CHARCOT ARTHROPATHY: COMPREHENSIVE OVERVIEW
Charcot arthropathy (neuropathic osteoarthropathy) is a progressive, devastating, and potentially limb-threatening condition characterized by joint dislocation, pathologic fractures, and severe destruction of the pedal architecture. While historically associated with tabes dorsalis (neurosyphilis), the modern orthopedic landscape sees diabetes mellitus as the overwhelming primary etiology. The management of the Charcot foot remains one of the most formidable challenges in operative orthopedics, requiring a profound understanding of biomechanics, neurovascular pathology, and advanced reconstructive techniques.
PATHOPHYSIOLOGY AND BIOMECHANICS
The pathogenesis of Charcot arthropathy is multifactorial, traditionally understood through the synthesis of two classic theories: the Neurovascular (French) Theory and the Neurotraumatic (German) Theory. Modern evidence suggests that both mechanisms act synergistically in the diabetic foot.
The most plausible explanation for the development of neuropathic arthropathy begins with the loss of autonomic control of the vasculature. In a healthy patient, sympathetic tone regulates capillary flow. In patients with diabetic autonomic neuropathy, this sympathetic tone is lost, leading to profound vasodilation. Resting blood flow in patients with diabetic neuropathy may be up to five times normal values.
Arteriovenous shunting has been extensively documented in these feet. This high flow rate creates a hyperemic state that actively stimulates osteoclastic bone resorption, resulting in localized osteopenia.
Concurrently, the neurotraumatic mechanism takes effect. Combined with the somatosensory loss of pain and proprioception, multiple small mechanical insults—completely unrecognized by the patient—occur in this osteopenic bone. This sets the stage for rapid bony dissolution, periarticular fractures, and ligamentous failure. The loss of structural integrity is inevitably followed by a collapse deformity, most classically the "rocker-bottom" foot, where the midfoot arch collapses plantarward.
Clinical Pearl: Even minor trauma to the foot (e.g., mild sprains, contusions, or minor undisplaced fractures) can trigger the profound inflammatory cascade that initiates neuropathic skeletal changes in a patient with diabetes mellitus.
Recent molecular research has also implicated the RANKL/OPG (Receptor Activator of Nuclear Factor Kappa-B Ligand / Osteoprotegerin) signaling pathway. The acute inflammatory state in a Charcot event upregulates pro-inflammatory cytokines (TNF-α, IL-1, IL-6), which in turn upregulate RANKL expression, driving aggressive osteoclastic activity and rapid bone destruction.
CLINICAL EVALUATION AND DIAGNOSTIC DILEMMAS
The diagnosis of acute Charcot arthropathy is primarily clinical, supported by radiographic findings. The hallmark presentation of an acute (Eichenholtz Stage 0 or I) Charcot foot is a unilateral, erythematous, warm, and profoundly swollen foot.
Because these signs perfectly mimic acute infection, Charcot arthropathy is frequently misdiagnosed as cellulitis or osteomyelitis.
Differentiating Charcot Arthropathy from Infection
The diagnostic dilemma reaches its peak when Charcot arthropathy is accompanied by an open ulceration and possible underlying infection. Differentiating the two is critical, as the treatment pathways diverge significantly.
- The Elevation Test: Erythema, warmth, and swelling in an acute Charcot foot are largely driven by autonomic hyperemia. If the affected limb is elevated above the level of the heart for 5 to 10 minutes, the erythema and swelling will noticeably decrease. In contrast, the erythema associated with an active infection will persist despite elevation.
- Glycemic Control: With an active systemic infection, glucose control typically becomes highly erratic and difficult to manage due to insulin resistance driven by systemic inflammation. This is generally not the case in a patient with isolated Charcot arthropathy.
- Systemic Symptoms: A patient with acute Charcot arthropathy usually feels systemically well, lacking fevers, chills, or malaise, which may not be the case with a deep space infection.
