Introduction & Epidemiology
Stenosing tenosynovitis of the flexor pollicis longus (FPL), colloquially known as pediatric trigger thumb, is a common acquired condition presenting in early childhood. While often referred to as "congenital trigger thumb," its typical presentation months or years after birth suggests a developmental rather than truly congenital etiology. The condition is characterized by a mechanical obstruction to the smooth gliding of the FPL tendon within its fibro-osseous sheath at the level of the A1 pulley, leading to triggering, locking, or a fixed flexion deformity of the interphalangeal (IP) joint of the thumb.
Epidemiologically, pediatric trigger thumb has an estimated incidence ranging from 0.03% to 3.3% in children. There is no clear gender predilection, and bilateral involvement is reported in 20-30% of cases. The most common age of presentation is between six months and three years, with symptoms rarely noted at birth. While the exact etiology remains debated, leading theories propose a disproportionate growth rate between the FPL tendon and its sheath, or a localized thickening of the A1 pulley and/or the tendon itself, forming a nodule (Notta's nodule) at the level of the metacarpophalangeal (MCP) joint. Histological studies of Notta's nodule reveal fibrocartilaginous metaplasia and myxoid degeneration within the tendon substance, suggesting a localized inflammatory or degenerative process rather than a purely congenital malformation. Familial cases are rare, further supporting an acquired or developmental basis.
Surgical Anatomy & Biomechanics
A thorough understanding of the surgical anatomy of the thumb's flexor mechanism is paramount to safe and effective intervention for pediatric trigger thumb. The FPL tendon originates from the anterior surface of the radius and interosseous membrane, traversing distally through the carpal tunnel and then into the thumb. Its course is maintained by a series of annular and cruciform pulleys, which act as retinacular restraints, preventing bowstringing and optimizing mechanical advantage.
The critical structure implicated in pediatric trigger thumb is the A1 pulley . This first annular pulley originates from the volar plate and neck of the proximal phalanx, bridging the FPL tendon at the level of the MCP joint. In trigger thumb, the A1 pulley becomes thickened and constricted, impeding the smooth passage of the FPL tendon. A palpable nodule, termed Notta's nodule, typically forms on the FPL tendon just proximal to the A1 pulley. This nodule is essentially an eccentric thickening of the tendon, which then becomes ensnared within the narrowed A1 pulley as the child attempts to extend the thumb, causing the characteristic "triggering" or "locking" phenomenon. In severe cases, particularly with chronic locking, a fixed flexion contracture of the IP joint can develop due to adaptive shortening of the volar plate and collateral ligaments.
Neurovascular Structures of Concern
The median nerve innervates the FPL muscle in the forearm. Distally, the primary neurovascular structures at risk during A1 pulley release are the
digital nerves and vessels
of the thumb. The radial digital nerve of the thumb and the ulnar digital nerve of the thumb (branching from the median nerve) lie in close proximity to the A1 pulley incision site.
The
radial digital nerve of the thumb
typically courses along the radial side of the FPL sheath, superficial to the A1 pulley.
The
ulnar digital nerve of the thumb
(often splitting from the common digital nerve to the index finger) generally lies on the ulnar side of the FPL sheath. The precise anatomical variability of these nerves, particularly their superficial course within the subcutaneous tissue of the thenar crease, mandates careful dissection. The vascular supply to the thumb, primarily from the princeps pollicis artery, is also superficial in the area and must be protected.
The biomechanical consequence of a stenotic A1 pulley is an increase in friction and a mechanical block to FPL tendon excursion. During flexion, the nodule passes easily into the wider proximal sheath. However, during active or passive extension, the nodule catches at the distal edge of the constricted A1 pulley. With sufficient force, it may snap through, producing the "triggering" sensation. Persistent obstruction leads to locking, and chronic locking can result in secondary contractures of the IP joint and potentially the MCP joint.
Indications & Contraindications
The management approach for pediatric trigger thumb depends on the child's age, the severity of the condition, and the presence of a fixed deformity.
Non-Operative Indications
- Younger children (<1 year of age) : Many clinicians advocate for an initial period of observation due to reports of spontaneous resolution rates ranging from 11% to 60%, particularly in infants. The rationale is that disproportionate growth may resolve over time.
- Mild or intermittent triggering : Without a fixed flexion deformity.
