EXTRACTION OF A BROKEN FEMORAL ANTEGRADE NAIL
The fatigue failure and subsequent breakage of a femoral intramedullary (IM) nail is a complex complication, almost exclusively resulting from fracture nonunion. When the bone fails to heal, the continuous cyclical loading of weight-bearing is transferred entirely to the implant, eventually exceeding its endurance limit. Extracting a broken antegrade femoral nail demands meticulous preoperative planning, a comprehensive understanding of femoral biomechanics, and a mastery of specialized extraction techniques.
Preoperative Planning and Equipment
Before attempting extraction, the surgeon must identify the exact make, model, and diameter of the broken nail. This dictates the inner cannula diameter, which is critical for the guidewire wedging technique.
💡 Clinical Pearl: The Extraction Arsenal
Never begin a broken nail extraction without a comprehensive extraction system on standby. Your setup must include universal sliding extractors, vice-grip (locking) pliers, multiple lengths of ball-tipped and smooth guidewires (1.5 mm to 3.2 mm), rigid reamers, and metal-cutting carbide drills in the event of cold-welded locking screws.
Step-by-Step Surgical Technique
The closed extraction of the distal segment of a broken nail relies on the principle of internal friction. By wedging multiple wires within the hollow cannula of the nail, the surgeon creates an interference fit robust enough to withstand the axial pull of a slap hammer.
- Patient Positioning: Position the patient supine on a fracture table or in the lateral decubitus position on a radiolucent flat table, depending on the planned revision fixation. Ensure high-quality fluoroscopic visualization of the entire femur in both anteroposterior (AP) and lateral planes.
- Hardware Removal: Systematically remove all proximal and distal locking screws.
> ### ⚠️ Surgical Warning
> A common pitfall is failing to identify and remove a distal locking screw that has been obscured by heterotopic ossification or robust callus. Verify the removal of all screws fluoroscopically before attempting extraction. - Proximal Approach: Utilize the previous surgical incision to approach the proximal femur. Insert a long 3.2-mm guide pin through the greater trochanter or piriformis fossa entry site, directing it into the proximal segment of the broken nail.
- Clearing the Aperture: Over time, heterotopic bone and dense fibrous tissue will encapsulate the proximal end of the nail. Use rigid curettes, a cannulated awl, or a rigid reamer over the guide pin to meticulously clear the driving end of the nail.
- Proximal Segment Extraction: Attach the manufacturer-specific extraction device to the proximal nail segment and remove it using gentle back-slapping.
- Guidewire Insertion: Remove the initial guide pin. Insert a robust, hooked guidewire (or a ball-tipped guidewire) down the medullary canal. Carefully navigate it through the fracture site and advance it through the hollow cannula of the retained distal broken nail segment until the hook/ball exits the distal tip of the nail.
- The Wedging Technique: Once the hooked wire is engaged at the distal tip, wedge it by passing multiple smaller, smooth guidewires (e.g., 2.0 mm or 1.5 mm) down the cannula alongside the primary hooked wire.
- Biomechanics of Wedging: This step aligns the broken ends, making the distal segment act as a single unit with the wires. The friction generated prevents the hooked wire from pulling back through the nail.
- Deformity Correction: If angular deformity is present at the nonunion site, manipulation of the femur is necessary to allow for a "linear" extraction, preventing the nail from catching on the endosteal cortex.
- Grasping and Extraction: Bundle the proximal ends of the multiple guidewires protruding from the hip. Grasp them firmly with locking (vice-grip) pliers. Attach the pliers to a universal sliding extractor (slap hammer).
- Nail Removal: Carefully extract the distal nail segment with gentle, consistent mallet blows.
If the closed wedging technique is unsuccessful due to severe incarceration or a solid distal bony pedestal, an open approach may be necessary. This involves creating a small cortical window distal to the nail tip to drive the nail retrogradely, or utilizing specialized over-reaming techniques (e.g., using a trephine reamer) to free the incarcerated segment.
MANAGEMENT OF INFECTIONS AFTER INTRAMEDULLARY FIXATION
A deep infection following either open or closed intramedullary fixation is a devastating complication that threatens both limb viability and patient life. The literature demonstrates a clear correlation between the method of reduction and infection rates. Open reduction and intramedullary fixation carry a reported deep infection rate of 1.5% to 10%. Conversely, after closed reduction and nailing, most authors report a deep infection rate of less than 1%. This stark contrast is the primary justification for mastering closed nailing techniques, which preserve the fracture hematoma and the periosteal blood supply.
