Reverse Radial Forearm Flap: Comprehensive Review, Techniques & Complications | Part 22162
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
A 38-year-old right-hand dominant carpenter sustains a severe crush injury to his left dorsal hand, resulting in a 6x8 cm soft tissue defect with exposed extensor tendons and metacarpal bone. Local tissue options are insufficient. Preoperative assessment reveals a positive Allen's test on the left hand, confirming adequate ulnar collateral circulation. The surgeon plans a reverse radial forearm flap (RRFF) for coverage. Which of the following statements accurately describes the primary vascular supply mechanism for this flap?
Explanation
Correct Answer: B
The reverse radial forearm flap (RRFF) is an axial pattern flap based on the radial artery. Its unique characteristic is that it relies on retrograde flow through the radial artery. After the proximal radial artery is ligated and divided during harvest, the blood supply to the flap is maintained by collateral circulation from the u ulnar artery, primarily through the palmar and dorsal carpal arches around the wrist, which then perfuses the radial artery in a reverse direction. This retrograde flow then supplies the fasciocutaneous perforators within the flap.
Option A is incorrect because the flap is distally based, meaning the proximal radial artery is ligated, and flow is reversed, not antegrade through its entire course.
Option C is incorrect because while fasciocutaneous perforators are crucial, the primary vascular pedicle is the radial artery itself, which carries the main blood supply, not solely musculocutaneous perforators from a specific muscle.
Option D is incorrect as the anterior interosseous artery is not the primary arterial supply for the radial forearm flap; the radial artery is the main pedicle.
Option E is incorrect because the RRFF is an axial pattern flap, meaning it has a defined, named vascular pedicle (the radial artery), unlike a random pattern flap which relies on the less predictable subdermal plexus.
Question 2
A 55-year-old diabetic patient presents with a chronic non-healing ulcer over the dorsal aspect of his right wrist, exposing the extensor retinaculum. He has a history of peripheral vascular disease. Prior to considering a reverse radial forearm flap, the most critical preoperative assessment to perform is:
Explanation
Correct Answer: C
The most critical preoperative assessment for a reverse radial forearm flap (RRFF) is a thorough Allen's test. The entire principle of the RRFF relies on retrograde flow from the ulnar artery via the palmar and dorsal carpal arches to perfuse the radial artery after its proximal ligation. If the ulnar artery's collateral circulation is compromised (a negative Allen's test), harvesting the radial artery would risk significant ischemia to the entire hand, making it an absolute contraindication. Given the patient's history of diabetes and peripheral vascular disease, this assessment is even more paramount.
Option A is incorrect, while a neurological exam is important for overall assessment, it is not the most critical step specifically for determining the safety of radial artery harvest.
Option B is incorrect, defect measurement is essential for flap planning but does not address the absolute contraindication related to hand vascularity.
Option D is incorrect, nutritional status and HbA1c are important for overall healing, especially in a diabetic patient, but they do not supersede the immediate safety concern of hand vascularity.
Option E is incorrect, Doppler mapping of the superficial radial nerve is relevant if a sensate flap is desired, but it is not the most critical step for flap viability or hand safety.
Question 3
A 28-year-old male presents with a complex soft tissue defect on the dorsal aspect of his left hand following a motorcycle accident, exposing the extensor tendons and metacarpal heads. A reverse radial forearm flap is planned. The image below shows the intraoperative marking for the flap. Based on the principles of RRFF harvest, what is the primary reason for maintaining the distal margin of the skin paddle at least 2-3 cm proximal to the radial styloid?
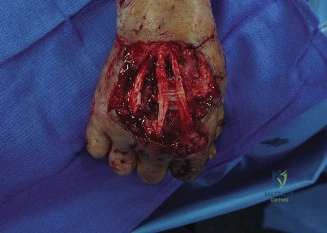
Explanation
Correct Answer: B
As stated in the case, the distal margin of the flap should be at least 2-3 cm proximal to the radial styloid. This is done primarily to preserve the distal perforators that contribute to the blood supply of the hand, ensuring adequate circulation to the hand itself after radial artery harvest. Additionally, it helps to minimize donor site morbidity and aesthetic concerns at the wrist, as the scar is less conspicuous away from the joint line.
Option A is incorrect; while donor site closure is a consideration, the primary reason for the distal margin placement is vascular preservation, not solely to facilitate primary closure (which often requires a skin graft for wider flaps anyway).
Option C is incorrect; the superficial radial nerve (SRN) does become superficial distally, but its preservation or inclusion is a separate consideration. The 2-3 cm margin is specifically for arterial perforator preservation to the hand.
Option D is incorrect; the ease of dissection of the radial artery from the flexor carpi radialis tendon is not the primary determinant for the distal margin of the skin paddle.
Option E is incorrect; while venous drainage is critical, the specific 2-3 cm margin is more directly related to preserving distal arterial perforators for hand viability rather than solely preventing venous congestion.
