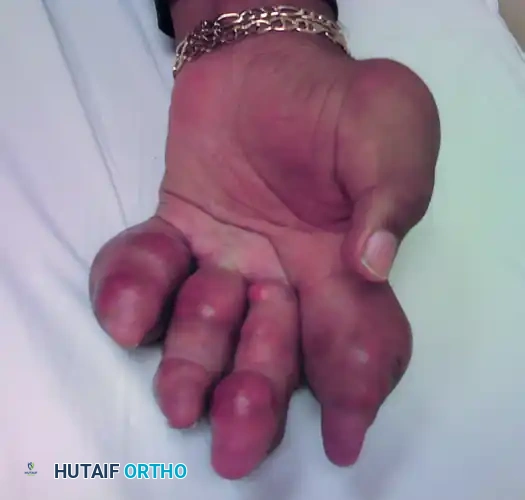
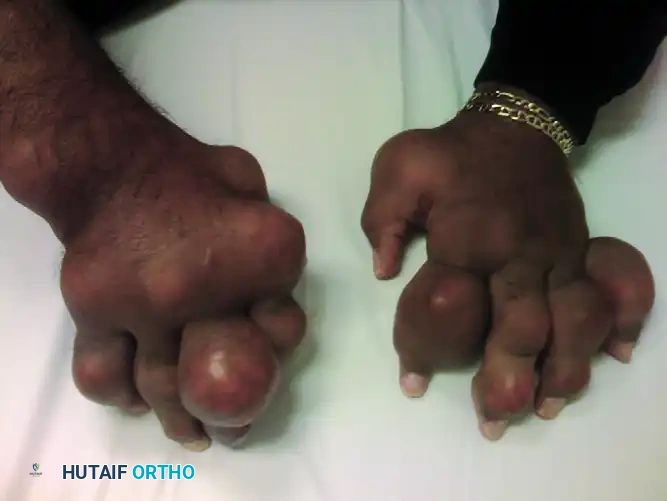
FIGURE 73-7 Severe gout in multiple joints of the hand of a 54-year-old man. Heavy calcium urate deposits have caused severe deformities of all fingers.
Surgical Management of Tophaceous Gout:
Surgery is indicated when tophi cause skin necrosis, intractable pain, severe functional impairment, or nerve compression.
* Debulking: Careful excision of the chalky, white urate deposits. Complete eradication is often impossible without sacrificing vital structures; therefore, the goal is functional debulking and skin preservation.
* Joint Salvage vs. Ablation: In cases of complete joint destruction (as seen in the severe deformities above), arthrodesis or ray amputation may be required to restore a functional, albeit modified, hand architecture.
SCLERODERMA (PROGRESSIVE SYSTEMIC SCLEROSIS)
Scleroderma is a complex autoimmune disease characterized by microvascular hyperreactivity, immune dysregulation, and progressive fibrosis of the skin and internal organs. The age at onset is typically older than 40 years.
Classification
Two primary types of scleroderma are recognized, both of which have profound implications for the hand surgeon:
1. Diffuse Scleroderma (Progressive Systemic Sclerosis): Usually more severe, affecting the proximal extremities and the trunk. It involves not only the skin but also critical internal organs, including the gastrointestinal tract (especially the esophagus), heart, lungs, and kidneys. Telangiectasia is frequently observed.
2. CREST Syndrome: A limited cutaneous form of systemic sclerosis. The acronym stands for:
* Calcinosis cutis
* Raynaud phenomenon
* Esophageal motility disturbance
* Sclerodactyly
* Telangiectasia
Clinical Manifestations in the Hand
Hand surgeons frequently evaluate these patients for complications arising from microvascular ischemia and soft tissue fibrosis.
* Raynaud Phenomenon: Episodic vasospasm causing digital ischemia, often the presenting symptom.
* Calcinosis Cutis: Painful calcium deposits, typically at the fingertips or over extensor surfaces, which may ulcerate and exude a chalky white material.
* Arthritic Involvement: Causes severe finger contractures. Notably, unlike rheumatoid arthritis, synovial thickening is minimal.
* Tendon Involvement: Fibrosis of the hand tendons and tendon sheaths produces a palpable tendon friction rub or a distinct leathery crepitus during active motion. This must be clinically distinguished from the coarse, gritty crepitus palpable in osteoarthritis.
