Patient Presentation & History
A 78-year-old male presented to the emergency department following a ground-level fall at home. He reported immediate onset of severe left hip pain and an inability to bear weight on the affected limb. He was found lying on the floor by his spouse approximately one hour after the fall. The mechanism described was a simple slip on a rug, resulting in direct impact to the left hip.
His medical history is significant for:
* Hypertension (managed with Amlodipine 5mg OD)
* Type 2 Diabetes Mellitus (managed with Metformin 1000mg BID, HbA1c 7.1%)
* Atrial Fibrillation (on Apixaban 5mg BID)
* Chronic Kidney Disease Stage 3a (eGFR 52 mL/min/1.73m²)
* Osteoporosis (diagnosed 3 years prior, not on specific anti-resorptive therapy)
* Previous right total knee arthroplasty 5 years ago.
He lives independently with his wife and is usually ambulatory with a cane for longer distances. Social history includes being a retired school teacher, non-smoker, and occasional alcohol consumer. He denies any prodromal symptoms such as syncope, dizziness, or chest pain prior to the fall.
Clinical Examination
Upon arrival, the patient was conscious, alert, and in acute distress due to pain.
*
Inspection:
The left lower extremity was noticeably shortened and held in an externally rotated position compared to the right. There was ecchymosis noted over the greater trochanter and lateral thigh, with diffuse swelling around the hip joint. No open wounds or skin tenting were observed.
*
Palpation:
Tenderness was elicited over the greater trochanter and groin region on the left. Crepitus was palpable with gentle manipulation, but further extensive palpation was avoided due to patient discomfort and suspected fracture. Peripheral pulses (femoral, popliteal, dorsalis pedis, posterior tibial) were palpable and symmetrical bilaterally. Capillary refill was brisk in all digits.
*
Range of Motion (ROM):
Active ROM of the left hip was severely limited due to pain. Passive ROM was attempted cautiously, revealing markedly restricted internal rotation, adduction, and flexion. Any attempt at hip movement exacerbated pain. Knee and ankle ROM were full and painless.
*
Neurological Assessment:
Sensation was intact to light touch and pinprick in all dermatomes of the left lower extremity (L1-S1). Motor strength was difficult to assess accurately due to pain, but gross ankle dorsiflexion and plantarflexion, and toe movements were present and symmetrical. Patellar and Achilles reflexes were 2+ bilaterally.
*
Systemic Examination:
Cardiopulmonary examination was unremarkable. Abdominal examination revealed no tenderness or organomegaly.
Imaging & Diagnostics
Initial imaging in the emergency department included standard radiographs of the left hip and pelvis.
-
Radiographic Findings:
- Anteroposterior (AP) pelvis view demonstrated a comminuted fracture involving the intertrochanteric region of the left femur. The fracture line extended from the greater trochanter inferiorly and medially, with significant comminution of the posteromedial cortex, specifically the lesser trochanter. There was proximal migration of the femoral shaft relative to the head-neck segment, indicating an unstable fracture pattern.
- AP view of the left hip confirmed the intertrochanteric fracture with significant comminution.
- Lateral view of the left hip further delineated the comminution, particularly posteriorly, and highlighted the degree of external rotation and shortening.
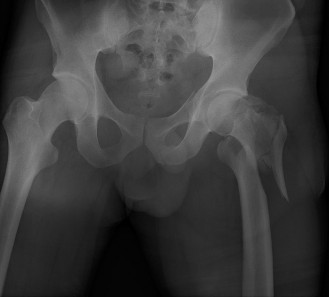
(Representative image of an intertrochanteric femur fracture, demonstrating typical comminution and displacement.) -
Classification: Based on the radiographs, the fracture was classified as an AO/OTA 31-A2.2 fracture (multifragmentary, lateral wall intact, but with significant posterior/medial comminution including the lesser trochanter), indicating an unstable pattern. It would also be classified as an unstable intertrochanteric fracture by Evans-Jensen criteria due to the posteromedial comminution and greater trochanter involvement.
- CT Scan Indication: A CT scan was considered given the comminution, primarily to better define the posteromedial cortex and lateral wall integrity, and for precise surgical planning and templating, though it was ultimately deemed unnecessary for this typical unstable pattern, given clear radiographic findings. CT may be more routinely indicated for atypical fracture patterns, pathological fractures, or when plain radiographs are inconclusive for characterising the true extent of comminution or fracture lines (e.g., reverse obliquity).
