Comprehensive Introduction and Patho-Epidemiology
The surgical management of the forefoot and midfoot requires a profound, multidimensional understanding of intricate biomechanical relationships, soft-tissue balancing, and osseous architecture. Deformities in this anatomical region rarely exist in isolation; they are typically the culmination of progressive, interconnected failures of both static and dynamic stabilizing structures. A flexion deformity of the proximal interphalangeal joint (PIPJ), commonly known as a hammertoe, is frequently associated with first ray pathology, such as hallux valgus or hallux rigidus, as well as underlying midfoot instability. The epidemiology of these conditions reveals a high prevalence, particularly in the aging population and in females, largely driven by a combination of genetic predisposition, inflammatory arthropathies, and the biomechanical constraints of modern, restrictive footwear.
Hammertoe deformities are characterized by an extension contracture at the metatarsophalangeal (MTP) joint and a flexion contracture at the PIPJ, often accompanied by a hyperextension or neutral position at the distal interphalangeal joint (DIPJ). The pathophysiology is rooted in an imbalance between the intrinsic musculature (lumbricals and interossei) and the extrinsic musculature (extensor digitorum longus and flexor digitorum longus). As the MTP joint hyperextends—often due to plantar plate attenuation or rupture—the intrinsic muscles lose their mechanical advantage, leading to an unopposed pull of the extrinsic flexors at the PIPJ. This dynamic imbalance eventually transitions into a rigid, fixed deformity as the joint capsule and collateral ligaments undergo fibrotic contracture.
Concurrently, pathology of the first ray, such as advanced hallux valgus, often exacerbates lesser toe deformities. As the hallux drifts laterally, it physically displaces the second digit, leading to crossover toe deformities and further destabilization of the lesser MTP joints. In severe cases, the lateral subluxation of the sesamoid apparatus renders the first ray biomechanically incompetent, transferring immense pressure to the central metatarsal heads (transfer metatarsalgia). Addressing these deformities requires a holistic approach; correcting a hammertoe without addressing the incompetent first ray or a destabilized midfoot will inevitably lead to recurrent deformity and surgical failure.
Furthermore, the midfoot serves as the critical mechanical transition zone between the mobile, adaptive forefoot and the rigid, load-bearing hindfoot. Instability of the tarsometatarsal (Lisfranc) joint complex can result from high-energy axial loading trauma, subtle low-energy athletic injuries, progressive primary osteoarthritis, or inflammatory and neuropathic arthropathies (such as Charcot neuroarthropathy). Regardless of the etiology, failure of the midfoot architecture leads to progressive collapse of the medial longitudinal arch, debilitating pain due to altered joint kinematics, and the formation of dorsal and plantar bony prominences that render standard shoe wear nearly impossible. This comprehensive academic guide delineates the evidence-based surgical techniques for correcting PIPJ flexion deformities, performing a safe fibular sesamoidectomy, executing first MTP joint arthrodesis, and understanding the complex stabilizing mechanisms of the midfoot and Lisfranc articulation.
Detailed Surgical Anatomy and Biomechanics
The anatomical complexity of the forefoot and midfoot demands meticulous surgical precision. The lesser toe PIPJ is a hinge joint stabilized by a complex capsuloligamentous network. The primary static stabilizers include the collateral ligaments, which originate from the condylar recesses of the proximal phalanx and insert onto the base of the middle phalanx, and the plantar plate, a robust fibrocartilaginous structure that resists hyperextension. Dynamically, the extensor hood mechanism, comprising the central slip inserting on the middle phalanx and the terminal tendon inserting on the distal phalanx, orchestrates extension. In the setting of a rigid hammertoe, the plantar plate and collateral ligaments become severely contracted, tethering the joint in a flexed posture. The extensor digitorum longus (EDL) loses its mechanical advantage at the PIPJ, while the flexor digitorum longus (FDL) exerts an unopposed deforming force, necessitating both osseous resection and soft-tissue release for adequate correction.
