Patient Presentation & History
We present a case of a 32-year-old right-hand dominant male, a construction worker, who sustained multiple metacarpal fractures following a high-energy crush injury to his right hand. The mechanism involved his dominant hand becoming trapped between a heavy piece of equipment and a fixed structure at a construction site. He presented to the emergency department approximately 45 minutes post-injury.
His past medical history was notable only for well-controlled essential hypertension, managed with an ACE inhibitor. He was an active smoker, consuming approximately 15 pack-years. There was no history of diabetes mellitus, peripheral vascular disease, or previous hand injuries. He denied any allergies. His tetanus immunization status was up-to-date.
Upon initial assessment, he reported severe pain, inability to move his digits, and significant swelling of the right hand. He had no complaints of head injury, chest pain, or abdominal pain, suggesting a focused injury to the hand.
Clinical Examination
Initial examination revealed a significantly swollen, ecchymotic, and deformed right hand, particularly over the dorsum.
Inspection
- Gross Deformity: Obvious dorsal angulation and shortening visible in the 4th and 5th rays. The normal cascade of the digits was disrupted, with the 5th digit appearing to scissoring over the 4th digit in gentle flexion, indicative of malrotation.
- Skin Integrity: Two small, punctate lacerations were noted over the dorsum of the hand, one proximal to the 4th metacarpal head and another over the mid-shaft of the 5th metacarpal. These were less than 1 cm each and appeared to be caused by direct trauma, raising concern for an open fracture. No active bleeding was observed, but the skin around the lacerations was severely contused.
- Edema: Marked diffuse edema was present across the entire dorsum of the hand, extending to the wrist.
- Digital Cascade: Absent normal metacarpal arch and significant disruption of the digital cascade, particularly involving the ulnar two digits.
Palpation
- Tenderness: Exquisite tenderness was elicited globally across the dorsum of the hand, maximally over the shafts and necks of the 2nd, 4th, and 5th metacarpals.
- Crepitus: Palpable crepitus was noted with gentle attempts at movement and direct palpation over the involved metacarpals.
- Stability: Gross instability was appreciated with gentle stressing of the 4th and 5th metacarpals, indicating complete fracture displacement. The 2nd metacarpal fracture felt relatively less unstable compared to the ulnar two.
- Compartment Status: While significant edema was present, the hand compartments felt soft and compressible. Capillary refill was brisk in all digits (<2 seconds).
Range of Motion
- Active ROM: Severely limited and painful active flexion/extension of all metacarpophalangeal (MCP) and interphalangeal (IP) joints due to pain and swelling. The patient was unable to make a full fist.
- Passive ROM: Passive range of motion was also severely restricted by pain and guarding, but no fixed contractures were present. Attempts to passively flex the digits accentuated the rotational deformity of the 5th digit.
Neurological and Vascular Assessment
- Vascular: Radial and ulnar pulses were palpable at the wrist. Capillary refill was rapid (<2 seconds) in all digits. No pallor or cyanosis was observed. The overall perfusion to the hand and digits appeared intact.
-
Neurological:
- Motor: Patient was unable to fully extend or flex digits against resistance due to pain. Specific intrinsic motor function assessment was limited by pain, but gross observation suggested some preserved function without formal testing. The ability to abduct and adduct fingers was severely compromised.
- Sensory: Sensation to light touch and two-point discrimination was intact in the distribution of the median, ulnar, and radial nerves distally in all digits. No obvious areas of anesthesia or paresthesia were noted, which was reassuring given the high-energy mechanism.
In summary, the clinical picture was consistent with multiple, unstable, displaced metacarpal shaft fractures with associated significant soft tissue injury and suspicion of an open fracture, necessitating urgent imaging and definitive management.
Imaging & Diagnostics
Following the clinical assessment, immediate radiographic imaging of the right hand was performed.
X-ray Findings
Standard three-view (posteroanterior (PA), oblique, and true lateral) radiographs of the right hand were obtained.
