INTRODUCTION TO CEREBRAL PALSY CLASSIFICATION
Cerebral palsy (CP) represents a heterogeneous group of permanent, non-progressive disorders of movement and posture caused by a developmental insult to the immature fetal or infant brain. Because of the wide variability in clinical presentation, neuroanatomical pathology, and physiological manifestations, there is no single universally accepted classification scheme. Instead, orthopedic surgeons rely on a multidimensional classification approach to accurately describe the patient, predict the natural history of musculoskeletal deformities, and formulate precise surgical indications.
Cerebral palsy is systematically classified across three primary domains:
1. Topographical (Anatomical) Classification: Based on the region of the body affected.
2. Physiological (Motor) Classification: Based on the clinical movement disorder and the neuroanatomical region of the brain injured.
3. Functional Classification: Based on the patient's gross motor capabilities and need for assistive devices.
Understanding these classifications is not merely an academic exercise; it is the foundational step in preoperative planning. The surgical management of a patient with spastic diplegia differs fundamentally from that of a patient with athetoid quadriplegia.
TOPOGRAPHICAL CLASSIFICATION (ANATOMICAL DISTRIBUTION)
The topographical classification describes the anatomical distribution of motor impairment. While overlaps exist, this system provides an immediate clinical picture of the patient's structural deficits.
Hemiplegia
In hemiplegia, one side of the body is involved, with the upper extremity typically more affected than the lower extremity. Hemiplegia accounts for approximately 30% of all patients with cerebral palsy.
Clinical Pearl: Patients with hemiplegia frequently exhibit sensory changes in the affected extremities. Severe sensory deficits, particularly impaired stereognosis and two-point discrimination in the upper extremity, are strong predictors of poor functional outcomes following reconstructive tendon transfers.
Orthopedic manifestations often include a leg-length discrepancy, with the affected side being shorter due to diminished longitudinal bone growth secondary to decreased mechanical loading and neurological trophic factors. Equinovarus foot deformities are common and often require split anterior tibial tendon (SPLATT) transfers combined with Achilles tendon lengthening.
Diplegia
Diplegia is the most common anatomical type of cerebral palsy, constituting approximately 50% of all cases. Patients with diplegia exhibit motor abnormalities in all four extremities, but the lower extremities are significantly more affected than the upper extremities.
The pathophysiology is strongly linked to periventricular leukomalacia (PVL) in premature infants. The close anatomical proximity of the descending corticospinal tracts serving the lower extremities to the lateral ventricles explains the disproportionate lower limb involvement. Intelligence is usually normal or near-normal. Most children with diplegia will eventually achieve ambulation, although independent walking is typically delayed until around 4 years of age. These patients are the classic candidates for Single-Event Multilevel Surgery (SEMLS) to correct crouch gait or equinus deformities.
Quadriplegia
In quadriplegia, all four extremities are equally and severely involved. The neurological insult is usually global, such as hypoxic-ischemic encephalopathy (HIE). Many patients have significant cognitive deficiencies, seizure disorders, and visual impairments that complicate multidisciplinary care.
Head and neck control are usually present to some degree, which aids in communication, education, and wheelchair seating. The orthopedic treatment goals for quadriplegic patients are strictly palliative and focused on facilitating care:
* A straight, balanced spine over a level pelvis.
* Located, mobile hips with at least 90 degrees of flexion for sitting and 30 degrees of abduction for perineal hygiene.
* Plantigrade feet that can accommodate standard footwear or orthoses.
* An appropriate, customized wheelchair seating system.
Total Body Involvement
Patients with total body involvement represent the most severe end of the spectrum. They typically possess profound cognitive deficits combined with a complete loss of head and neck control. These patients require full-time, maximal assistance for all activities of daily living (ADLs). Dysphagia, dysarthria, and severe drooling are common, often necessitating gastrostomy tubes and complicating anesthesia due to high aspiration risks.
Rare and Atypical Presentations
- Double Hemiplegia: Results from bilateral, asymmetrical hemispheric bleeding. The upper extremities are typically more involved than the lower extremities, differentiating it from diplegia.
- Monoplegia: Extremely rare, usually occurring post-meningitis. Most patients diagnosed with monoplegia actually have subtle hemiplegia with one extremity only very mildly affected.
- Paraplegia: Characterized by bilateral lower extremity involvement with completely normal upper extremity function. True paraplegic CP is exceedingly rare; most are actually diplegic patients with very mild upper limb deficits.
- Triplegia: The involvement of three extremities. Most authorities agree true triplegia does not exist; careful neurological examination usually reveals subtle motor deficits in the "uninvolved" fourth limb, reclassifying the patient as quadriplegic or double hemiplegic.
PHYSIOLOGICAL CLASSIFICATION (NEUROANATOMICAL SUBSTRATE)
Physiological classification categorizes the predominant movement disorder, which directly correlates with the specific neuroanatomical timing and location of the brain injury.
