Introduction & Epidemiology
Supracondylar fractures of the humerus (SCHF) represent a significant proportion of pediatric elbow injuries, commanding careful attention due to their potential for severe neurovascular complications and long-term functional deficits. These fractures are the most common elbow fracture in children, accounting for approximately 60-70% of pediatric elbow fractures and 17% of all childhood fractures. The peak incidence occurs in early to middle childhood, typically between 5 and 7 years of age, coinciding with periods of increased motor activity and developing bone architecture.
The vast majority (approximately 97%) of SCHFs are of the extension type, resulting from a fall onto an outstretched hand with the elbow hyperextended. Less commonly, flexion-type injuries occur, typically from a direct fall onto the posterior aspect of a flexed elbow. While open injuries are rare (occurring in about 1% of cases), concurrent fractures, most commonly involving the distal radius, scaphoid, or proximal humerus, can occur in a similar proportion. A critical aspect of these injuries is the potential for associated neurovascular compromise. Preoperative nerve injury is reported in up to 8% of cases, predominantly affecting the median and anterior interosseous nerves, followed by the radial and ulnar nerves. Vascular insufficiency, typically involving the brachial artery, presents in 1% to 2% of cases and warrants immediate attention. The high incidence, specific age group, and potential for complications underscore the importance of a comprehensive understanding of their management, with closed reduction and percutaneous pinning (CRPP) remaining the gold standard for displaced fractures.
Surgical Anatomy & Biomechanics
A thorough understanding of the distal humeral anatomy and its biomechanical response to injury is paramount for successful reduction and stable fixation of supracondylar fractures. The distal humerus features a complex configuration designed for articulation with the radius and ulna, comprising medial and lateral columns that converge proximally at the supracondylar ridges. The trochlea (medial) articulates with the ulna, while the capitellum (lateral) articulates with the radial head. The coronoid and radial fossae anteriorly, and the olecranon fossa posteriorly, accommodate the respective forearm bones during flexion and extension.
The critical neurovascular structures surrounding the distal humerus are intimately related to the fracture planes, particularly in extension-type injuries. The brachial artery and median nerve course anterior to the humerus, crossing the fracture line and becoming susceptible to direct injury, entrapment, or kinking with fracture displacement. The radial nerve typically spirals around the posterior aspect of the humerus more proximally, but its deep branch (posterior interosseous nerve) or terminal branches can be affected. The ulnar nerve is particularly vulnerable, tracking posteromedially in the cubital tunnel region, adjacent to the medial epicondyle, making it susceptible to injury during medial pin placement or significant medial displacement of the fracture fragment.
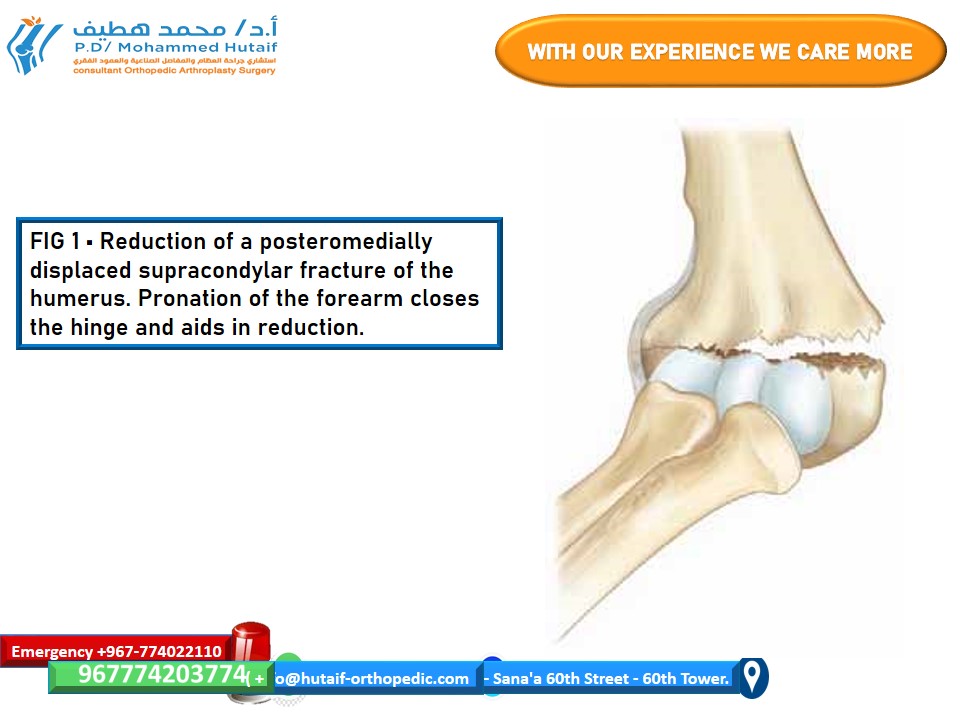
In extension-type supracondylar fractures, the periosteum typically fails anteriorly, acting as a critical hinge posteriorly. This posterior periosteal hinge is exploited during reduction maneuvers. The pattern of periosteal failure can vary with the direction of distal fragment displacement:
* With
posteromedial displacement
, the periosteum also fails laterally. In such instances, pronation of the forearm can tighten the intact medial periosteal hinge, aiding in the reduction by correcting rotational and medial displacement components.

