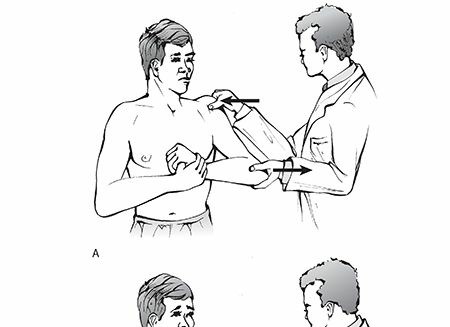
Anterior Glenohumeral Dislocation: Signs, Causes, and Diagnosis
Introduction & Epidemiology
Anterior glenohumeral dislocation represents the predominant pattern of shoulder instability, accounting for approximately 96% of all shoulder dislocations. This high incidence underscores its significance in orthopedic practice. The epidemiology demonstrates a bimodal distribution, with a peak incidence in young, active males (15-25 years old) involved in contact sports, and a secondary peak in older individuals, often associated with falls and higher rates of concomitant rotator cuff tears or fractures. The annual incidence is estimated to be 17 to 23.9 per 100,000 person-years, with a lifetime prevalence as high as 2%. The economic and functional burden, particularly due to recurrent instability, is substantial, often necessitating surgical intervention.
The chronicity of dislocation is a critical factor influencing management. Acute dislocations are those presenting within days of injury, while chronic or "locked" dislocations may have existed for weeks or months, often complicating reduction and increasing the risk of associated injuries. Understanding the pattern of recurrence, including the number of episodes and inciting events, is paramount for guiding treatment decisions.
Surgical Anatomy & Biomechanics
The glenohumeral joint is inherently unstable, prioritizing mobility over stability. Its stability is conferred by a complex interplay of static and dynamic stabilizers.
Static Stabilizers
- Bony Anatomy: The glenoid fossa is a shallow, pear-shaped articular surface, typically retroverted by 0-10 degrees, with an average depth of 2.5 mm. The humeral head, significantly larger than the glenoid, articulates with only 25-30% of the glenoid surface at any given time. Abnormal glenoid version, hypoplasia, or significant bony defects (e.g., osseous Bankart lesions) predispose to instability.
- Glenoid Labrum: A fibrocartilaginous ring that deepens the glenoid fossa by approximately 50%, increasing glenoid depth by 5-9 mm. The anterior-inferior labrum is critical for resisting anterior translation of the humeral head.
-
Capsuloligamentous Complex:
-
Glenohumeral Ligaments (GHLs):
These are thickenings of the anterior joint capsule.
- Inferior Glenohumeral Ligament Complex (IGHLC): The primary static restraint to anterior translation when the arm is abducted and externally rotated. It consists of anterior and posterior bands and an axillary pouch. The anterior band of the IGHLC is most crucial in resisting anterior dislocation.
- Middle Glenohumeral Ligament (MGHL): A secondary restraint to anterior translation, particularly when the arm is in 45-60 degrees of abduction and external rotation.
- Superior Glenohumeral Ligament (SGHL): Functions primarily in adduction and inferior translation, contributing to the rotator interval.
- Capsule: The fibrous capsule is redundant, allowing for wide ranges of motion, but provides little inherent stability unless taut.
-
Glenohumeral Ligaments (GHLs):
These are thickenings of the anterior joint capsule.
Dynamic Stabilizers
- Rotator Cuff Muscles: The supraspinatus, infraspinatus, teres minor, and subscapularis muscles provide dynamic compression and centralization of the humeral head within the glenoid fossa, particularly during active motion. The subscapularis is especially important in resisting anterior and superior translation.
- Scapular Stabilizers: Muscles like the serratus anterior, rhomboids, and trapezius contribute to scapulothoracic rhythm, optimizing glenohumeral mechanics.
Biomechanical Considerations in Anterior Dislocation
Anterior glenohumeral dislocation commonly results from an excessive force that overwhelms these stabilizers, typically with the arm in abduction, external rotation, and extension. This position places the anterior band of the IGHLC under maximal tension, predisposing it to avulsion from the glenoid rim (Bankart lesion) or elongation.

Concomitant osseous lesions are critical to recognize:
*
Bankart Lesion:
An avulsion of the anterior-inferior labroligamentous complex from the glenoid rim. Osseous Bankart lesions involve a fracture of the anterior glenoid rim, significantly reducing the effective glenoid arc.
*
Hill-Sachs Lesion:
A compression fracture of the posterior-superior aspect of the humeral head, occurring as the humeral head impacts the anterior glenoid rim during dislocation.

