Patient Presentation & History
A 32-year-old right-hand dominant male presented to the emergency department approximately 2 hours after sustaining a deep laceration to the volar aspect of his left middle finger. The mechanism of injury involved a kitchen knife accident while preparing food. He reported immediate severe pain, profuse bleeding, and an inability to bend the affected finger, specifically noting a lack of motion at the middle and distal interphalangeal joints. He applied direct pressure to the wound at home prior to arrival.
His past medical history was unremarkable, with no known chronic illnesses, allergies, or previous surgeries. He denied smoking, illicit drug use, and consumed alcohol socially. He was not on any regular medications. His tetanus immunization status was up to date. He works as an office administrator, making fine motor control and dexterity of his dominant hand crucial for his occupation. The prompt presentation and clear mechanism suggested a high likelihood of significant soft tissue injury requiring urgent assessment.
Clinical Examination
Upon initial inspection, a clean, transverse laceration measuring approximately 2.5 cm was noted on the volar aspect of the left middle finger, overlying the middle phalanx, consistent with Flexor Tendon Zone II. The wound edges were sharp, and there was minimal active bleeding at the time of examination, suggesting the primary injury was a direct cut rather than a crush or avulsion. There was moderate swelling around the wound, but no obvious hematoma or signs of active infection. The finger presented in a relatively extended posture compared to adjacent digits, losing the natural "cascade" of the hand.
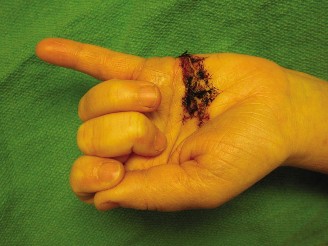
Palpation: Tenderness was localized to the laceration site. No crepitus was elicited, and no bony abnormalities were palpable. Distal warmth and capillary refill were brisk (<2 seconds), suggesting adequate macrovascular perfusion.
Range of Motion (ROM):
*
Active ROM:
* The patient was unable to actively flex the left middle finger at the proximal interphalangeal (PIP) joint against resistance, despite attempting to isolate the flexor digitorum superficialis (FDS) by holding the other fingers in full extension. There was a subtle attempt at PIP flexion, but no active motion against gravity or resistance, indicative of FDS disruption.
* When attempting to isolate the flexor digitorum profundus (FDP) by holding the PIP joint in full extension, the patient was unable to actively flex the distal interphalangeal (DIP) joint. This confirmed FDP involvement.
* Active flexion and extension were preserved at the metacarpophalangeal (MCP) joint, suggesting intact extrinsic flexors proximal to the injury site and intrinsic muscle function.
* Full passive ROM was achievable at both the PIP and DIP joints, confirming that joint integrity was preserved and there was no mechanical block.
*
Neurological Assessment:
* Light touch and two-point discrimination were assessed on both the radial and ulnar aspects of the middle finger distal to the laceration. Sensation was diminished but not entirely absent along the radial digital nerve distribution, indicating a partial or neuropraxia-level injury, while the ulnar digital nerve sensation appeared intact. This suggested a possible associated radial digital nerve injury.
* Motor function of the ulnar, median, and radial nerves proximal to the hand was assessed and found to be intact.
*
Vascular Assessment:
Digital pulses were palpable, and capillary refill was brisk in all digits including the injured middle finger, confirming no significant digital artery transection. An Allen's test was not performed as the primary concern was not main arterial supply compromise to the entire hand, but focused on the affected digit's perfusion.
Based on the clinical findings, the complete inability to actively flex the PIP and DIP joints of the middle finger in the presence of a deep volar laceration, a diagnosis of complete flexor digitorum superficialis and flexor digitorum profundus lacerations in Zone II was made. The diminished sensation on the radial side of the digit raised suspicion for an associated partial radial digital nerve injury.
Imaging & Diagnostics
Plain Radiographs:
Standard anteroposterior (AP), lateral, and oblique views of the left hand and middle finger were obtained.