ADVANCED IMAGING MODALITIES
Imaging studies are essential but can be confounding, as plain radiographs, CT scans, and standard bone scans can be positive in both Charcot arthropathy and osteomyelitis.
Magnetic Resonance Imaging (MRI)
MRI is the modality of choice for evaluating the diabetic foot, but differentiating Charcot from infection remains challenging.
* Indicators of Infection: The presence of a sinus tract, replacement of soft tissue fat, localized fluid collections, and extensive bone marrow abnormality (marrow edema that replaces normal fatty marrow) strongly indicate osteomyelitis.
* Indicators of Charcot: Thin rim enhancement of joint effusions, subchondral cysts, and the presence of intra-articular fracture fragments (debris) suggest a lack of infection and point toward neuropathic destruction.
Nuclear Medicine
White blood cell (WBC) scans (Indium-111 or Tc-99m HMPAO) can be highly helpful, especially when combined with sulfur colloid bone marrow imaging.
* If infection is present, the tagged white cells will accumulate at the site, but the sulfur colloid scan will be negative (cold) because normal bone marrow activity is depressed by the localized infection.
* Pitfall: It takes approximately 1 week for the sulfur colloid scan to become negative after the onset of infection. Concordant uptake on both scans suggests Charcot arthropathy.
Positron emission tomography (PET) can be very sensitive and specific for differentiating the two conditions, but this test is not widely available in all orthopedic centers.
Percutaneous Bone Biopsy
Percutaneous bone biopsy has long been recommended as the gold standard to differentiate Charcot arthropathy from osteomyelitis. However, its reliability is not absolute. In recent studies where percutaneous bone biopsies were performed in diabetic patients with suspected osteomyelitis, authors concluded that approximately 25% of patients who have a negative percutaneous bone biopsy will ultimately develop or harbor osteomyelitis. Therefore, biopsy results must be correlated with clinical and advanced imaging findings.
CONSERVATIVE MANAGEMENT: OFF-LOADING PROTOCOLS
The absolute cornerstone of managing acute (Eichenholtz Stage I) Charcot arthropathy is immediate and strict off-loading. The goal is to arrest the inflammatory cycle, prevent further microtrauma, and allow the osteopenic bone to consolidate without progressing to a severe collapse deformity.
Total Contact Casting (TCC)
The Total Contact Cast is the gold standard for off-loading the acute Charcot foot. By intimately conforming to the contours of the foot and lower leg, the TCC redistributes plantar pressures away from bony prominences (such as a collapsed cuboid or navicular) and transfers the load to the entire surface area of the lower leg.
Step-by-Step TCC Application:
-
Skin Preparation and Stockinette: The foot is inspected, and any minor wounds are dressed. A protective stockinette is applied smoothly over the foot and leg to prevent wrinkles that could cause pressure necrosis.

-
Foam Padding Preparation: Specialized foam padding is measured and cut to protect the bony prominences of the malleoli, the anterior tibia, and the toes. The adhesive backing is peeled away for application.
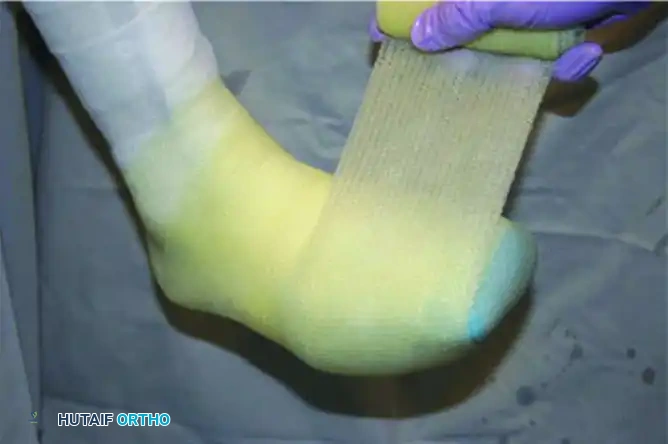
-
Applying Foam to the Foot: The foam is carefully molded around the ankle and foot, ensuring no tight constricting bands are formed.