The size and "engagement" of the Hill-Sachs lesion, in conjunction with glenoid bone loss, are crucial for assessing the risk of recurrence and guiding surgical strategy (the "glenoid track" concept). An "off-track" lesion occurs when the Hill-Sachs defect extends medial to the glenoid track, indicating a higher risk of engagement with the glenoid rim during abduction and external rotation.

Mechanism of Injury
Anterior glenohumeral dislocation typically occurs as a result of trauma, either through direct or indirect forces.
Indirect Trauma
The most common mechanism involves indirect trauma to the upper extremity with the shoulder in a position of
abduction, extension, and external rotation
. This position levers the humeral head out of the glenoid fossa anteriorly. Examples include:
* Falling on an outstretched arm.
* Sporting injuries (e.g., throwing motion in baseball, tackling in football, falling during skiing).
* Motor vehicle accidents where the arm is forcefully pushed backward.
Direct Trauma
Direct, anteriorly directed impact to the posterior shoulder (e.g., a direct blow to the posterior aspect of the humeral head or scapula) can also produce an anterior dislocation by pushing the humeral head anteriorly. This mechanism is less common than indirect trauma.
Other Mechanisms
- Convulsive Mechanisms and Electrical Shock: While these typically produce posterior shoulder dislocations due to unopposed internal rotation and adduction from strong muscle contractions, severe cases or specific arm positions can also result in an anterior dislocation.
- Recurrent Instability: In individuals with pre-existing congenital or acquired capsular laxity, or those with volitional (often psychological) mechanisms of dislocation, anterior dislocation may occur with minimal or even no discernible trauma. This can be due to global ligamentous laxity or attenuation of the anterior capsuloligamentous structures from prior episodes.
Associated Injuries Based on Mechanism
The specific mechanism and forces involved often dictate the pattern of associated injuries:
* High-energy trauma in younger individuals is more likely to result in significant labral tears (Bankart lesions, ALPSA lesions), Hill-Sachs lesions, and sometimes glenoid rim fractures.
* In older individuals, even low-energy falls can lead to rotator cuff tears, particularly the subscapularis, due to age-related degenerative changes. Greater tuberosity fractures are also more common in this demographic.
* Chronic or recurrent dislocations can lead to progressive bone loss from the anterior glenoid and posterior humeral head, increasing the risk of subsequent dislocations and complicating surgical repair.
Clinical Evaluation
A thorough clinical evaluation is paramount for accurate diagnosis and management planning.
History
- Nature of the Trauma: Ascertain the mechanism (indirect vs. direct), direction of force, and arm position at the time of injury (e.g., abduction, external rotation). This guides suspicion for associated injuries.
- Chronicity of Dislocation: Acute (first-time vs. recurrent), subacute, or chronic (locked). This impacts reduction techniques and urgency.
- Pattern of Recurrence: For recurrent instability, inquire about the number of previous dislocations, the level of trauma required to dislocate, ease of reduction (spontaneous, patient-assisted, medical intervention), and intervening symptomatic episodes of subluxation.
- Associated Symptoms: Pain severity, paresthesias (suggesting nerve involvement), weakness.
- Contralateral Shoulder History: History of instability or laxity in the unaffected shoulder can indicate generalized ligamentous laxity.
- Medical History: Seizure disorders, Ehlers-Danlos syndrome, or other connective tissue disorders can predispose to instability.
Physical Examination
The physical examination in an acute anterior glenohumeral dislocation reveals characteristic findings:
*
Patient Presentation:
The patient typically presents with the injured shoulder held in slight abduction and external rotation, often supporting the arm with the contralateral hand. Movement is severely restricted and extremely painful, often accompanied by muscular spasm.

*
Inspection:
*
Squaring of the Shoulder:
This classic sign is due to the loss of the normal rounded contour of the deltoid, created by the humerus displacing inferiorly and anteriorly. The acromion appears relatively prominent.
*
Hollow Beneath the Acromion:
A palpable hollow or sulcus beneath the acromion posteriorly is often evident due to the absence of the humeral head in its normal position.
*
Palpable Mass Anteriorly:
The humeral head may be palpable anteriorly, inferior to the coracoid process, particularly in slender individuals.
*
Palpation:
Tenderness over the anterior shoulder joint. Palpation can confirm the presence of the humeral head anteriorly.
*
Range of Motion:
Grossly restricted and painful active and passive range of motion. Any attempt at internal rotation or adduction is met with significant resistance and pain.
*
Neurovascular Examination:
A meticulous neurovascular examination is critical, both pre- and post-reduction.
*
Axillary Nerve (C5-C6):
The most commonly injured nerve in anterior shoulder dislocations, with reported incidence rates varying from 5% to 55%. Assess deltoid motor function (shoulder abduction) and sensation over the regimental badge area (lateral aspect of the upper arm).
*
Musculocutaneous Nerve (C5-C7):
Assess biceps motor function (elbow flexion, forearm supination) and sensation over the lateral forearm.
*
Median, Ulnar, Radial Nerves:
Assess motor and sensory function in the forearm and hand.
*
Vascular Assessment:
Palpate radial, ulnar, and brachial pulses. Assess capillary refill and skin color/temperature to rule out brachial artery injury, which is rare but limb-threatening.