- Patient or parental preference : If surgery is not desired initially and the condition is not causing significant functional impairment or fixed deformity.
- Splinting : While less commonly effective than in adults for true stenosing tenosynovitis, dynamic splinting or static splinting of the IP joint in extension may be attempted in some centers, though strong evidence for its efficacy in children is limited.
Operative Indications
- Persistent locking or triggering : Despite a period of observation, especially in children over one year of age.
- Fixed flexion deformity : Any degree of fixed flexion contracture of the IP joint is a strong indication for surgical release, as spontaneous resolution is unlikely once a fixed deformity is established, and prolonged deformity can lead to secondary joint changes.
- Functional impairment : If the condition significantly impacts fine motor skills or grasp.
- Recurrence after a period of spontaneous resolution.
Contraindications
- Active local infection : Cellulitis or abscess in the region of the proposed incision.
- Coagulopathy or other significant medical comorbidities : Relative contraindications that require careful preoperative assessment and optimization.
- Unrealistic parental expectations : Requires thorough pre-operative counseling regarding potential complications and expected outcomes.
- Misdiagnosis : Ensuring that the thumb pathology is indeed stenosing tenosynovitis and not other conditions like congenital clasped thumb (arthrogryposis, etc.) or post-traumatic contracture.
Summary Table: Operative vs. Non-Operative Indications
| Feature | Non-Operative Management | Operative Management |
|---|---|---|
| Age | Typically children < 1 year of age | Typically children > 1 year of age, or any age with specific criteria |
| Severity of Symptoms | Mild, intermittent triggering; no fixed deformity | Persistent, bothersome triggering/locking; fixed flexion deformity of IP joint |
| Response to Observation | Spontaneous resolution noted or expected | Failure of observation period (e.g., 6-12 months) |
| Functional Impairment | Minimal or absent | Significant impact on daily activities or grasp |
| Fixed Deformity | Absent | Present |
| Primary Approach | Observation, potentially gentle stretching exercises (parental instruction) | Surgical release of A1 pulley |
| Prognosis for Resolution | Variable (11-60% spontaneous resolution reported) | High success rates (>90-95%) |
Pre-Operative Planning & Patient Positioning
Pre-operative Planning:
1.
Clinical Assessment
: A thorough history and physical examination are essential. Document the presence and severity of triggering, locking, and any fixed flexion deformity. Palpate for Notta's nodule over the FPL tendon at the MCP joint level. Assess passive range of motion to determine if a fixed contracture is present and its reducibility.
2.
Parental Counseling
: Discuss the nature of the condition, the surgical procedure, potential risks (digital nerve injury, recurrence, infection, scar formation), expected recovery, and high success rates. Ensure understanding and obtain informed consent. For the child, the conversation would be age-appropriate reassurance, but for this academic document, the focus is on parental education for consent.
3.
Anesthesia Consultation
: Pediatric cases invariably require general anesthesia. A pre-operative anesthetic assessment is critical, particularly for infants and young children.
4.
Surgical Site Marking
: The affected thumb should be clearly marked, typically the day of surgery, and confirmed with the parents.
5.
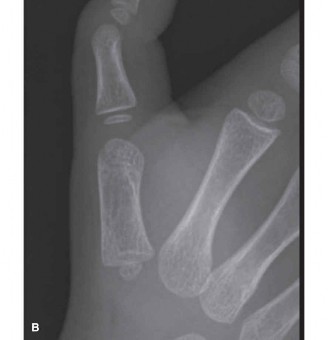
Imaging
: Radiographs are generally not required for typical pediatric trigger thumb but may be considered if there is suspicion of other pathologies (e.g., bony abnormality, tumor) or if the diagnosis is unclear.
Patient Positioning:
1.
Supine Position
: The child is placed supine on the operating table.
2.
Arm Board
: The affected upper extremity is positioned on a hand table or an arm board, abducted and externally rotated for optimal exposure of the volar aspect of the thumb.
3.
Tourniquet
: A pneumatic tourniquet is applied to the upper arm. The limb is exsanguinated prior to inflation, typically to 200-250 mmHg, or 100 mmHg above systolic pressure for the duration of the procedure. This provides a bloodless field, which is crucial for identifying and protecting delicate neurovascular structures in the small anatomy of a child's hand.
4.