In our institutional experience encompassing more than 2,500 femoral nailings, infection occurs after the closed nailing of closed fractures in approximately 0.5% of patients. Of the femoral fractures treated, 25% are open injuries; in this high-risk cohort, infection occurs after closed nailing in 2% to 3% of patients.
Principles of Surgical Management
If a deep infection occurs after intramedullary nailing, the involved site—usually the fracture site—must be surgically opened and widely drained. The management algorithm is dictated by two primary factors: the stability of the intramedullary implant and the union status of the fracture.
1. Stable Hardware in an Ununited Fracture
If the intramedullary nail is providing rigid, stable fixation, it should generally be left in place. Removing a stable nail in the presence of an ununited fracture almost universally results in an infected nonunion, which is exceedingly difficult to manage.
* Surgical Debridement: Perform a radical debridement. All devitalized tissue, small avascular bone fragments, infected granulation tissue, and hematoma must be excised. Depending on the virulence of the organism (e.g., MRSA, Pseudomonas), the surgical site may require multiple sequential debridements.
* Biofilm and Callus: The infection usually remains localized to the fracture site. Although drainage may continue indefinitely and a medullary sequestrum may form, involucrum and callus will still form despite the infection, provided the fixation remains rigid.
* Definitive Removal: The nail should not be removed until the bony healing is strong enough to support the femur independently. Once union is achieved, a sequestrectomy is performed, the nail is extracted, and the medullary canal undergoes aggressive reaming, debridement, and irrigation.
2. Unstable or Broken Hardware in an Infected Fracture
If the fracture is infected and the nail is broken, loose, or providing inadequate stability, it acts merely as a nidus for infection and must be removed.
* Hardware Exchange: At the time of the open drainage and debridement procedure, the unstable nail is extracted.
* Stabilization: The fracture fragments must be immobilized to promote soft tissue healing and infection clearance. This can be achieved by inserting a larger-diameter intramedullary nail (if the canal allows for aggressive reaming to clear infected endosteum) or by applying a rigid external fixator.
* Antibiotic Cement Nails (ACN): For infections that are highly virulent or difficult to control, early deep hardware removal followed by the temporary insertion of an antibiotic-impregnated polymethyl methacrylate (PMMA) cement nail is highly effective. This provides local delivery of high-dose antibiotics while maintaining dead-space management and partial mechanical stability.
Postoperative Antibiotic Protocol
Surgical debridement must be paired with targeted antimicrobial therapy. Intraoperative cultures (minimum of 3 to 5 distinct tissue samples) should be obtained before the administration of perioperative antibiotics.
* Intravenous Therapy: Patients typically receive organism-specific intravenous antibiotics for 6 weeks following the definitive debridement surgery.
* Suppressive Therapy: If the hardware is retained to allow for fracture union, the patient is transitioned to an oral suppressive antibiotic regimen. This is often maintained until radiographic union is achieved and the hardware can be safely removed.
* Monitoring: The patient’s clinical progress and response to therapy are monitored via serial physical examinations and inflammatory markers, specifically the erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP).
INTRAMEDULLARY FIXATION IN PATHOLOGICAL FRACTURES
Pathological fractures present a unique biomechanical and biological challenge. The host bone is often severely compromised by osteolysis, osteoporosis, or altered bone remodeling, making standard plate-and-screw constructs prone to catastrophic failure. Intramedullary nailing offers a load-sharing biomechanical advantage that is ideal for these scenarios.
Metastatic Bone Disease
For pathological fractures resulting from metastatic tumors (e.g., breast, prostate, lung, renal, thyroid carcinoma), intramedullary fixation is usually rigid enough to allow the patient to mobilize in relative comfort for their remaining months of life.
- Prophylactic Nailing: If a metastatic deposit is discovered before a fracture occurs, closed prophylactic intramedullary nailing is highly justified if a pathological fracture is deemed impending (often evaluated using Mirels' criteria). Prophylactic stabilization significantly reduces morbidity, blood loss, and hospital length of stay compared to treating a completed fracture.
- Adjuvant PMMA: If a fracture occurs through a massive metastatic tumor with significant cortical destruction, a standard intramedullary nail may lack rotational or axial stability. In these cases, supplementing the intramedullary nail with methyl methacrylate (PMMA) bone cement affords excellent immediate fixation. The cement fills the lytic defect, interdigitates with the remaining host bone, and supports the nail. With rigid fixation, bony union may even occur, depending on the patient's life expectancy and tumor biology.
