INTRODUCTION TO REVISION HALLUX VALGUS SURGERY
Recurrent hallux valgus following a primary basilar or distal metatarsal osteotomy is a formidable complication that demands a rigorous biomechanical and radiographic evaluation. The etiology of recurrence is often multifactorial, stemming from unrecognized preoperative deformity (such as an abnormal distal metatarsal articular angle [DMAA] or severe metatarsus adductus), inadequate surgical execution, failure to achieve soft tissue balance, or loss of fixation.
Revision forefoot surgery requires the orthopedic surgeon to navigate altered anatomy, compromised vascularity, and dense scar tissue. The primary objective is to restore a congruous first metatarsophalangeal (MTP) joint, re-establish the weight-bearing mechanics of the first ray, and alleviate pain. Depending on the patient's age, functional demands, and the presence of osteoarthritis, surgical options range from a correcting distal metatarsal osteotomy (biplanar chevron) to first MTP joint arthrodesis or resection arthroplasty.
RECURRENT DEFORMITY AFTER BASILAR METATARSAL OSTEOTOMY
Recurrent deformity following a basilar metatarsal osteotomy combined with a first web space dissection or lateral release indicates a failure to maintain the corrected intermetatarsal angle (IMA) or an underlying hypermobility of the first ray.
When addressing this specific recurrence, the surgeon has two primary joint-sparing options: performing a second basilar metatarsal osteotomy combined with aggressive medial capsular imbrication and a revision first web space dissection to release contracted lateral structures, or opting for a first MTP joint arthrodesis. In selected patients—particularly men with high functional demands or those with severe deformity—arthrodesis of the first MTP joint is often the most reliable and definitive procedure.
Indications for First MTP Joint Arthrodesis in Recurrence
Arthrodesis provides a stable, predictable outcome and eliminates the risk of further recurrence. It is highly recommended when the following clinical and radiographic parameters are present:
* Severe Intermetatarsal Angle: An IMA of 14 degrees or greater.
* Severe Hallux Valgus Angle: A hallux valgus angle (HVA) exceeding 30 degrees.
* Normal DMAA: A distal metatarsal articular angle within the normal range of 10 to 15 degrees, making a distal corrective osteotomy unnecessary.
* Forefoot Splaying: A globally splayed forefoot that cannot be adequately narrowed with osteotomies alone.
* Osteoarthritic Changes: Minimal-to-mild (or greater) osteoarthritic changes at the first MTP joint. If the articular cartilage is frankly damaged, joint-sparing procedures are contraindicated.
* Sesamoid Subluxation: Markedly subluxed or dislocated sesamoid bones that cannot be reduced through soft tissue balancing.
* Preserved Passive ROM: 50 to 60 degrees of passive range of motion of the first MTP joint (though this motion will be sacrificed, its presence indicates the deformity is primarily structural rather than ankylosed).
* Pathologic Arch Structures: Pes planovalgus or other arch structures that inherently increase valgus stress on the MTP joint, predisposing the patient to further recurrence if a joint-sparing procedure is attempted.
💡 Clinical Pearl: The Lapidus Procedure
For severe recurrent deformities, particularly those associated with first ray hypermobility or medial column instability, Lapidus recommended combining an arthrodesis of the first metatarsal-medial cuneiform joint (Lapidus procedure) with a distal soft tissue release. This addresses the apex of the deformity and provides powerful correction of the intermetatarsal angle.
RECURRENT VALGUS DEFORMITY WITH ABNORMAL DMAA
A frequent cause of recurrent hallux valgus is the failure to recognize and correct an increased Distal Metatarsal Articular Angle (DMAA) during the index procedure. The DMAA represents the relationship of the articular surface of the metatarsal head to the longitudinal axis of the metatarsal shaft.
When an increased DMAA is present, simply reducing the hallux via soft tissue balancing or a standard translational osteotomy will place the MTP joint incongruously on the metatarsal head. The proximal phalanx will rest in varus relative to the articular cartilage, leaving the lateral aspect of the first metatarsal head uncovered and leading to rapid joint degeneration and recurrent deformity.