*
Findings:
The radiographs demonstrated no evidence of acute fracture, dislocation, or subluxation involving the phalanges or interphalangeal joints. There was no visible radiopaque foreign body embedded within the soft tissues. While radiographs are not diagnostic for tendon or nerve injuries, they are essential to rule out associated bony injuries and radiopaque foreign bodies that might complicate management or alter the surgical approach. The absence of bony pathology allowed us to focus solely on soft tissue reconstruction.
Further Diagnostic Considerations:
*
Ultrasound:
In ambiguous cases of partial tendon lacerations or where tendon retraction is uncertain, high-resolution ultrasound can sometimes provide valuable information regarding tendon continuity, the extent of laceration, and the location of retracted ends. However, for complete flexor tendon lacerations with clear clinical signs, as in this case, ultrasound is generally not required and would only delay definitive surgical management.
*
MRI:
Magnetic Resonance Imaging (MRI) offers excellent soft tissue resolution and can clearly visualize tendons, nerves, and vessels. However, its use is typically reserved for subacute or chronic flexor tendon injuries, or complex cases involving large hematomas, suspected occult fractures, or when there is uncertainty regarding the extent of injury to multiple structures. In the acute setting of a clean laceration with unequivocal clinical findings, MRI provides no additional information that would alter immediate surgical planning and is not cost-effective or time-efficient.
*
Laboratory Tests:
Standard pre-operative blood work, including a complete blood count (CBC), basic metabolic panel (BMP), and coagulation studies (PT/INR, PTT), were obtained. All results were within normal limits, confirming the patient's suitability for surgery. A Group & Save was performed in line with our institutional protocol for hand surgery cases, although significant blood loss was not anticipated.
The comprehensive clinical examination, supported by negative plain radiographs, was sufficient to confirm the diagnosis and proceed with urgent surgical intervention.
Differential Diagnosis
The presentation of a sharp volar laceration with functional deficits in finger flexion necessitates a differential diagnosis that considers various causes of impaired digital motion and sensation. While the clinical picture for complete FDS and FDP lacerations in Zone II is often direct, distinguishing it from partial injuries, isolated nerve injuries, or other rare causes of pseudo-paralysis is critical.
| Feature | FDS/FDP Laceration (Case 18) | Isolated FDS Laceration | Isolated FDP Laceration | Digital Nerve Laceration (Isolated) | Tendon Avulsion (Jersey Finger) | Joint Capsular Injury/Dislocation |
|---|---|---|---|---|---|---|
| Mechanism of Injury | Sharp volar trauma (e.g., knife, glass), direct cut. | Sharp volar trauma, direct cut. | Sharp volar trauma, direct cut. | Sharp trauma, direct cut (often concurrent with tendon injury). | Forceful hyperextension of DIP (Zone I), usually closed injury. | Direct impact, twisting injury, often closed. |
| Clinical Presentation | Open wound, inability to actively flex PIP and DIP joints against resistance. | Open wound, inability to actively flex PIP, preserved active DIP flexion. | Open wound, preserved active PIP flexion, inability to actively flex DIP. | Open wound, sensory deficit (numbness, paresthesia), normal motor function of tendons . | No open wound typically. Inability to actively flex DIP, pain over volar DIP. | Pain, swelling, deformity, restricted passive and active ROM. No specific tendon deficit. |
| Specific Functional Tests | FDS test: No PIP flexion. FDP test: No DIP flexion. | FDS test: No PIP flexion. FDP test: Intact DIP flexion. | FDS test: Intact PIP flexion. FDP test: No DIP flexion. | FDS/FDP tests: Intact active flexion. Sensory testing abnormal. | FDS test: Intact PIP flexion. FDP test: No DIP flexion. | May have pain with FDS/FDP tests but motor function present if not severely pain-limited. |
| Associated Neurovascular Injury | High incidence of associated digital nerve/artery injury. | Moderate incidence of associated digital nerve/artery injury. | Moderate incidence of associated digital nerve/artery injury. | Often isolated, but can occur with partial tendon injury. | Usually no nerve/vascular injury directly. | Possible neurovascular compromise if dislocation is severe. |