- Templating: Pre-operative templating using digital radiographs was performed to estimate appropriate intramedullary nail length, diameter, and optimal lag screw/blade position within the femoral head. Key measurements included trochanteric entry point to just proximal to the femoral condyles for nail length, and femoral head diameter for lag screw length and position (aiming for central-inferior in AP and central in lateral views).
-
Laboratory Investigations:
- Complete Blood Count (CBC): Hb 13.2 g/dL, WBC 9.8 x 10^9/L, Platelets 280 x 10^9/L.
- Basic Metabolic Panel: Na 138 mEq/L, K 4.1 mEq/L, Cr 1.6 mg/dL (elevated from baseline, likely due to dehydration), BUN 28 mg/dL.
- Coagulation Profile: INR 1.9 (on Apixaban, requiring reversal/bridging strategy), PTT 32s.
- Type & Crossmatch: Four units of packed red blood cells were crossmatched.
- ECG: Revealed controlled atrial fibrillation, no acute ischemic changes.
- Chest X-ray: No acute cardiopulmonary pathology.
Differential Diagnosis
The acute presentation of hip pain and inability to bear weight following a fall in an elderly patient mandates consideration of several hip region injuries.
| Feature | Intertrochanteric Femur Fracture (AO/OTA 31-A) | Femoral Neck Fracture (AO/OTA 31-B) | Subtrochanteric Femur Fracture (AO/OTA 32-A/B/C) | Pelvic Ring Injury (AO/OTA 61-A/B/C) |
|---|---|---|---|---|
| Location | Between greater and lesser trochanters | Intracapsular, just distal to articular surface to intertrochanteric line | Distal to lesser trochanter, up to 5cm distal | Involving ilium, ischium, pubis, sacrum, sacroiliac joints |
| Mechanism | Low-energy fall in elderly; high-energy trauma in younger | Low-energy fall in elderly; high-energy trauma in younger | High-energy trauma; atypical in osteoporotic patients (bisphosphonates) | High-energy trauma; rarely low-energy in elderly with severe osteoporosis |
| Clinical Exam | Shortened, externally rotated limb; diffuse hip/trochanteric pain | Shortened, externally rotated limb; groin pain; sometimes minimal deformity with impacted # | Significant deformity, pain along proximal thigh; often significant blood loss | Pelvic instability, bruising in groin/perineum, leg length discrepancy (often rotational) |
| Radiographic Features | Extracapsular. Fracture lines through cancellous bone. Comminution of lesser/greater trochanter common. | Intracapsular. Displaced, non-displaced, impacted. Garden/Pauwel's classifications. | Fracture line typically transverse or short oblique. Often involves lateral cortex. Spiral component possible. | Disruption of pelvic ring (anterior/posterior). Symphysis diastasis, sacral fx, SI joint disruption. |
| Blood Supply Risk | Excellent, due to extracapsular location | High risk of avascular necrosis (AVN) due to intracapsular nature | Typically good, but soft tissue stripping can compromise | Dependent on fracture pattern; retroperitoneal hemorrhage common |
| Typical Treatment | Intramedullary nailing (PFN, Gamma nail, TFN) or DHS with barrel plate | Internal fixation (cannulated screws) for non-displaced/young. Hemiarthroplasty/THA for displaced/elderly. | Intramedullary nailing (cephalomedullary or reconstruction nail) | Non-operative for stable. Operative for unstable (anterior/posterior fixation). |
| Prognosis | Good union rates with appropriate fixation. Complications: cut-out, non-union, malunion, infection | AVN, non-union, malunion, infection, post-traumatic arthritis | Non-union, malunion, hardware failure | Instability, chronic pain, neurological deficits, persistent gait dysfunction |
Surgical Decision Making & Classification
Given the patient's age, medical comorbidities, and the unstable nature of the intertrochanteric femur fracture, surgical intervention was deemed imperative. Non-operative management of displaced intertrochanteric fractures, especially in an active, independent patient, is associated with prolonged bed rest, increased complications (e.g., pneumonia, DVT, pressure ulcers, muscle atrophy), malunion, and persistent pain, making it an unacceptable option.
Classifications Guiding Treatment:
1.
AO/OTA Classification (31-A):
*
31-A1:
Simple two-part intertrochanteric (stable).
*
31-A2:
Multifragmentary (unstable, lateral wall intact, or greater trochanter involved). Our case was 31-A2.2 (multifragmentary with posteromedial comminution, but lateral wall theoretically sufficient if preserved and supported).
*
31-A3:
Reverse obliquity (highly unstable, requiring intramedullary nailing).
The unstable A2 patterns, particularly with significant posteromedial comminution, generally benefit from intramedullary nailing due to its biomechanical advantages in load sharing and resisting varus collapse.