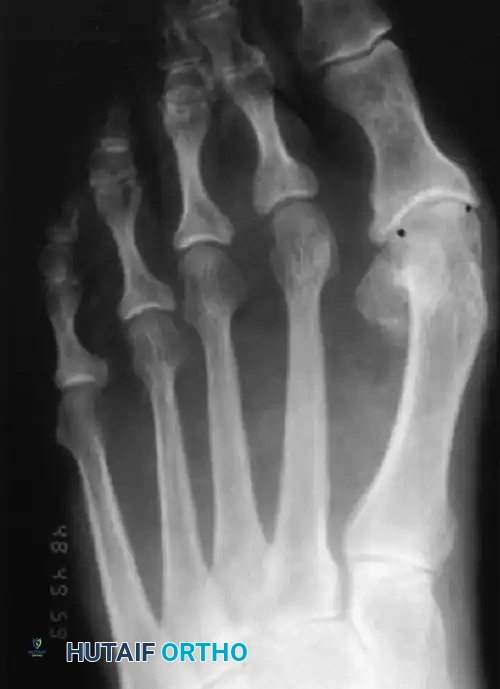
Figure 81-73: Anteroposterior weight-bearing radiograph in an elderly woman, 20 years after a McBride bunionectomy. In reality, this is a congruous hallux valgus that assumed its normal position on the first metatarsal head after a soft tissue realignment for hallux valgus. A biplanar correcting distal metatarsal osteotomy is needed to address the abnormal DMAA.
To correct this specific pathomechanics, the surgeon must perform a medial capsulorrhaphy, a distal metatarsal displacement osteotomy (biplanar chevron), and a first web space dissection with lateral soft tissue release.
The Risk of Osteonecrosis (AVN)
Historically, performing a distal metatarsal osteotomy concurrently with a lateral soft tissue release was thought to carry an unacceptably high risk of osteonecrosis (avascular necrosis) of the first metatarsal head. However, contemporary anatomical studies have shown that while the risk exists, the extent of necrosis and its clinical significance are often overstated. This complication is not to be feared as much as previously thought, provided the surgeon respects the vascular "safe zones" of the first metatarsal.
⚠️ Surgical Warning: Vascular Supply
The primary blood supply to the first metatarsal head enters via the plantar-lateral capsular network. A cadaveric study identified the plantar-lateral corner of the metatarsal neck as the major site of vascular ingress. To prevent osteonecrosis, the long plantar limb of a chevron osteotomy must exit well proximal to the capsular attachment, and lateral releases must be performed carefully to avoid stripping this critical vascular leash.
SURGICAL TECHNIQUE: CORRECTING DISTAL METATARSAL OSTEOTOMY
The following technique describes the biplanar chevron osteotomy utilized to correct a recurrent hallux valgus deformity associated with an abnormal DMAA.
🔪 Surgical Technique 81-26: Biplanar Chevron Osteotomy
Phase 1: Exposure and Soft Tissue Release
1. Incision and Capsulotomy: Utilize a standard medial longitudinal incision. Perform an inverted-L capsulotomy and carefully elevate the capsular flap to expose the medial eminence and the MTP joint.
2. First Web Space Dissection: The web space dissection, lateral release, partial adductor hallucis resection, and tendinous release must be performed before the osteotomy. Once the metatarsal head is displaced following the osteotomy, exposure to the lateral structures becomes markedly limited.
3. Vascular Preservation: Keep the lateral dissection strictly distal to the neck of the first metatarsal. Preserving the soft tissue attachments at the plantar-lateral metatarsal neck is paramount to maintaining perfusion to the capital fragment.
Phase 2: The Biplanar Osteotomy
1. Chevron Cut: Perform a standard chevron osteotomy. Ensure the apex is centered in the metatarsal head and the plantar limb exits proximal to the capsular reflections.
2. Correcting the DMAA: The primary goal is to reduce the valgus tilt of the articular surface to approximately 10 degrees, bringing the hallux into a congruous position. To achieve this, convert the standard chevron into a biplanar cut by removing a 1- to 2-mm wedge-shaped sliver of bone from the medial aspect of the distal metatarsal shaft (or from the capital fragment). This creates a "closing wedge osteotomy."
3. Impaction: The size of the medial wedge should be deliberately small. Slight bony impaction occurs medially as the cancellous surfaces are manually pressed together, which will further correct the angle.
Phase 3: Fixation and Closure
1. Internal Fixation: Secure the osteotomy using small absorbable pins, nonabsorbable Kirschner wires, or dedicated compression screws, depending on bone quality and surgeon preference.
