Introduction & Epidemiology
Middle-third clavicle fractures represent a substantial portion of orthopedic trauma, accounting for 2-10% of all fractures and 45-80% of all clavicle fractures. The clavicle is the most commonly fractured bone in the adult population. Its subcutaneous location and biomechanical role as a strut connecting the axial skeleton to the upper extremity render it vulnerable to injury. These fractures exhibit a bimodal distribution, with a high incidence in young, active males (due to high-energy trauma) and in elderly females (often associated with osteoporosis and low-energy falls).
The mechanism of injury is typically a direct blow to the superior aspect of the shoulder, or an indirect force transmitted through the arm (e.g., fall onto an outstretched hand or directly onto the shoulder). Associated injuries, though uncommon for isolated midshaft fractures, can include scapular fractures, rib fractures, pneumothorax, brachial plexus injury, or subclavian vessel compromise, particularly in high-energy trauma or highly displaced fractures. A thorough neurovascular examination is paramount in the initial assessment.
Historically, the vast majority of middle-third clavicle fractures were managed non-operatively with good results. However, growing evidence highlighting higher rates of malunion and symptomatic nonunion, particularly in significantly displaced and comminuted fractures, has shifted the treatment paradigm towards operative fixation for select indications. This document aims to provide an exhaustive academic review of the classification, treatment rationale, and strategies for optimizing outcomes in middle-third clavicle fractures.
Surgical Anatomy & Biomechanics
The clavicle is a unique S-shaped long bone, acting as a strut that maintains the length of the shoulder girdle and provides attachment for numerous muscles and ligaments. Its subcutaneous position along its entire length makes it susceptible to direct trauma and allows for easy palpation of fracture deformities.
Bony Anatomy
The clavicle has a medial (sternal) end, a shaft (middle third), and a lateral (acromial) end. The middle third is the thinnest and most acutely curved portion, predisposing it to fracture.
*
Medial Third:
Round and articulates with the manubrium via the sternoclavicular joint.
*
Middle Third (Shaft):
Typically prismatic, becoming flatter laterally. It lacks a medullary canal, instead containing cancellous bone and trabeculae, which has implications for intramedullary nailing.
*
Lateral Third:
Flat and articulates with the acromion via the acromioclavicular joint.
Muscular Attachments
Crucial muscle attachments influence fracture displacement patterns:
*
Sternocleidomastoid:
Originates from the medial clavicle and sternum, inserts onto the mastoid process. Its pull on the medial fragment causes superior displacement.
*
Pectoralis Major:
Originates from the medial clavicle and sternum, inserts onto the humerus. Contributes to medial fragment stability but also contributes to shortening.
*
Deltoid:
Originates from the lateral clavicle and acromion, inserts onto the deltoid tuberosity of the humerus. Its weight and pull on the lateral fragment cause inferior displacement.
*
Trapezius:
Originates from the occiput, nuchal ligament, and thoracic vertebrae, inserts onto the lateral clavicle and acromion. Provides superior support to the lateral fragment, though its effect is often overwhelmed by the deltoid and arm weight in displaced fractures.
*
Subclavius:
Originates from the first rib, inserts onto the inferior surface of the clavicle. Offers some protection to underlying neurovascular structures.
Ligamentous Attachments
The primary ligamentous stabilizers for midshaft fractures are the coracoclavicular ligaments and the costoclavicular ligament.
*
Coracoclavicular Ligaments:
Comprising the conoid and trapezoid ligaments, these connect the clavicle (conoid tubercle, trapezoid line) to the coracoid process of the scapula. While critical for the stability of lateral third fractures, their integrity
usually
remains intact with midshaft fractures, as they typically attach to the lateral fragment. If the fracture extends medially to their attachment, the lateral fragment's displacement will be significantly altered.
*
Costoclavicular Ligament (Rhomboid Ligament):
Connects the medial clavicle to the first rib. Provides stability to the sternoclavicular joint and medial clavicle.
Neurovascular Structures
Posterior and inferior to the clavicle lie vital neurovascular structures:
*
Subclavian Artery and Vein:
Pass beneath the clavicle and over the first rib.
*
Brachial Plexus:
Runs posterior to the subclavian vessels.
These structures are at risk during severe displacement of fracture fragments, particularly posteriorly, and during surgical dissection.
Biomechanics of Displacement
Fractures of the middle third clavicle typically demonstrate characteristic displacement patterns:
*
Medial Fragment:
Pulled superiorly by the sternocleidomastoid muscle.
*
Lateral Fragment:
Pulled inferiorly by the weight of the arm and the deltoid muscle, and medially by the pectoralis major and latissimus dorsi, leading to significant shortening and overriding.
Understanding these forces is crucial for achieving anatomical reduction during operative fixation.
