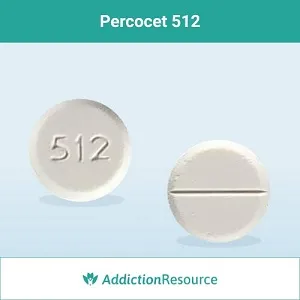
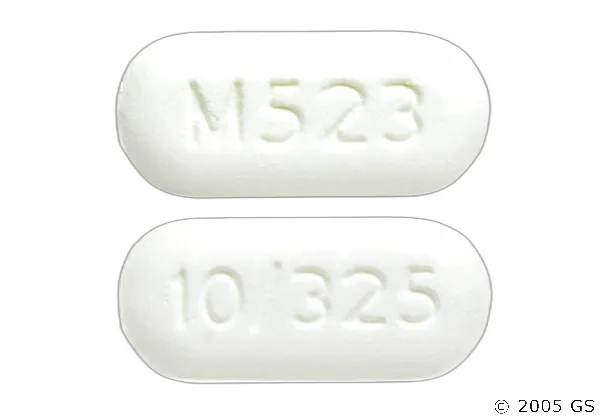
Percocet: A Comprehensive Medical SEO Guide to Moderate to Severe Pain Relief
Percocet is a widely recognized prescription medication used for the management of moderate to severe pain. As an expert medical SEO copywriter and orthopedic specialist, this guide aims to provide an exhaustive, authoritative, and technically accurate overview of Percocet, encompassing its mechanisms, clinical uses, safety profiles, and critical considerations for both patients and healthcare providers. Understanding this powerful analgesic combination is paramount for appropriate and safe pain management.
Percocet is a combination opioid analgesic containing two active ingredients: oxycodone hydrochloride, an opioid agonist, and acetaminophen, a non-opioid analgesic and antipyretic. This dual-action formulation allows for enhanced pain relief compared to either component alone, by targeting different pain pathways. Due to its opioid component, Percocet is classified as a Schedule II controlled substance, underscoring its potential for abuse, dependence, and addiction, and necessitating careful prescribing and monitoring.
Deep-Dive into Technical Specifications and Mechanisms
Understanding how Percocet works at a physiological level is crucial for appreciating its therapeutic effects and potential risks.
Mechanism of Action
Percocet's effectiveness stems from the synergistic action of its two components:
- Oxycodone Hydrochloride (Opioid Analgesic):
- Primary Action: Oxycodone is a semi-synthetic opioid agonist that primarily acts on mu-opioid receptors within the central nervous system (CNS) and to a lesser extent on kappa and delta receptors.
- Analgesia: By binding to these receptors, oxycodone mimics the effects of endogenous opioids (endorphins), inhibiting the transmission of pain signals from the periphery to the brain. It also alters the brain's perception of pain and emotional response to pain, leading to a sense of euphoria and pain relief.
- Other Effects: Opioid receptor activation can also lead to respiratory depression, sedation, miosis (pupil constriction), constipation, and physical dependence.
- Acetaminophen (Non-Opioid Analgesic/Antipyretic):
- Primary Action: The precise mechanism of acetaminophen is not fully elucidated, but it is believed to exert its analgesic and antipyretic effects primarily through central actions.
- Analgesia: It is thought to inhibit prostaglandin synthesis in the CNS, thereby raising the pain threshold. Unlike NSAIDs, it has minimal peripheral anti-inflammatory activity.
- Antipyresis: Acetaminophen produces antipyresis (fever reduction) by acting directly on the hypothalamic heat-regulating centers, leading to peripheral vasodilation and sweating, which facilitates heat dissipation.
Pharmacokinetics
The pharmacokinetics describe how the body absorbs, distributes, metabolizes, and eliminates Percocet's components.
- Absorption:
- Oxycodone: Rapidly absorbed from the gastrointestinal (GI) tract following oral administration. Peak plasma concentrations are typically reached within 1-2 hours.