Moving proximally, the first ray is a biomechanical powerhouse, heavily reliant on the sesamoid apparatus for efficient function. The fibular (lateral) and tibial (medial) sesamoids are embedded within the respective tendons of the flexor hallucis brevis (FHB). These sesamoids articulate with the plantar aspect of the first metatarsal head, separated by the crista, acting as a fulcrum to increase the mechanical advantage of the FHB and protecting the flexor hallucis longus (FHL) tendon that glides between them. The fibular sesamoid is intimately associated with the adductor hallucis tendon and the deep transverse metatarsal ligament. Crucially, the neurovascular bundle supplying the first web space courses in dangerously close proximity to the proximal-lateral border of the fibular sesamoid. Iatrogenic injury to this bundle during sesamoidectomy can result in devastating neuromas and sensory deficits.
Biomechanically and anatomically, the midfoot is divided into three distinct functional columns. The medial column comprises the first metatarsal and the medial cuneiform, possessing a small degree of sagittal plane mobility essential for accommodating uneven terrain and facilitating the windlass mechanism. The middle column, comprising the second and third metatarsals articulating with the middle and lateral cuneiforms, is the most rigid column, acting as the central stabilizing strut of the foot. The lateral column, comprising the fourth and fifth metatarsals articulating with the cuboid, is highly mobile, allowing for triplanar accommodation during the contact phase of gait.
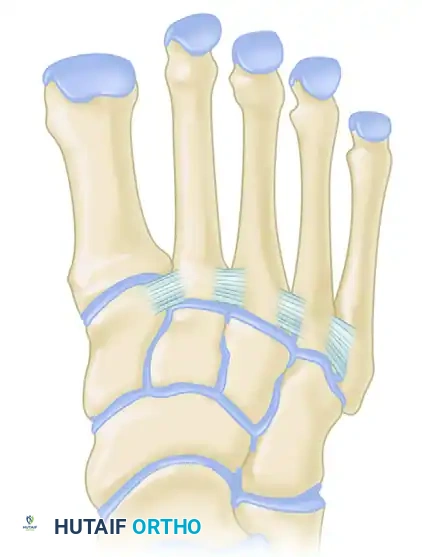
The inherent stability of the midfoot is derived from its unique coronal plane architecture. The cuneiforms are wedge-shaped, being significantly wider dorsally than plantarly. When articulated, they form a structural "Roman arch." Furthermore, the base of the second metatarsal is recessed proximally between the medial and lateral cuneiforms, locking it into place like the keystone of an arch. This osseous mortise severely limits translation in the transverse and coronal planes.
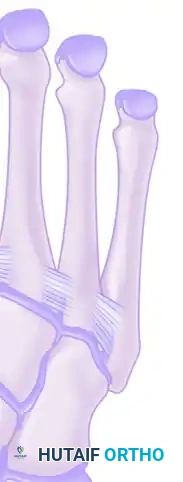

While the bony architecture provides static stability, the ligamentous network is the primary restraint against dynamic deforming forces. Crucially, there is no intermetatarsal ligament connecting the base of the first metatarsal to the base of the second metatarsal. Instead, the critical stabilizing structure is the Lisfranc ligament, a robust plantar intra-articular ligament that originates on the lateral aspect of the medial cuneiform and inserts onto the medial aspect of the second metatarsal base. Disruption of this ligament uncouples the medial and middle columns, leading to rapid diastasis, arch collapse, and severe degenerative joint disease.
Exhaustive Indications and Contraindications
The decision to proceed with operative intervention in the forefoot and midfoot must be predicated on a thorough evaluation of the patient's symptoms, functional limitations, and the failure of exhaustive conservative management. Indications for PIPJ resection arthroplasty or arthrodesis include rigid hammertoe deformities that cause intractable dorsal PIPJ ulcerations, severe pain with standard footwear, and failure of accommodating measures such as extra-depth shoes, crest pads, and digital taping. Flexible deformities may be managed with soft-tissue procedures alone (e.g., flexor-to-extensor transfer), but once the deformity becomes fixed, osseous resection is absolutely mandatory to decompress the joint and restore linear alignment.