Imaging Studies
Appropriate imaging is essential for confirming the diagnosis, identifying associated injuries, and guiding management.
Radiographs
Standard radiographic series include:
*
Anteroposterior (AP) View:
Often reveals the humeral head inferior and medial to the glenoid.
*
Scapular Y View:
Considered the best view for distinguishing anterior from posterior dislocations. In an anterior dislocation, the humeral head is displaced anterior to the glenoid and coracoid process.

*
Axillary View (Modified West Point or Velpeau Axillary):
Crucial for confirming the direction of dislocation, assessing glenoid rim fractures (osseous Bankart), and visualizing Hill-Sachs lesions. Obtaining this view can be challenging and painful in an acute setting; a Velpeau axillary view may be better tolerated.

*
Stryker Notch View:
Specifically designed to visualize Hill-Sachs lesions by demonstrating a defect in the posterolateral humeral head.
*
Garth View (Apical Oblique):
Another view to assess glenoid bone loss and the congruity of the humeral head.
Post-reduction radiographs are mandatory to confirm successful reduction and rule out iatrogenic fractures or persistent subluxation.
Advanced Imaging
-
Magnetic Resonance Imaging (MRI):
- Indications: Suspected soft tissue injuries (labral tears, capsular avulsions, rotator cuff tears), especially in recurrent dislocations or when pain/dysfunction persists after reduction.
-
Findings:
Clearly visualizes Bankart lesions (fibrous and osseous), ALPSA (Anterior Labroligamentous Periosteal Sleeve Avulsion) lesions, HAGL (Humeral Avulsion of the Glenohumeral Ligament) lesions, rotator cuff tears, and Hill-Sachs lesions. MRI arthrography can enhance visualization of these structures.


-
Computed Tomography (CT) Scan:
- Indications: Primarily indicated when significant bone loss from the glenoid or humeral head is suspected, particularly in recurrent dislocations, pre-operative planning for revision surgery, or when radiographs are inconclusive regarding bony lesions.
-
Findings:
Provides detailed assessment of glenoid bone loss (critical bone loss is typically >20-25% of the inferior glenoid diameter), Hill-Sachs lesion size and location, and glenoid version. 3D reconstructions are invaluable for surgical planning.


