INTRODUCTION TO COMPLEX UPPER EXTREMITY RECONSTRUCTION
The management of severe congenital anomalies and complex acquired deformities of the upper extremity requires a profound understanding of biomechanics, neurovascular anatomy, and longitudinal growth patterns. This masterclass provides an exhaustive, evidence-based review of two distinct but highly specialized topics in operative orthopedics: the excision of the proximal ulna and the surgical management of macrodactyly (digital overgrowth).
While excision of the proximal ulna is typically reserved as a salvage procedure or a component of complex reconstructive efforts for synostosis or severe trauma, macrodactyly presents a unique pediatric challenge requiring staged, meticulous soft-tissue and osseous interventions. Both conditions demand rigorous preoperative planning, precise surgical execution, and structured postoperative rehabilitation to optimize functional outcomes.
EXCISION OF THE PROXIMAL ULNA
Excision of the proximal ulna is a formidable procedure. It is rarely performed in isolation but is rather utilized as a critical step in managing severe proximal radioulnar synostosis, chronic recalcitrant osteomyelitis, aggressive benign or malignant neoplasms, or as a salvage procedure following catastrophic, un-reconstructible comminuted fractures of the proximal ulna. The primary surgical objective is to restore a functional arc of motion (flexion and extension) while meticulously preserving the collateral ligamentous complex to prevent gross elbow instability.
Anatomic and Biomechanical Considerations
The proximal ulna forms the primary hinge of the elbow joint via the greater sigmoid notch articulating with the humeral trochlea. Resection of this critical osseous structure inherently destabilizes the ulnohumeral joint.
To mitigate this, the surgeon must understand the isometric properties of the medial ulnar collateral ligament (MUCL) and the lateral ulnar collateral ligament (LUCL). The preservation of a robust periosteal sleeve and the ligamentous insertions is non-negotiable. Failure to reconstruct these soft-tissue constraints will result in a flail elbow, rendering the extremity functionally useless despite achieving an improved arc of motion.
Indications and Preoperative Planning
- Congenital Proximal Radioulnar Synostosis: In cases where derotational osteotomies are insufficient, and mobilization of the joint is attempted.
- Post-Traumatic Ankylosis: Severe heterotopic ossification or intra-articular comminution where total elbow arthroplasty (TEA) is contraindicated (e.g., young, high-demand laborers).
- Neoplastic Resection: En bloc resection of tumors involving the olecranon or proximal ulnar diaphysis.
- Infection: Chronic osteomyelitis requiring radical debridement.
Preoperative imaging must include orthogonal radiographs of the elbow and forearm. Advanced imaging, such as a CT scan with 3D reconstruction, is highly recommended to template the exact length of the resection and identify the precise location of the radioulnar articulation.
🔪 Surgical Warning: Ulnar Nerve Management
The ulnar nerve is at extreme risk during proximal ulnar resections. It must be identified early, neurolysed, and protected throughout the procedure. In cases of extensive resection or altered anatomy, an anterior subcutaneous or submuscular transposition of the ulnar nerve should be performed to prevent postoperative traction neuritis or direct compression.
Surgical Technique: Step-by-Step
1. Positioning and Preparation
- Place the patient in the supine position with the affected arm draped free across the chest or positioned on a radiolucent hand table.
- Apply a sterile pneumatic tourniquet high on the brachium. Exsanguinate the limb and inflate the tourniquet to standard upper extremity pressures (typically 250 mm Hg or 100 mm Hg above systolic pressure) to ensure a bloodless surgical field.
2. Surgical Approach
- Make a longitudinal, slightly curved incision over the posterior aspect of the elbow, centered over the proximal preaxial ulnar bone. The incision should bypass the tip of the olecranon radially to avoid placing the scar directly over a pressure point.
- Carry the dissection through the subcutaneous tissue, maintaining thick skin flaps to preserve the subdermal vascular plexus.
3. Extraperiosteal Exposure and Ligament Preservation
- Identify the ulnar nerve in the cubital tunnel. Perform a meticulous neurolysis and retract it safely using a vessel loop.
- Expose the proximal ulna extraperiosteally. This is a critical departure from standard fracture exposures. You must preserve a thick, continuous periosteal and ligamentous strip, particularly on the medial and lateral borders.
- Carefully elevate the triceps insertion if the olecranon is to be resected, preserving its continuity with the anconeus and the forearm fascia.
- The preserved periosteal sleeve will serve as the foundation for reconstructing the collateral ligaments and the triceps mechanism, which is vital for postoperative stability.
4. Osseous Resection
- Determine the extent of the resection based on preoperative templating and intraoperative assessment of motion.
- Excise a sufficient amount of the ulna—usually approximately 1 inch (2.5 cm) of bone—along with its intimately attached, diseased, or ankylosed periosteum.
- Use an oscillating saw under continuous saline irrigation to prevent thermal necrosis of the remaining bone stump.
- Ensure the resection allows for adequate, unimpeded extension and flexion of the elbow joint.