-
Conversely, with
posterolateral displacement
, the periosteum also fails medially. Here, forearm supination can be utilized to close the intact lateral periosteal hinge, thereby assisting in the reduction of the distal fragment.
The dynamic interplay between the distal fragment's displacement and the remaining periosteal integrity dictates specific reduction maneuvers, highlighting the importance of assessing fracture morphology comprehensively. The goal of reduction is to restore anatomical alignment, specifically the anterior humeral line passing through the middle third of the capitellum on a true lateral view, and to normalize Baumann's angle (the angle between the capitellar physis and the lateral cortex of the humeral shaft) on an AP view.
Indications & Contraindications
The management strategy for supracondylar fractures of the humerus is primarily dictated by the degree of displacement, as classified by Gartland:
Gartland Classification (Modified)
- Type I: Non-displaced fracture.
-
Type II:
Displaced fracture with an intact posterior cortex or hinge.
- Type IIA: Rotationally stable, minimally displaced.
- Type IIB: Rotationally unstable, anterior cortical comminution, or significant gapping of the anterior cortex with intact posterior hinge.
-
Type III:
Completely displaced fracture with no cortical contact between the proximal and distal fragments.
- Type IIIA: Posteromedial displacement.
- Type IIIB: Posterolateral displacement.
- Type IV: Multidirectionally unstable in flexion and extension, indicating complete disruption of both anterior and posterior periosteum. Often associated with significant soft tissue injury.
Operative vs. Non-Operative Indications
The decision for operative intervention, specifically closed reduction and percutaneous pinning (CRPP), hinges on the fracture type and associated complications.
| Indication Category | Operative Management (CRPP) | Non-Operative Management |
|---|---|---|
| Gartland Type I | Rare. Only if concerns for occult displacement, severe pain, or impending neurovascular compromise, though typically unnecessary. | Standard: Long arm cast or splint in 90 degrees of flexion and neutral rotation for 3-4 weeks. Close follow-up with radiographs to monitor for secondary displacement. |
| Gartland Type II |
Mandatory for Type IIB
(rotationally unstable, significant anterior gapping).