Indications & Contraindications
Management of anterior glenohumeral dislocation spans a spectrum from non-operative rehabilitation to complex open or arthroscopic surgical reconstructions. The decision-making process is individualized, considering patient age, activity level, recurrence risk factors, and the presence of significant associated pathologies.
Indications for Operative vs. Non-Operative Management
| Factor/Condition | Non-Operative Management Indications | Operative Management Indications |
|---|---|---|
| First-time Dislocation | * Older patients (>40-50 years old), especially with low-demand activity. * Absence of significant osseous lesions (glenoid bone loss <15-20%, non-engaging Hill-Sachs). * Young, active patients (<25-30 years old), particularly athletes involved in contact or overhead sports (high recurrence rates). * Concomitant significant injuries: Large, displaced Bankart lesions (soft tissue or osseous), significant Hill-Sachs lesions (engaging, "off-track"), symptomatic rotator cuff tears, significant glenoid bone loss (>15-20% of glenoid diameter). * Patients with documented generalized ligamentous laxity or multiligamentous injury. | |
| Recurrent Dislocation | * Rarely indicated. May be considered in very low-demand, elderly patients with stable reductions and minimal functional impairment, or in those with significant medical comorbidities precluding surgery. * Primary indication for surgery in most cases. * Functional instability (recurrent dislocations or symptomatic subluxations affecting daily activities or sport). * Progressive bone loss with each episode. | |
| Associated Pathologies | * Small, non-displaced Hill-Sachs lesions that are "on-track" (not engaging). * Minimal or no glenoid bone loss. * Significant glenoid bone loss: Typically >15-20% of the inferior glenoid diameter (often requires bone augmentation procedures like Latarjet). * Engaging Hill-Sachs lesion (off-track): May require Remplissage in addition to Bankart repair, or glenoid bone block. * Large, displaced rotator cuff tears: Often require repair. | |
| Patient Factors | * Sedentary lifestyle. * Significant medical comorbidities that increase surgical risk (ASA III/IV), where non-operative management offers acceptable functional outcome. * High-demand activity, competitive athletes, military personnel. * Patients who cannot tolerate immobilization or functional limitations from repeated dislocations. | |
| Failed Non-Operative Tx | * Initial management for low-risk, first-time dislocations. * Recurrence after adequate non-operative rehabilitation. |
Contraindications
Absolute contraindications to surgery are rare and typically relate to the patient's overall health status:
* Acute infection in the surgical field.
* Severe medical comorbidities precluding safe anesthesia and surgery (e.g., uncontrolled cardiac disease, severe coagulopathy).
* Non-compliance with post-operative rehabilitation protocols.
Relative contraindications may include:
* Severe psychiatric illness affecting compliance.
* Extreme generalized ligamentous laxity (may require more extensive capsular plication or bone block procedures).
* Significant active shoulder arthritis (may require arthroplasty rather than instability repair).
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning and appropriate patient positioning are critical for successful surgical outcomes in anterior glenohumeral instability.
Pre-Operative Planning
-
Comprehensive Imaging Review:
- Review all radiographs, MRI, and especially CT scans with 3D reconstructions. Quantify glenoid bone loss using methods like the "perfect circle" technique or "anterior-inferior glenoid line" method. Assess the size, location, and "on-track" vs. "off-track" nature of any Hill-Sachs lesion.
- Identify concomitant pathologies such as rotator cuff tears, biceps pathology, or chondral damage.
-
Procedure Selection:
Based on the clinical assessment and imaging, determine the most appropriate surgical technique:
- Arthroscopic Bankart Repair: Indicated for soft tissue Bankart lesions, minimal glenoid bone loss (<15-20%), and "on-track" Hill-Sachs lesions.
- Arthroscopic Bankart Repair with Remplissage: For soft tissue Bankart lesions with an "off-track" Hill-Sachs lesion.
- Open Bankart Repair: Historically the gold standard, now largely reserved for complex cases or failed arthroscopic repairs.
- Bone Augmentation Procedures (Latarjet/Bristow): Indicated for significant glenoid bone loss (>20-25%), engaging "off-track" Hill-Sachs lesions with substantial bone loss, failed previous soft tissue repairs, or high-demand overhead athletes with significant risk factors for recurrence.
- Capsular Shift/Plication: For global laxity or multidirectional instability (MDI) with an anterior component.
- Equipment and Implant Selection: Ensure availability of appropriate arthroscopic equipment (scopes, pumps, shavers, radiofrequency probes), suture anchors (bioabsorbable vs. non-absorbable, PEEK), sutures, knot-tying devices, and, for bone block procedures, specific Latarjet instrumentation, screws, and potentially specialized drills.
- Anesthesia: General anesthesia is typically employed. Regional nerve blocks (interscalene brachial plexus block) are often used as an adjunct for post-operative pain control.
Patient Positioning
Two primary positions are utilized for shoulder arthroscopy and open instability repair:
-
Beach Chair Position:
- Advantages: Allows for easy conversion to an open procedure if needed, anatomical orientation similar to physical exam, ability to assess range of motion throughout the procedure, comfortable for the anesthesiologist to manage the airway.
- Setup: The patient is placed in a semi-recumbent position (30-70 degrees of trunk elevation) on a specialized beach chair table. The head is secured in a well-padded headrest, angled slightly away from the operative shoulder. The operative arm is draped free. The non-operative arm is tucked or placed on an arm board. The hip and knee joints are flexed to improve venous return and reduce pressure on the calves.
-
Key Considerations:
Careful padding of pressure points (occiput, elbows, sacrum). Hypotensive anesthesia is often employed to reduce bleeding, but attention to cerebral perfusion is paramount; blood pressure must be carefully monitored, and the height difference between the heart and brain accounted for.

-
Lateral Decubitus Position:
- Advantages: Provides excellent visualization, particularly of the posterior and inferior glenoid; gravity-assisted distraction of the joint; stability of the arm with traction.
- Setup: The patient is positioned on their non-operative side. The operative shoulder is positioned at the edge of the table. A beanbag or supportive bolsters are used to stabilize the torso. The non-operative arm is supported on an arm board. The operative arm is placed in a traction device, typically with 10-15 lbs of traction, abducted to 30-70 degrees and forward flexed to 15-20 degrees.
-
Key Considerations:
Careful padding of the dependent arm (axillary roll to prevent brachial plexus compression), dependent leg, and bony prominences. Avoid excessive traction to prevent neurovascular compromise.