*
PA View:
This view demonstrated significant shortening and dorsal angulation of the 4th and 5th metacarpals.
*
Second Metacarpal:
A transverse, comminuted shaft fracture of the right second metacarpal was identified, with approximately 10 degrees of dorsal angulation and 2 mm of shortening. This fracture appeared extra-articular.
*
Fourth Metacarpal:
A short oblique shaft fracture of the right fourth metacarpal was present, with approximately 30 degrees of dorsal angulation, 5 mm of shortening, and significant comminution at the fracture site. The distal fragment was displaced volarly and radially.
*
Fifth Metacarpal:
A highly unstable, spiral shaft fracture of the right fifth metacarpal was observed, with substantial dorsal angulation (approximately 45 degrees), 7 mm of shortening, and significant rotational displacement, manifesting as overlap of the distal shaft fragment over the 4th metacarpal on the PA view.
*
Oblique View:
The oblique view provided further clarity on the angulation and rotational deformities, confirming the complex nature of the 4th and 5th metacarpal fractures. Rotational malalignment was particularly evident in the 5th metacarpal.
*
Lateral View:
The lateral view was crucial for assessing the dorsal angulation of all fractures, which was most pronounced in the 4th and 5th metacarpals. The articular surfaces of the MCP and carpometacarpal (CMC) joints appeared congruent on all views, indicating no immediate concern for primary dislocations or articular involvement at these joints, though subtle injuries could not be entirely ruled out without further imaging.
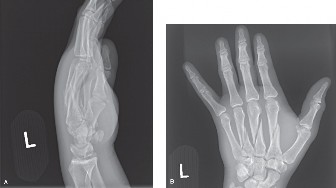
(Initial PA radiograph demonstrating comminuted transverse shaft fracture of the 2nd metacarpal, short oblique shaft fracture of the 4th metacarpal, and spiral shaft fracture of the 5th metacarpal with significant angulation, shortening, and rotational deformity.)
CT Scan Indications and Findings
Given the high-energy mechanism, suspicion of open fractures, multiple comminuted fractures, and the potential for subtle intra-articular extension or occult carpal injuries, a Computed Tomography (CT) scan of the right hand was indicated and performed.
*
CT Findings:
The CT scan confirmed the complex fracture patterns identified on X-ray, providing superior detail regarding comminution and displacement.
*
2nd Metacarpal:
Coronal and sagittal reconstructions confirmed a stable transverse fracture, with minimal comminution.
*
4th Metacarpal:
Axial and sagittal views better delineated the degree of dorsal comminution and confirmed the short oblique pattern. No intra-articular extension was found.
*
5th Metacarpal:
The spiral nature and multiplanar displacement of the 5th metacarpal fracture were precisely mapped. The CT scan confirmed severe rotational deformity and significant bone loss/comminution, particularly on the volar aspect, which would complicate stable fixation.
*
Carpal Bones:
The carpal bones and CMC joints were found to be intact, ruling out associated carpal fractures or major ligamentous injuries in this immediate context.
*
Soft Tissues:
The CT provided additional information on the extent of soft tissue swelling and contusion, but no overt foreign bodies were identified, and no obvious active extravasation was noted.
The CT scan was invaluable for pre-operative templating, allowing for precise measurement of fragment lengths, assessment of potential bone loss, and planning for hardware selection.
MRI Indications
While not routinely indicated for isolated metacarpal shaft fractures, an MRI might be considered in cases with suspected significant ligamentous injury (e.g., sagittal band rupture, CMC ligamentous instability), occult tendon injury, or if neurovascular compromise was equivocal after initial workup. In this specific case, based on the clear fracture patterns and intact neurovascular status, MRI was not deemed immediately necessary for acute surgical planning.
Templating
Pre-operative templating was performed using the CT images and high-resolution radiographs. This involved:
* Measuring the length of the intact metacarpals (primarily the 3rd) and estimating the required length for the fractured metacarpals to restore normal hand length.