Highly Recommended for Type IIA if significant displacement, angulation >20 degrees, or if closed reduction without pinning cannot maintain stable reduction. CRPP provides superior stability and earlier mobilization potential. |
Type IIA: Attempt at closed reduction and cast/splint is possible if reduction is stable and acceptable alignment is achieved. Frequent follow-up is crucial. |
| Gartland Type III | Standard of care: Closed reduction and percutaneous pinning (CRPP) is indicated for all completely displaced fractures. | Not indicated. Risk of malunion, nonunion, and neurovascular compromise is unacceptably high. |
| Gartland Type IV | Standard of care: CRPP. Often challenging due to complete periosteal disruption and instability. May require greater pin fixation or even open reduction if closed reduction fails. | Not indicated. Extreme instability. |
| Vascular Compromise | Absolute indication for emergent reduction and fixation. If pulseless "pink" hand, reduction may restore perfusion. If pulseless "white" hand or no restoration after reduction, vascular exploration (with or without repair) is indicated. | Not indicated. |
| Nerve Injury | Pre-existing nerve injury itself is not a contraindication to CRPP; careful reduction and fixation are still indicated to prevent further injury. Post-reduction neurovascular assessment is critical. | Not indicated for displaced fractures with nerve injury. Reduction and fixation help decompress or realign structures potentially causing nerve injury. |
| Open Fractures | Following thorough irrigation and debridement, CRPP is generally performed for appropriate fracture types. External fixation may be considered for severe contamination or soft tissue loss. | Not indicated. |
| Failed Closed Reduction | If acceptable reduction cannot be achieved or maintained under fluoroscopy, even after multiple attempts, conversion to open reduction may be necessary. | Not applicable. |
Contraindications for CRPP
Absolute contraindications for CRPP are rare. The primary contraindication is a non-displaced (Gartland Type I) fracture, which can be managed non-operatively. Relative contraindications include:
*
Significant skin compromise or severe contamination in open fractures:
May necessitate external fixation initially, followed by delayed definitive fixation, or primary open reduction for debridement.
*
Excessive swelling:
While not a contraindication to immediate reduction and pinning for displaced fractures, severe swelling may increase the risk of compartment syndrome post-operatively.
*
Age and bone quality:
Extremely young children with very soft bone may have reduced pin purchase, but this usually impacts pin technique rather than contraindicating CRPP.
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning and appropriate patient positioning are crucial for successful closed reduction and percutaneous pinning.
Pre-Operative Assessment
-
Clinical Examination:
- Neurovascular Assessment: This is paramount. Document pre-injury and pre-operative neurological function (median, ulnar, radial nerves – motor and sensory components) and vascular status (radial and ulnar pulses, capillary refill, hand warmth and color). Any changes post-injury or during transport must be noted. Special attention to the "pulseless pink hand" phenomenon.
- Soft Tissue Assessment: Evaluate for open wounds, abrasions, ecchymosis, and degree of swelling. Document skin integrity.
- Compartment Syndrome Evaluation: Be vigilant for signs of acute compartment syndrome, particularly in cases with significant swelling or vascular compromise.
-
Radiographic Evaluation:
- Standard Views: True anteroposterior (AP) and lateral radiographs are essential. Oblique views may be helpful to characterize fracture patterns fully.
- Traction Views (Optional): In cases of severe displacement and significant overlap, gentle in-line traction radiographs can help delineate the fracture pattern and identify potential comminution or interposition of soft tissues.
- Assessment: Evaluate the degree of displacement, angulation (varus/valgus, flexion/extension), and rotation. Identify the status of the medial and lateral columns, and assess the integrity of the posterior periosteum. Measure Baumann's angle on the AP view and anterior humeral line on the lateral view.
Equipment
- Fluoroscopy (C-arm): Essential for real-time visualization of reduction and pin placement. Must be capable of obtaining true AP and lateral views without significant repositioning of the extremity.
- Operating Table: Radiolucent hand table or carbon fiber extension is ideal.
- Tourniquet: Sterile pneumatic tourniquet is routinely used for a bloodless field, typically inflated after limb elevation.
- K-wires: 1.6 mm (0.062 inches) or 2.0 mm (0.078 inches) diameter, usually threaded tips for improved bone purchase. A range of lengths should be available.
- Pin Driver: Battery-powered oscillating drill or hand driver.
- Pin Cutters, Bending Irons, Caps: For post-fixation management of pins.
- Sterile Drape Kit: Specific elbow draping kit.
- Cast Materials: Appropriate materials for a long arm cast.
Patient Positioning
The patient is typically positioned supine on the operating table.
-
Arm Positioning:
- The affected arm is placed on a radiolucent hand table or allowed to hang off the side of the table. The latter allows for gravity-assisted traction and easier manipulation, but requires a sterile assistant to hold the arm.
- Drape the arm free from the shoulder to the fingertips to allow full range of motion during reduction.