5. Reconstruction and Stability Assessment
- Reconstruct the collateral ligament complex by suturing the preserved medial and lateral periosteal/ligamentous strips to the remaining ulnar stump or the surrounding robust fascial tissues. Use heavy, non-absorbable sutures (e.g., #2 FiberWire) placed through drill holes in the bone.
- If the triceps was detached, advance and repair it securely to the remaining proximal ulna or the reconstructed fascial sleeve.
- Release the tourniquet, achieve meticulous hemostasis, and assess the stability of the elbow through a full range of motion. The joint should demonstrate a smooth arc without subluxation.
6. Closure
- Place a closed suction drain if dead space is significant.
- Close the deep fascial layers, subcutaneous tissue, and skin in a layered fashion.
- Apply a well-padded, long-arm cast or a rigid posterior splint with the elbow immobilized in exactly 90 degrees of flexion and the forearm in neutral rotation.
Postoperative Care and Rehabilitation Protocol
The postoperative protocol must balance the need for soft-tissue healing with the prevention of secondary stiffness.
- Immobilization Phase (Weeks 0 to 3-6): The long-arm cast is worn for 3 to 6 weeks. The exact duration is dictated by the intraoperative assessment of elbow stability and the quality of the ligamentous reconstruction.
- Monitoring: The neurovascular status must be carefully and frequently monitored in the immediate postoperative period, given the extensive dissection and proximity to the ulnar nerve.
- Mobilization Phase (Post-Cast Removal): Once the cast is removed, initiate active-assisted flexion and extension exercises under the guidance of a specialized hand/upper extremity therapist. Passive stretching is strictly avoided initially to prevent heterotopic ossification and attenuation of the reconstructed ligaments.
- Splinting: A custom-molded thermoplastic night splint is highly recommended to hold the elbow in 90 degrees of flexion. This splint is utilized until the child (or adult patient) can actively flex the elbow against gravity and mild resistance.
- Strengthening: As healing progresses, emphasis should be placed on progressive resistance exercises targeting the elbow flexors (biceps, brachialis) and extensors (triceps) to maintain the functional arc of motion achieved during surgery and to provide dynamic stability to the joint.
OVERGROWTH (MACRODACTYLY)
Macrodactyly is a profoundly complex and rare congenital anomaly, representing approximately 0.9% of all congenital hand differences. It is characterized by a disproportionate, hamartomatous enlargement of the fibrofatty tissues, nerves, and osseous structures of a digit or multiple digits.
The index finger is involved most frequently, followed by the middle finger and the thumb. The condition is notoriously difficult to treat, as the overgrowth affects all tissue layers—skin, subcutaneous fat, nerves, vessels, tendons, and bone—making simple debulking procedures inadequate.
Etiology and Pathophysiology
Macrodactyly does not follow a traditional Mendelian inheritance pattern and is generally considered a sporadic mutation. While the exact etiology was historically debated, modern molecular genetics has identified somatic gain-of-function mutations in the PIK3CA gene as a primary driver for many overgrowth syndromes, including isolated macrodactyly.
Historically, three possible factors were strongly suspected and remain relevant to the phenotypic expression:
1. Abnormal Nerve Supply: There is a well-documented association with fibrolipomatous hamartoma (FLH) of the median nerve. The nerve territory dictates the overgrowth, explaining why the radial-sided digits (median nerve distribution) are most commonly affected.
2. Abnormal Blood Supply: Hypervascularity and altered hemodynamics during embryogenesis.
3. Abnormal Humoral Mechanism: Localized dysregulation of growth factors.
💡 Clinical Pearl: Syndromic Associations
Some authors have historically postulated that macrodactyly is an aborted or localized type of neurofibromatosis type 1 (NF1). However, other systemic manifestations of NF1 (café-au-lait spots, Lisch nodules) are usually not seen in isolated macrodactyly patients. It is crucial, however, to differentiate isolated macrodactyly from syndromic overgrowth such as Proteus syndrome, Klippel-Trenaunay syndrome, or CLOVES syndrome.
Clinical Presentation and Classification
Macrodactyly most commonly exists as an isolated condition, but syndactyly is associated with macrodactyly in about 10% of cases. The enlargement is typically unilateral and asymmetric.
Barsky’s classification remains the gold standard for categorizing true macrodactyly into two distinct clinical types, which dictate the prognosis and surgical timing:
- Type I: Static Enlargement: The enlarged digit is present at birth and grows proportionally with the child. While the digit is larger than its neighbors, the ratio of size difference remains constant throughout skeletal maturation.
- Type II: Progressive Enlargement: This is the more aggressive and problematic variant. The digit may not appear significantly enlarged during infancy but begins to grow rapidly and disproportionately during early childhood. This form is frequently associated with severe angular deformities (clinodactyly), joint stiffness, and progressive loss of function.
Clinical Imaging and Assessment
Below are classic clinical presentations of progressive macrodactyly involving the index finger and thumb, demonstrating the massive fibrofatty infiltration and angular deviation typical of the condition.