2.
Evans-Jensen Classification (modified):
*
Type I (Stable):
Two-part fractures without comminution (e.g., A1).
*
Type II (Unstable):
Three- or four-part fractures with comminution of the posteromedial cortex (lesser trochanter), or extension into the greater trochanter, or reverse obliquity. This patient's fracture was an unstable Type II due to the posteromedial comminution and greater trochanter involvement.
Choice of Implant:
For unstable intertrochanteric fractures, particularly those with significant posteromedial comminution or reverse obliquity,
intramedullary nailing
(e.g., Proximal Femoral Nail (PFN), TFN, Gamma Nail) is generally the preferred implant over a Dynamic Hip Screw (DHS).
*
Biomechanical Advantages of IM Nailing:
* Load sharing through the central axis of the femur.
* Shorter lever arm, reducing bending stress at the fracture site.
* Greater rotational stability provided by the nail.
* Minimally invasive approach with smaller incision.
* Less risk of collapse into varus compared to DHS in unstable patterns.
* Specifically beneficial in fractures with extension into the subtrochanteric region or in reverse obliquity patterns where DHS is contraindicated.
-
Disadvantages of IM Nailing: Potential for greater trochanter pain, risk of iatrogenic femoral shaft fracture during nail insertion, difficulty with reduction in very complex cases.
-
DHS (Dynamic Hip Screw): While excellent for stable intertrochanteric fractures (AO/OTA 31-A1), it is associated with higher rates of cut-out and varus collapse in unstable patterns due to loss of the posteromedial buttress. The lever arm is longer, placing more bending stress on the implant.
Given the unstable 31-A2.2 pattern with significant posteromedial comminution, a cephalomedullary nail (e.g., a short TFN or PFN) was selected as the optimal implant to provide stable fixation, resist varus collapse, and facilitate early weight-bearing.
Pre-operative Optimization:
*
Anticoagulation Management:
Apixaban was held. INR was partially reversed with Prothrombin Complex Concentrate (PCC) to achieve an INR < 1.5. A bridging strategy with unfractionated heparin was considered but deferred given the urgency of surgery and the patient's low risk of thromboembolism over a very short pre-operative period.
*
Medical Clearance:
Cardiology and Internal Medicine consultations confirmed fitness for surgery with close monitoring of blood glucose and renal function.
*
Timing of Surgery:
The patient was taken to the operating room within 24 hours of presentation, adhering to guidelines for early surgical fixation to reduce morbidity and mortality in hip fractures.
Surgical Technique / Intervention
1. Patient Positioning:
The patient was positioned supine on a fracture table. The contralateral limb was abducted and flexed to allow sufficient space for C-arm imaging. The affected left limb was placed in a boot and secured to the traction apparatus. Gentle traction was applied to achieve initial reduction, aiming for appropriate length, rotation, and alignment. The amount of traction and limb position were guided by fluoroscopy. Slight internal rotation helps to correct the typical external rotation deformity.
2. Surgical Approach:
A small, approximately 4-6 cm longitudinal incision was made over the tip of the greater trochanter, centered to allow reaming and nail insertion. The skin, subcutaneous tissue, and fascia lata were incised. The gluteus medius was split bluntly or incised in line with its fibers, exposing the piriformis fossa and the tip of the greater trochanter.
3. Reduction Techniques:
This is the most critical step for success.
*
Longitudinal Traction:
Applied via the fracture table to restore length.
*
Internal Rotation:
Applied via the fracture table to correct the external rotation deformity.
*
Abduction/Adduction:
Adjusted as needed to align the femoral shaft with the femoral head-neck fragment.
*
Manual Reduction:
Often required additional manual manipulation of the thigh and hip by the surgeon to achieve acceptable alignment. This might involve pushing the shaft anteriorly or medially.
*
Closed Reduction:
Attempted primarily under fluoroscopic guidance. If closed reduction was inadequate, a limited open reduction via a separate small incision (e.g., percutaneous clamp application, reduction spoon, or K-wire joy-sticking) was prepared for. In this case, acceptable reduction was achieved with traction and manual manipulation. The goal was to restore anatomical alignment with minimal varus or valgus malalignment and to achieve contact between the main fragments, especially at the lateral wall, if possible.
4. Entry Point & Reaming:
* A guide wire (often a large-diameter K-wire) was inserted under fluoroscopic guidance at the piriformis fossa or slightly medial to the tip of the greater trochanter, aiming down the central axis of the femoral shaft. Correct entry point is crucial to avoid iatrogenic malalignment (e.g., varus or valgus) or fracture.