Question 4
A 42-year-old patient undergoes a reverse radial forearm flap for coverage of a complex wrist defect. During the postoperative period, the patient complains of persistent pain and numbness over the dorsum of the thumb and index finger of the donor hand. Which of the following is the most likely cause of this donor site complication?
Explanation
Correct Answer: C
The symptoms of persistent pain and numbness over the dorsum of the thumb and index finger of the donor hand are classic for injury or entrapment of the superficial radial nerve (SRN). The SRN provides sensory innervation to this specific area. If the SRN was not intentionally harvested with the flap for sensate reconstruction, it can be inadvertently damaged during dissection, entrapped in the donor site scar, or develop a painful neuroma, leading to these symptoms. If it was harvested for a sensate flap, this sensory deficit would be an expected, discussed outcome.
Option A is incorrect; radial artery insufficiency would manifest as signs of hand ischemia (pallor, coldness, absent pulses), not primarily as pain and numbness in the SRN distribution, especially if a positive Allen's test was confirmed pre-operatively.
Option B is incorrect; partial flap necrosis is a complication of the transferred flap at the recipient site, not a donor site complication causing pain and numbness in the donor hand.
Option D is incorrect; infection at the recipient site would cause local signs of inflammation (redness, swelling, warmth, pain) at the recipient site, not specific sensory deficits in the donor hand.
Option E is incorrect; while functional deficits can occur, they typically involve grip strength or wrist flexion and are not directly associated with specific sensory complaints in the SRN distribution.
Question 5
A surgeon is preparing to elevate a reverse radial forearm flap for a large dorsal hand defect. The patient has undergone all necessary preoperative assessments, including a positive Allen's test. Which of the following steps is most consistent with the commonly preferred technique for flap elevation?
Explanation
Correct Answer: B
The case describes two main approaches for flap elevation, with proximal-to-distal dissection commonly preferred. This approach involves making an incision along the ulnar border of the planned skin paddle, dissecting subfascially (lifting skin, subcutaneous tissue, and deep fascia), identifying and ligating the radial artery at the proximal extent of the flap, and then meticulously dissecting distally, preserving the radial artery and its venae comitantes while ligating branches not supplying the flap.
Option A is incorrect; this describes the distal-to-proximal approach, which is an alternative but not the 'commonly preferred' method as stated in the text.
Option C is incorrect; the dissection is typically performed in a subfascial plane to ensure inclusion of the fasciocutaneous perforators that supply the flap. Preserving the paratenon is important for donor site skin graft take, but the flap itself is elevated subfascially.
Option D is incorrect; the skin paddle is incised first, and the dissection proceeds to identify the vascular pedicle, not the other way around.
Option E is incorrect; ligating the ulnar artery would be catastrophic, as the ulnar artery is the source of the retrograde flow to the radial artery via collateral circulation. This would lead to hand ischemia.
Question 6
A 60-year-old patient requires reconstruction of a thumb pulp defect with a sensate reverse radial forearm flap. During the flap harvest, which nerve is specifically identified and included with the flap to provide sensation to the reconstructed area, and what is the expected trade-off at the donor site?
Explanation
Correct Answer: C
For sensate reconstruction with a reverse radial forearm flap, a segment of the superficial radial nerve (SRN) can be harvested with the flap. The SRN provides sensation to the dorsum of the hand and thumb, index, and middle fingers. The expected trade-off for harvesting the SRN is a sensory deficit in its native distribution on the dorsum of the donor hand, which must be carefully considered and discussed with the patient.
Option A is incorrect; the median nerve is a major nerve providing motor and sensory function to the hand, and its harvest would lead to severe functional impairment, not just thenar muscle loss, and it is not typically harvested with an RRFF.
Option B is incorrect; the ulnar nerve is also a major nerve providing motor and sensory function, and its harvest is not part of an RRFF for sensate reconstruction.
Option D is incorrect; the lateral antebrachial cutaneous nerve provides sensation to the radial forearm, but its harvest is not the primary method for providing sensation to a hand flap, and it does not affect elbow flexion.
Option E is incorrect; the posterior interosseous nerve is a motor nerve supplying wrist and finger extensors, and its harvest would lead to significant motor deficits, not sensory, and it is not included in an RRFF.
Question 7
A 70-year-old patient with a history of diabetes and smoking undergoes a reverse radial forearm flap for coverage of an exposed distal radius fracture plate. On the first postoperative day, the flap appears dusky, swollen, and has sluggish capillary refill, despite adequate arterial Doppler signals. What is the most likely immediate complication, and what is the appropriate initial management?
Explanation
Correct Answer: C
The clinical presentation of a dusky, swollen flap with sluggish capillary refill, despite adequate arterial Doppler signals, is highly indicative of venous congestion. This is a common complication, especially in patients with comorbidities like diabetes and smoking, which can affect microvascular health. The initial management for venous congestion includes elevating the extremity to promote venous outflow, releasing any tight sutures or dressings that might be causing external compression, and considering adjunctive measures like medicinal leeches or heparin paste to improve venous drainage.