Sterile Preparation and Drape
: The entire hand and forearm are prepped with an antiseptic solution and draped in a sterile fashion, ensuring adequate exposure of the thumb and the ability to manipulate it during the procedure.
Detailed Surgical Approach / Technique
The surgical objective is to release the constricted A1 pulley to allow unrestricted gliding of the FPL tendon, while meticulously protecting the adjacent neurovascular structures. The procedure is typically performed under general anesthesia.
-
Incision Planning :
- A small transverse incision within a natural skin crease of the thumb's volar surface is often preferred, typically just distal to the distal palmar crease, overlying the MCP joint. This allows for excellent cosmetic outcomes. The incision should be approximately 8-10 mm in length.
- Alternatively, a longitudinal incision (e.g., 10-15 mm) centered over the A1 pulley may be used, particularly in cases of severe fixed deformity or in revisions, offering potentially wider exposure but with a less aesthetic scar. For primary cases in children, the transverse incision is generally favored.
-
Careful marking is done pre-tourniquet to ensure accurate placement.
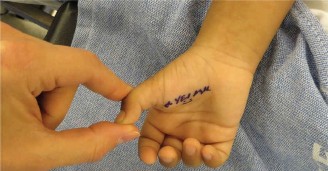
-
Skin Incision and Subcutaneous Dissection :
- Infiltrate local anesthetic (e.g., 0.5% bupivacaine with epinephrine) into the incision site for post-operative analgesia and hemostasis (pre-tourniquet).
- Make the skin incision with a #15 blade. Deepen the incision cautiously through the subcutaneous fat.
- CRITICAL STEP : The digital nerves and vessels are extremely superficial in the pediatric thumb. Using fine dissecting scissors (e.g., iris scissors) or a fine blunt dissector (e.g., mosquito hemostat), gently spread the subcutaneous tissues in line with the expected course of the digital nerves. This allows identification and protection of the radial and ulnar digital neurovascular bundles. The radial digital nerve of the thumb is particularly vulnerable on the radial aspect of the FPL sheath. The ulnar digital nerve of the thumb is typically on the ulnar aspect.
-
Exposure of the Flexor Tendon Sheath :
- Once the neurovascular bundles are identified and retracted, the underlying FPL tendon sheath, appearing as a whitish, fibrous structure, becomes visible.
- The A1 pulley is located directly proximal to the MCP joint's volar plate, overlying the FPL tendon. A thickened, glistening appearance of the pulley is often evident. Notta's nodule may also be seen proximal to the pulley.
-
A1 Pulley Release :
-
Method 1 (Transverse Incision Approach)
:
- Gently elevate the A1 pulley with a small hook or forceps.
- Using a #11 blade or a fine scalpel, make a precise longitudinal incision along the ulnar side of the A1 pulley. This ulnar approach is often preferred as the radial digital nerve of the thumb is generally considered more superficial and closer to the midline incision site. Alternatively, a central incision may be performed. The key is to avoid incising the entire width of the pulley at once.
- Extend the incision proximally and distally for the full length of the A1 pulley.
- CRITICAL STEP : Ensure the release is complete by probing the incision with a blunt instrument (e.g., curved mosquito hemostat or nerve hook) to confirm that no remaining fibers of the A1 pulley are constricting the FPL tendon.
-
Method 2 (Blind Percutaneous Release -
Not recommended for pediatric cases in general training due to higher risk of nerve injury
)
: This technique is described in literature but carries a higher risk of neurovascular injury in the pediatric population due to smaller structures and variable anatomy, and therefore is generally not advocated for resident training or routine use.
-
Method 1 (Transverse Incision Approach)
:
-
Confirm Tendon Gliding :
- Once the A1 pulley is completely released, flex and extend the thumb's IP joint and MCP joint repeatedly. The FPL tendon and Notta's nodule (if present) should glide freely without any catching, triggering, or mechanical impedance. The fixed flexion deformity, if present, should resolve, allowing full passive extension of the IP joint.
- Notta's nodule typically does not need to be excised. Its presence resolves spontaneously once the mechanical obstruction is removed.
-
Hemostasis and Closure :
- Deflate the tourniquet and achieve meticulous hemostasis using bipolar cautery.
- Irrigate the wound with sterile saline.
- Close the skin with fine absorbable sutures (e.g., 6-0 or 7-0 plain gut or chromic gut) in a subcuticular fashion, or with fine non-absorbable sutures that will be removed post-operatively. For children, absorbable sutures are often preferred to avoid the need for suture removal, which can be distressing.