Regardless of the position, a thorough surgical scrub, preparation, and sterile draping are performed, ensuring adequate exposure for portal placement or incision. The bony landmarks (acromion, coracoid, clavicle, scapular spine) are marked.
Detailed Surgical Approach / Technique
The surgical management of anterior glenohumeral dislocation aims to restore static and dynamic stability, primarily by addressing the anatomical lesions identified pre-operatively.
Arthroscopic Bankart Repair
This is the most common procedure for soft tissue Bankart lesions and minimal glenoid bone loss.
-
Diagnostic Arthroscopy & Portal Placement:
- A standard posterior portal (approx. 2 cm inferior and 1 cm medial to the posterior angle of the acromion) is established for initial diagnostic arthroscopy.
- Systematic evaluation of the glenohumeral joint is performed: assess the labrum, articular cartilage (glenoid and humeral head), rotator cuff, biceps tendon, and capsule. Confirm the presence of an anterior-inferior labral avulsion (Bankart lesion) and evaluate the Hill-Sachs lesion.
-
Anterior portals are established under direct visualization. Typically, an anterosuperior (rotator interval) portal and an anteroinferior (working) portal are created. The anteroinferior portal is critical for suture anchor placement and tissue manipulation.

-
Labral Mobilization and Glenoid Preparation:
- Using a shaver or radiofrequency ablator, the detached labrum is mobilized from the anterior glenoid neck. Ensure complete mobilization of the anterior capsuloligamentous complex to allow for anatomical reduction and tensioning.
-
The anterior glenoid rim and neck are decorticated using a shaver or burr to create a bleeding bed, promoting biological healing of the repaired labrum to the glenoid.

-
Suture Anchor Placement:
- Suture anchors (typically 2-5, depending on the extent of the lesion) are placed along the anterior-inferior glenoid rim, from 2 to 5 o'clock position (right shoulder) or 7 to 10 o'clock (left shoulder). The first anchor is typically placed at the 5 o'clock position (right shoulder), directly at the inferior aspect of the Bankart lesion.
-
A drill guide is used to create pilot holes, followed by anchor insertion. The anchors should be placed firmly into the bone, flush with the articular surface or slightly subchondral.

-
Sutures from each anchor are then passed through the substance of the avulsed labrum and capsule, typically in a mattress or simple fashion, using a suture passer. The goal is to capture sufficient tissue to recreate the "anterior bumper."

-
Suture Management and Knot Tying:
- Sutures are retrieved through the working portals. Each suture limb is carefully identified.
-
Knot tying is performed to re-approximate the labral-capsular complex to the prepared glenoid rim. It is crucial to achieve appropriate tension, recreating the anterior bumper without over-constraining the joint.

- After tying, the stability of the repair is assessed by manual range of motion.
Arthroscopic Remplissage (for Engaging Hill-Sachs Lesion)
If an engaging Hill-Sachs lesion is present (defined by the "off-track" concept), an arthroscopic remplissage (filling in) procedure may be performed concurrently with Bankart repair.
- Preparation: A posterior-lateral portal is established to visualize the Hill-Sachs lesion. The defect is debrided with a shaver to create a bleeding surface.
- Suture Anchor Placement: 1-2 suture anchors are placed into the Hill-Sachs defect.
-
Capsulotenodesis:
The sutures are then passed through the infraspinatus tendon and posterior capsule, effectively tenodesing these structures into the Hill-Sachs defect. This converts the intra-articular defect to an extra-articular one, preventing engagement with the anterior glenoid during abduction and external rotation.

Open Latarjet Procedure (Coracoid Transfer)
Indicated for significant glenoid bone loss (>20-25%), recurrent dislocations after failed arthroscopic repair, or in high-demand athletes with multiple risk factors. This is a bone-block procedure that provides both a bone block effect and a sling effect from the conjoined tendon.
- Incision: A deltopectoral approach is utilized through a skin incision extending from the coracoid process distally along the deltopectoral groove.
- Dissection: The cephalic vein is identified and typically retracted laterally with the deltoid. The interval between the deltoid and pectoralis major is developed.
-
Coracoid Osteotomy:
The coracoid process is exposed. The pectoralis minor, coracobrachialis, and short head of the biceps (conjoined tendon) are detached from their insertions on the coracoid process, but kept attached to the osteotomized coracoid fragment. The coracoacromial ligament is released. An osteotomy is performed at the base of the coracoid process, carefully preserving the attachment of the conjoined tendon.

- Subscapularis Split: The subscapularis muscle is identified. A split is made in the subscapularis tendon, typically along the inferior two-thirds, to gain access to the joint capsule. Alternatively, the subscapularis can be incised longitudinally and reflected.
- Capsule Incision and Glenoid Preparation: The anterior capsule is incised. The anterior-inferior glenoid neck is exposed, and any remaining detached labrum or fibrous tissue is debrided. The glenoid neck is prepared to receive the coracoid block.
-
Coracoid Transfer and Fixation:
The osteotomized coracoid fragment, with the conjoined tendon attached, is then passed through the split in the subscapularis and positioned flush against the prepared anterior-inferior glenoid rim. It is typically fixed with two cortical screws, ensuring bicortical purchase into the scapular neck. The inferior screw is typically placed first, followed by the superior screw. Careful attention is paid to ensure adequate compression and anatomical positioning.