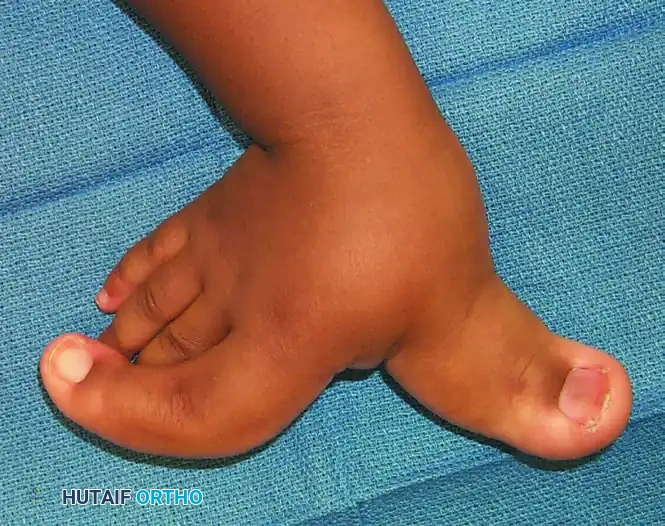
FIGURE 79-58 A: Dorsal view of macrodactyly affecting the index finger and thumb. Note the gross distortion of the nail fold, the massive expansion of the soft tissue envelope, and the secondary angular deformity of the index finger.
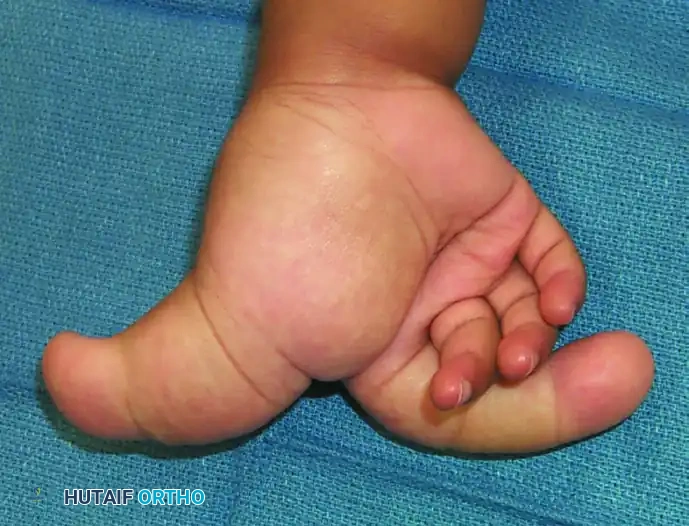
FIGURE 79-58 B: Volar view of the same patient. The volar skin is thickened, and the normal palmar creases are obliterated by the underlying fibrolipomatous hamartoma of the digital nerves. The sheer bulk of the digits severely limits flexion and opposition.
Surgical Management Strategies
The surgical management of macrodactyly is fraught with complications, including skin necrosis, nerve injury, joint stiffness, and recurrence of overgrowth. Parents must be counseled extensively that a "normal" digit is an impossible goal; the objective is to achieve a functional, sensate, and aesthetically acceptable digit.
Treatment is almost always staged and tailored to whether the condition is static or progressive.
1. Soft Tissue Debulking
Debulking is the cornerstone of early management but must be performed in stages to prevent vascular compromise to the digit.
* Technique: A mid-axial incision is utilized. The hypertrophic fibrofatty tissue is meticulously excised. The digital nerves are often found to be massively enlarged (macrodystrophia lipomatosa) and tortuous.
* Staging: Only one side of the digit (radial or ulnar) is debulked at a time. The contralateral side is addressed no sooner than 3 to 6 months later to ensure adequate collateral revascularization.
2. Epiphysiodesis
For progressive macrodactyly, arresting the longitudinal growth of the bone is critical.
* Timing: This is typically performed when the enlarged digit reaches the estimated adult length of the parent's corresponding digit.
* Technique: The physes of the distal and middle phalanges are surgically destroyed using a curette or drill under fluoroscopic guidance. If angular deformity is present, a corrective closing-wedge osteotomy can be performed concurrently.
3. Phalangeal Shortening Osteotomies
If the digit has already surpassed acceptable length, shortening osteotomies are required.
* Technique: A step-cut or diaphyseal resection of the proximal or middle phalanx is performed. Rigid internal fixation with K-wires or interosseous wires is necessary. This is often combined with aggressive soft tissue debulking.
4. Terminal Syme Amputation or Ray Resection
In severe, progressive cases where the digit is grotesquely enlarged, stiff, insensate, and mechanically obstructs the function of the adjacent normal digits, salvage procedures are indicated.
* Indications: Recalcitrant Type II progressive macrodactyly, severe joint ankylosis, or when multiple debulking procedures have failed.
* Technique: A ray amputation of the index or middle finger can dramatically improve the overall function and appearance of the hand. The adjacent metacarpals can be transposed to close the cleft, resulting in a highly functional, albeit three-fingered, hand.
Postoperative Care for Macrodactyly
Following any intervention for macrodactyly, strict elevation and immobilization are required to manage edema, which can be profound due to the abnormal lymphatic and venous drainage of the hamartomatous tissue. Prolonged occupational therapy is mandatory to maintain range of motion, manage scar tissue, and integrate the reconstructed digit into the child's global hand function.