* Assessing the fracture morphology to determine the most appropriate plate and screw configuration (e.g., standard vs. locking plates, plate length, screw count).
* Planning the incision approaches to minimize soft tissue dissection while allowing adequate exposure for reduction and fixation.
* Anticipating the potential for bone grafting for comminuted areas, especially in the 4th and 5th metacarpals where bone loss was noted.
Differential Diagnosis
The presentation of pain, swelling, deformity, and functional loss in the hand following trauma mandates a systematic approach to differential diagnosis to ensure accurate identification and appropriate management.
| Condition | Key Clinical Features | Key Imaging Features | Management Distinction |
|---|---|---|---|
| Multiple Metacarpal Fractures | Severe pain, gross deformity, palpable crepitus, disrupted digital cascade, inability to grip. Open wounds possible. | X-rays show clear fracture lines (transverse, oblique, spiral, comminuted), angulation, shortening, rotation. CT clarifies comminution and intra-articular extension. | Operative fixation for unstable, displaced, angulated, shortened, or rotationally malaligned fractures (as in our case). Goals: anatomical reduction, stable fixation, early mobilization. Non-operative for stable, minimally displaced fractures. |
| Carpal Fractures | Localized tenderness over specific carpal bones (e.g., scaphoid snuffbox, hamate hook), wrist pain, limited wrist ROM. | X-rays may be subtle (e.g., scaphoid), often requiring repeat views, CT (gold standard for complex carpal fractures), or MRI (for occult fractures or ligament injury). | Management varies by carpal bone and fracture pattern: Scaphoid often requires casting/surgery. Hamate hook may require excision. Lunate/perilunate dislocations are surgical emergencies. |
| Metacarpophalangeal (MCP) Joint Dislocation | Deformity at the MCP joint, painful, restricted motion, prominent metacarpal head volarly or dorsally. | X-rays show loss of articular congruence between metacarpal head and proximal phalanx base. May be simple or complex (with interposition of soft tissues). | Closed reduction under regional anesthesia is the primary treatment. Open reduction may be necessary for complex dislocations or irreducible cases (e.g., volar plate interposition). Often no associated fracture. |
| Tendon Laceration/Rupture | Inability to actively move digit(s) against gravity in specific planes (e.g., inability to extend finger for extensor, inability to flex for flexor). Often a penetrating injury or forceful contracture. | X-rays typically normal unless avulsion fracture present. Ultrasound can visualize tendon disruption. MRI is sensitive for partial tears, ruptures, and retraction. | Surgical repair of the tendon is typically required for complete lacerations/ruptures to restore function. Differs significantly from bone fixation. |
| Severe Hand Contusion with Soft Tissue Swelling | Diffuse pain and swelling, ecchymosis, but no gross deformity. Pain with palpation but no crepitus. | X-rays are negative for fracture or dislocation. May show soft tissue swelling. | Conservative management: RICE (rest, ice, compression, elevation), pain control, early gentle mobilization as tolerated. No surgical intervention for the contusion itself. |
In this specific case, the presence of gross deformity, palpable crepitus, significant angulation and shortening on X-ray, and a clear history of high-energy trauma strongly supported the diagnosis of multiple metacarpal fractures and guided immediate surgical planning. The associated punctate skin lacerations converted these from closed to open fractures, necessitating urgent debridement and antibiotic prophylaxis.
Surgical Decision Making & Classification
The decision for operative intervention in this patient's case was straightforward and guided by several critical factors, primarily the nature of the fractures and the anticipated functional outcome with non-operative management.
Why Operative vs. Non-operative?
Non-operative management for metacarpal fractures typically involves closed reduction and casting or splinting. This approach is generally reserved for:
* Minimally displaced, stable fractures (e.g., angulation < 10-15 degrees for 2nd/3rd metacarpals, < 20-30 degrees for 4th/5th, shortening < 2-3 mm, no rotational deformity).
* Non-displaced or stable buckle fractures.
* Patients with significant comorbidities precluding surgery.