-
Capsular Repair and Closure:
The capsule is then repaired over the transferred coracoid block. The subscapularis split is closed, and the deltopectoral interval is reapproximated. Layered closure of the subcutaneous tissue and skin is performed.

Open Bankart Repair (Capsular Shift)
This procedure is less common now but remains an option for specific cases, such as large, redundant capsules or failed arthroscopic repairs without significant bone loss. It allows for direct visualization and robust tissue repair.
- Incision and Dissection: Similar deltopectoral approach as Latarjet.
- Subscapularis Management: The subscapularis tendon can be detached laterally and reflected medially, or an interval can be made within the muscle.
- Capsular Repair and Shift: The anterior capsule is incised, typically in an inverted "T" or "L" fashion. The detached labrum is reattached to the glenoid rim with sutures. The redundant capsule is then imbricated or shifted (e.g., inferiorly based capsular shift) and sutured to the glenoid rim and humerus, effectively tightening the anterior capsule.
- Closure: Subscapularis and wound closure.
Key Anatomical Considerations During Surgery
- Axillary Nerve: Courses inferiorly and posteriorly around the surgical neck of the humerus. At risk during anchor placement in the inferior glenoid, posterior capsular dissection, and during traction or instrument manipulation.
- Musculocutaneous Nerve: Pierces the coracobrachialis muscle. At risk during coracoid osteotomy and manipulation in Latarjet procedures.
- Brachial Plexus: Generally protected but can be injured by excessive traction, especially in the lateral decubitus position.
- Vessels: Brachial artery (medially), axillary artery (anteriorly/inferiorly). Care must be taken to avoid vascular injury, especially during screw insertion in Latarjet.
- Internervous Planes: The deltopectoral interval (for open approaches) exploits the space between the deltoid (axillary nerve innervation) and pectoralis major (medial and lateral pectoral nerve innervation).
Complications & Management
Despite advancements in surgical techniques, anterior glenohumeral instability repair can be associated with various complications. Comprehensive understanding of their incidence and appropriate management is critical.
| Complication | Incidence (Approximate Range) | Management Strategy |
|
Recurrent Instability/Failure
| * Often 5-20% even after surgery. * Higher in young athletes, presence of bone loss, or primary soft tissue repair for significant bone loss. | Recurrence | 1-15% (Arthroscopic repair) | Re-evaluation of stability pathway. Consider repeat soft-tissue repair (Bankroscopic) if initial repair failed without bone loss. If bone loss or engaging Hill-Sachs, consider bone block augmentation (Latarjet) or Remplissage/bone block. For MDI, consider capsular shift. Surgical revision guided by specific etiology of failure. |
|
Neurovascular Injury
| Axillary nerve: 5-55% (acute dislocation); 0.5-2% (surgery) Musculocutaneous nerve: <1% (surgery, esp. Latarjet) Brachial artery: <0.1% |
Pre-Op/Acute:
Immediate reduction of dislocation. Post-reduction neurovascular exam.
Intra-Op:
Meticulous technique, careful portal placement, visualization of critical structures. Protect nerves with retractors. Ensure correct screw length in Latarjet.
Post-Op:
Neurological deficit: Observation, EMG/NCS for localization and prognosis. Vascular injury: Immediate surgical exploration, repair of vessel. |
|
Stiffness / Loss of ROM
| 5-15% (more common after open procedures or Latarjet) | Aggressive physical therapy, including early passive and active-assisted ROM. Consider manipulation under anesthesia or arthroscopic capsular release for recalcitrant cases. Prevention includes controlled immobilization periods and early, structured rehabilitation. |
|
Infection
| <1% |
Superficial:
Oral antibiotics, local wound care.
Deep (PJI):
Surgical debridement, irrigation, IV antibiotics. May require implant removal and staged revision. Prevention: Sterile technique, pre-operative antibiotics. |
|
Pain (Persistent)
| 5-10% | Rule out recurrent instability, hardware irritation, nerve entrapment, or progression of arthritis. Non-operative management (PT, injections) initially. Consider hardware removal, revision surgery, or pain management specialist referral. |
|
Hardware-Related Complications
| 2-5% (arthroscopic anchors); 5-10% (Latarjet screws) |
Arthroscopic Anchors:
Anchor pull-out, breakage, articular cartilage damage from proud anchors. Management: Removal if symptomatic, revision.
Latarjet Screws:
Screw breakage, loosening, neurovascular impingement, non-union of coracoid. Management: Removal of symptomatic hardware, revision fixation, nerve decompression. |
|
Glenohumeral Arthritis (Post-traumatic)
| Long-term risk, incidence varies (up to 10-20% at 10-20 years post-op) | Prevention: Meticulous technique, anatomical reduction, minimal articular damage. Management: Non-operative (PT, injections, activity modification). For severe cases, consider arthroplasty (total shoulder arthroplasty or hemiarthroplasty). |
|
Fracture (Iatrogenic)
| <1% (glenoid, humeral head, greater tuberosity) |
Intra-op:
Recognize and manage immediately; internal fixation if displaced or unstable.
Post-op:
Immobilization, protected ROM. May require delayed fixation if displaced. |
Salvage Strategies
When initial surgical management fails, a systematic approach to revision surgery is necessary. This involves:
1.
Thorough Re-evaluation:
Detailed history, physical exam, and advanced imaging (CT for bone loss, MRI for soft tissue status, particularly for HAGL lesions or failed capsular repairs).
2.
Addressing Bone Loss:
Often, failure of soft tissue repair is due to unrecognized or inadequately addressed glenoid or humeral bone loss. Revision surgery may then involve a Latarjet procedure or glenoid bone grafting, possibly combined with Remplissage if a persistent engaging Hill-Sachs lesion is present.