- Tumor Seeding: The theoretical disadvantage that the passage of an intramedullary nail through the tumor bed may dislodge tumor cells and accelerate systemic metastatic spread has been widely debated. However, extensive clinical evidence demonstrates that this theoretical risk does not justify the condemnation of the method. The immediate improvement in the patient's quality of life and pain control far outweighs the risk of endosteal seeding.
- Radiation Therapy: Because the host bone is often severely osteoporotic, fixation is inherently more secure with a load-sharing intramedullary nail than with load-bearing plates and screws. Furthermore, local adjuvant radiation therapy can be administered postoperatively to the nailed femur without ill effect on the hardware or the stability of the construct.
Paget Disease of Bone
Paget disease (osteitis deformans) is characterized by excessive, disorganized bone remodeling, resulting in enlarged, highly vascular, and mechanically weakened bone. The femur is frequently affected, typically presenting with a pronounced anterolateral bow.
Grundy’s historical review of 63 femoral fractures in patients with Paget disease noted that the most common site of fracture was the subtrochanteric area, followed by the upper femoral shaft.
🔪 Surgical Pitfall: The Bowed Femur
Attempting to pass a standard, straight, long intramedullary nail down a severely bowed Pagetic femur is a recipe for disaster. The mismatch between the nail's radius of curvature and the bone's deformity will inevitably cause the nail to become incarcerated, or it will cut out through the anterior cortex, creating an iatrogenic fracture.
Historically, Grundy recommended treating shaft fractures with traction followed by cast immobilization. However, in modern orthopedic practice, prolonged immobilization is poorly tolerated and carries high risks of pulmonary and thromboembolic complications.
For subtrochanteric fractures in Pagetic bone, the use of a short intramedullary nail (e.g., a cephalomedullary reconstruction nail) is highly recommended. The short nail provides robust proximal fixation, bypasses the severe diaphyseal bowing, allows the fracture to heal, and effectively prevents the progressive varus deformity that commonly plagues these patients.
Case Study: Hardware Failure in Paget Disease
The biomechanical superiority of intramedullary nailing over plating in abnormal bone is perfectly illustrated in cases of hardware failure. Plates applied to the tension side of a bowed Pagetic femur are subjected to massive bending moments, frequently leading to plate fracture or peri-implant bone failure.
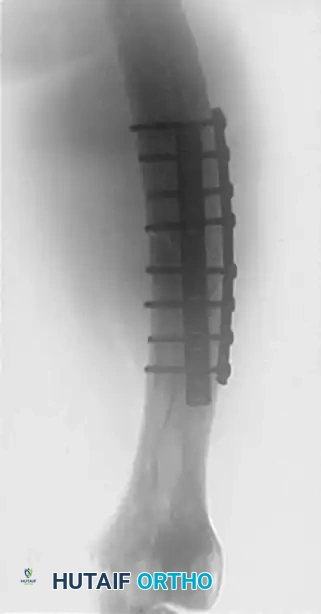
FIGURE 54-92 A: Anteroposterior (AP) radiograph demonstrating a femoral fracture in a patient with Paget disease, initially managed with double-plate fixation. Note the thickened cortices and altered trabecular pattern typical of Paget disease.

FIGURE 54-92 B: Lateral radiograph of the same double-plate construct. The rigid plates create a massive stress riser at their distal extent in the mechanically compromised, bowed bone.

FIGURE 54-92 C: AP radiograph revealing a catastrophic peri-implant fracture that occurred just below the distal extent of the plates. The plates were subsequently removed.
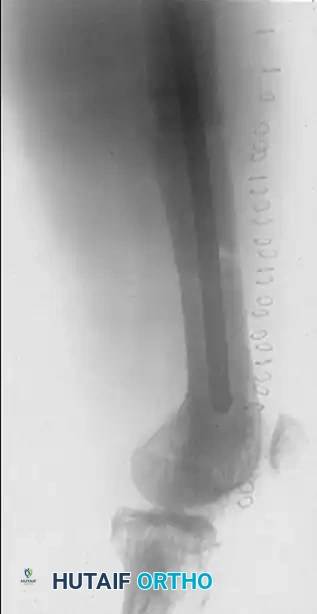
FIGURE 54-92 D: Lateral radiograph demonstrating the successful revision surgery. The femur was stabilized with a load-sharing intramedullary nail, which spans the entire length of the bone, neutralizes bending forces, and accommodates the altered biomechanics of the Pagetic femur far better than extramedullary plating.