2. Joint Reduction: Reduce the hallux congruously onto the newly aligned articular surface of the metatarsal head. Maintain this corrected position with a robust medial capsulorrhaphy.
3. Intraoperative Radiography: Evaluate the repair radiographically. Obtain an anteroposterior (AP) radiograph with the foot resting flat (flex the knee) on a radiolucent image board to simulate weight-bearing. While not always mandatory in primary cases, intraoperative imaging is strictly required when surgically treating a recurrence.
💡 Clinical Pearl: Combined Osteotomies
A combination of a chevron osteotomy and a proximal phalangeal (Akin) osteotomy can be used for greater correction of the valgus deformity. However, this combined procedure should be used with extreme caution if severe sesamoid subluxation or a very wide intermetatarsal angle is present, as it may mask underlying first ray instability.
MANAGEMENT IN ELDERLY PATIENTS WITH OSTEOARTHRITIS
In the elderly population, recurrent hallux valgus is frequently accompanied by degenerative joint disease, osteopenia, and lower functional demands. Joint-sparing osteotomies may be contraindicated due to poor bone healing potential or existing cartilage destruction.
Resection Arthroplasty (Keller Procedure)
Resection arthroplasty remains a viable salvage option for recurrent deformity in elderly, low-demand patients with osteoarthritis. The procedure involves resecting the base of the proximal phalanx to decompress the joint.
* Technique Modification: The usefulness of the Keller procedure is significantly expanded if the hallux is temporarily secured to the first metatarsal with two longitudinal Kirschner wires after the metatarsal is manually displaced laterally as far as possible.
* Sesamoid Management: Excision of the fibular sesamoid bone is highly recommended before the hallux is pinned to the first metatarsal to remove the deforming lateral force.
Replacement Arthroplasty vs. Arthrodesis
The results of silastic or metallic replacement arthroplasty for the first MTP joint in recurrent hallux valgus have been highly variable and are generally falling out of favor due to risks of implant subsidence, reactive synovitis, and failure.
While replacement arthroplasty has historically been recommended for rheumatoid arthritis patients with severe joint destruction, modern consensus favors arthrodesis. In most patients, a modified Keller resection or a formal first MTP joint arthrodesis provides superior, more predictable results with less expense and fewer long-term complications than joint replacement.
COMPLICATIONS AFTER CHEVRON OSTEOTOMY
Understanding the complications of the chevron osteotomy is critical for both primary execution and revision planning. Johnson described several key complications and outlined strategies for avoidance:
- Recurrent MTP Joint Valgus: Prevented by ensuring the medial capsular imbrication is structurally firm and by holding the hallux in the exact proper alignment before and during skin closure.
- Insufficient Narrowing of the Forefoot: Often associated with unrecognized preoperative metatarsus adductus, which leaves insufficient room between the first and second metatarsals to shift the capital fragment laterally. Careful preoperative radiographic templating is essential.
- Osteonecrosis (AVN): Prevented by meticulously preserving the lateral blood supply to the capital fragment. Two technical errors cause AVN: cutting the first dorsal metatarsal artery by overpenetrating the saw blade laterally, and incorrectly placing the proximal arms of the osteotomy inside the joint capsule.
- Joint Incongruity: Results from a failure to recognize a valgus posture of the articular surface (abnormal DMAA) prior to surgery, or from inadvertently closing the osteotomy medially, which places the capital fragment in a straight or varus position.
- Unfulfilled Patient Expectations: Minimized through exhaustive preoperative counseling regarding the realistic benefits, recovery timeline, and potential drawbacks of bunion surgery. A common surgical error is attempting to correct a severe deformity with a chevron osteotomy; it is strictly indicated for mild-to-moderate deformities.
Managing Malunion
Malunion after a chevron osteotomy is uncommon if three technical tenets are followed: (1) rigid internal fixation is achieved and manually tested intraoperatively; (2) the distal fragment is slightly plantarflexed (inferiorly displaced) relative to the proximal fragment to account for shortening; and (3) postoperative weight-bearing is strictly guarded.