- Acetaminophen: Also rapidly and almost completely absorbed from the GI tract. Peak plasma concentrations usually occur within 0.5-2 hours.
- Distribution:
- Both oxycodone and acetaminophen are widely distributed throughout body tissues.
- Oxycodone: Crosses the blood-brain barrier, placental barrier, and is excreted in breast milk. Plasma protein binding is approximately 45%.
- Acetaminophen: Plasma protein binding is minimal (10-25%) at therapeutic concentrations but increases with overdose. Also crosses the placental barrier and is excreted in breast milk.
- Metabolism:
- Oxycodone: Primarily metabolized in the liver via the cytochrome P450 (CYP) enzyme system, specifically CYP3A4 and CYP2D6. Major metabolites include noroxycodone (via CYP3A4) and oxymorphone (via CYP2D6), both of which are active. Oxymorphone is a potent opioid agonist and contributes to the analgesic effect.
- Acetaminophen: Primarily metabolized in the liver through glucuronidation (major pathway) and sulfation (minor pathway). A small amount is metabolized by CYP2E1 to a highly reactive, toxic intermediate metabolite, N-acetyl-p-benzoquinone imine (NAPQI). Under normal conditions, NAPQI is rapidly detoxified by conjugation with glutathione and excreted. In overdose, glutathione stores become depleted, leading to NAPQI accumulation and hepatotoxicity.
- Elimination:
- Oxycodone: Primarily excreted by the kidneys as metabolites and unchanged drug. The elimination half-life is approximately 3-4 hours.
- Acetaminophen: Excreted predominantly by the kidneys as glucuronide and sulfate conjugates, with less than 5% excreted as unchanged drug. The elimination half-life is approximately 2-3 hours.
Extensive Clinical Indications and Usage
Percocet is a potent analgesic reserved for specific pain management scenarios, with strict guidelines to ensure efficacy and minimize risks.
Detailed Indications
Percocet is indicated for the management of moderate to severe pain when the use of an opioid analgesic is appropriate and when alternative treatments are inadequate. It is generally recommended for short-term use due to the risks associated with long-term opioid therapy.
Common clinical situations where Percocet may be prescribed include:
- Post-Surgical Pain: Particularly following orthopedic surgeries (e.g., joint replacements, fracture repair), dental procedures, or abdominal surgeries, where acute pain is significant.
- Acute Traumatic Pain: Pain resulting from injuries such as fractures, severe sprains, dislocations, or extensive burns.
- Cancer Pain: For patients experiencing moderate to severe pain associated with cancer, often as part of a comprehensive pain management plan.
- Acute Pain Exacerbations: For severe acute flares of chronic conditions where baseline pain management is insufficient.
- Other Acute Pain Conditions: When non-opioid analgesics or weaker opioids fail to provide adequate relief.
Important Note: Due to the acetaminophen component, Percocet is generally not suitable for chronic pain management requiring high daily doses, as this increases the risk of liver toxicity.
Dosage Guidelines
Percocet dosing must be individualized, considering the patient's pain severity, response to treatment, prior analgesic experience, and risk factors for opioid-related adverse events.
- General Principles:
- Use the lowest effective dose for the shortest possible duration.
- Do not exceed the maximum recommended daily dose for either oxycodone or acetaminophen.
- Administer orally, with or without food.
- Available Strengths (Oxycodone/Acetaminophen):
- 2.5 mg / 325 mg
- 5 mg / 325 mg
- 7.5 mg / 325 mg
- 10 mg / 325 mg
- Typical Adult Starting Dose:
- One tablet of Percocet (e.g., 5 mg/325 mg) every 4-6 hours as needed for pain.
- Maximum Daily Doses:
- Oxycodone: The maximum recommended daily dose of oxycodone is generally 60 mg, though in some highly supervised cases for severe pain, up to 80 mg/day may be used.