-
C-arm Positioning:
- The C-arm unit is positioned to allow for immediate acquisition of true AP and lateral views without significant repositioning of the arm or the C-arm. This is critical for efficient and accurate reduction and pinning.
- Typically, the C-arm is placed perpendicular to the limb for the lateral view, and then rotated 90 degrees for the AP view. Some setups utilize an oblique C-arm position with the arm oriented specifically to capture both views with minimal C-arm rotation. Ensure the contralateral limb is secured out of the field of view.

* Lateral View Check: Confirm a true lateral view by superimposing the medial and lateral epicondyles. The anterior humeral line should pass through the middle third of the capitellum.
* AP View Check: Confirm a true AP view by ensuring the trochlea and capitellum are clearly visible, and the olecranon fossa is centered. Baumann's angle should be assessed.

-
Tourniquet Application: A sterile tourniquet is applied to the upper arm. The limb is elevated for exsanguination, and the tourniquet is inflated to appropriate pressure (e.g., 200-250 mmHg or 100 mmHg above systolic blood pressure). A bloodless field significantly enhances visualization and precision during pin placement.
Detailed Surgical Approach / Technique
The goal of CRPP is to achieve stable, anatomical or near-anatomical reduction of the fracture and maintain it with percutaneous K-wire fixation, minimizing neurovascular risks.
Anesthesia and Preparation
General anesthesia is standard. After proper positioning and tourniquet inflation, the entire arm is prepped and draped using sterile technique, allowing full motion of the shoulder, elbow, and wrist.
Reduction Maneuvers
Reduction is typically performed under fluoroscopic guidance and consists of several sequential steps:
-
Traction:
- Apply gentle, sustained in-line traction to the forearm with the elbow in slight extension (approximately 20-30 degrees). This helps to disimpact the fracture, stretch the soft tissues, and restore length. Traction is often applied for several minutes to achieve adequate relaxation.
-
Correction of Displacement:
- Medial/Lateral Displacement: While maintaining traction, correct any varus or valgus angulation. For posteromedial displacement (most common), correct the medial displacement. For posterolateral displacement, correct the lateral displacement.
- Rotation: Correct rotational deformity. As discussed, pronation is used for posteromedial displacement (to tighten the medial periosteal hinge), and supination for posterolateral displacement (to tighten the lateral periosteal hinge). This helps to realign the distal fragment with the humeral shaft.
- Anterior/Posterior Displacement: Apply direct pressure to the olecranon posteriorly to push the distal fragment anteriorly and reduce posterior displacement. This is often combined with traction.
-
Flexion and Stabilization:
- Once length, rotation, and medial/lateral displacements are corrected, the elbow is acutely flexed, typically to 100-110 degrees, or even to the point where the radial pulse is lost (then slightly extended until the pulse returns). Acute flexion helps to "lock" the fracture fragments by engaging the olecranon into the olecranon fossa and tensioning the posterior periosteum, stabilizing the reduction. It also helps to prevent anterior displacement of the distal fragment.
-
Confirmation of Reduction:
-
Fluoroscopic Assessment:
Obtain true AP and lateral views.
- Lateral View: The anterior humeral line (a line drawn along the anterior cortex of the humeral shaft) should pass through the middle third of the capitellum. Assess for any residual posterior displacement or rotational malalignment.
- AP View: Assess Baumann's angle (normal range 64-81 degrees) and ensure restoration of the medial and lateral columns. Check for any varus/valgus angulation.
- Palpation: Palpate the medial and lateral epicondyles to ensure their relationship with the olecranon is anatomically correct and symmetric.
-
Fluoroscopic Assessment:
Obtain true AP and lateral views.
If a satisfactory reduction cannot be achieved after several attempts, consider conversion to open reduction, although this is usually a last resort due to increased soft tissue disruption and infection risk.
Pinning Techniques
The primary goal of pinning is stable fixation while minimizing iatrogenic neurovascular injury. Several pinning configurations are described, each with its advantages and disadvantages.
-
Lateral Entry Pinning (Most Common and Safest):
- This technique is preferred due to a significantly lower risk of iatrogenic ulnar nerve injury compared to cross-pinning.