Indications & Contraindications
The decision to treat middle-third clavicle fractures operatively versus non-operatively is guided by several factors, including fracture morphology, patient characteristics, and associated injuries. While non-operative management historically predominated, modern literature increasingly supports operative intervention for specific indications to improve functional outcomes and reduce rates of symptomatic malunion and nonunion.
Classification Systems
While numerous systems exist, the
Edinburgh classification
is particularly relevant for midshaft fractures:
*
Type 2 (Midshaft):
This is the focus.
*
Type 2A:
Undisplaced or minimally displaced.
*
Type 2B:
Displaced.
*
Type 2B1:
Simple (two parts).
*
Type 2B2:
Comminuted (three or more parts).
Other descriptive factors include fracture shortening (>2 cm), cortical apposition (<50% or 100% displacement), degree of comminution, and displacement (superior/inferior, anterior/posterior).
Indications for Operative vs. Non-Operative Management
The following table summarizes common indications for operative and non-operative management. It is important to note that many indications for operative treatment are relative, requiring clinical judgment and shared decision-making with the patient.
| Feature / Indication | Operative Management | Non-Operative Management | Non-Operative Management |
|
Primary Indications
|
Fracture displacement:
Complete loss of cortical apposition between fracture fragments. |
|
Primary Indications
|
Displacement:
Complete offset of the bone ends (100% cortical displacement). | |
| |
Indications for Operative Management
|
Non-Operative (Conservative) Management
|
|
Fracture Characteristics
| Complete displacement (100% cortical offset). |
Indications for Operative Treatment
| | | | | | | | | | | |

Contraindications for Operative Treatment
Absolute contraindications are rare and typically relate to the patient's overall medical condition or local factors precluding safe surgery.
*
Absolute Contraindications:
* Active local infection.
* Severe overlying soft tissue compromise (e.g., open fracture with significant contamination, severe burns).
* Unstable medical comorbidities precluding safe anesthesia and surgery.
* Non-displaced fracture in a patient with significant medical comorbidities.
*
Relative Contraindications:
* Patient preference for non-operative management after informed consent regarding risks/benefits of both options.
* Minimal displacement or shortening with good cortical apposition.
* Significant osteoporosis with poor bone quality that may not hold hardware securely.
* Smokers or patients with other factors known to impede bone healing (e.g., diabetes, poor nutrition), which may increase nonunion rates post-operatively, though these are often also considered indications for surgery to maximize union potential.
* Young, skeletally immature patients (non-operative often preferred due to remodeling potential).
Pre-Operative Planning & Patient Positioning
Careful pre-operative planning is essential to ensure a smooth surgical procedure, appropriate implant selection, and optimal patient outcomes.
Pre-Operative Assessment and Imaging
-
Clinical Evaluation:
- Thorough history (mechanism of injury, handedness, previous shoulder injuries, comorbidities, medications, smoking/alcohol history).
- Detailed physical examination: Inspect for skin integrity, ecchymosis, swelling. Palpate the clavicle for tenderness and deformity. Assess shoulder range of motion (active and passive, limited by pain). Crucially, perform a neurovascular assessment of the ipsilateral upper extremity, including brachial plexus function (axillary, musculocutaneous, radial, ulnar, median nerves) and distal pulses (radial, ulnar). Any deficits warrant immediate investigation (e.g., CT angiogram).
-
Radiographic Evaluation:
-
Standard Clavicle Series:
- Anteroposterior (AP) view: Provides initial assessment of displacement, shortening, and comminution.
- 30-degree cephalic tilt view: Projects the clavicle off the underlying thoracic cage, allowing for better visualization of the fracture pattern and displacement. This is often the most critical view.
- Axillary lateral view (optional but helpful): Can demonstrate anterior/posterior displacement.
-
Computed Tomography (CT) Scan:
Indicated for:
- Complex comminution, particularly if articular involvement (sternal or acromial end) is suspected.
- Confirmation of significant posterior displacement or suspected neurovascular impingement.
- Evaluation for associated injuries (e.g., scapular fracture, rib fractures, hemopneumothorax).
- 3D Reconstructions from CT: Aid in visualizing complex fracture patterns and planning implant contouring.
-
Standard Clavicle Series:
Implant Selection and Templating
-
Plating Systems:
- Precontoured Locking Compression Plates (LCPs): These are the gold standard for clavicle fixation. They provide angular stability, which is particularly advantageous in comminuted fractures or osteopenic bone. Plate length and screw trajectory are optimized for the clavicular anatomy.
- Plate Material: Titanium is preferred due to its lower profile and biocompatibility, reducing hardware prominence and irritation compared to stainless steel.
-
Plate Placement:
- Superior Plating: Offers superior biomechanical strength against bending and torsional forces due to direct counteraction of muscle forces. However, hardware prominence is a common issue given the subcutaneous location.