Fibular sesamoidectomy is indicated in the presence of severe, localized fibular sesamoiditis that has failed conservative care, osteonecrosis of the sesamoid, intractable plantar keratosis directly beneath the fibular sesamoid, or as an adjunctive procedure during the correction of severe hallux valgus where the sesamoid apparatus is irreducible. First MTP joint arthrodesis remains the gold standard for end-stage hallux rigidus, severe rheumatoid forefoot deformities, and salvage of failed prior first ray surgeries (such as failed Keller arthroplasties or recurrent hallux valgus). Lisfranc stabilization (either via open reduction internal fixation or primary arthrodesis) is indicated for any acute midfoot injury demonstrating instability on weight-bearing radiographs, or for chronic midfoot collapse resulting in debilitating midfoot arthrosis.
Contraindications must be rigorously respected to avoid catastrophic postoperative complications. Absolute contraindications include active local or systemic infection, severe peripheral arterial disease (PAD) precluding incisional healing, and medically unstable patients unable to tolerate anesthesia. Relative contraindications include poorly controlled diabetes mellitus (HbA1c > 8.0%), severe peripheral neuropathy (which increases the risk of Charcot neuroarthropathy and hardware failure), active smoking (due to significantly elevated rates of nonunion and wound dehiscence), and patient non-compliance with strict postoperative weight-bearing restrictions.
| Procedure | Primary Indications | Absolute Contraindications | Relative Contraindications |
|---|---|---|---|
| PIPJ Resection Arthroplasty | Rigid hammertoe, dorsal ulceration, failed conservative care | Active infection, severe ischemia (ABI < 0.5) | Flexible deformity (consider soft tissue transfer), heavy smoking |
| Fibular Sesamoidectomy | Osteonecrosis, intractable keratosis, irreducible severe hallux valgus | Asymptomatic subluxation, medial sesamoid absence (risk of hallux varus) | High-demand athletic jumping sports (alters biomechanics) |
| First MTP Arthrodesis | End-stage hallux rigidus, severe rheumatoid foot, salvage of failed bunionectomy | Active joint infection, critical limb ischemia | Severe IP joint arthrosis, patient refusal of stiff joint |
| Lisfranc Stabilization | Diastasis >2mm on WB films, unstable acute injury, chronic midfoot collapse | Active infection, non-ambulatory patient | Severe uncontrolled diabetes, active Charcot active phase |
Pre-Operative Planning, Templating, and Patient Positioning
Thorough preoperative planning is the cornerstone of successful forefoot and midfoot reconstruction. Clinical evaluation must begin with a comprehensive neurovascular assessment. Palpation of the dorsalis pedis and posterior tibial pulses is mandatory; if pulses are diminished, non-invasive vascular studies, including Ankle-Brachial Indices (ABI) and Toe Pressures, must be obtained. An ABI of less than 0.5 or a toe pressure of less than 40 mmHg represents a significant risk for wound necrosis and requires vascular surgery consultation prior to any elective orthopedic intervention. The clinical exam must also assess the flexibility of the deformities. The Kelikian push-up test is utilized to determine the reducibility of MTP joint hyperextension, dictating whether a metatarsal shortening osteotomy (Weil osteotomy) is required in conjunction with PIPJ correction.