-
Two Divergent Lateral Pins:
- Entry Point: Both pins enter the lateral epicondylar region. The exact entry point for the first pin is typically just proximal to the lateral epicondyle, aiming to engage the medial cortex proximally.
-
Trajectory:
- First Pin: Often placed from posterior-lateral to anterior-medial. It should cross the fracture line and engage the far medial cortex of the humerus, providing a strong purchase.
- Second Pin: Placed anterior-lateral to posterior-medial, diverging from the first pin. It also crosses the fracture and engages the medial cortex, creating a stable construct. The divergence increases the stability against rotational forces.
- Fluoroscopic Guidance: Drive pins under continuous fluoroscopy, observing both AP and lateral views to ensure they traverse the fracture and engage the medial cortex without penetrating the anterior or posterior cortex of the humeral shaft or the articular surface. Ensure pins are well separated at the fracture site.
-
Pearls:
- Avoid placing pins parallel to each other to maximize stability.
- Aim for maximum bone purchase in both fragments.
- Ensure the pin does not penetrate the medial soft tissue envelope, which could jeopardize the ulnar nerve or brachial artery.
- The pin tips should ideally be within the medial cortex, but not excessively far into the soft tissues.

-
Cross-Pinning (Medial and Lateral Entry Pins):
- This technique theoretically provides superior biomechanical stability compared to two lateral pins alone, particularly against torsional forces. However, it carries a higher risk of ulnar nerve injury.
- Lateral Pin: Similar to the lateral pinning technique, a lateral pin is placed first, typically from the lateral epicondyle crossing the fracture and engaging the medial cortex.
-
Medial Pin:
- Ulnar Nerve Protection: This is the critical step. The elbow is maximally flexed to tension the ulnar nerve, causing it to displace posteriorly. A mini-open approach (a small incision, ~1cm, centered over the medial epicondyle) is strongly recommended to directly visualize and protect the ulnar nerve. The nerve is gently retracted posteriorly.
- Entry Point: The pin is then inserted through the medial epicondyle.
- Trajectory: The medial pin crosses the fracture and engages the lateral cortex of the humerus.
- Fluoroscopic Guidance: Verify trajectory in AP and lateral views.
- Advantages: Biomechanically strong, offering good rotational stability.
- Disadvantages: Increased risk of iatrogenic ulnar nerve injury, necessitating meticulous technique and often an open approach for nerve protection.
-
Hybrid Configurations:
- In some complex or unstable fractures (e.g., Gartland IV), a combination of techniques might be used, such as two lateral pins and one medial pin (with ulnar nerve protection), or even three lateral pins. The goal is to achieve maximal stability without compromising neurovascular structures.
Post-Pinning Assessment
- Neurovascular Exam: Crucially, perform a repeat neurovascular assessment immediately after pinning and before casting. Check radial pulse, capillary refill, and motor/sensory function of median, ulnar, and radial nerves. Any new deficit warrants immediate investigation (e.g., pin removal, repositioning, or exploration).
- Fluoroscopic Check: Obtain final AP and lateral views to confirm satisfactory reduction and optimal pin placement. Ensure pin tips are not intra-articular and do not excessively protrude beyond the bone cortex.
Pin Management and Casting
- Pin Ends: Pins are typically bent at a gentle angle and cut just outside the skin, leaving enough length for easy removal in the clinic. Caps can be placed over the pin ends to prevent snagging and reduce infection risk. Alternatively, pins can be cut flush with the skin, requiring an incision for removal. The former is generally preferred for ease of removal.
- Cast Application: A long arm cast is applied, typically with the elbow flexed to 90 degrees and the forearm in neutral rotation. The cast extends from the axilla to just proximal to the metacarpophalangeal joints, ensuring adequate immobilization and protection of the pins. The cast should not be excessively tight, especially with swelling, to avoid compartment syndrome.