-
Plantar Sole Pad: A custom-cut foam or felt sole pad is applied to the plantar aspect of the foot. This is critical for cushioning the collapsed midfoot and preventing ulceration during incidental weight-bearing.

-
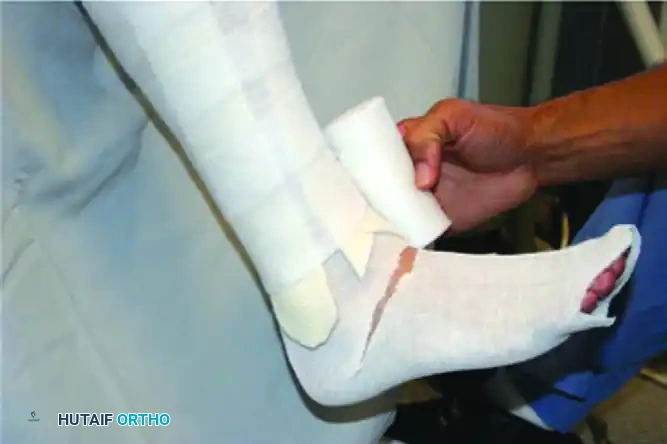
Applying the Cast Material: Fiberglass or plaster cast rolls are applied circumferentially. The ankle is held in neutral (90 degrees) if possible, taking care not to force correction that might cause skin tension.

-
Wrapping and Molding: The cast is wrapped and meticulously molded to the contours of the foot, particularly supporting the medial longitudinal arch.
-
Integration of the Metal Stirrup: A metal stirrup is applied to the total contact cast. This device takes pressure off the plantar surface of the foot and transmits the axial load directly to the shank of the cast, bypassing the fragile midfoot architecture.
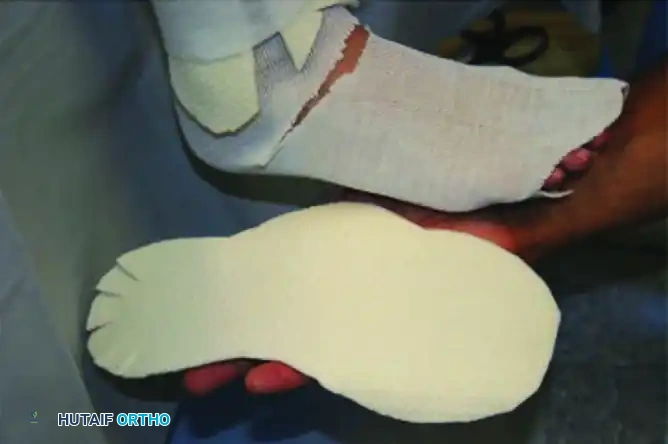
FIGURE 85-9 Metal stirrup applied to total contact cast takes pressure off plantar surface of foot and transmits it to shank of cast.