* Extensor Tendon Rupture: As the extensor tendons become attenuated over the PIP joints due to friction and tight overlying skin, they may rupture. The ischemic skin frequently breaks down, exposing the joint.
SURGICAL MANAGEMENT OF SCLERODERMA COMPLICATIONS
Surgical intervention in scleroderma is fraught with complications, primarily due to the severe underlying vasculopathy. Wound healing is notoriously poor. Surgery is generally reserved for limb-threatening ischemia, intractable pain, or severe functional deficits.
Distal Interphalangeal (DIP) Joint Interventions
Changes at the DIP joint are often the most severe, including chronic skin ulceration, fixed joint contracture, dry gangrene, and secondary osteomyelitis. The usual surgical choices for these end-stage changes at the distal joint are amputation and arthrodesis.
1. Terminal Amputation:
* Indications: Dry gangrene, osteomyelitis of the distal phalanx, or painful, non-healing ischemic ulcers that have failed conservative management (e.g., iloprost infusions, sympathectomy).
* Technique: Performed under digital block (without epinephrine). The level of amputation is dictated by tissue viability. Bone is rongeured back to allow tension-free closure of the skin flaps. If primary closure is impossible due to skin tightness, the wound may be allowed to heal by secondary intention to avoid compromising the tenuous microcirculation.
2. DIP Joint Arthrodesis:
* Indications: Painful instability or severe fixed flexion contracture with viable overlying skin.
* Technique:
* A dorsal H-shaped or transverse incision is made.
* The extensor tendon is divided, and the collateral ligaments are excised to expose the joint.
* The articular cartilage is resected using a cup-and-cone reamer or oscillating saw to expose bleeding subchondral bone.
* The joint is positioned in 0 to 10 degrees of flexion.
* Fixation is typically achieved using a headless compression screw (if bone stock permits) or crossed 0.045-inch Kirschner wires.
* Postoperative Care: Immobilization for 6 to 8 weeks. Union rates may be delayed in scleroderma patients due to compromised vascularity.
Proximal Interphalangeal (PIP) Joint Interventions
At the PIP joint, scleroderma changes lead to severe flexion contractures. Because the severe contracture of all volar structures (skin, fascia, flexor sheath, volar plate) limits extension, soft tissue releases are rarely successful and often result in skin necrosis.
PIP Joint Arthrodesis:
* When the PIP joint is exposed due to extensor tendon rupture and skin breakdown, or when flexion contractures render the digit useless, arthrodesis is the procedure of choice.
* The joint is shortened significantly through bone resection to allow the tight, sclerotic skin to close without tension.
* The index and middle fingers are typically fused in 30 to 40 degrees of flexion, while the ring and small fingers are fused in 40 to 50 degrees to facilitate grip.
Clinical Pearl: In scleroderma patients, never attempt to lengthen the digit or correct a severe contracture to full extension. The digital arteries are fibrotic and inelastic; acute extension will result in immediate vascular compromise and digital loss. Always shorten the skeleton to accommodate the soft tissue envelope.
Management of Calcinosis Cutis
Surgical excision of calcinosis is indicated when deposits cause severe pain, recurrent infection, or mechanical block to motion.
* Technique: Meticulous dissection is required. The deposits are often intimately involved with the dermis and neurovascular bundles. High-loop magnification is essential. Avoid aggressive curettage that might damage adjacent ischemic digital nerves.
POSTOPERATIVE PROTOCOLS AND REHABILITATION
Rehabilitation following hand surgery in patients with systemic arthropathies requires a delicate balance between mobilizing joints to prevent stiffness and protecting tenuous soft tissue repairs.
- Wound Care: In scleroderma and severe rheumatoid patients, sutures should be left in place longer than the standard 10-14 days (often up to 21 days) due to delayed wound healing.
- Edema Control: Compressive dressings must be used with extreme caution in patients with Raynaud phenomenon or vasculopathy to avoid precipitating digital ischemia.
- Mobilization: Following tenosynovectomy, early active motion is critical. A dorsal blocking splint may be utilized if flexor pulleys were reconstructed, but active flexion within the splint should commence immediately.
- Thermotherapy: Patients with scleroderma benefit from warm water soaks prior to therapy sessions to induce vasodilation and improve tissue compliance, strictly avoiding cold therapy which can trigger severe vasospasm.