Complications & Management
Despite meticulous surgical technique, complications can arise following closed reduction and percutaneous pinning of supracondylar humeral fractures. Prompt recognition and appropriate management are crucial for optimal outcomes.
| Complication | Incidence | Management Strategy |
|---|---|---|
| Nerve Injury | ||
| - Pre-operative | 8-10% (most common: median/AION, then radial, ulnar) | Document thoroughly. Usually resolves spontaneously with reduction and stabilization. If no improvement or worsening, consider exploration. |
| - Post-operative (new or worsened) | 1-2% (iatrogenic: ulnar nerve most common, especially with medial pins) | Immediately re-evaluate reduction and pin placement (fluoroscopy). If related to a pin, remove or reposition pin. Observe for spontaneous recovery. If no recovery after 3-6 months, or if a nerve is impaled by a pin, consider nerve exploration (neurolysis or repair if transected). |
| Vascular Injury | ||
| - Pulseless Pink Hand | 1-2% pre-op; >50% resolve with reduction/pinning | Immediate, gentle closed reduction and pinning. Recheck pulses. If pulse returns and hand is pink/warm, observe. If pulse remains absent but hand is well-perfused ("pulseless pink"), closely monitor with Doppler or pulse oximetry. Some advocate observation; others recommend formal vascular exploration if no pulse persists. |
| - Pulseless Pale/White Hand | Rare, but critical. | Surgical Emergency. Immediate reduction and pinning. If pulses do not return promptly (within minutes), emergent vascular exploration is required. Consider fasciotomy if significant ischemia or reperfusion injury is suspected. Brachial artery repair, graft, or thrombectomy may be necessary. |
| Compartment Syndrome | <0.1% to 0.5% (higher risk with severe swelling, vascular injury, or tight cast) | Recognize early: pain out of proportion, pain with passive stretch of fingers, paresthesia, pallor, pulselessness (late sign). Immediately release cast and split all dressings. If symptoms persist or clinical suspicion is high, measure compartment pressures. Urgent forearm fasciotomy is indicated for confirmed compartment syndrome. |
| Malunion (Cubitus Varus) | 5-10% (most common long-term complication) | Prevention through accurate reduction and stable fixation. Managed non-operatively for cosmetic deformity alone in most cases. For severe functional deficits or significant cosmetic concerns (e.g., "gunstock deformity"), corrective osteotomy (e.g., lateral closing wedge osteotomy) is performed, typically after skeletal maturity. |
| Loss of Reduction | 1-3% | Most common in unstable fractures or inadequate fixation. Re-evaluate radiographs. If significant displacement, return to OR for re-reduction and re-pinning with potentially more pins or a different configuration. If minimal displacement and stable, may manage with continued immobilization and close observation. |
| Pin Tract Infection | 1-5% | Localized inflammation, erythema, drainage around pin sites. Minor infections: local wound care, oral antibiotics, continue to monitor. Severe infections (osteomyelitis or cellulitis): IV antibiotics, consider early pin removal if fracture sufficiently healed, debridement if necessary. Pin care instructions to parents are crucial. |
| Stiffness / Loss of Motion | Variable (often subtle, especially in extension) | Usually transient and resolves with gentle physical therapy. Avoid aggressive passive stretching, as this can lead to heterotopic ossification. Encourage early active range of motion after pin removal. Prolonged immobilization (beyond 3-4 weeks) or severe intra-articular changes can contribute to stiffness. |
| Hardware Failure/Migration | Rare | Fracture of K-wires or migration. If pins migrate, they must be removed. If significant fracture displacement occurs due to hardware failure, re-operation is indicated. |
| Heterotopic Ossification | Rare, but can occur with aggressive rehabilitation or repeated trauma | Avoid aggressive passive ROM. Manage symptomatically. Resection rarely indicated unless causing significant functional limitation after skeletal maturity. |
| Volkmann's Ischemic Contracture | Rare, severe (sequela of unmanaged compartment syndrome/vascular injury) | Prevention is key (early recognition and treatment of compartment syndrome/vascular compromise). Management involves staged releases (e.g., flexor mass release), tendon transfers, or free muscle transfers for severe, established contracture. |
Post-Operative Rehabilitation Protocols
Post-operative management following CRPP of supracondylar humerus fractures is a critical phase aimed at maintaining reduction, promoting fracture healing, and restoring functional range of motion while preventing complications.