- Anteroinferior Plating: Less hardware prominence. While biomechanically shown to be slightly weaker in some cadaveric studies, clinical outcomes are often comparable to superior plating, with potentially lower rates of symptomatic hardware. Careful contouring is critical for optimal fit. The optimal position is often cited as a neutral zone on the anterior cortex, approximately 10-15mm inferior to the superior cortex, or along the anterior-inferior border.
-
Screw Selection:
- Typically, 3.5mm locking and cortical screws are used.
- At least 3 bicortical screws are recommended on each side of the fracture, ideally 6 cortices.
- Lag screws can be used through the plate to achieve interfragmentary compression in simple fracture patterns.
- Templating: Using radiographic images and implant templates, surgeons can pre-plan plate length, anticipated contour, and screw trajectories to ensure adequate fixation and avoid critical structures.
Anesthesia and Pain Management
- General Anesthesia: Typically used.
- Regional Anesthesia: An interscalene brachial plexus block can be a valuable adjunct for both intraoperative and postoperative pain control, reducing opioid requirements.
Patient Positioning
Proper positioning is critical for optimal surgical exposure and to facilitate fracture reduction.
1.
Beach Chair Position:
*
Advantages:
Excellent exposure of the entire clavicle, allows for easy manipulation of the ipsilateral arm for reduction, and permits visualization of the shoulder girdle's overall alignment. Minimizes blood loss.
*
Technique:
Patient is positioned semi-recumbent (30-60 degrees of trunk elevation). The head is supported and turned away from the operative side. The ipsilateral arm is draped free or supported on an arm board. A small bump (e.g., a rolled towel or blanket) placed longitudinally beneath the ipsilateral scapula can protract the scapula and bring the clavicle anteriorly, improving exposure and facilitating reduction.
2.
Supine Position:
*
Advantages:
Simpler setup.
*
Technique:
Patient is supine. A bolster or rolled blanket is placed longitudinally along the spine, extending from the head to the iliac crest. This extends the neck and retracts the shoulders posteriorly, bringing the clavicle into a more prominent and accessible position. The head is turned away from the operative side. The ipsilateral arm can be draped free.
*
Draping:
A sterile field should encompass the entire ipsilateral shoulder, arm (often to the hand to allow for manipulation), and extending onto the chest and neck. This allows for clear visualization of anatomical landmarks and manipulation of the arm during reduction.

Detailed Surgical Approach / Technique
Operative fixation of middle-third clavicle fractures typically involves open reduction and internal fixation (ORIF) with a precontoured locking plate. The goal is anatomical reduction, restoration of length, rotation, and alignment, and stable fixation to allow for early rehabilitation and optimal union.
Incision
The choice of incision depends on surgeon preference, fracture complexity, and cosmetic considerations.
*
Transverse (Saber) Incision:
*
Description:
A slightly curved incision, typically 4-8 cm in length, centered over the fracture site and following Langer's lines.
*
Advantages:
Excellent cosmetic outcome, follows skin tension lines.
*
Disadvantages:
May limit exposure for highly comminuted or widely displaced fractures, particularly if extending to the medial or lateral ends.
*
Longitudinal Incision:
*
Description:
An incision directly along the superior border of the clavicle, centered over the fracture.
*
Advantages:
More extensile exposure, particularly useful for complex fractures or revision surgery.
*
Disadvantages:
Less cosmetic, higher risk of hypertrophic scarring.
*
Recommendation:
For most midshaft fractures, a slightly curved transverse incision generally provides adequate exposure and superior cosmesis.
Dissection and Exposure
- Skin and Subcutaneous Tissue: Incise the skin and subcutaneous tissues. Identify and carefully preserve the supraclavicular nerves traversing the operative field, if possible. Patients should be counselled pre-operatively about potential numbness or dysesthesia in the distribution of these nerves regardless of attempts at preservation.
- Platysma Muscle: The platysma muscle may be encountered and should be sharply incised along its fibers or carefully retracted to expose the deep fascia overlying the clavicle.
- Deep Fascia: Incise the deep fascia longitudinally along the superior border of the clavicle.
- Subperiosteal Dissection: This should be minimized to preserve the periosteal blood supply, which is critical for bone healing. Use fine dissection to expose the fracture fragments. Elevate the periosteum only as much as necessary to facilitate reduction and plate application. For highly comminuted fractures, a more limited subperiosteal exposure (e.g., "biological fixation") is preferable to preserve vascularity.
Fracture Reduction
Restoration of length, alignment, and rotation is paramount for functional recovery.
1.
Debridement:
Remove any hematoma or small, devitalized bone fragments from the fracture site that may impede reduction. Larger, well-vascularized fragments should be preserved.
2.
Indirect Reduction:
* Often the first attempt. Apply gentle traction to the ipsilateral arm in line with the clavicle.