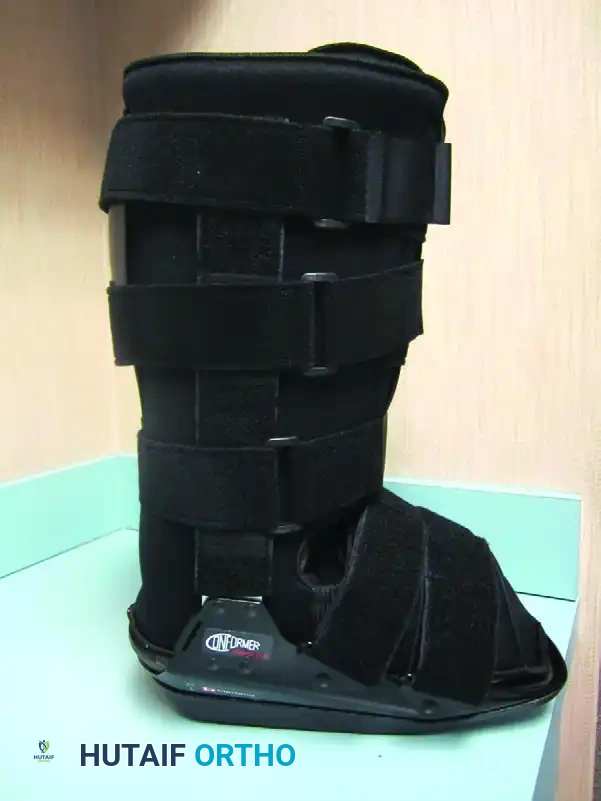
Removable Diabetic Boots (CROW)
As the acute phase resolves (transitioning to Eichenholtz Stage II/III), or in patients who cannot tolerate a TCC, a Charcot Restraint Orthotic Walker (CROW) or a specialized removable diabetic boot can be utilized.
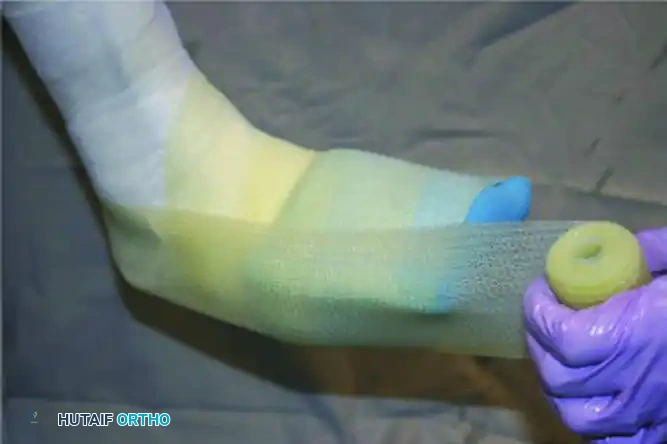

FIGURE 85-10 Removable diabetic boot can be used as alternative to total contact cast. A, Exterior. B, Interior.
These boots feature a rigid exterior shell to prevent sheer forces and a highly customized, multi-density foam interior to accommodate deformities. While effective, their removable nature introduces the risk of patient non-compliance.
SURGICAL MANAGEMENT: OPERATIVE ORTHOPAEDICS
Surgical intervention in Charcot arthropathy is technically demanding and carries a high complication rate. It is generally reserved for patients who have failed conservative management or present with limb-threatening deformities.
Indications for Surgery
- Severe, unbraceable deformity (e.g., rigid rocker-bottom foot).
- Recurrent or recalcitrant plantar ulceration due to bony prominences.
- Gross clinical instability preventing ambulation.
- Impending skin compromise or deep infection requiring debridement.
Surgical Warning: Surgery is generally contraindicated during the acute, highly inflammatory fragmentation phase (Eichenholtz Stage I) due to the extreme risk of hardware failure in hyperemic, osteopenic bone. The exception is an isolated exostectomy for an impending ulcer or incision and drainage for an active infection. Reconstructive arthrodesis should be delayed until the coalescence phase (Stage II or III).
1. Exostectomy
For stable feet with a localized bony prominence (typically the plantar-medial aspect of the medial cuneiform or the plantar-lateral cuboid) causing recurrent ulceration, a simple exostectomy is highly effective.
* Approach: A medial or lateral incision is made just dorsal to the transition line of the plantar skin.
* Technique: The prominent bone is resected using an oscillating saw or osteotome until the plantar surface is completely flat. The cortical edges are rasped smooth.
* Postoperative: The patient is kept non-weight-bearing until the incision heals, followed by custom orthotics.