In contrast, our patient presented with:
1.
Multiple Fractures:
Fractures involving the 2nd, 4th, and 5th metacarpals significantly disrupt the normal architecture and biomechanics of the hand. Maintaining reduction of multiple unstable fractures with non-operative methods is exceedingly difficult and unlikely to yield an acceptable functional outcome.
2.
Significant Displacement:
The 4th and 5th metacarpals demonstrated substantial dorsal angulation (30-45 degrees) and shortening (5-7 mm). Even the 2nd metacarpal had 10 degrees of angulation and 2mm of shortening. These degrees of displacement exceed accepted thresholds for non-operative treatment, particularly in a young, active, working-age patient whose livelihood depends on hand function.
3.
Rotational Malalignment:
The spiral fracture of the 5th metacarpal exhibited significant rotational deformity, evident by scissoring of the digits on clinical examination. Rotational malunion is one of the most debilitating complications of metacarpal fractures, leading to significant functional impairment (finger overlap during gripping) that is poorly tolerated and extremely difficult to revise. This is an absolute indication for operative fixation.
4.
Open Fractures:
The presence of small punctate lacerations communicating with the fracture sites classified these as Gustilo-Anderson Type I open fractures. Open fractures mandate surgical debridement and irrigation to prevent infection, often combined with stable internal fixation.
5.
Comminution:
The comminution, especially in the 4th and 5th metacarpals, indicates inherent instability and a higher likelihood of collapse or displacement if treated non-operatively, even if an initial reduction is achieved.
Given these factors, open reduction and internal fixation (ORIF) was the only viable option to restore anatomical alignment, provide stable fixation, facilitate early mobilization, and minimize the risk of complications such as malunion, nonunion, and post-traumatic arthritis.
Classification Systems
-
Anatomical Location:
- Metacarpal Shaft Fractures: All three fractures (2nd, 4th, 5th) involved the shaft of the metacarpals.
- This distinction is crucial as shaft fractures generally tolerate less angular deformity in the 2nd and 3rd metacarpals (more rigid) compared to the more mobile 4th and 5th rays.
-
Fracture Pattern:
- 2nd Metacarpal: Transverse, comminuted.
- 4th Metacarpal: Short oblique, comminuted.
- 5th Metacarpal: Spiral, highly comminuted.
- The spiral nature of the 5th metacarpal fracture inherently predisposes to significant rotational instability, reinforcing the need for plate fixation.
-
Displacement & Angulation:
- 2nd Metacarpal: Displaced, dorsally angulated (10°), shortened (2mm).
- 4th Metacarpal: Displaced, dorsally angulated (30°), shortened (5mm), radially angulated.
- 5th Metacarpal: Displaced, severely dorsally angulated (45°), shortened (7mm), significantly rotationally malaligned.
-
Gustilo-Anderson Classification (for Open Fractures):
- The two small punctate lacerations associated with the fractures classified them as Gustilo-Anderson Type I open fractures . This implies a wound size less than 1 cm, minimal soft tissue damage, and usually a simple fracture pattern, though our fracture patterns were complex. This classification dictated immediate irrigation and debridement, along with intravenous antibiotic prophylaxis.
The combination of multiple unstable, displaced, angulated, shortened, and rotationally malaligned shaft fractures, along with their open nature, solidified the indication for urgent surgical intervention.
Surgical Technique / Intervention
The patient was taken to the operating theatre on an emergent basis for irrigation, debridement, and open reduction and internal fixation of the multiple metacarpal fractures.
Pre-operative Preparation and Anesthesia
- Anesthesia: General endotracheal anesthesia was administered. A regional block (axillary block) was performed prior to the general anesthetic to provide excellent post-operative pain control and muscle relaxation during the procedure.
- Positioning: The patient was positioned supine on the operating table. The right upper limb was prepped and draped free, allowing full manipulation and fluoroscopic access. A hand table was used to support the limb. A tourniquet was applied to the upper arm for a bloodless field, inflated to 250 mmHg after limb exsanguination.