* A cannulated reamer was then used over the guide wire to create an entry portal and ream the proximal femoral canal to the appropriate diameter for the chosen intramedullary nail. Reaming was performed incrementally.
5. Nail Insertion:
* The selected cephalomedullary nail (short PFN, 10mm diameter, 200mm length) was loaded onto the insertion handle.
* The nail was gently inserted into the reamed canal, guided by the guide wire. Fluoroscopy was used to monitor nail progression and ensure it did not propagate a fracture. The nail was advanced until its distal tip reached the desired level, typically 1-2 cm proximal to the vastus lateralis ridge, ensuring it did not protrude past the greater trochanter proximally.
6. Lag Screw/Blade Insertion:
* With the nail in place, the targeting device was attached.
* A guide wire for the femoral neck lag screw (or blade) was inserted under dual-plane fluoroscopy (AP and lateral views). The optimal position for the lag screw/blade is central in the lateral view and central-inferior in the AP view (often referred to as tip-apex distance (TAD) principle, aiming for a TAD < 25mm to reduce cut-out risk).
* The femoral head was then reamed, and the lag screw (10.5mm diameter, 85mm length) was inserted and fully seated into the femoral head, providing dynamic compression at the fracture site.
* The anti-rotation screw/distal locking screw for the neck was then inserted through the targeting guide.
7. Distal Locking:
* A distal locking guide or freehand technique was used to insert distal locking screws (typically two, depending on nail design) into the femoral shaft, providing rotational and axial stability. This was performed under careful fluoroscopic guidance to ensure correct screw placement and to avoid neurovascular injury.
8. Final Assessment:
* Final fluoroscopic images (AP and lateral views) were obtained to confirm:
* Anatomical or near-anatomical reduction of the fracture.
* Correct placement of the intramedullary nail.
* Optimal position of the lag screw/blade within the femoral head (TAD < 25mm).
* Secure distal locking.
* The fracture table was disengaged, and a stability assessment was performed by gently rotating the hip.
9. Wound Closure:
The surgical site was copiously irrigated. The gluteus medius was repaired, fascia lata closed, and skin closed in layers. A sterile dressing was applied.
Post-Operative Protocol & Rehabilitation
1. Immediate Post-Operative Period (Day 0-3):
*
Pain Management:
Multimodal analgesia including IV acetaminophen, NSAIDs (if not contraindicated by renal function), and opioid analgesics as needed. Regional nerve blocks (e.g., Fascia Iliaca Block) were administered pre-operatively to aid in immediate pain control and reduce opioid requirements.
*
DVT Prophylaxis:
Subcutaneous enoxaparin 40mg daily was initiated 12 hours post-surgery, continued for 4-6 weeks, alongside mechanical prophylaxis (sequential compression devices).
*
Antibiotics:
Prophylactic IV antibiotics (e.g., Cefazolin) continued for 24 hours post-operatively.
*
Weight Bearing:
Given the stable fixation with the cephalomedullary nail, the patient was allowed
weight-bearing as tolerated (WBAT)
on the operative limb. This is crucial for early mobilization and bone healing.
*
Mobilization:
Physical therapy began on post-operative day 1. Patient encouraged to sit out of bed, perform ankle pumps, and begin transfers with assistance.
*
Labs:
Daily CBC and electrolytes monitored. Transfusion triggered if Hb < 7-8 g/dL or symptomatic.
2. In-Hospital Rehabilitation (Day 3-7):
*
Physical Therapy (PT):
Intensified. Focus on:
* Initiating standing and ambulation with a walking frame or crutches, progressing to a cane as tolerated.
* Gait training with WBAT.
* Therapeutic exercises: quadriceps sets, gluteal sets, heel slides, hip abduction/adduction in supine.
* Transfer training (bed to chair, toileting).
*
Occupational Therapy (OT):
Assessment of activities of daily living (ADLs), home safety, and provision of adaptive equipment if needed.
*
Discharge Planning:
Aim for discharge to home with outpatient PT or to a skilled nursing facility/rehabilitation center, depending on functional status and home support.
3. Outpatient Rehabilitation (Weeks 2-12):
*
Physical Therapy:
Continued 2-3 times per week.
* Progressive strengthening exercises for hip abductors, extensors, and quadriceps.
* Balance and proprioception training.
* Endurance training.
* Gait training to improve walking symmetry and reduce assistive device dependence.
*
Radiographic Follow-up:
* Initial X-rays at 2 weeks post-op to assess reduction maintenance and early signs of healing.
