INTRODUCTION TO CANCELLOUS INSERT GRAFTS
The management of diaphyseal bone defects and recalcitrant nonunions remains a formidable challenge in orthopedic surgery. While modern techniques such as vascularized bone transfers and bone transport via distraction osteogenesis are available for massive defects, smaller gaps require a more streamlined, biologically robust approach. Nicoll described a highly effective technique for bridging gaps in long bones utilizing solid blocks of cancellous bone, combined with rigid internal fixation using metal plates.
This procedure, widely known as the Nicoll cancellous insert graft, is particularly useful in patients with segmental bone defects measuring less than 2.5 cm in length. The biological rationale relies on the superior osteogenic and osteoinductive properties of autologous cancellous bone compared to cortical grafts. The porous architecture of cancellous bone provides an ideal osteoconductive scaffold, allowing for rapid revascularization and creeping substitution.
Clinical Pearl: While Nicoll originally utilized ordinary neutralization plates and wedged the graft into position, contemporary orthopedic principles dictate that dynamic compression plates (DCP) or locking compression plates (LCP) are vastly preferable. Compression enhances the stability of the construct and promotes primary bone healing across the graft-host interfaces.
INDICATIONS AND PREOPERATIVE PLANNING
Patient Selection
The primary indication for a cancellous insert graft is an aseptic, atrophic, or oligotrophic nonunion of a long bone with a structural defect of less than 2.5 cm. It is frequently employed in the radius, ulna, clavicle, and occasionally the tibia or humerus.
Contraindications include:
* Active osteomyelitis or infected nonunions (which require staged management with antibiotic spacers prior to grafting).
* Defects exceeding 2.5 cm (which typically require structural cortical grafts, vascularized fibular grafts, or Ilizarov bone transport).
* Severe soft tissue compromise lacking adequate vascularized muscle coverage.
Preoperative Optimization
A thorough metabolic workup is essential for any patient presenting with a nonunion. Vitamin D levels, thyroid function, and nutritional markers should be optimized. Smoking cessation is mandatory, as nicotine significantly impairs microvascular ingrowth and osteogenesis, exponentially increasing the risk of graft failure.
Preoperative imaging should include orthogonal radiographs of the affected limb. Computed Tomography (CT) is highly recommended to accurately quantify the volumetric size of the defect and assess the geometry of the sclerotic bone ends that will require resection.
SURGICAL ANATOMY: THE ILIAC CREST DONOR SITE
The anterolateral aspect of the iliac crest is the premier donor site for harvesting large, solid blocks of cancellous bone. The crest is superficial and easily palpable.
Key anatomical considerations include:
* Muscular Attachments: The external oblique, internal oblique, and transversus abdominis attach to the superior margin. The tensor fasciae latae and gluteus medius originate from the outer table, while the iliacus originates from the inner table.
* Neurological Structures: The lateral femoral cutaneous nerve exits the pelvis medial to the anterior superior iliac spine (ASIS). Incisions must remain at least 2 to 3 cm posterior to the ASIS to avoid iatrogenic injury, which can result in meralgia paresthetica. The cluneal nerves cross the posterior iliac crest and must be respected if a posterior harvest is chosen.
SURGICAL TECHNIQUE: GRAFT HARVEST
The harvest of a structurally sound cancellous block requires meticulous technique to preserve the integrity of the graft while minimizing donor site morbidity.
Step 1: Exposure of the Iliac Crest
Position the patient supine with a bump under the ipsilateral hip to elevate the pelvis.
1. Make an incision along the contour of the iliac crest, beginning 3 cm posterior to the ASIS to protect the lateral femoral cutaneous nerve.
2. Deepen the incision through the subcutaneous tissue to the fascia.
3. Incise the periosteum directly over the crest.
4. Expose the crest via subperiosteal dissection. Carefully reflect the muscular attachments of the inner (medial) and outer (lateral) tables using a Cobb elevator to expose the cortical bone.
Step 2: Creating the Cortical Window
- Using an oscillating saw or a sharp, thin osteotome, remove the superior cortex of the iliac crest. This creates a "trapdoor" or "lid."
- Reflect the medial and lateral cortical walls slightly to fully expose the rich, underlying cancellous bone bed.
Step 3: Harvesting the Cancellous Block
- With a thin, sharp osteotome, carefully outline and remove a solid block of cancellous bone.
- The harvested block should be approximately 1.3 cm longer than the estimated length required for the recipient defect.