| Imaging (X-ray) | Rule out foreign bodies/fractures. Generally normal bony anatomy. | Rule out foreign bodies/fractures. Generally normal bony anatomy. | Rule out foreign bodies/fractures. Generally normal bony anatomy. | Normal bony anatomy, no foreign bodies. | May show avulsion fracture at FDP insertion (type I-III, Leddy & Packer). | May show fracture or joint incongruity. |
| Treatment | Urgent surgical repair. | Urgent surgical repair. | Urgent surgical repair. | Urgent surgical repair (micro-neurosurgery). | Surgical repair (reinsertion of FDP) or occasionally amputation for chronic. | Reduction (open or closed), immobilization, early ROM. |
| Prognosis (Untreated) | Permanent loss of function, stiffness, adhesion, contracture. | Permanent loss of PIP function, stiffness. | Permanent loss of DIP function, stiffness. | Permanent sensory loss, trophic changes, potential neuromas. | Permanent loss of DIP flexion, pain, chronic instability. | Chronic pain, stiffness, instability, degenerative changes. |
Our patient's clinical presentation, specifically the complete absence of both PIP and DIP active flexion in the presence of a deep volar laceration, strongly pointed towards a complete transection of both FDS and FDP tendons. The partial sensory deficit added to the complexity, indicating a probable associated digital nerve laceration. The inability to move the joints actively, despite full passive range, ruled out conditions like joint capsular injury or simple pain-induced pseudo-paralysis as the sole etiology. The sharp nature of the injury and the open wound ruled out typical closed avulsion injuries like a "jersey finger" as the primary mechanism, although an avulsion could theoretically occur with sharp trauma.
Surgical Decision Making & Classification
Operative vs. Non-operative Management:
Acute, complete flexor tendon lacerations are universally managed with urgent surgical repair. Non-operative management is typically reserved for very specific scenarios, such as very small partial lacerations (<50-60% of tendon cross-sectional area) where active motion is preserved without gapping, or in patients with prohibitive surgical risks. In our case, the complete loss of active PIP and DIP flexion, coupled with the open wound and high suspicion of full tendon transection, mandated immediate operative intervention. Delaying repair beyond 24-72 hours significantly increases the difficulty of tendon retrieval due to retraction and can lead to increased scarring and poorer functional outcomes.
Timing of Surgery:
The goal is to perform primary repair as soon as possible, ideally within 24 hours, to minimize tendon retraction and edema. Our patient presented within 2 hours, allowing for prompt surgical planning.
Relevant Classifications:
The most critical classification system for flexor tendon injuries is
Verdan's Zones of Flexor Tendon Injury
:
*
Zone I:
Distal to the FDS insertion (FDP only injury).
*
Zone II:
"No Man's Land" – extends from the FDS insertion to the distal palmar crease. This zone is characterized by both FDS and FDP tendons existing within the fibro-osseous sheath, making repair challenging due to tight confines, potential for adhesions, and proximity to the delicate vincula and pulleys. This was the zone of injury for our patient.
*
Zone III:
Extends from the distal palmar crease to the origin of the lumbricals. Tendons are within the palm, but outside the digital sheath.
*
Zone IV:
The carpal tunnel, involving all flexor tendons and the median nerve.
*
Zone V:
Proximal to the carpal tunnel, in the forearm.
Our patient sustained a laceration in Zone II of the left middle finger, involving both FDS and FDP tendons. This is considered one of the most challenging zones for flexor tendon repair due to the close proximity of the tendons, the digital sheath, and critical pulleys (A2 and A4), which if compromised, can lead to functional deficits like bowstringing. The presence of a concomitant digital nerve injury further complicated the management, requiring meticulous repair of two critical structures.
The decision was to proceed with urgent primary repair of both the FDS and FDP tendons, along with exploration and repair of the radial digital nerve, under regional anesthesia with tourniquet control.