Radiographic evaluation strictly requires weight-bearing imaging. Standard views include the weight-bearing anteroposterior (AP), lateral, and oblique views of the foot. For sesamoid pathology, a specialized sesamoid axial view is critical to evaluate the crista and the degree of sesamoid subluxation. When assessing midfoot instability, the weight-bearing AP view must be scrutinized for the alignment of the medial border of the second metatarsal with the medial border of the middle cuneiform. A diastasis of greater than 2 mm between the first and second metatarsal bases, or the presence of the "fleck sign" (an avulsion fracture off the base of the second metatarsal), is pathognomonic for a Lisfranc injury. In cases of subtle midfoot instability or chronic arthrosis, Computed Tomography (CT) provides unparalleled osseous detail for preoperative templating, while Magnetic Resonance Imaging (MRI) is highly sensitive for purely ligamentous Lisfranc disruptions.
Preoperative templating is particularly critical for first MTP joint arthrodesis and midfoot fusions. For the first MTP joint, the surgeon must template the desired position of arthrodesis: typically 10 to 15 degrees of valgus to match the physiological cascade of the lesser toes, and 15 to 20 degrees of dorsiflexion relative to the first metatarsal axis to allow for a normal rollover during the terminal stance phase of gait. Hardware selection, including the size of the headless compression screw and the contour of the dorsal neutralization plate, should be anticipated.
Patient positioning for these procedures is almost universally supine. A well-padded bump is placed under the ipsilateral hip to internally rotate the leg, bringing the foot into a neutral, plantigrade position that is easily accessible to the surgeon. A pneumatic thigh or calf tourniquet is applied over copious padding. While an ankle block or popliteal block provides excellent regional anesthesia and postoperative pain control, a calf tourniquet is often preferred by surgeons to minimize the risk of ischemic complications associated with prolonged thigh tourniquet times, though it must be kept out of the surgical field to avoid compromising the sterile environment.
Step-by-Step Surgical Approach and Fixation Technique
PIPJ Resection Arthroplasty
The primary objective of this procedure is to decompress the contracted joint, realign the digit, and provide a stable, functional toe that clears the toe box of standard footwear. The procedure begins with a dorsal elliptical incision centered directly over the PIPJ. The ellipse should be oriented transversely or longitudinally depending on the redundancy of the dorsal skin. Excision of this skin wedge is critical; it removes the hyperkeratotic lesion (corn) and utilizes the subsequent skin closure to mechanically splint the toe in extension.
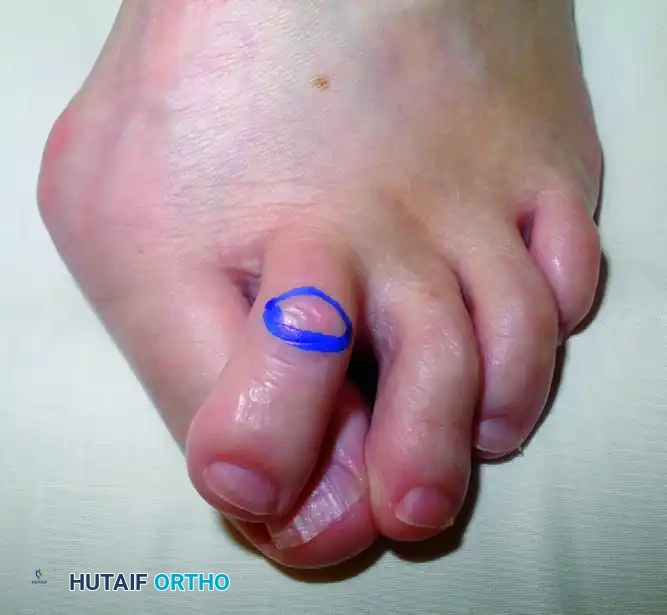
Deepen the incision through the subcutaneous tissue, taking extreme care to retract the dorsal cutaneous nerves. Perform a transverse tenotomy of the extensor tendon over the joint, or split it longitudinally to expose the PIPJ capsule. Perform a thorough collateral ligament release to allow the proximal phalanx head to be delivered into the wound. Using a microsaw or sharp bone-cutting forceps, excise the head and neck of the proximal phalanx. The resection must be perpendicular to the long axis of the phalanx. Ensure sufficient bone is removed to allow the toe to rest in a neutral position without tension. Inadequate bone resection is the leading cause of recurrent deformity and vascular compromise upon straightening the digit. If tension persists, resect an additional 1 to 2 mm of the proximal phalanx. Internal fixation is highly recommended for rigid deformities. Insert a 0.054-inch Kirschner wire (K-wire) in a retrograde fashion from the resected surface of the middle phalanx, through the distal phalanx, exiting the tip of the toe. Reduce the PIPJ and drive the K-wire proximally into the medullary canal of the proximal phalanx.