Dorsal Malunion:
The most debilitating malunion is dorsal elevation of the capital fragment. The initial chevron osteotomy inherently shortens the first ray by 3 to 5 mm. If impaction, necrosis, or dorsal tilt occurs, the ray can shorten an additional 3 to 5 mm (totaling 6 to 10 mm of shortening). This dorsal elevation unloads the first ray, leading to severe transfer metatarsalgia beneath the lesser metatarsal heads (typically the second). Correcting a dorsal malunion is technically demanding because restoring length requires structural bone grafting.
Coronal Plane Malunion:
Varus or valgus malunions can occur but are less common than dorsal malunions. Interestingly, a varus or valgus malunion—even with mild-to-moderate MTP joint incongruity—is generally tolerated much better by the patient than a dorsal malunion with transfer metatarsalgia.
🔪 Surgical Technique 81-27: Correcting Chevron Malunion
Regardless of the plane of the malunion (dorsal, varus, or valgus), the surgical approach to correct the deformity follows a standard protocol:
- Exposure: Expose the distal first metatarsal from the junction of the middle and distal thirds down to the base of the proximal phalanx. Ensure meticulous hemostasis and handle the soft tissues gently to preserve any remaining vascularity.
- Inspection: Inspect the previous osteotomy site. The bone will often be remodeled, and the original osteotomy lines may be obscured by callus or scar tissue.
- De novo Planning: Crucial Step: Do not allow the "limbs" of the previous osteotomy to predetermine the plane of your corrective osteotomy. Plan the new osteotomy based on the current mechanical axis, the required plantarflexion to restore weight-bearing, and the necessary length restoration (which may require an opening wedge with structural allograft or autograft).
POSTOPERATIVE PROTOCOL: THE "RULE OF THREES"
Rehabilitation following a revision distal metatarsal osteotomy requires strict adherence to postoperative protocols to prevent displacement and manage edema. The classic "Rule of Threes" applies to the recovery timeline:
- 3 Days: Strict rest and continuous elevation of the operative extremity above heart level to minimize acute postoperative edema and hematoma formation.
- 3 Weeks: Protected weight-bearing in a rigid postoperative shoe with a compressive surgical dressing. The dressing acts as a splint to maintain the soft tissue correction.
- 3 Months: The minimum time required before postoperative swelling is sufficiently reduced to attempt wearing standard footwear. Patients should be counseled to transition into a low-heeled, round toe box dress shoe constructed of a soft, yielding material to accommodate residual edema. Full bony consolidation and maximal medical improvement may take up to one year.
📚 Medical References
- Distal metatarsal osteotomy for intractable plantar keratoses, Foot Ankle Int 10:247, 1990.
- Mann RA: Intractable plantar keratosis, Instr Course Lect 33:287, 1984.
- Mann RA, Chou LB: Surgical management for intractable metatarsalgia, Foot Ankle Int 16:322, 1995.
- Mann RA, DuVries H: Intractable plantar keratosis, Orthop Clin North Am 4:67, 1973.
- Mann RA, Wapner KL: Tibial sesamoid shaving for treatment of intractable plantar keratosis, Foot Ankle 13:196, 1992.
- Meyer J, Tomeno B, Burdet A: Metatarsalgia due to insuffi cient support by the fi rst ray, Int Orthop 5:193, 1981.
- Montgomery R: Dermatologic care of the painful foot, J Bone Joint Surg 46A:1129, 1964.
- Pedowitz WJ: Distal oblique osteotomy for intractable plantar keratosis of the middle three metatarsals, Foot Ankle 9:7, 1988.
- Schlamberg EL, Lorenz MA: A dorsal wedge V-osteotomy for painful plantar callosities, Foot Ankle 4:30, 1983.
- Slovenkai MP, Linehan D, McGrady L, et al: Comparison of two fi xation methods of oblique lesser metatarsal osteotomies: a biomechanical study, Foot Ankle Int 16:437, 1995.
- Spence KF, O’Connell SJ, Kenzora JE: Proximal metatarsal segmental resection: a treatment for intractable plantar keratoses, Orthopedics 13:741, 1990.
- Thompson FM, Hamilton WG: Problems of the second metatarsophalangeal joint, Orthopedics 10:83, 1987.
- Trnka HJ, Kabon B, Zettl R, et al: Helal metatarsal osteotomy for the treatment of metatarsalgia: a critical analysis of results, Orthopedics 19:457, 1996.
- Bunionette Coughlin MJ: Etiology and treatment of the