Phase 1: Immobilization (0-3 to 6 weeks)
-
Immobilization:
- The limb is immobilized in a long arm cast, typically with the elbow flexed at 90 degrees and the forearm in neutral rotation. This position maintains reduction and protects the pin sites. The cast should extend from the axilla to just proximal to the metacarpophalangeal joints.
- The cast is often bivalved in the immediate post-operative period or replaced with a new cast after 3-5 days to accommodate for resolving swelling and reduce the risk of compartment syndrome.
-
Pain Management:
- Appropriate analgesia is provided, typically with acetaminophen and NSAIDs. Opioids are rarely needed beyond the initial 24-48 hours.
-
Elevation:
- Maintain the limb elevated above heart level, especially for the first 48-72 hours, to minimize swelling.
-
Pin Site Care:
- Instructions are given to parents/guardians regarding pin site cleanliness, monitoring for signs of infection (redness, swelling, warmth, drainage), and avoiding excessive movement of the pins.
-
Neurovascular Monitoring:
- Close monitoring of neurovascular status (pulses, capillary refill, motor and sensory function) is continued, particularly for the first 24-48 hours. Parents are educated on signs of neurovascular compromise to seek immediate medical attention.
-
Radiographic Follow-up:
- Initial follow-up typically occurs at 1-2 weeks post-operatively with radiographs (AP and lateral) to confirm maintenance of reduction.
- Subsequent follow-up is around 3-4 weeks or 4-6 weeks, depending on fracture stability and age, for pin removal.
Phase 2: Pin Removal & Early Motion (3-6 weeks)
-
Timing of Pin Removal:
- Pins are generally removed at 3-4 weeks for stable fractures in younger children, and at 4-6 weeks for more complex or unstable fractures, or in older children. Radiographic evidence of early callus formation is desirable. Pin removal is typically performed in an outpatient clinic setting under local anesthesia.
-
Post-Pin Removal Immobilization:
- After pin removal, some surgeons opt for a short period (1-2 weeks) of continued immobilization in a removable splint or cast for comfort and protection, especially if radiographs show immature callus. Others transition directly to activity modification.
-
Initiation of Motion:
- Gentle Active Range of Motion (AROM): Begin active, pain-free range of motion exercises for the elbow, forearm, and wrist. Emphasis is placed on gentle, active flexion and extension.
- Avoid Passive Range of Motion (PROM): Aggressive passive stretching or forced manipulation is strongly discouraged, as it can incite periosteal reaction and heterotopic ossification, leading to permanent stiffness. Gravity-assisted stretching (e.g., hanging arm exercises while standing) can be cautiously introduced as tolerated.
- Activities of Daily Living (ADLs): Encourage use of the arm for light ADLs within pain limits.
-
Physical Therapy (PT):
-
Formal physical therapy is usually not required for most uncomplicated supracondylar fractures in children, as they typically regain full or near-full range of motion spontaneously. However, it may be indicated for:
- Older children or adolescents with initial stiffness.
- Persistent limited range of motion (loss of >10-15 degrees compared to contralateral side).
- Complex fractures or associated injuries.
- The focus remains on active, functional movements, and patient/parent education on avoiding forceful activities.
-
Formal physical therapy is usually not required for most uncomplicated supracondylar fractures in children, as they typically regain full or near-full range of motion spontaneously. However, it may be indicated for:
Phase 3: Strengthening & Return to Activity (6 weeks - 3 months +)
-
Progressive Strengthening:
- Once a good range of motion is achieved and pain has subsided, gentle strengthening exercises can be initiated. This typically involves light resistance activities.
-
Activity Modification:
- Avoid high-impact activities, contact sports, or activities involving heavy lifting or pushing for at least 6-12 weeks post-pin removal, or until radiographic healing is evident and full strength/ROM is regained.
-
Return to Sports:
- A gradual return to sports and vigorous activities is permitted once full range of motion, strength, and confidence are restored, and there is no pain or tenderness at the fracture site. This usually occurs around 3-6 months post-injury.