-
Apply a sterile dressing, typically a non-adherent dressing directly over the wound, followed by gauze and a soft cohesive bandage that allows for thumb mobility but protects the wound.

Complications & Management
While surgical release of pediatric trigger thumb is generally safe and highly effective, potential complications exist, requiring careful attention to surgical technique and post-operative monitoring.
| Complication | Incidence | Etiology | Management Strategy |
|---|---|---|---|
| Digital Nerve Injury | <1% (rare) | Laceration or contusion during dissection or pulley release due to superficial course and anatomical variation of radial/ulnar digital nerves. |
Prevention is key
: Meticulous, cautious dissection, especially in subcutaneous plane. Use blunt dissection. Identify nerves before incising pulley.
Intraoperative : If nerve laceration is recognized, primary repair with microsurgical technique. Postoperative : If neuropraxia (temporary dysfunction), observation and possibly hand therapy. If persistent deficit, nerve exploration and repair. |
| Incomplete Pulley Release | <5% | Insufficient incision of the A1 pulley, leading to persistent triggering or locking. |
Prevention
: Intraoperative confirmation of full tendon gliding.
Management : Revision surgery to completely release the remaining constricting fibers. |
| Recurrence | <2% (very rare) | Usually due to incomplete primary release or rarely, re-scarring. | Often requires revision surgery with careful identification and release of the remaining pulley. |
| Infection | <1% | Contamination of the surgical site. |
Prevention
: Strict aseptic technique, appropriate skin prep.
Management : Oral or IV antibiotics for superficial cellulitis. Incision and drainage for abscess, with wound cultures and directed antibiotic therapy. |
| Scarring | Variable | Hypertrophic or keloid scarring, particularly in individuals with predisposition. |
Prevention
: Transverse incision along a skin crease, meticulous skin closure, gentle tissue handling.
Management : Scar massage, silicone sheeting/gel, steroid injections for hypertrophic scars. Rarely, scar revision. |
| Flexion Contracture Persistence/Recurrence | <1% | Prolonged fixed deformity leading to adaptive shortening of volar plate/collaterals; rarely, insufficient A1 release. |
Prevention
: Adequate A1 pulley release.
Management : Hand therapy with passive stretching. In rare, recalcitrant cases, consideration of surgical release of secondary contractures (e.g., volar plate release), although very uncommon after adequate A1 pulley release. |
| Tendon Bowstringing | Extremely rare | Over-release of essential pulleys (e.g., A2 or A3), or excessive release of the A1 pulley leading to FPL instability. |
Prevention
: Confine release strictly to the A1 pulley.
Management : Surgical reconstruction of the pulley, if functionally significant. |
| Stiffness/Decreased ROM | Rare | Post-operative pain, edema, or fear of movement. |
Prevention
: Early mobilization protocols.
Management : Hand therapy, encouragement of active range of motion. |
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation for pediatric trigger thumb release is typically straightforward, emphasizing early mobilization and scar care. The primary goal is to restore full, pain-free range of motion rapidly while ensuring proper wound healing.
Immediate Post-Operative Period (Day 0-7)
- Dressing : A soft, bulky dressing is applied in the operating room. This usually includes a non-adherent contact layer, gauze, and a soft cohesive bandage. It is typically kept on for 2-5 days. The dressing should allow for active and passive range of motion of the thumb.
- Pain Management : Age-appropriate analgesia (e.g., acetaminophen, ibuprofen) is prescribed. A local anesthetic block placed during surgery (e.g., bupivacaine) provides excellent initial post-operative pain relief.
- Elevation : Keep the hand elevated (e.g., on pillows) for the first 24-48 hours to minimize swelling.
- Activity : Encourage gentle, active range of motion of the thumb and fingers as tolerated within the dressing. Avoid heavy lifting, pushing, or grasping.
- Wound Care : Keep the dressing clean and dry. Parents are instructed to observe for signs of infection (redness, swelling, purulent discharge).
Early Rehabilitation Phase (Week 1-4)
- Dressing Removal / Wound Check : Typically performed around 5-7 days post-surgery. If absorbable sutures were used, no removal is necessary. Non-absorbable sutures are removed at this visit.