Surgical Technique / Intervention
Anesthesia and Positioning:
The patient was brought to the operating theater. A regional anesthetic (axillary block) was administered to provide excellent pain control and sympathetic block for potential microvascular repair, supplemented with mild sedation. The patient was positioned supine on the operating table with the left arm abducted and pronated on a specialized hand table. A pneumatic tourniquet was applied to the upper arm, and the limb was prepped and draped in a sterile fashion.
Surgical Approach:
The existing transverse laceration was extended proximally and distally using a modified Bruner zig-zag incision. This approach provides excellent exposure to the flexor sheath and minimizes the risk of scar contracture over the repaired tendons. Care was taken to make the skin incisions precisely and avoid compromising the delicate underlying neurovascular structures. The skin flaps were elevated carefully.
Exploration and Identification of Structures:
Upon opening the subcutaneous tissue, the transected radial digital nerve of the middle finger was identified. Both ends were visible, suggesting a clean transection.
The digital fibro-osseous sheath was then carefully opened, initially revealing a gaping defect where the flexor tendons should have been. The proximal ends of the FDS and FDP tendons were found to be retracted significantly, typical for Zone II injuries. The FDP tendon, being deeper, typically retracts further proximally into the palm or even forearm due to its long excursion. The FDS tendon retracts less, but still out of the immediate field.
*
Tendon Retrieval:
To retrieve the retracted proximal tendon ends, the palmar wound was gently palpated while applying pressure proximally in the forearm ("milking" maneuver) to encourage the tendons to glide distally into view. This successfully brought the FDS slips into the wound. The FDP was more elusive. A small, atraumatic rubber catheter (e.g., paediatric feeding tube) was sometimes used to gently 'fish' for the profundus tendon within the sheath, or a small incision could be made in the palm (proximal to the A1 pulley) to guide the tendon distally with a tendon retriever. In this case, persistent milking and gentle exploration with a blunt hook were sufficient to bring the FDP end into the operative field.
Tendon Repair:
1.
Preparation:
The tendon ends were carefully debrided of any frayed or devitalized tissue using a sharp blade, ensuring clean, perpendicular cuts for optimal apposition. Minimal tendon substance was removed to preserve length.
2.
FDP Repair:
The FDP tendon was repaired first. A modified Kessler core suture technique was employed using 3-0 braided non-absorbable polyester suture (e.g., FiberWire®). This involves passing the suture longitudinally through the tendon, creating a locking configuration, and then tying it with sufficient tension to achieve good apposition without gapping. This technique provides strong initial repair strength.
3.
FDS Repair:
After the FDP was repaired, the two slips of the FDS tendon were meticulously identified. If only one slip is cut, it is generally repaired. If both are cut, both are repaired to maintain balance and strength. In this case, both slips were lacerated and required repair. Each FDS slip was repaired using a similar modified Kessler technique with 4-0 braided non-absorbable suture. It is crucial to ensure that the FDP glides smoothly beneath the repaired FDS slips and within the sheath.
4.
Epitendinous Suture:
Following the core suture repair of both FDP and FDS, a running epitendinous suture (e.g., 6-0 Prolene or Nylon) was applied to the circumference of each tendon repair. This superficial suture technique smooths the repair site, improves tensile strength by adding load-sharing, and promotes a gliding surface, thus minimizing friction and adhesion formation.
5.
Pulley System Management:
The A2 and A4 pulleys are critical for preventing tendon bowstringing and maintaining mechanical efficiency. These were carefully inspected. Fortunately, the laceration was between the A2 and A3 pulleys, thus sparing these crucial structures. If a pulley had been significantly damaged, a limited longitudinal vent or reconstruction would have been considered, but always with an emphasis on preserving as much of the original pulley system as possible.
Digital Nerve Repair:
The transected radial digital nerve was carefully isolated. Using microsurgical technique under an operating microscope, the nerve ends were meticulously coapted. An epineurial repair was performed using 8-0 non-absorbable monofilament sutures (e.g., Nylon) placed circumferentially to align the fascicular bundles. Tension-free repair was ensured.
Irrigation and Closure:
The surgical site was thoroughly irrigated with copious amounts of sterile saline to remove any debris or blood clots. Meticulous hemostasis was achieved. The skin flaps were then re-approximated and closed with 5-0 monofilament nylon sutures, using a tension-free closure.