Fibular Sesamoidectomy
Through a dorsal first web space incision or a medial incision (if performing concurrent bunion surgery), identify the fibular sesamoid. Clasp the sesamoid firmly with a Kocher clamp and apply medial traction. Free the soft tissue surrounding the fibular sesamoid using blunt dissection. Proceed with sharp dissection to release the intersesamoidal ligament and the lateral head of the FHB. Extreme caution must be exercised at the proximal lateral border of the fibular sesamoid. The neurovascular bundle supplying the first web space is highly vulnerable in this region. Keep the scalpel blade directed strictly toward the bone of the sesamoid to avoid catastrophic nerve injury. Once excised, thoroughly inspect the FHL tendon to ensure it has not been inadvertently lacerated, and achieve meticulous hemostasis.
First MTP Joint Arthrodesis
Exposure is achieved via a dorsal longitudinal incision just medial to the extensor hallucis longus (EHL) tendon. The joint capsule is incised longitudinally, and full-thickness flaps are elevated. The articular cartilage is resected using a cup-and-cone reamer system, which allows for multiplanar adjustments of the arthrodesis position without compromising bony contact. The joint is provisionally fixated with K-wires in the templated position (10-15 degrees valgus, 15-20 degrees dorsiflexion). The gold standard construct is an obliquely placed headless compression screw crossing the arthrodesis site from distal-medial to proximal-lateral, augmented with a precontoured dorsal neutralization plate. This construct provides superior resistance to plantar gapping during the terminal stance phase of gait.
Midfoot and Lisfranc Stabilization
For Lisfranc injuries, a dorsal approach is utilized. A longitudinal incision is made centered over the first intermetatarsal space, lateral to the EHL tendon. The deep peroneal nerve and dorsalis pedis artery must be identified and protected. The interval between the first and second metatarsals is developed. The joints are debrided of all hematoma and interposed soft tissue. Anatomic reduction is paramount and must proceed in a specific sequence: the medial column is reduced first, followed by the middle column. Provisional fixation is achieved with rigid K-wires. Definitive fixation typically involves a "homerun screw" placed from the medial cuneiform into the base of the second metatarsal, replicating the trajectory of the native Lisfranc ligament. Dorsal bridge plating has gained significant popularity as it avoids iatrogenic articular cartilage damage caused by transarticular screws and provides robust stability.
Wound Closure and Hemostasis Protocols
Meticulous soft tissue handling and hemostasis are paramount. Close the joint capsules with 2-0 or 3-0 absorbable sutures to restore the soft tissue tension band. Close the dorsal skin with 3-0 or 4-0 monofilament nylon. Release the pneumatic tourniquet prior to final dressing application. Carefully inspect all wounds for pulsatile bleeding and cauterize vessels as needed. Diffuse, non-pulsatile bleeding is exceedingly common due to preoperative NSAID use. Placing the patient in the Trendelenburg position during wound closure decreases venous hydrostatic pressure and aids hemostasis. Apply a conforming, nonconstricting, bulky compression forefoot dressing to act as a soft-tissue splint.
