FOCAL DYSTONIA OF THE HAND
Idiopathic focal hand dystonia is a highly debilitating, task-specific movement disorder characterized by involuntary, sustained muscle contractions that cause abnormal postures or twisting movements. These muscle cramps strictly accompany the execution of specific, highly practiced motor tasks. In clinical practice, these task-specific dystonias involving the hand are frequently referred to by their occupational triggers, including writer’s cramp, keyboarder’s cramp, occupational hand cramp, musician’s cramp, or the golfer’s “yip.”
While focal dystonia is primarily a neurological condition, patients almost exclusively present to orthopedic or hand surgery clinics first, complaining of stiffness, cramping, or loss of dexterity. It is incumbent upon the orthopedic surgeon to recognize this pathology to prevent unnecessary surgical interventions.
Pathophysiology and Biomechanics
Although there are documented cases of focal dystonia emerging after peripheral musculoskeletal trauma, paravertebral injury, or central nerve injury, the vast majority of cases are idiopathic. The underlying pathophysiology is believed to involve a profound dysfunction in the integration and circuitry of the basal ganglia, the sensory thalamus, and the somatosensory and sensorimotor cortices.
Extensive functional MRI (fMRI) and electroencephalogram (EEG) studies have demonstrated maladaptive neuroplasticity in these patients. In a healthy individual, the somatosensory cortex maintains distinct, well-defined representations for each digit. In patients with focal hand dystonia (particularly musicians and writers), these cortical representations become blurred or overlapping. This degradation of sensory feedback leads to a failure of surround inhibition in the motor cortex, causing agonist and antagonist muscles to co-contract simultaneously during specific tasks.
Clinical Evaluation and Differential Diagnosis
A meticulous history and physical examination are paramount. The hallmark of focal hand dystonia is its task-specificity; the hand may function perfectly during activities of daily living (e.g., buttoning a shirt, using a fork) but will immediately posture abnormally the moment a pen or musical instrument is grasped.
Clinical Pearl: Look for a geste antagoniste (sensory trick). Many patients with focal dystonia can temporarily relieve their involuntary muscle contractions by lightly touching the affected limb or altering their grip in a non-standard way.
The differential diagnosis for task-specific hand cramping is extensive. The orthopedic surgeon must systematically rule out:
* Peripheral Neuropathy: Carpal tunnel syndrome, cubital tunnel syndrome, or radial tunnel syndrome.
* Radiculopathy and Plexopathy: Cervical nerve root compression or brachial plexus lesions.
* Thoracic Outlet Syndrome (TOS): Neurogenic or vascular compression at the thoracic inlet.
* Repetitive Overuse Injuries: Tenosynovitis, intersection syndrome, or tendinosis.
* Vascular Anomalies: Exercise-induced thrombosis of the radial artery or ulnar artery pseudoaneurysms (which can present as delayed nerve palsy).
* Neurological Disorders: Focal seizures, early-onset Parkinson's disease, or medication-induced extrapyramidal effects.
* Psychogenic Movement Disorders: Conversion disorders or factitious disorders.
Management Protocols for Focal Dystonia
Because focal hand dystonia is fundamentally a central neurological problem, traditional orthopedic interventions (e.g., tendon transfers, releases, or neurolysis) are strictly contraindicated and will not yield functional improvement.
1. Chemodenervation (Botulinum Toxin)
The current gold standard for symptomatic management is the targeted injection of Botulinum toxin type A. This neurotoxin blocks the presynaptic release of acetylcholine at the neuromuscular junction, effectively weakening the overactive muscles.
* Technique: Injections must be highly precise, often requiring electromyographic (EMG) or ultrasound guidance to isolate the specific fascicles of the flexor digitorum superficialis (FDS), flexor digitorum profundus (FDP), or intrinsic muscles responsible for the dystonic posture.
* Limitations: Botulinum toxin is not a cure; it merely targets the peripheral symptoms. Injections must be repeated every 3 to 4 months, and there is a risk of transient, unwanted weakness in adjacent digits.
2. Sensorimotor Retraining
Because the etiology involves maladaptive cortical plasticity, proprioceptive activities and sensorimotor retraining are highly recommended. Techniques such as Braille reading, sensory discrimination tasks, and mirror visual feedback therapy aim to restore the distinct cortical mapping of the digits.
PSYCHOGENIC AND FACTITIOUS POSTURES OF THE HAND
In stark contrast to focal dystonia, psychogenic movement disorders and factitious postures of the hand are rooted in psychiatric illness. These conditions present a unique and frustrating challenge for the orthopedic surgeon. Patients may present with severe, rigid deformities that mimic organic pathology but lack any underlying anatomical or neurological deficit.
Psychoflexed and Psychoextended Hands
At least two typical, severe postures of the hand are strongly associated with psychiatric disorders: the psychoflexed hand and the psychoextended hand.