- It is entirely feasible to obtain a graft measuring up to 7.5 cm in length, 2 cm in width, and 1.3 cm in thickness from a well-developed adult pelvis.
Surgical Warning: To strengthen a particularly large graft and prevent it from crushing under the axial load of a compression plate, it is highly recommended to retain one cortical plate (usually the inner or outer table) attached to the cancellous block.
Step 4: Closure of the Donor Site
- Once the graft is harvested, achieve meticulous hemostasis using bone wax or topical hemostatic agents (e.g., Gelfoam, Surgicel) within the defect.
- Replace the superior cortical "lid" over the defect. Alternatively, this superior cortex can be retained for use as an adjunctive onlay graft at the nonunion site.
- Close the periosteum and fascial layers securely with heavy absorbable sutures to prevent herniation. Close the subcutaneous tissue and skin in a standard layered fashion.
SURGICAL TECHNIQUE: RECIPIENT SITE PREPARATION AND FIXATION
The success of the Nicoll technique hinges entirely on the radical debridement of the nonunion site and the achievement of absolute mechanical stability.
Step 1: Exposure and Debridement
- Expose the nonunion through an extensile, internervous longitudinal incision appropriate for the specific long bone (e.g., Henry approach for the volar radius).
- Radically excise the pseudarthrosis. Remove all avascular scar tissue and interposed fibrous material.
- Resect all sclerotic, eburnated bone from the ends of the proximal and distal fragments. You must cut back to healthy, bleeding bone—often referred to as the "paprika sign."
- Freshen the surrounding muscle bed by excising fibrotic tissue, ensuring the graft will be enveloped by a highly vascularized soft-tissue envelope.
Step 2: Graft Preparation and Insertion
- Measure the exact dimensions of the prepared bony gap using inside calipers.
- Using a scalpel or a fine rongeur, meticulously trim the harvested cancellous block to match the defect.
- The goal is an absolute press-fit. The graft should wedge tightly between the freshened bone ends.
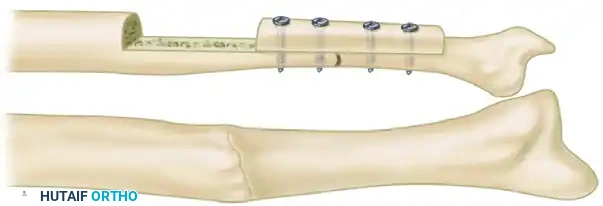
Step 3: Plating and Compression
- Align the bone fragments anatomically, correcting any angular or rotational deformities.
- Apply a heavy-duty metal plate (preferably a dynamic compression plate or locking compression plate) across the defect.
- Secure the plate to the host bone fragments. Utilize the compression holes in the plate or an articulated tension device to apply axial compression across the host-graft-host interfaces.
- If the superior cortex of the ilium was harvested, it can be used as an adjunctive onlay graft spanning the defect opposite the plate. Tie it securely in place with strong absorbable sutures or cerclage.
ALTERNATIVE GRAFTING TECHNIQUES FOR COMPLEX DEFECTS
While the Nicoll cancellous insert graft is ideal for defects under 2.5 cm, larger or more complex defects require alternative reconstructive strategies. Understanding these historical and contemporary techniques is crucial for the advanced orthopedic surgeon.
Boyd Dual Onlay Grafts
For highly recalcitrant nonunions, particularly those involving congenital pseudarthrosis of the tibia or severe atrophic nonunions, the Boyd dual onlay graft technique provides immense mechanical stability and biological stimulation. This technique utilizes two cortical grafts applied to opposing sides of the host bone, effectively creating a biological vise.

FIGURE 59-5 Boyd dual onlay grafts. A, Before surgery. B, After application of grafts and fusion of proximal tibiofibular joint. SEE TECHNIQUE 59-1.
The dual grafts are typically harvested from the tibia and are secured with transfixing screws that pass through both grafts and the intervening host bone. The space between the grafts is densely packed with endosteum and cancellous bone to promote rapid consolidation.
Gill Massive Sliding Graft
The Gill massive sliding graft is an elegant autologous technique primarily used for diaphyseal nonunions where local bone stock is adequate but bridging is required.

FIGURE 59-6 Gill massive sliding graft. SEE TECHNIQUE 59-3.
In this procedure, a large cortical window is cut from the longer fragment adjacent to the nonunion. This massive cortical slab is then advanced (slid) across the nonunion site to bridge the defect and is secured with screws. The resulting empty trough in the donor segment is subsequently filled with cancellous bone.