During the first trimester, the immature brain separates into gross structures (cerebrum, cerebellum, medulla). Neurons form in the second trimester, and the total neuronal count is fixed by the end of this period; lost neurons are irreplaceable. Synaptogenesis and myelination begin in the third trimester and continue through adolescence. Because different neural pathways myelinate at different rates, the clinical presentation of CP evolves. Spastic diplegia is usually detected at 8 to 10 months, hemiplegia at 20 months, and athetoid CP after 24 months.
Physiologically, CP is divided into Spastic (Pyramidal) and Extrapyramidal types.
Spastic (Pyramidal) Cerebral Palsy
Spasticity is the most common physiological form, comprising approximately 80% of cases. It results from injury to the pyramidal tracts (motor cortex and descending corticospinal tracts). Spasticity is defined clinically as a velocity-dependent increase in muscle tone with passive stretch, caused by an exaggeration of the normal muscle stretch reflex due to a loss of descending cortical inhibition.
Pathophysiological Pearl: Booth demonstrated histologically that chronic spasticity alters muscle architecture, leading to the pathological deposition of type I collagen in the endomysium. This results in irreversible muscle thickening, fibrosis, and shortening (contracture). The degree of fibrosis correlates directly with the clinical severity of the spasticity. This explains why physical therapy alone cannot reverse established contractures, necessitating surgical lengthening.
Extrapyramidal Cerebral Palsy
Extrapyramidal CP results from damage to the basal ganglia, thalamus, or cerebellum. It is characterized by abnormal regulation of tone and coordination, rather than true spasticity.
- Athetoid (Dyskinetic): Characterized by slow, writhing, purposeless movements exacerbated by stress or environmental stimulation. Historically associated with kernicterus (Rh incompatibility), its incidence has decreased. Joint contractures are uncommon because the limbs are in constant motion. Surgical Warning: Soft-tissue releases in pure athetoid CP are highly unpredictable and carry a severe complication rate, including iatrogenic joint instability and reversal of deformity.
- Choreiform: Features rapid, jerky, continual purposeless movements of the distal extremities (wrists, fingers, toes). This continuous movement makes orthotic bracing and wheelchair seating exceptionally difficult.
- Rigid: Patients exhibit "cogwheel" or "lead pipe" hypertonicity without the hyperreflexia or clonus seen in spasticity. Surgical Pitfall: When surgical release is attempted for rigid contractures, it is critical not to over-weaken the muscle, as the unopposed antagonist will rapidly drive the joint into the opposite deformity.
- Ataxic: Results from cerebellar injury, leading to a profound disturbance of coordinated movement and balance. It is frequently misdiagnosed. True ataxia must be distinguished from spasticity because overaggressive tendon lengthening in ataxic patients causes devastating iatrogenic weakness, permanently destroying their ability to ambulate.
- Hypotonic: Characterized by profound weakness, low muscle tone, but normal deep tendon reflexes. Many children pass through a transient hypotonic stage lasting 1 to 2 years before the true spastic or ataxic nature of their injury manifests.
Mixed Cerebral Palsy
Many patients exhibit features of both pyramidal and extrapyramidal damage. The final clinical appearance depends on the relative balance of spasticity, athetosis, and ataxia. Surgical outcomes in mixed CP are less predictable, particularly if a large dyskinetic component is present.
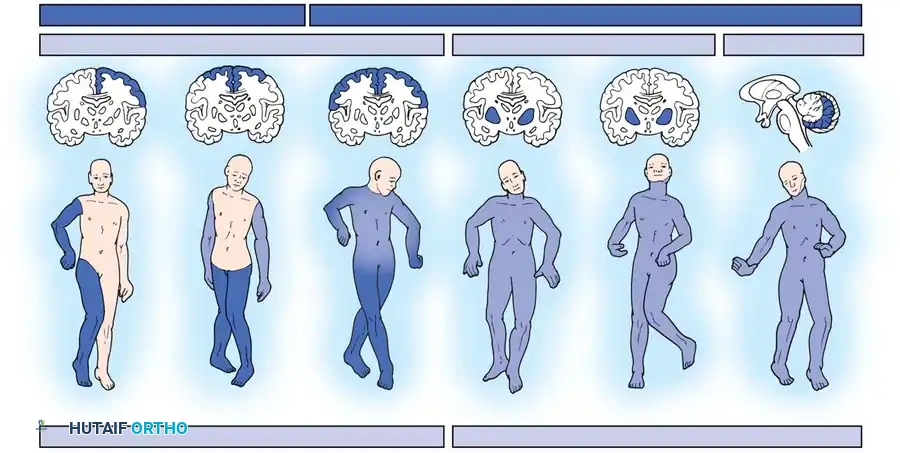
FUNCTIONAL CLASSIFICATION: THE GMFCS
Because topographical and physiological classifications do not adequately describe a child's functional capacity, Palisano et al. developed the Gross Motor Function Classification System (GMFCS). This five-level grading system is a highly reliable, age-stratified method for predicting motor function, focusing on self-initiated movement, sitting, and walking.
- GMFCS Level I: Walks without limitations.
- GMFCS Level II: Walks with limitations (struggles with long distances or uneven terrain).
- GMFCS Level III: Walks using a hand-held mobility device (walkers, crutches).