3.
Capsular Redundancy/Deficiency:
In cases of global laxity or persistent capsular stretch, a formal capsular shift or plication may be required.
4.
Hardware Removal:
Symptomatic or prominent hardware should be removed.
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is a structured, progressive process critical for optimizing functional recovery and preventing recurrence or stiffness. Protocols vary based on the surgical procedure (arthroscopic Bankart vs. Latarjet), quality of tissue repair, and surgeon preference. The general principles involve protecting the repair, regaining motion, and progressive strengthening.
Phase I: Protection & Early Motion (Weeks 0-6)
- Goals: Protect the surgical repair, minimize pain and swelling, initiate early, controlled motion, prevent stiffness.
-
Immobilization:
- Bankart Repair: Sling immobilization, typically for 3-6 weeks, with arm in slight internal rotation to protect the anterior repair. Removal for hygiene and supervised exercises.
- Latarjet Procedure: Sling immobilization for 3-4 weeks. Immobilization may be shorter as the bone block provides inherent stability.
-
Motion:
- Passive Range of Motion (PROM): Initiated early, often within the first week, under strict supervision. Emphasis on pendulum exercises, supine passive flexion, and external rotation to a protected limit (e.g., 0-15 degrees for Bankart, slightly more for Latarjet due to mechanical block). Avoid abduction and external rotation beyond neutral.
- Scapular Mobilization: Gentle scapular retraction and protraction exercises.
- Strengthening: Isometrics for the rotator cuff and deltoid, with the arm in the sling, without stressing the repair.
-
Patient Education:
Instructions on proper sling use, posture, precautions (no lifting, pushing, pulling, or sudden movements), and pain management.

Phase II: Intermediate Motion & Light Strengthening (Weeks 6-12)
- Goals: Restore full passive and active range of motion (AROM), initiate dynamic shoulder stability, increase strength.
- Sling Discontinuation: Gradual weaning from the sling, typically around 4-6 weeks post-op.
-
Motion:
- Continue PROM, progressing to active-assisted range of motion (AAROM) and then AROM.
- Gradually increase external rotation and abduction as tolerated, guided by surgeon protocol and tissue healing.
- Focus on multi-planar movements.
-
Strengthening:
- Initiate light isotonic strengthening for rotator cuff (internal/external rotation with resistance bands, prone horizontal abduction for teres minor), deltoid, and scapular stabilizers.
- Begin with low resistance, high repetition exercises.
- Progress to closed-chain exercises (e.g., wall push-ups).
- Proprioception: Introduction of proprioceptive exercises (e.g., rhythmic stabilization with manual resistance).
Phase III: Advanced Strengthening & Return to Activity (Weeks 12-24)
- Goals: Maximize strength, power, and endurance; achieve functional readiness for sport-specific or work-specific activities.
-
Strengthening:
- Progressive resistive exercises for all major shoulder muscle groups.
- Advanced rotator cuff strengthening, plyometrics, and eccentric training.
- Focus on core stability and kinetic chain integration.
-
Sport-Specific Training:
- For athletes, progressive return to sport-specific drills (e.g., throwing progression, overhead movements).
- Gradual increase in intensity and complexity.
-
Return to Activity:
- Return to light, non-contact activities may begin around 4-6 months, with full unrestricted contact sports or overhead activities typically deferred until 6-9 months post-op, assuming full strength, ROM, and no pain or apprehension. This timeline can be longer, especially for Latarjet.
-
Criteria for return to sport typically include: full pain-free ROM, >90% strength compared to contralateral side, no apprehension, and successful completion of a functional testing battery.