* Subsequent X-rays at 6 weeks, 3 months, 6 months, and 1 year to monitor union and implant integrity.
*
Return to Activities:
Gradual return to light activities as pain subsides and strength improves. Avoid high-impact activities for at least 6 months.
4. Long-Term (Beyond 3 Months):
* Discontinue assistive devices when strength and balance are adequate.
* Continue home exercise program.
* Address osteoporosis with appropriate pharmacotherapy (e.g., bisphosphonates, denosumab) and vitamin D/calcium supplementation.
* Focus on fall prevention strategies: home safety assessment, medication review, vision checks.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls for Success:
- Pre-operative Optimization: Crucial for elderly, comorbid patients. Timely medical clearance, anticoagulation management, and hydration. Surgery within 24-48 hours significantly reduces morbidity and mortality.
- Anatomical Reduction is Key: Although intertrochanteric fractures often heal in suboptimal alignment, the goal should always be to achieve anatomical or near-anatomical reduction, especially of the medial and lateral cortices. This dictates load sharing and prevents mechanical failure. Varus malreduction is the enemy.
- Proper Entry Point for IM Nailing: The entry point should be at or just medial to the tip of the greater trochanter, in line with the femoral canal, to avoid varus malalignment, iatrogenic greater trochanter fracture, or reaming through the lateral cortex. Fluoroscopic guidance in two planes is essential.
- Optimal Lag Screw/Blade Placement (TAD): The Tip-Apex Distance (TAD) is paramount. Aim for a central-inferior position in the AP view and a central position in the lateral view. A TAD < 25mm is strongly correlated with a reduced risk of cut-out. Avoid superior and anterior placement. The screw/blade should be as long as possible without violating the subchondral bone.
- Stable Lateral Wall: For unstable fractures, preserving or reconstructing the lateral wall (if comminuted) is critical. While IM nails are good for lateral wall fractures, loss of the lateral wall after DHS insertion leads to high failure rates. IM nailing supports the lateral wall indirectly.
- Dynamic Compression: Ensure the lag screw/blade allows for dynamic collapse at the fracture site to promote impaction and secondary bone healing.
- Early Mobilization and WBAT: Crucial for elderly patients. WBAT should be encouraged with stable fixation to prevent complications of immobility and promote bone healing.
- Osteoporosis Management: Address the underlying osteoporosis post-operatively to prevent future fragility fractures.
Pitfalls to Avoid (Causes of Failure):
- Inadequate Reduction: Failure to restore acceptable length, rotation, and especially alignment (varus malreduction). This leads to increased stress on the implant and higher risk of mechanical failure or non-union.
- Poor Entry Point: An entry point too lateral can lead to varus malalignment. An entry point too medial can lead to iatrogenic fracture of the greater trochanter or proximal femoral shaft.
-
Suboptimal Lag Screw/Blade Placement:
- High TAD (>25mm): The most common cause of fixation failure, leading to lag screw cut-out from the femoral head due to poor purchase.
- Placement too superior or anterior: Increases risk of cut-out.
- Screw too short: Insufficient purchase in the femoral head.
- Screw too long: Penetration into the joint, causing chondral damage.
- Failure to Recognize Unstable Fracture Patterns: Treating an unstable fracture (e.g., A2 or A3 reverse obliquity) with a DHS is a common pitfall leading to varus collapse and implant failure. IM nailing is the implant of choice for unstable patterns.
- Iatrogenic Fracture: During reaming or nail insertion, especially in osteoporotic bone or with incorrect entry point/reaming trajectory. Use gentle technique and monitor with fluoroscopy.
- Non-Union/Delayed Union: Can occur due to poor reduction, inadequate fixation, biological factors (e.g., severe osteoporosis, comorbidities), or infection.
- Malunion: Persistent varus, valgus, or rotational deformity, leading to gait disturbance, limb length discrepancy, and pain.
- Cut-out: The lag screw/blade migrates superiorly or anteriorly through the femoral head into the joint. Directly related to high TAD.
- Z-effect / Reverse Z-effect: Complications specific to dual-screw cephalomedullary nails where one screw migrates into the joint while the other backs out, or vice-versa. Often due to inadequate purchase of one screw.
- Infection: Standard surgical site infection prophylaxis and sterile technique are paramount.
- Greater Trochanteric Pain: Can occur due to prominent hardware (proximal nail tip) or irritation of soft tissues.
- Hardware Breakage: Rare, but can occur with delayed union, non-union, or excessive stress on the implant due to poor reduction.