* Manipulation of the arm (flexion, extension, rotation, abduction) can help bring the lateral fragment into alignment with the medial fragment.
* A bump under the scapula (in beach chair) can also aid in bringing the lateral fragment superiorly.
3.
Direct Reduction:
*
Medial Fragment:
The sternocleidomastoid typically pulls the medial fragment superiorly. Counteract this by applying downward pressure or by using a periosteal elevator as a lever.
*
Lateral Fragment:
Often displaced inferiorly and medially. Apply upward and lateral traction.
*
Reduction Instruments:
*
Pointed Reduction Clamps:
Essential for bringing fragments together and maintaining reduction. Apply carefully to avoid excessive soft tissue stripping.
*
Bone-holding Forceps:
For larger fragments.
*
Hohmann Retractors/Periosteal Elevators:
Can be used as levers to disimpact and reduce fragments.
*
"Joy-stick" K-wires:
Inserting a small K-wire into each main fragment can provide leverage for manipulating and rotating them into anatomical alignment, especially useful for severely displaced fragments or comminuted patterns.
*
Rotational Alignment:
Crucial but often overlooked. Ensure the superior and inferior cortical surfaces are correctly oriented. The clavicle has a natural S-curve; ensure this morphology is restored.
4.
Temporary Fixation:
Once anatomical reduction is achieved, maintain it with temporary K-wires (inserted carefully to avoid neurovascular structures) or additional reduction clamps.
Plate Application and Definitive Fixation
- Plate Contouring: Select a precontoured locking plate. While precontoured, minor adjustments may be necessary to ensure a perfect fit onto the superior or anteroinferior surface of the clavicle. The plate should span the fracture site adequately, providing sufficient purchase in both the medial and lateral fragments.
-
Plate Position:
- Superior Plating: Position the plate centrally on the superior surface of the clavicle. This offers maximal biomechanical stability.
- Anteroinferior Plating: Position the plate on the anterior or anteroinferior surface. This reduces prominence but requires precise contouring to match the clavicular curvature.
-
Screw Insertion:
- Distal and Proximal Screws: Secure the plate to the most distal and proximal fragments first, using at least two screws in each main fragment (one locking, one cortical, or two locking). This establishes the length and initial stability. Aim for at least 3 bicortical screws per main fragment, total of 6 cortices.
- Lag Screw (if applicable): For simple, oblique fractures, a lag screw placed through the plate or separately (ahead of the plate) can achieve excellent interfragmentary compression, significantly enhancing stability.
- Locking Screws: Provide angular stability and are particularly useful in comminuted fractures or osteopenic bone, preventing pull-out. They do not provide compression directly across the fracture gap.
- Cortical Screws: Provide compression across the plate-bone interface and can be used to generate interfragmentary compression if desired before locking screws are placed.
- Avoidance of Neurovascular Structures: All screws must be bicortical to maximize purchase. Prioritize screw placement in the central and lateral portions of the clavicle, as the medial third has a higher risk of penetrating vital structures (subclavian vessels, brachial plexus, pleura). Measure screw length meticulously and ensure gentle advancement. Use fluoroscopy intermittently to confirm screw trajectory and length, especially medially.
- Comminuted Fractures: For highly comminuted fractures, the principle is bridging osteosynthesis. The plate acts as an extramedullary splint, restoring overall length and alignment without necessarily achieving anatomical reduction of every small fragment. Avoid excessive stripping of comminuted fragments to preserve their blood supply. Bone graft (autograft or allograft) may be considered if there is a large bone defect or significant comminution increasing the risk of nonunion.

Wound Closure
- Hemostasis: Ensure meticulous hemostasis.
- Drain: A small closed suction drain (e.g., Jackson-Pratt) may be placed, particularly if a large hematoma is anticipated, though it is not always necessary.
-
Layered Closure:
- Repair the deep fascia (over the clavicle) if possible.
- Repair the platysma muscle (if incised) to prevent hypertrophic scarring and provide an additional layer of closure.
- Close subcutaneous tissue and skin with absorbable sutures and/or skin staples/sutures.
- Apply sterile dressing.
Complications & Management
Despite advancements in surgical techniques, complications can arise following operative management of middle-third clavicle fractures. Understanding their incidence and appropriate management is crucial.
| Complication | Incidence | Management / Salvage Strategies | |
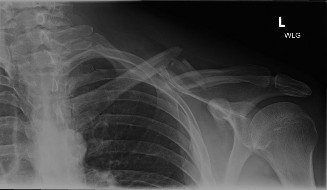
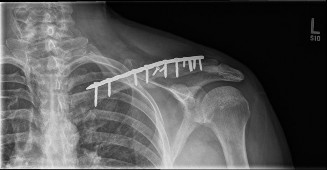
Clinical & Radiographic Imaging