- Antibiotics: Intravenous broad-spectrum antibiotics (e.g., Cefazolin and Gentamicin, or Clindamycin for penicillin-allergic patients) were administered pre-operatively due to the open nature of the fractures.
Surgical Approach and Debridement
- Debridement & Irrigation: The two small punctate lacerations were formally extended and thoroughly debrided. Copious irrigation with several liters of sterile saline solution was performed to remove any potential contaminants from the fracture sites. Devitalized tissue was sharply excised.
- Incisions: A single dorsal longitudinal incision was utilized to expose the 2nd, 4th, and 5th metacarpal shafts. For the 2nd metacarpal, the incision was made between the 1st and 2nd extensor compartments. For the 4th and 5th metacarpals, a curvilinear incision was made dorsal to the 4th metacarpal, raising a flap to expose both shafts. Meticulous care was taken to identify and protect the dorsal sensory nerves (branches of the radial and ulnar nerves) and extensor tendons. The extensor tendons were gently retracted radially or ulnarly, or occasionally split longitudinally between the compartments if necessary, to gain access to the bone. Minimal periosteal stripping was employed to preserve vascularity.
Reduction Techniques
- Indirect Reduction: Initial attempts at indirect reduction were made using finger traps on the involved digits with counter-traction at the wrist. This technique often helps to restore length and correct some angulation.
-
Direct Reduction:
For the significantly displaced and comminuted fractures, direct manipulation of the fragments was necessary.
- K-wires as Joysticks: Small K-wires (1.0 mm or 1.2 mm) were temporarily inserted into the distal and proximal fragments to serve as joysticks, facilitating precise control and alignment.
- Rotational Correction: Rotational alignment was critically assessed by simultaneously flexing the fingers to confirm the correct digital cascade and ensure no scissoring. This was performed before final plate fixation.
- Length Restoration: Restoration of metacarpal length was paramount to prevent intrinsic muscle tightness and preserve grip strength. This was achieved through traction and direct manipulation, often facilitated by the temporary K-wires.
- Fluoroscopic Guidance: Intraoperative fluoroscopy (C-arm) was used extensively to confirm satisfactory reduction in multiple planes (AP, lateral, oblique) before and after temporary fixation, and after final plating.
Fixation Construct
A strategy of sequential fixation was employed, starting with the least comminuted and most amenable fracture, then moving to the more complex ones.
*
2nd Metacarpal:
This transverse shaft fracture was reduced and fixed with a 1.5 mm low-profile locking plate with 5 holes, applying a compression technique to achieve interfragmentary compression. Two bicortical screws were placed proximally and two distally, avoiding the articular surfaces.
*
4th Metacarpal:
The short oblique, comminuted shaft fracture required careful reduction. A 1.5 mm low-profile locking plate (6 holes) was applied. Due to the comminution, the plate acted as a bridging plate, and locking screws were strategically placed. One lag screw was applied through the plate for interfragmentary compression of the oblique component, augmenting stability.
*
5th Metacarpal:
The highly unstable spiral and comminuted fracture posed the greatest challenge. After achieving anatomical reduction and confirming rotational alignment, a 1.5 mm low-profile locking plate (7 holes) was contoured and applied to the dorsal surface. Given the significant comminution and potential for bone void, the plate served primarily as a neutralization and bridging plate, with careful placement of locking screws to buttress the fragments. No primary lag screw was feasible given the comminution.
* In cases of severe comminution or bone loss, judicious use of autogenous bone graft (e.g., from the distal radius or olecranon) might be considered, but in this case, sufficient cortical contact was achieved to allow for primary plate fixation without grafting.