- GMFCS Level IV: Self-mobility with limitations; may use powered mobility.
- GMFCS Level V: Transported in a manual wheelchair; severe limitations in head and trunk control.
Clinical Significance: Soo et al. demonstrated that GMFCS level is the single most powerful predictor of hip displacement in cerebral palsy. Patients with GMFCS Levels IV and V have a >70% risk of progressive hip subluxation and dislocation, mandating rigorous radiographic surveillance programs (AP pelvis X-rays every 6-12 months).
BIOMECHANICS AND PATHOPHYSIOLOGY OF DEFORMITY
The orthopedic manifestations of cerebral palsy are a direct result of the underlying neurological deficit acting on the growing musculoskeletal system. The primary biomechanical driver is lever arm dysfunction.
In a normal child, balanced muscle forces guide the physiological remodeling of bone (e.g., the gradual decrease in femoral anteversion and neck-shaft angle). In spastic CP, simultaneous co-contraction of antagonistic muscle groups and chronic spasticity lead to:
1. Muscle Fibrosis and Contracture: As described by Booth, the failure of the muscle belly to grow in tandem with the long bones.
2. Bony Torsion: Persistent fetal alignment, such as excessive femoral anteversion and external tibial torsion.
3. Joint Instability: The classic example is the spastic hip, where overpowering adductors and flexors drive the femoral head posterosuperiorly, leading to acetabular dysplasia and eventual dislocation.
SURGICAL PRINCIPLES AND OPERATIVE APPROACHES
Orthopedic intervention in cerebral palsy aims to optimize function, prevent joint degeneration, and ease the burden of care. Surgery does not cure the neurological deficit; it addresses the secondary musculoskeletal consequences.
Preoperative Planning and Indications
Surgical decision-making relies heavily on computerized 3D gait analysis (CGA) for ambulatory patients (GMFCS I-III) to differentiate between dynamic spasticity and fixed contractures.
* Indications for Surgery: Fixed joint contractures failing conservative management (Botulinum toxin, serial casting), progressive hip subluxation (Reimers' migration percentage >30%), severe spinal deformity, and lever arm dysfunction (rotational malalignment).
Patient Positioning and Anesthesia
- Positioning: Meticulous padding is required. Patients with severe contractures (GMFCS IV-V) are at high risk for pressure necrosis and iatrogenic fractures during positioning.
- Anesthesia: Avoid succinylcholine due to the theoretical risk of hyperkalemia in upper motor neuron lesions. Neuromonitoring (SSEP/MEP) is mandatory during spinal fusions and complex pelvic osteotomies.
Single-Event Multilevel Surgery (SEMLS)
For ambulatory patients with diplegia, the modern standard of care is SEMLS. Rather than performing isolated procedures year after year ("birthday syndrome"), all soft-tissue and bony deformities are corrected simultaneously in one anesthetic event.
Step-by-Step Overview of a Typical SEMLS:
1. Soft Tissue Releases:
* Hip: Psoas lengthening over the pelvic brim (avoiding complete tenotomy to preserve hip flexion power).
* Knee: Medial hamstring lengthening (semitendinosus and gracilis) and fractional lengthening of the semimembranosus to correct flexion contractures.
* Ankle: Gastrocnemius recession (Strayer or Baumann procedure) or Achilles tendon lengthening, depending on the Silfverskiöld test results.
2. Bony Osteotomies:
* Femur: Varus Derotational Osteotomy (VDRO) to correct excessive femoral anteversion and contain the hip. Fixed with a pediatric locking blade plate.
* Tibia: Distal tibial derotational osteotomy to correct external tibial torsion, restoring the foot progression angle.
* Foot: Calcaneal lengthening osteotomy (Evans procedure) to correct spastic pes planovalgus and restore the lateral column.
Hip Reconstruction in Non-Ambulatory Patients (GMFCS IV-V)
For severe hip subluxation, soft-tissue release alone is inadequate. A comprehensive bony reconstruction is required:
1. Approach: Anterior Smith-Petersen or lateral approach.
2. Femoral Osteotomy: A VDRO is performed to redirect the femoral head into the true acetabulum.
3. Pelvic Osteotomy: A Dega or San Diego pericapsular osteotomy is performed to hinge the acetabular roof downward, providing anterolateral coverage. The osteotomy is grafted with bone wedges obtained from the femoral shortening.
Postoperative Protocols and Rehabilitation
Postoperative care is as critical as the surgery itself.
* Immobilization: Depending on the procedures, patients may require short-leg casts, long-leg casts, or a hip spica cast for 4 to 6 weeks.
* Orthotics: Upon cast removal, patients are transitioned to custom Ankle-Foot Orthoses (AFOs) to maintain plantigrade alignment and prevent recurrence of equinus.
* Rehabilitation: Intensive physical therapy is initiated immediately to restore baseline strength. It typically takes 9 to 12 months for a patient to fully realize the functional benefits of a SEMLS procedure.
By integrating topographical, physiological, and functional classifications, the orthopedic surgeon can navigate the profound complexities of cerebral palsy, tailoring surgical interventions to maximize the patient's quality of life and functional independence.
===CONTENT===