- Acetaminophen: The maximum daily dose for acetaminophen from all sources (including Percocet and other acetaminophen-containing products) should not exceed 4000 mg. However, to mitigate liver toxicity risk, many clinicians and regulatory bodies recommend a maximum of 3250 mg/day for combination products.
- Dosage Adjustments:
- Renal Impairment: Reduced doses may be necessary due to decreased clearance of both components. Close monitoring is essential.
- Hepatic Impairment: Significant dose reduction is required, especially due to the acetaminophen component, which carries a heightened risk of hepatotoxicity in patients with liver disease.
- Elderly Patients: Start with lower doses and titrate slowly, as elderly patients may be more sensitive to opioid effects and have reduced renal/hepatic function.
- Pediatric Patients: Percocet is generally not recommended for pediatric use. If used in severe cases, it must be under strict specialist supervision with precise weight-based dosing.
- Discontinuation:
- For patients on Percocet for more than a few days, abrupt discontinuation can lead to opioid withdrawal symptoms. A gradual tapering schedule is recommended under medical supervision to minimize these effects.
Important Safety Information: Risks, Side Effects, and Contraindications
While effective for pain, Percocet carries significant risks that necessitate careful consideration and patient education.
Common Side Effects
Many side effects are dose-related and can often be managed.
- Gastrointestinal: Nausea, vomiting, constipation, abdominal pain.
- Management for Constipation: Increase dietary fiber, maintain adequate hydration, use stool softeners or laxatives as directed by a healthcare provider.
- Neurological: Drowsiness, dizziness, headache, lightheadedness.
- Dermatological: Pruritus (itching), sweating.
Serious Side Effects
These require immediate medical attention.
- Respiratory Depression: The most serious opioid-related adverse effect, potentially life-threatening. Symptoms include shallow breathing, slow breathing rate, cyanosis (bluish skin).
- Hepatotoxicity: Liver damage due to the acetaminophen component, especially with overdose, excessive daily doses, or concomitant alcohol use. Symptoms include jaundice (yellowing of skin/eyes), dark urine, abdominal pain, nausea, vomiting.
- Adrenal Insufficiency: Chronic opioid use can lead to symptoms like nausea, vomiting, anorexia, fatigue, weakness, dizziness, and low blood pressure.
- Serotonin Syndrome: Potentially life-threatening, particularly when Percocet is used with other serotonergic drugs. Symptoms include agitation, hallucinations, rapid heart rate, fever, sweating, muscle rigidity, tremor, incoordination, nausea, vomiting, diarrhea.
- Hypotension and Syncope: Especially with initial dosing or dose escalation.
- Allergic Reactions: Rare but possible, including rash, hives, swelling of the face, lips, tongue, or throat, difficulty breathing.
- Opioid Use Disorder, Physical Dependence, and Withdrawal: High potential for psychological and physical dependence. Abrupt cessation after prolonged use can lead to severe withdrawal symptoms.
Contraindications
Percocet should not be used in patients with:
- Hypersensitivity: Known allergy to oxycodone, acetaminophen, or any component of the formulation.
- Significant Respiratory Depression: Acute or severe respiratory depression.
- Acute or Severe Bronchial Asthma: In an unmonitored setting or in the absence of resuscitative equipment.
- Known or Suspected Paralytic Ileus: Or other gastrointestinal obstruction.
- Severe Hepatic Impairment: Due to the increased risk of acetaminophen toxicity.
- Acute Alcohol Intoxication: Or delirium tremens.
- Concomitant use with Monoamine Oxidase Inhibitors (MAOIs): Or within 14 days of discontinuing MAOI therapy, due to risk of serious adverse reactions, including serotonin syndrome.
Drug Interactions
Numerous medications can interact with Percocet, altering its effects or increasing the risk of adverse reactions.
| Category of Interacting Drug | Specific Examples | Potential Interaction |
| Oxycodone | Acetaminophen | Clinical Effect & Management