In the psychoflexed hand, the ulnar three digits (long, ring, and small fingers) are severely flexed and contracted into the palm. This posture is rigidly maintained by the patient, often leading to severe secondary complications.
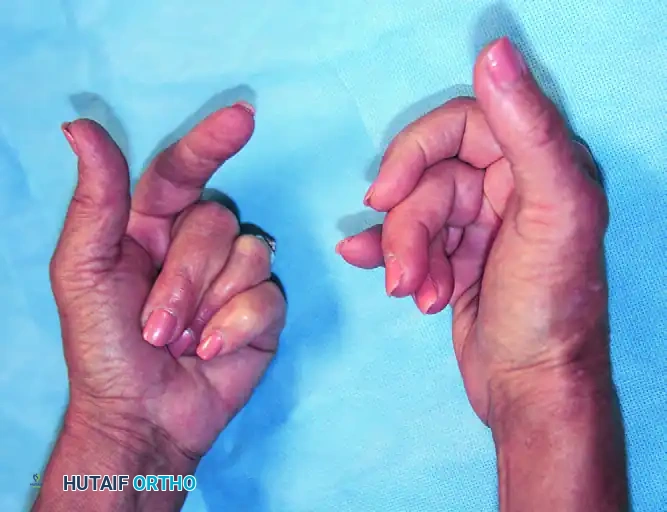
FIGURE 70-14 Psychoflexed hands. Patient had flexion contractures of the ulnar three fingers of both hands with severe palmar maceration.
Biomechanics and Complications:
Initially, the flexion is purely active and driven by the patient's psychiatric state. However, prolonged maintenance of this posture leads to true organic contractures. The volar plates of the metacarpophalangeal (MCP) and proximal interphalangeal (PIP) joints become fibrotic and shortened. The collateral ligaments contract, and the flexor tendons may develop adhesions.
A critical complication of the psychoflexed hand is palmar maceration. The tightly clenched fingernails dig into the palmar skin, creating a dark, moist environment that is highly susceptible to fungal and bacterial infections.
Surgical Warning: The surgeon must be acutely aware that almost nothing is of lasting functional help for the psychoflexed hand. Casting, physical therapy, and soft-tissue releases will inevitably fail if the underlying psychiatric disorder is not addressed. The posture will quickly recur postoperatively.
Clenched Fist Syndrome
Clenched fist syndrome is a specific variant of factitious disorder or conversion reaction. It typically presents in young to middle-aged females, often with a complex medical history of multiple hospital admissions for vague pain syndromes, headaches, or unexplained neurological deficits.
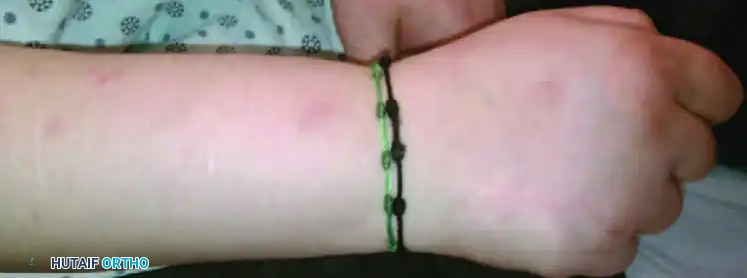
FIGURE 70-15 (A) Dorsal aspect of the hand and wrist in a patient with clenched fist syndrome. Note the presence of tightly bound bracelets, which may serve as factitious constriction bands.

FIGURE 70-15 (B) Volar aspect of the same patient. The clenched fist posture is rigidly maintained, often resisting passive extension.
Clinical Presentation:
The patient presents with tightly clenched fists. When the examiner attempts passive extension of the digits, they will feel paradoxical, active resistance from the patient's flexor muscles. If the examiner manages to force the fingers into extension, the patient will often exhibit a "give-way" weakness, and upon release, the fingers will instantly snap back into the clenched posture. Over time, persistent stretching and abnormal posturing can lead to increased hyperextension instability at the PIP joints.
Interestingly, these patients are rarely distressed by their severe functional deficit. They may exhibit la belle indifférence (a naive, inappropriate lack of emotion or concern about their disability) and rarely demand treatment to correct the posture, though they may passively permit surgery to be performed.
SECRETAN DISEASE AND FACTITIOUS LYMPHEDEMA
Secretan Disease (Peritendinous Fibrosis)
First described by Henri-François Secretan in 1901, Secretan disease is characterized by a hard, brawny, edematous process over the dorsal metacarpal area of the hand. Historically referred to as peritendinous fibrosis or factitious lymphedema, the etiology of this condition has been heavily debated but is now widely considered to be the result of repetitive, self-inflicted blunt trauma.
Pathophysiology:
The patient repeatedly strikes the dorsum of their hand against a hard surface, usually in private. This repetitive microtrauma causes chronic inflammation, leading to the proliferation of fibroblasts and the deposition of dense mucopolysaccharides and peritendinous fibrosis around the extensor tendons. The condition is driven by a desire for secondary gain (e.g., worker's compensation, avoidance of duty) or as a manifestation of a conversion reaction.