-
Long-term Follow-up:
- Final follow-up is often at 6 months to 1 year to assess for long-term complications such as cubitus varus, persistent stiffness, or other deformities. Most children achieve excellent long-term functional outcomes, though a small residual loss of extension (typically <5-10 degrees) can be common but rarely functionally significant.
Summary of Key Literature / Guidelines
The management of supracondylar fractures of the humerus has evolved over decades, with closed reduction and percutaneous pinning establishing itself as the evidence-based gold standard for displaced variants. Key literature and guidelines consistently highlight several critical principles:
-
Closed Reduction and Percutaneous Pinning (CRPP) as the Gold Standard: Numerous studies and systematic reviews have affirmed that CRPP provides superior outcomes compared to open reduction for Gartland Type II, III, and IV fractures, with lower rates of complications such as infection, stiffness, and malunion. Open reduction is generally reserved for rare instances of failed closed reduction, open fractures requiring extensive debridement, or severe neurovascular compromise where soft tissue interposition is suspected.
- Meta-analyses by Zionts (1990), Ramachandran et al. (2018), and others consistently demonstrate the effectiveness and safety of CRPP.
-
Neurovascular Assessment is Paramount: Strict adherence to pre- and post-operative neurovascular examination protocols is emphasized. The presence of a "pulseless pink hand" remains a debated topic, with some literature supporting initial observation after successful reduction and others advocating for aggressive management including vascular exploration if the pulse does not return within a specified timeframe. However, a "pulseless pale hand" after reduction demands urgent vascular intervention.
- Recent guidelines from the American Academy of Orthopaedic Surgeons (AAOS) and Pediatric Orthopaedic Society of North America (POSNA) stress immediate reduction and careful monitoring for vascular compromise.
-
Pinning Configuration and Ulnar Nerve Risk:
- Lateral Entry Pins: Biomechanically, lateral-entry pins (typically two divergent pins) have been shown to provide adequate stability for most Gartland Type II and III fractures, with a significantly lower risk of iatrogenic ulnar nerve injury compared to cross-pinning. Many studies have demonstrated comparable clinical outcomes between lateral and cross-pinning techniques, leading to a strong preference for lateral pinning by many surgeons.
- Cross-Pinning (Medial and Lateral): While potentially offering superior biomechanical stability against rotational forces, cross-pinning carries a documented higher risk of iatrogenic ulnar nerve injury (up to 5-10%). If a medial pin is deemed necessary for enhanced stability (e.g., in highly unstable Gartland IV fractures or significantly comminuted fractures), a mini-open technique for direct visualization and protection of the ulnar nerve is strongly recommended and widely adopted.
- The debate regarding lateral vs. cross-pinning has been extensively studied, with a consensus favoring lateral pinning as the primary method, reserving medial pin placement for specific, high-instability cases with strict ulnar nerve precautions.
-
Importance of Acute Elbow Flexion for Reduction Stability: Achieving acute flexion (often 100-110 degrees) of the elbow after initial traction and rotational correction is a key maneuver to stabilize the fracture fragments by utilizing the intact posterior periosteal hinge and engaging the olecranon in the olecranon fossa. However, care must be taken not to excessively flex the elbow to the point of compromising the brachial artery.
-
Minimizing Malunion (Cubitus Varus): Cubitus varus, the most common long-term complication, is primarily a cosmetic deformity resulting from rotational and coronal plane malalignment. Accurate reduction, especially ensuring correct rotational alignment and restoration of Baumann's angle, is critical for prevention. Long-term functional deficits are rare even with significant cubitus varus, but corrective osteotomy can be performed for severe cosmetic concerns in older children.
-
Avoidance of Aggressive Physical Therapy: Pediatric literature emphasizes that aggressive passive range of motion exercises post-operatively can increase the risk of heterotopic ossification and lead to persistent stiffness. Gentle, active range of motion is preferred, with most children regaining excellent motion spontaneously.
In conclusion, the management of supracondylar humerus fractures requires a systematic approach, from accurate diagnosis and neurovascular assessment to precise surgical technique and careful post-operative rehabilitation. Adherence to established guidelines, coupled with clinical judgment and an understanding of the potential pitfalls, ensures optimal functional outcomes for these common pediatric injuries.