Summary of Key Literature / Guidelines
The management of anterior glenohumeral instability has evolved significantly, driven by a robust body of literature and the development of evidence-based guidelines.
Seminal Works & Concepts
- Bankart Lesion: Arthur Bankart's classic description in 1923 highlighted the essential lesion in recurrent anterior dislocation as an avulsion of the anterior labrum from the glenoid rim. His work emphasized the importance of anatomical repair.
- Latarjet Procedure: Originally described by Latarjet in 1954, this procedure gained renewed interest for its effectiveness in cases with significant glenoid bone loss. Patte and Neer further popularized the technique, emphasizing the "sling effect" of the conjoined tendon in addition to the bone block effect.
- Hill-Sachs Lesion: Described by Hill and Sachs in 1940, this posterolateral humeral head compression fracture is a critical factor in recurrent instability.
- Glenoid Track Concept: Developed by Itoi et al., this concept revolutionized understanding of the interplay between glenoid bone loss and Hill-Sachs lesions. It defines a "glenoid track" on the humeral head that contacts the anterior glenoid rim during abduction and external rotation. If the Hill-Sachs lesion is "off-track" (extends medial to the glenoid track), it can engage the glenoid, leading to recurrent instability, even after Bankart repair. This concept guides the addition of remplissage or bone block procedures.
Current Evidence and Guidelines
-
Arthroscopic vs. Open Repair:
- Numerous meta-analyses and systematic reviews have compared arthroscopic Bankart repair to open Bankart repair. Generally, open repair has historically shown lower recurrence rates, particularly in young, high-risk patients. However, arthroscopic techniques have significantly advanced, and with meticulous attention to detail, proper indications, and appropriate patient selection, recurrence rates can be comparable. Arthroscopic repair typically offers better cosmetic results and potentially faster initial recovery but may have a higher risk of recurrence in specific patient cohorts (e.g., competitive overhead athletes, those with significant bone loss).
- The "Instability Severity Index Score (ISIS)" developed by Balg and Boileau is a widely used clinical tool to predict recurrence risk and guide the choice between arthroscopic soft tissue repair and the Latarjet procedure. A score ≥3 often indicates a higher risk of recurrence after arthroscopic repair, favoring a Latarjet.
-
Management of Bone Loss:
- Glenoid Bone Loss: A critical threshold of 20-25% glenoid bone loss is widely accepted as an indication for bone augmentation (e.g., Latarjet or distal tibial allograft) rather than isolated soft tissue repair. Studies by Burkhart, Shaha, and others have highlighted the direct correlation between glenoid bone loss and increased recurrence rates following arthroscopic Bankart repair.
- Hill-Sachs Lesion: Engaging Hill-Sachs lesions, especially "off-track" lesions, require specific management. Remplissage, which involves tenodesis of the infraspinatus and posterior capsule into the defect, has shown efficacy in preventing engagement and reducing recurrence rates when performed concurrently with Bankart repair. For very large Hill-Sachs lesions, bone grafting or even humeral head allograft resurfacing may be considered, though less common.
-
Role of Latarjet:
- The Latarjet procedure has emerged as a highly effective and reliable procedure for recurrent anterior instability, particularly in cases with significant glenoid bone loss, engaging Hill-Sachs lesions, revision instability surgery, or in high-demand contact/overhead athletes with high recurrence risk factors. It provides both a mechanical bone block and a dynamic sling effect from the conjoined tendon. While effective, it has a distinct set of potential complications including musculocutaneous nerve injury, non-union of the coracoid, and hardware complications.
-
Special Populations:
- Adolescents: Recurrence rates are particularly high in adolescents after first-time dislocation, even with conservative management. Early surgical intervention is often considered in this active population.
- Older Adults: While anterior dislocations are common in older adults, the incidence of associated rotator cuff tears and greater tuberosity fractures is higher. Non-operative management for first-time dislocations may be favored if no significant soft tissue or bony lesions requiring intervention are present, due to lower functional demands and potentially higher surgical risks.
The overarching principle in current guidelines is that treatment decisions for anterior glenohumeral instability must be individualized, based on a thorough assessment of patient-specific risk factors, anatomical lesions (especially bone loss), and functional demands. The goal is to provide a durable repair that restores stability while preserving range of motion and preventing long-term complications such as arthropathy.
Clinical & Radiographic Imaging