Whole Fibular Transplant for Massive Defects
When dealing with massive bone loss—such as those resulting from high-velocity ballistic trauma, shotgun wounds, or wide tumor resections—cancellous inserts are insufficient. In these scenarios, a whole fibular transplant (either non-vascularized or as a free vascularized tissue transfer) is indicated to span the defect.
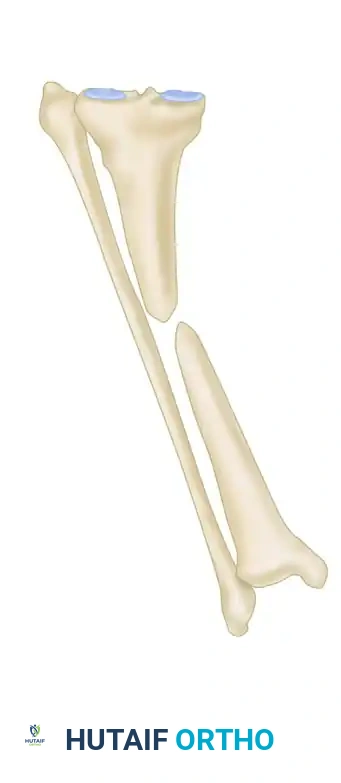
FIGURE 59-7 Bridging of bone defect with whole fibular transplant. A, Defect in radius was caused by shotgun wound.
The fibula provides excellent cortical strength and can bridge gaps exceeding 10 cm. In the upper extremity, such as the radius, it restores the structural strut necessary for forearm rotation and wrist stability.

FIGURE 59-7 B and C, Ten months after defect was spanned by whole fibular transplant, patient had 25% range of motion in wrist, 50% pronation and supination, and 80% use of fingers. SEE TECHNIQUE 59-4.

Radiographic progression demonstrating successful incorporation and hypertrophy of the fibular strut graft.
POSTOPERATIVE CARE AND REHABILITATION
The postoperative protocol must balance the need for mechanical protection of the graft with the prevention of adjacent joint stiffness.
- Immobilization: Historically, a well-molded cast was applied and worn for 2 to 3 months, depending on the location of the fracture, the size of the bone, and the radiographic progress of union.
- Modern Modifications: With the advent of modern locking plate technology, absolute rigid fixation is often achieved intraoperatively. In compliant patients, a removable thermoplastic splint may replace prolonged cast immobilization, allowing for early, protected passive range of motion (ROM) of adjacent joints to prevent arthrofibrosis.
- Weight-Bearing: For lower extremity grafts (e.g., tibia), patients must remain strictly non-weight-bearing until radiographic evidence of bridging callus or graft incorporation is visible at both the proximal and distal host-graft interfaces. This typically takes 8 to 12 weeks.
- Radiographic Monitoring: Serial orthogonal radiographs should be obtained at 2, 6, 12, and 24 weeks postoperatively. The surgeon should look for blurring of the osteotomy lines, indicating creeping substitution and successful biological incorporation of the cancellous block.
COMPLICATIONS AND PITFALLS
Donor Site Morbidity
The iliac crest harvest site is notorious for postoperative pain, which frequently exceeds the pain at the recipient site. Meticulous surgical technique, avoiding excessive traction on the surrounding musculature, and continuous local anesthetic infiltration (e.g., bupivacaine pain pumps) can mitigate this. Hematoma formation is a risk; thus, careful hemostasis and occasionally a closed suction drain are warranted.
Graft Resorption and Failure
If the nonunion site is inadequately debrided of avascular tissue, or if the fixation is mechanically unstable, the cancellous graft will fail to revascularize. This leads to graft resorption, hardware failure (plate breakage or screw pullout), and recurrence of the nonunion.
Infection
Infection is a catastrophic complication in bone grafting. Prophylactic intravenous antibiotics should be administered prior to tourniquet inflation. If a postoperative deep infection occurs, it typically necessitates aggressive surgical debridement, removal of the bone graft, and placement of an antibiotic-impregnated cement spacer, effectively resetting the reconstructive timeline.
CONCLUSION
The Nicoll cancellous insert graft remains a foundational technique in the armamentarium of the orthopedic surgeon. By strictly adhering to the principles of radical debridement, precise graft harvesting, press-fit insertion, and rigid compressive fixation, surgeons can achieve high union rates in challenging diaphyseal defects. While massive bone loss requires more complex reconstructive ladders such as fibular transplants or dual onlay grafts, the biological superiority of the solid cancellous block makes it the gold standard for defects under 2.5 cm.