Complications, Incidence Rates, and Salvage Management
Despite meticulous surgical technique, complications in forefoot and midfoot reconstruction are not uncommon and can significantly impact patient outcomes. The surgeon must be acutely aware of potential pitfalls and possess the armamentarium to execute salvage procedures when necessary. In lesser toe surgery, the most common complication is recurrent deformity or a "floating toe." A floating toe occurs when the toe fails to purchase the ground during the stance phase of gait, often resulting from over-resection of the proximal phalanx, failure to address a contracted dorsal capsule at the MTP joint, or iatrogenic disruption of the plantar plate. Salvage of a floating toe is notoriously difficult and may require a flexor-to-extensor tendon transfer (Girdlestone-Taylor procedure) or an MTP joint arthroplasty.
Vascular compromise is a devastating complication following profound deformity correction. Straightening a chronically flexed digit stretches the digital neurovascular bundles. If the toe appears blanched and pulseless after K-wire insertion, the wire must be removed immediately, and the toe placed in a slightly flexed position. If perfusion does not return, the surgeon must resect additional bone from the proximal phalanx to relieve tension on the digital arteries. Vasodilators and warm compresses may be utilized, but mechanical decompression via bone shortening is the definitive solution.
In midfoot and first ray arthrodesis procedures, nonunion and malunion are the primary concerns. Nonunion of the first MTP joint occurs in approximately 5-10% of cases and is heavily correlated with patient factors such as smoking, diabetes, and non-compliance with weight-bearing restrictions. Asymptomatic nonunions may be observed, but painful nonunions require revision arthrodesis with structural bone grafting (autograft or allograft) and robust revision hardware. Malunion, particularly excessive plantarflexion of the first MTP joint, leads to severe interphalangeal joint arthritis and dorsal shoe-wear irritation, necessitating a corrective closing wedge osteotomy.
| Complication | Estimated Incidence | Primary Etiology | Salvage Management Strategy |
|---|---|---|---|
| Floating Toe | 10 - 15% | Over-resection of bone, MTP hyperextension | Flexor-to-extensor transfer, Weil osteotomy |
| First MTP Nonunion | 5 - 10% | Smoking, inadequate fixation, early weight-bearing | Revision arthrodesis with structural bone graft |
| Digital Ischemia | < 2% | Excessive tension on NV bundle after straightening | Immediate K-wire removal, additional bone resection |
| Hardware Failure (Lisfranc) | 10 - 20% | Fatigue failure of transarticular screws | Hardware removal, transition to dorsal bridge plating or primary arthrodesis |
| Neuroma (1st Web Space) | 2 - 5% | Iatrogenic injury during fibular sesamoidectomy | Excision of neuroma, proximal nerve burying into muscle belly |
Phased Post-Operative Rehabilitation Protocols
The success of complex forefoot and midfoot reconstruction relies as heavily on strict adherence to postoperative rehabilitation protocols as it does on intraoperative execution. Rehabilitation must be carefully phased to respect the biological healing of soft tissues and osseous arthrodesis sites, while preventing the debilitating stiffness that accompanies prolonged immobilization. The protocols vary depending on the exact procedures performed, but a generalized framework for complex reconstructions involves four distinct phases.
Phase 1: Immediate Postoperative Phase (0-2 Weeks)
The primary goals during this phase are wound healing, edema control, and pain management. Strict elevation of the operative extremity above the level of the heart is mandatory for the first 72 hours to mitigate profound postoperative edema and prevent wound dehiscence. Ambulation is strictly limited to bathroom privileges using crutches or a walker, maintaining a non-weight-bearing (NWB) status on the operative extremity. The bulky surgical dressing applied in the operating room remains intact and undisturbed until the first postoperative clinic visit at 10 to 14 days, at which point sutures are removed.