Diagnostic Modalities: The "Cast Test"
Diagnosing Secretan disease requires a high index of suspicion. The definitive diagnostic maneuver is the application of a well-padded, rigid short-arm cast.
* Mechanism: The cast physically prevents the patient from inflicting further trauma to the dorsum of the hand.
* Result: If the edema rapidly resolves while the cast is on, but mysteriously recurs within days or weeks after the cast is removed, the diagnosis of factitious trauma is established.
* Pitfall: Most of these patients are non-compliant and will not wear the cast long enough to make a difference, often removing it themselves or complaining of unbearable, unexplainable pain beneath the plaster.
Factitious Constriction and Vascular Complications
Another manifestation of factitious hand disorders involves the intentional application of constricting bands (e.g., rubber bands, tight bracelets, or strings) to the proximal forearm or arm.
Clinical Evaluation:
Always inspect the entire extremity meticulously for evidence of a constricting band proximally. Look for circumferential indentations, bruising, or abrasions. The resulting distal edema varies in severity depending on the length of time, the frequency, and how recently the limb has been constricted. The constriction is usually applied when the individual is alone and removed before medical evaluation.
Vascular Pathologies Mimicking or Resulting from Factitious Trauma:
It is critical to rule out organic, anatomical bases for the patient's complaints. However, the surgeon must also recognize that self-inflicted trauma can cause true, organic vascular emergencies.
* Thrombosis: Repetitive blunt trauma or prolonged application of constricting bands can cause intimal damage to the radial or ulnar arteries, leading to spontaneous thrombosis.
* Pseudoaneurysms: Minor, self-inflicted penetrating trauma (often hidden or denied by the patient) can result in false aneurysms (pseudoaneurysms) of the ulnar or radial artery. For instance, an ulnar artery pseudoaneurysm in Guyon's canal may present as a delayed ulnar nerve palsy, mimicking a psychoflexed hand or organic compressive neuropathy.
PRINCIPLES OF MANAGEMENT AND SURGICAL CONSIDERATIONS
The Limitations of Operative Intervention
The most critical tenet in managing psychogenic and factitious disorders of the hand is that surgery is rarely, if ever, beneficial.
Operating on a clenched fist syndrome or Secretan disease is fraught with peril. Tendon lengthenings, volar plate releases, and fasciectomies will fail because the underlying psychiatric drive to maintain the posture remains intact. The patient will actively overpower the surgical repair, leading to ruptured tendons, severe scar formation, and a worse clinical picture than before.
Salvage Procedures for Severe Complications
While functional reconstructive surgery is contraindicated, salvage procedures may occasionally be required for severe, life-threatening, or limb-threatening complications of long-standing psychogenic postures.
Indications for Salvage Surgery:
1. Intractable Palmar Maceration: When the nails have eroded through the palmar skin, causing deep space infections or osteomyelitis of the metacarpals.
2. Ischemic Necrosis: Due to severe, unyielding flexion contractures compromising digital perfusion.
Surgical Options:
* Joint Arthrodesis: Fixation of the PIP or MCP joints in a functional or extended position using Kirschner wires (K-wires) or plates. This is done purely to allow for palmar hygiene and prevent skin breakdown.
* Amputation: In extreme cases where the fingertips are necrotic or the palmar infection is uncontrollable, terminal amputation of the involved digits may be the only viable option to eradicate infection.
Surgical Pearl: Even when performing salvage arthrodesis or amputation, the surgeon must secure robust psychiatric support. Patients with factitious disorders may intentionally infect their surgical wounds or manipulate their K-wires postoperatively.
Multidisciplinary Postoperative and Psychiatric Protocols
The management of these complex patients cannot be undertaken by the orthopedic surgeon alone. A multidisciplinary approach is mandatory.
- Psychiatric Intervention: Psychological assistance and psychiatric counseling should be obtained as early as possible in the course of evaluation. The primary treatment for clenched fist syndrome, psychoflexed hands, and Secretan disease is psychiatric, not surgical.
- Conservative Orthopedic Care: Focus on non-operative modalities. Use soft, absorbent dressings (e.g., zinc oxide or silver-impregnated gauze) placed gently into the palm to manage maceration.
- Physical Therapy: Gentle, passive range-of-motion exercises and progressive splinting can be attempted, though the surgeon must set realistic expectations, as patient compliance will be exceptionally poor.
- Vascular Monitoring: Continuously monitor the limb for signs of factitious vascular compromise, utilizing Doppler ultrasound or angiography if thrombosis or pseudoaneurysm is suspected secondary to self-harm.
Ultimately, the orthopedic surgeon's role in focal dystonia and factitious hand disorders is one of astute diagnosis, protection of the limb from unnecessary surgical harm, and careful orchestration of multidisciplinary care.