Dressing and Splint Application:
A bulky soft dressing was applied, followed by a dorsal blocking splint. The splint was custom-molded to position the wrist in approximately 20-30 degrees of flexion, the metacarpophalangeal (MCP) joints in 50-70 degrees of flexion, and the interphalangeal (IP) joints in full extension. This specific position relaxes the repaired flexor tendons, minimizing tension on the repair and reducing the risk of re-rupture during the early healing phase.
Post-Operative Protocol & Rehabilitation
Post-operative rehabilitation is as critical as the surgical repair itself for optimal functional outcomes in flexor tendon injuries. Our protocol emphasizes early protected motion to prevent adhesions while safeguarding the repair. The patient was immediately referred to a specialized hand therapist.
Phase 1: Early Protected Mobilization (Weeks 0-4.5)
*
Immobilization:
The patient's hand remained in the dorsal blocking splint, maintaining the wrist in 20-30 degrees of flexion, MCPs in 50-70 degrees of flexion, and IP joints in full extension. This position is crucial for reducing tension on the repaired tendons.
*
Exercise Protocol (Modified Duran Protocol):
*
Passive Range of Motion (PROM):
Under the guidance of the hand therapist, the patient initiated passive flexion and extension exercises of the PIP and DIP joints within the confines of the splint. This involved 10 repetitions every waking hour.
*
Goal:
To promote tendon glide, prevent adhesions, and maintain joint mobility without actively stressing the repair.
*
Patient Education:
Emphasis on protecting the repair, avoiding active finger flexion, understanding signs of infection (redness, swelling, purulent discharge), and adhering strictly to the splint wear schedule (full-time).
*
Wound Care:
Regular dressing changes and monitoring of the incision site. Suture removal typically at 10-14 days post-op.
Phase 2: Gentle Active Motion & Splint Weaning (Weeks 4.5-7)
*
Initiation of Active Motion:
Gradual introduction of gentle active flexion and extension exercises for the PIP and DIP joints. These exercises were performed carefully, ensuring no resistance or excessive force.
*
Resistive Exercises:
Light, pain-free resistance exercises were started under therapist supervision. This may include gentle squeezing of soft foam or light gripping tasks.
*
Splint Adjustment/Weaning:
The dorsal blocking splint was gradually adjusted, and the degree of wrist and MCP flexion was reduced. Intermittent splint wear was initiated, particularly during sleep or activities where re-injury risk was higher.
*
Scar Management:
Initiation of scar massage and desensitization techniques for the nerve repair site.
*
Goal:
To increase active range of motion, begin strengthening, and further reduce adhesion formation.
Phase 3: Strengthening & Functional Recovery (Weeks 7-12)
*
Progressive Strengthening:
The intensity and resistance of exercises were progressively increased. This included using therapeutic putty, grip strengtheners, and light weights.
*
Functional Activities:
Integration of hand into daily functional activities.
*
Splint Discontinuation:
The dorsal blocking splint was typically discontinued by the end of this phase, with splinting potentially for specific activities or during the night if joint contractures were a concern.
*
Nerve Recovery:
Continued monitoring of nerve regeneration, including sensory mapping and two-point discrimination assessments. Desensitization and sensory re-education techniques were continued.
*
Goal:
To achieve full range of motion, restore strength, improve dexterity, and return to pre-injury functional levels.
Phase 4: Return to Activity (Weeks 12+)
*
Advanced Strengthening:
Continued progression of strengthening exercises.
*
Sport-Specific/Work-Specific Training:
If applicable, tailoring exercises to the patient's occupational or recreational demands.
*
Full Return to Activity:
Gradual return to strenuous activities, contact sports, or heavy manual labor, typically after 4-6 months, depending on individual progress and complete resolution of symptoms.