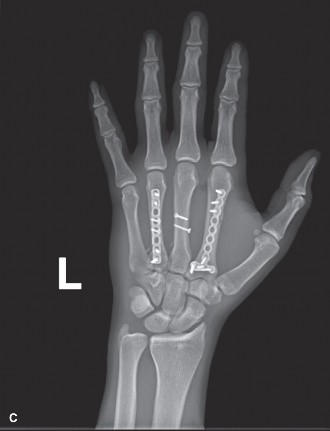
(Post-operative PA radiograph demonstrating anatomical reduction and stable internal fixation of the 2nd, 4th, and 5th metacarpal fractures with low-profile locking plates and screws.)
Post-Fixation Assessment
- Fluoroscopy: Final fluoroscopic images confirmed anatomical reduction in all planes, appropriate implant placement, and restoration of metacarpal length.
- Stability: The construct was stable to gentle stress.
- Soft Tissues: The extensor tendons were checked for smooth gliding without impingement by the hardware.
- ROM: Passive digital range of motion was assessed; the fingers moved freely without impingement and the digital cascade was restored.
- Wound Closure: The wounds were thoroughly irrigated again. The periosteum and extensor mechanism were closed anatomically. The skin was closed with simple interrupted sutures. A sterile dressing was applied.
Post-Operative Protocol & Rehabilitation
The post-operative management focused on early rehabilitation to prevent stiffness, promote functional recovery, and minimize complications, while ensuring fracture healing.
Immediate Post-Operative Period (Day 0-7)
- Immobilization: A well-padded bulky dressing incorporating a dorsal protective plaster splint (or volar if preferred by surgeon) was applied, maintaining the wrist in 20-30 degrees of extension, MCP joints in 70-90 degrees of flexion, and IP joints in full extension (the "position of safety"). This position protects the repair while preventing MCP collateral ligament shortening. The splint was removed for therapy.
- Elevation: Strict hand elevation above heart level was encouraged to minimize swelling.
- Pain Management: Multimodal analgesia was provided, leveraging the pre-operative regional block and transitioning to oral opioids and NSAIDs.
- Wound Care: The dressing was changed on post-operative day 2-3, and the wounds were inspected for signs of infection. Oral antibiotics (e.g., Cephalexin) were continued for 5-7 days for the open fractures.
- Early Motion: Under the guidance of a hand therapist, the patient began gentle active range of motion (AROM) exercises for the uninjured wrist, elbow, and shoulder. For the injured hand, very gentle, protected AROM of the IP joints was initiated within the splint, avoiding excessive stress on the healing metacarpals. Gentle passive range of motion (PROM) for the MCP joints was initiated with caution to the extent tolerated, staying within pain limits.
Early Mobilization Phase (Weeks 1-4)
- Splinting: The static dorsal splint was continued for protection, especially during sleep and activities of daily living (ADLs). A dynamic splint or a custom thermoplastic splint might be fabricated to assist with specific range of motion if progress was slow.
-
Therapy Focus:
- Edema Control: Continued elevation, light compression gloves, and retrograde massage.
- AROM Progression: Gradually increased AROM of all digits, including MCP and IP joints, within pain tolerance. Specific exercises aimed at restoring full flexion and extension.
- PROM: Carefully progressed PROM of the MCP and IP joints, ensuring no undue stress on the fracture sites.
- Scar Management: Gentle scar massage commenced once the wounds were healed (around 2 weeks post-op) to prevent adhesions.
- Avoidance: Heavy lifting, gripping, or forceful activities were strictly prohibited. The patient was instructed to avoid pushing through pain.
Intermediate Phase (Weeks 4-8)
- Splint Discontinuation: The protective splint was typically weaned off during the day around 4-6 weeks post-op, but often continued at night for another 2-4 weeks.
-
Therapy Focus:
- Strengthening: Gradual introduction of isometric strengthening exercises, progressing to light resistance band exercises and putty exercises.
- Functional Activities: Integration of hand into light functional tasks.
- Full ROM: Aim for restoration of full, pain-free AROM and PROM of all joints.
- Radiographic Assessment: Follow-up X-rays were performed at 6 weeks to assess fracture healing and ensure no loss of reduction.