Phase 2: Early Mobilization and Protection (2-6 Weeks)
Following suture removal, the management diverges based on the procedures performed. For isolated PIPJ arthroplasties, patients may transition to heel-weight-bearing in a rigid, flat-bottom postoperative shoe. If K-wires were utilized, they are meticulously protected. For first MTP arthrodesis and Lisfranc stabilization, patients are typically placed into a short-leg cast or a rigid controlled ankle motion (CAM) boot and must remain strictly non-weight-bearing for a minimum of 6 weeks to prevent hardware failure and allow for primary osseous union. Radiographs are obtained at the 4-to-6-week mark to assess for early callus formation and maintenance of alignment. K-wires from lesser toe procedures are generally removed in the clinic at 4 weeks.
Phase 3: Intermediate Phase (6-12 Weeks)
Assuming clinical and radiographic signs of healing are present at the 6-week mark, patients with midfoot and first ray fusions are permitted to begin progressive weight-bearing. The transition starts with partial weight-bearing in the CAM boot, advancing to full weight-bearing over a 2-to-3-week period. Physical therapy is initiated to focus on edema reduction, desensitization, and restoring range of motion to the un-fused joints (e.g., the ankle, subtalar, and lesser MTP joints). Strengthening of the extrinsic and intrinsic foot musculature is crucial to restore dynamic stability. Patients with lesser toe corrections transition to a deep, wide, jogging-type athletic shoe to accommodate residual swelling, which can persist for up to 6 months.
Phase 4: Long-Term Management (3+ Months)
Return to high-impact activities and unrestricted shoe wear is highly variable and depends on the patient's baseline function and the extent of the reconstruction. For long-term use, especially in patients with significant midfoot reconstruction or underlying systemic arthropathies, an extra-deep shoe with a soft, accommodating upper (such as deerskin) is highly recommended. Custom orthotics with a rigid Morton's extension may be utilized to protect a first MTP arthrodesis, while a medial longitudinal arch support is critical for patients following Lisfranc stabilization to prevent late-onset arch collapse. Patients must be counseled that maximal medical improvement and complete resolution of swelling may take up to a full year postoperatively.
Summary of Landmark Literature and Clinical Guidelines
The evolution of forefoot and midfoot reconstruction has been heavily guided by landmark biomechanical studies and long-term clinical outcome trials. In the realm of lesser toe deformities, the work by Coughlin et al. remains foundational. Their long-term follow-up studies on PIPJ resection arthroplasty demonstrated that while osseous union is not strictly necessary for a good clinical outcome (fibrous union is often well-tolerated), adequate decompression and restoration of the intrinsic-extrinsic muscle balance are paramount to prevent recurrence. Furthermore, Myerson's extensive biomechanical evaluations of the plantar plate have revolutionized our understanding of MTP joint instability, leading to the widespread adoption of direct plantar plate repair techniques in conjunction with PIPJ correction.
Regarding the first ray, the seminal papers by Coetzee and colleagues have established the current clinical guidelines for first MTP joint arthrodesis. Their comparative studies demonstrated that the use of a dorsal precontoured plate combined with an interfragmentary compression screw significantly increases construct rigidity and reduces the rate of nonunion compared to crossed K-wires or isolated screw fixation. This construct provides the necessary stability to resist the immense bending moments applied to the first ray during the terminal stance phase of gait. Additionally, the literature strongly supports a fusion position of slight valgus and dorsiflexion to optimize gait kinematics and patient satisfaction.
In the management of Lisfranc injuries, the paradigm has shifted significantly over the past two decades. Historically, transarticular screw fixation was the gold standard. However, landmark prospective randomized trials, notably by Ly and Coetzee, demonstrated that primary arthrodesis of the medial and middle columns in purely ligamentous Lisfranc injuries yields superior functional outcomes and lower reoperation rates compared to open reduction and internal fixation (ORIF). More recently, the advent of dorsal bridge plating has been supported by extensive biomechanical literature showing equivalent stability to transarticular screws while preserving the articular cartilage and mitigating the risk of late post-traumatic arthrosis. These evidence-based guidelines underscore the necessity for orthopedic surgeons to continually adapt their techniques to align with the highest quality of emerging clinical data.