2. Achilles Tendon Lengthening (TAL) or Gastrocnemius Recession
Equinus contracture is universally present in midfoot Charcot arthropathy. A tight Achilles tendon acts as a deforming force, driving the forefoot into the ground and exacerbating midfoot collapse.
* Technique: A percutaneous triple hemisection (Hoke technique) of the Achilles tendon or an open Strayer gastrocnemius recession is performed.
* Biomechanics: This reduces forefoot plantar pressures by up to 30%, significantly reducing the risk of recurrent midfoot ulceration and protecting midfoot arthrodesis constructs.
3. Midfoot and Hindfoot Arthrodesis (Superconstructs)
When gross instability or severe deformity is present, a major reconstructive arthrodesis is required. Because of the poor bone quality and lack of patient protective sensation, standard AO fixation principles frequently fail. Surgeons must employ the concept of "Superconstructs" (as described by Sammarco).
Principles of Superconstructs:
1. Extend Fusion Beyond the Zone of Injury: Arthrodesis must extend into normal, unaffected joints proximally and distally.
2. Resection of Bone: Adequate bone resection must be performed to shorten the extremity slightly, reducing tension on the soft tissue envelope.
3. Strongest Implant Possible: Use implants that maximize biomechanical strength (e.g., large diameter intramedullary beams, heavy locking plates).
4. Positioning on the Tension Side: Implants should be applied to the plantar (tension) aspect of the foot whenever possible.
Surgical Technique: Intramedullary Beaming
* Positioning: Supine with a bump under the ipsilateral hip.
* Approach: Medial utility incision for the medial column (talonavicular, naviculocuneiform, tarsometatarsal joints).
* Preparation: Joint surfaces are aggressively denuded of cartilage and sclerotic bone down to bleeding cancellous bone. Deformity is corrected manually.
* Fixation: A large-diameter (e.g., 6.5mm or 7.0mm) solid intramedullary bolt or "beam" is introduced from the head of the first metatarsal, driven proximally through the cuneiform and navicular, and anchored deep into the body of the talus. A second beam may be placed through the 4th metatarsal into the calcaneus to stabilize the lateral column.
* Augmentation: Plantar locking plates can be added to neutralize bending moments.
4. Circular External Fixation (Ilizarov / Taylor Spatial Frame)
In cases of active ulceration, osteomyelitis, or bone quality so poor that internal hardware would immediately fail, circular external fixation is the treatment of choice.
* Biomechanics: Tensioned wires (1.8mm) and half-pins provide rigid stability while allowing access to wounds. The frame acts as a load-sharing device, transmitting forces from the tibia directly to the ground, completely off-loading the foot.
* Technique: A tibial block is constructed with two rings. A foot plate is attached using crossed olive wires through the calcaneus and midfoot/forefoot. Gradual deformity correction can be achieved using hexapod struts.
POSTOPERATIVE PROTOCOLS AND COMPLICATIONS
The postoperative management of the Charcot reconstruction is as critical as the surgery itself.
- Weight-Bearing Status: Patients must remain strictly non-weight-bearing (NWB) for a minimum of 8 to 12 weeks. Premature weight-bearing is the leading cause of catastrophic hardware failure.
- Immobilization: The limb is maintained in a well-padded splint, transitioning to a fiberglass cast once incisions are fully healed.
- Transition: After radiographic evidence of consolidation (often taking 3 to 6 months), the patient is transitioned to a CROW boot, and eventually to custom-molded extra-depth diabetic footwear with rigid rocker soles.
- Complications: Surgeons must counsel patients extensively regarding the high risk of complications. Deep infection, hardware breakage, nonunion, and adjacent joint disease are common. Ultimately, despite heroic reconstructive efforts, the risk of major lower extremity amputation remains significant in this vulnerable population.
By adhering to strict biomechanical principles, utilizing superconstructs, and enforcing rigorous postoperative off-loading, the orthopedic surgeon can successfully salvage the limb and restore a plantigrade, braceable foot in the patient with Charcot arthropathy.