Advanced Phase (Weeks 8-12+)
- Progressive Strengthening: Intensified strengthening program, including grip, pinch, and dexterity exercises.
- Return to Activity: Gradual return to work-specific tasks and recreational activities. For a construction worker, this phase would involve significant work hardening and functional rehabilitation.
- Full Return: Full, unrestricted return to heavy labor or sports activities typically occurred at 3-4 months post-operatively, provided radiographic healing was confirmed and strength/ROM goals were met.
- Complication Monitoring: Continued monitoring for potential complications such as stiffness, nonunion, malunion, hardware irritation, nerve irritation, or complex regional pain syndrome (CRPS). Hardware removal (typically 6-12 months post-op) may be considered if symptoms related to prominent hardware develop, though often not routinely necessary.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls
- Pre-operative Planning is Paramount: Thorough review of radiographs (PA, oblique, lateral) and CT scans to understand fracture pattern, comminution, and displacement (angulation, shortening, rotation). Template implants to optimize length and fit.
- Rotational Assessment: Critically evaluate and correct rotational deformity. This is best done with the digits simultaneously flexed, checking the digital cascade and ensuring no scissoring. A malunited rotation is poorly tolerated and extremely difficult to revise.
- Anatomical Reduction: Strive for anatomical reduction, especially of intra-articular fractures. For shaft fractures, restoring length, angulation, and rotation is key.
- Stable Fixation: Choose an implant and technique that provides stable fixation to allow for early motion. Low-profile locking plates are often preferred for shaft fractures, especially comminuted or spiral patterns, providing multiplanar stability. K-wires may be used for temporary fixation or as joysticks.
- Soft Tissue Handling: Meticulous soft tissue technique is crucial. Minimize periosteal stripping to preserve vascularity. Utilize appropriate incisions (e.g., dorsal longitudinal incisions with careful retraction of extensor tendons and dorsal sensory nerves).
- Early Mobilization: The hand is prone to stiffness. Early, controlled active and passive range of motion under therapist guidance is essential to prevent adhesions and maintain joint mobility. Stable fixation enables this.
- Prophylactic Antibiotics: For open fractures, administer intravenous antibiotics promptly and continue post-operatively. Ensure thorough debridement and irrigation.
- Functional Outcomes: The goal is not just bone union, but a functional hand. Consider the patient's age, occupation, and demands on their hand when planning surgery and rehabilitation.
Pitfalls
- Inadequate Rotational Correction: The most common and functionally disabling complication. Often subtle, but evident on clinical exam (scissoring of fingers during flexion). Always re-check rotation before final fixation and after closure.
- Loss of Reduction/Unstable Fixation: Choosing an inadequate implant or applying it incorrectly (e.g., too short a plate, insufficient screws, inadequate screw purchase in comminuted bone) can lead to hardware failure, loss of reduction, and malunion or nonunion.
- Excessive Soft Tissue Dissection: Overzealous periosteal stripping or unnecessary dissection can devascularize fragments, increasing risks of nonunion and infection, and prolonging healing.
- Hardware Prominence/Irritation: Dorsal plates, especially on the 2nd and 5th metacarpals, can be prominent and irritate extensor tendons or overlying skin. Low-profile plates are preferred. May necessitate hardware removal later.
- Nerve Injury: Damage to dorsal sensory nerves (branches of radial or ulnar nerve) during the approach or retraction can lead to painful neuromas or persistent paresthesia. Careful dissection and protection are vital.
- Delayed Mobilization/Stiffness: Prolonged immobilization is a recipe for stiffness, particularly of the MCP joints. If fixation is stable, early motion is critical.
- Malunion/Nonunion: Inadequate reduction, unstable fixation, or significant comminution/bone loss can lead to malunion (deformity) or nonunion (failure to heal), both requiring potentially complex revision surgery.
- Complex Regional Pain Syndrome (CRPS): A debilitating complication that can occur after any hand trauma or surgery. Early recognition (disproportionate pain, swelling, skin changes) and aggressive management are critical.