- Scar Management : Once the wound is completely closed, initiation of scar massage is recommended. This involves gentle circular massage over the incision site multiple times a day to prevent adhesion and soften scar tissue. Silicone sheeting or gel can be applied to aid in scar maturation and reduce hypertrophy.
- Range of Motion : Active and passive range of motion exercises for the thumb (IP and MCP joints) are encouraged throughout the day. Emphasis is placed on full extension and flexion to prevent stiffness.
- Functional Activities : Gradual return to light, age-appropriate activities. Avoidance of activities that put direct pressure or shear forces on the incision site.
Late Rehabilitation Phase (Week 4 onwards)
- Full Activity : By 4-6 weeks post-surgery, most children can resume all normal activities, including sports, provided the wound is fully healed and pain-free range of motion is achieved.
- Continued Scar Management : Continue scar massage and silicone products for several months as needed until the scar matures.
- Monitoring : Follow-up appointments are scheduled as needed to monitor scar appearance, range of motion, and confirm complete resolution of symptoms. Recurrence is rare but should be assessed.
Formal hand therapy is generally not required for pediatric trigger thumb release unless there are specific complicating factors such as a persistent fixed contracture, significant pain, or a digital nerve injury requiring more intensive rehabilitation. The natural tendency of children to use their hands actively usually suffices for successful recovery.
Summary of Key Literature / Guidelines
Pediatric trigger thumb is a well-described condition with a strong consensus regarding its diagnosis and management, predominantly guided by clinical presentation and age.
Etiology and Natural History:
*
Developmental vs. Congenital
: The literature largely supports a developmental etiology rather than a true congenital malformation. Studies by Dinham and Meggitt (1974) and Kikuchi and Ogino (2002) highlighted the typical late presentation, often between 6 months and 3 years, as evidence against a purely congenital origin.
*
Spontaneous Resolution
: There is evidence for spontaneous resolution, particularly in younger infants. Studies by Baek et al. (2008) and Lee et al. (2014) reported spontaneous resolution rates ranging from 11% to 60%, with higher rates observed in infants less than one year of age and those without a fixed flexion deformity. This supports an initial period of observation for younger, less symptomatic patients.
Surgical Indications and Outcomes:
*
Consensus for Surgery
: Surgical release is generally indicated for children with persistent triggering, locking, or a fixed flexion deformity that has failed to resolve after a period of observation (typically 6-12 months, or immediately if a severe fixed deformity exists).
*
High Success Rates
: Numerous studies confirm high success rates for surgical A1 pulley release, often exceeding 95%. Results are excellent, with resolution of triggering and correction of fixed flexion deformities. A meta-analysis by Patel et al. (2009) underscored the efficacy of surgical intervention.
*
Timing of Surgery
: While observation is initially favored for very young children, persistent symptoms, especially with a fixed deformity, prompt earlier surgical intervention. Prolonged fixed flexion can theoretically lead to adaptive changes that are harder to reverse, though this is rare with prompt surgery.
*
Complications
: As discussed, complications are rare. Digital nerve injury, while a concern, has a very low reported incidence when meticulous surgical technique is employed (Ogino and Kikuchi, 2005). Recurrence is similarly rare.
Surgical Technique:
*
Open Release
: The open surgical release via a transverse or longitudinal incision remains the gold standard. The critical steps are accurate identification and complete release of the A1 pulley while protecting the digital neurovascular bundles.
*
Percutaneous Release
: While widely used in adults, percutaneous release in children is controversial and generally not recommended due to the small size of structures and increased risk of neurovascular injury (Moon et al., 2009; Kim and Kim, 2011). The consensus is that the increased safety margin of an open technique in pediatric hands outweighs any theoretical benefits of a percutaneous approach.
Post-operative Care:
*
Early Mobilization
: Protocols advocating early active range of motion without rigid immobilization are widely accepted and contribute to excellent functional outcomes.
*
Scar Management
: Attention to scar cosmesis, especially in pediatric patients, is important, favoring transverse incisions and early scar massage.
In summary, the current literature supports a judicious approach to pediatric trigger thumb, beginning with observation in younger children, but moving to surgical release for persistent or severe cases. The open surgical release of the A1 pulley is a highly effective procedure with predictable outcomes and a low complication rate when performed with careful attention to surgical anatomy.
Clinical & Radiographic Imaging