Throughout all phases, close collaboration between the surgeon, hand therapist, and patient is paramount. Regular follow-up appointments were scheduled to assess progress, address any complications (e.g., stiffness, infection, re-rupture, cold intolerance, neuroma formation), and adjust the therapy protocol as needed.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls:
- Clinical Examination is Paramount: The cornerstone of diagnosis for flexor tendon lacerations. Precise testing of FDS (isolate PIP flexion by extending adjacent fingers) and FDP (isolate DIP flexion by extending PIP) is critical. Do not underestimate pain-induced pseudo-paralysis – careful, gentle testing can differentiate.
- Verdan's Zones: Understanding the zones of injury (especially Zone II, "No Man's Land") guides prognosis, surgical approach, and expectations regarding post-operative rehabilitation challenges.
- Bruner Incision: Utilize a modified Bruner zig-zag incision for optimal exposure and to prevent scar contracture, particularly important in Zones I and II. Avoid straight longitudinal incisions across flexion creases.
- Tendon Retrieval: Be prepared for significant tendon retraction, especially of the FDP. Techniques include "milking" the forearm, using a small Foley catheter to inflate and pull the tendon, or making a small proximal palmar incision for retrieval.
- Strong Core Suture: Employ a robust core suture technique (e.g., modified Kessler, double modified Kessler, Lin-Tsai) using non-absorbable material (e.g., 3-0/4-0 braided polyester). This provides primary strength to resist early motion.
- Meticulous Epitendinous Repair: A running epitendinous suture (e.g., 6-0 Nylon/Prolene) is essential for smoothing the repair site, improving glide, increasing overall tensile strength, and preventing gapping.
- Pulley Preservation: Preserve the A2 and A4 pulleys at all costs. Damage to these leads to bowstringing and significant loss of mechanical advantage. Limited fenestration of the sheath or A3 pulley may be acceptable for exposure if necessary, but keep it minimal.
- Associated Injuries: Always check for and repair concomitant digital nerve and arterial injuries. These significantly impact long-term function and sensation. Microsurgical repair of digital nerves is critical.
- Early Protected Motion: This is the gold standard for flexor tendon rehabilitation (e.g., modified Duran or Kleinert protocols). It minimizes adhesions, preserves joint motion, and promotes tendon healing. Close collaboration with a specialized hand therapist is non-negotiable.
- Patient Compliance: Emphasize the critical role of patient adherence to the post-operative rehabilitation protocol. Non-compliance is a leading cause of complications.
Pitfalls:
- Missed Diagnosis: Failing to identify partial tendon lacerations or concomitant nerve injuries due to inadequate examination. Always assume full laceration until proven otherwise with careful testing.
- Inadequate Exposure: Attempting to perform the repair through a small, straight incision, leading to poor visualization, difficult tendon retrieval, and suboptimal repair.
- Excessive Tendon Debridement: Removing too much tendon substance can lead to significant gapping, making a tension-free repair difficult and potentially requiring grafting.
- Overly Tight Repair: Repairing tendons with excessive tension can impede blood supply, lead to a "locked" finger, and increase the risk of re-rupture or stiffness.
- Ignoring the Pulley System: Excision or severe damage to critical pulleys (A2, A4) results in irreversible bowstringing and functional deficit.
- Poor Tendon Handling: Traumatizing the tendon ends with aggressive clamps or excessive manipulation can compromise vascularity and healing.
- Insufficient Strength of Repair: Using too few sutures, inadequate technique, or absorbable sutures can lead to early re-rupture, especially with early motion protocols.
- Inadequate Post-Operative Management: Failure to refer to hand therapy, improper splinting, or allowing uncontrolled active motion too early are common causes of adhesions, stiffness, or re-rupture.
- Infection: Despite sterile technique, infection remains a risk, particularly in contaminated wounds. Aggressive irrigation and appropriate antibiotic prophylaxis are key.
- Adhesions: The most common complication, leading to stiffness and requiring tenolysis if severe. Early protected motion and meticulous surgical technique aim to minimize this.
- Re-rupture: A devastating complication, often requiring re-operation with potentially poorer outcomes. Usually due to non-compliance, too aggressive therapy, or an inherently weak repair.