Option A is incorrect; arterial occlusion would typically present with a pale, cold, non-blanching flap with absent arterial Doppler signals, which contradicts the presence of adequate arterial signals.
Option B is incorrect; while infection is a risk, the immediate presentation points more towards a vascular issue. Infection typically manifests later with signs of inflammation (redness, warmth, purulence).
Option D is incorrect; hematoma formation can cause swelling and compromise flap viability, but the dusky appearance and sluggish capillary refill are more specific to venous congestion. While a hematoma could contribute, venous congestion is the more direct diagnosis based on the description.
Option E is incorrect; partial flap necrosis is an outcome of prolonged vascular compromise (often venous congestion), not the immediate complication itself. The goal is to manage the congestion to prevent necrosis.
Question 8
A 25-year-old patient presents with a 4x5 cm full-thickness skin defect over the dorsal aspect of the proximal phalanx of the index finger, exposing the extensor tendon. The defect is too large for primary closure or a local flap. Considering the reconstructive ladder and the characteristics of the defect, which of the following reconstructive options would typically be considered a more complex alternative to the reverse radial forearm flap for this specific defect?
Explanation
Correct Answer: D
The reverse radial forearm flap (RRFF) occupies a crucial rung on the reconstructive ladder, balancing between local flaps and free tissue transfer. For a 4x5 cm defect on the dorsal proximal phalanx, an RRFF would be a suitable option. A Anterolateral Thigh (ALT) free flap would be considered a more complex alternative because it involves microsurgical free tissue transfer, requiring anastomosis of vessels at the recipient site. Free flaps are typically reserved for very large or complex defects involving multiple tissue types, or when regional pedicled flaps are not feasible or sufficient.
Options A and B (Split-thickness and Full-thickness skin grafts) are incorrect because they are simpler options on the reconstructive ladder, suitable for smaller, well-vascularized beds without exposed critical structures. They would not provide robust coverage for an exposed extensor tendon.
Option C (Cross-finger flap) is incorrect because while it is a regional flap, it is generally considered less complex than an RRFF and is limited in size and typically requires a two-stage procedure. It's often used for specific digital defects but might be too small or less versatile for a 4x5 cm defect exposing tendon.
Option E (V-Y advancement flap) is incorrect because it is a local flap, suitable for smaller defects with sufficient adjacent healthy tissue, and would be insufficient for a 4x5 cm defect exposing tendon.
Question 9
Following the successful harvest and transposition of a reverse radial forearm flap, the donor site defect is 5 cm wide. The surgeon plans to close the donor site. Which of the following is the most appropriate method for donor site closure in this scenario, and what critical structure must be preserved?
Explanation
Correct Answer: B
The case states that for wider flaps (typically >3-4 cm), primary closure is not feasible, and the defect is covered with a skin graft. For a 5 cm wide defect, a split-thickness skin graft is the most appropriate method. A critical aspect of successful skin graft take is a well-vascularized bed. Therefore, it is essential to preserve the paratenon of the flexor tendons, which provides the necessary vascularity for the graft to survive. Without intact paratenon, the tendons themselves would be exposed, leading to poor graft take, desiccation, and adhesion.
Option A is incorrect; primary closure is typically only feasible for narrower flaps (<3-4 cm) to avoid excessive tension. While preserving the superficial radial nerve is important to minimize donor site morbidity, it's not the primary consideration for graft take.
Option C is incorrect; while a full-thickness skin graft could be used, the primary concern for graft take is the bed, not the radial artery (which has already been harvested or preserved as the flap pedicle). The paratenon is the critical structure for graft viability.
Option D is incorrect; local flap advancement from the ulnar forearm is not a standard method for closing a large RRFF donor site, and the ulnar artery is crucial for hand perfusion, not for donor site closure.
Option E is incorrect; secondary intention healing for a 5 cm wide defect would be prolonged, lead to significant scarring and contracture, and is generally not preferred for such a large defect, especially over exposed tendons.
Question 10
A 32-year-old patient undergoes a reverse radial forearm flap for a complex hand injury. On the second postoperative day, the flap appears pale, cool to touch, and has absent capillary refill, with no audible Doppler signals over the pedicle. The patient also reports increasing pain. What is the most appropriate immediate course of action?
Explanation
Correct Answer: C
The signs described (pale, cool, absent capillary refill, no Doppler signals, increasing pain) are classic indicators of arterial occlusion or complete pedicle compromise. This is a surgical emergency requiring immediate intervention. Urgent re-exploration of the flap is mandatory to identify the cause of the vascular compromise (e.g., pedicle kinking, thrombosis, external compression) and attempt salvage through vascular revision or release of compression. Delay in re-exploration can lead to irreversible flap necrosis.
Option A is incorrect; continued observation would lead to irreversible flap loss. Elevation is helpful for venous congestion but not for arterial occlusion.
Option B is incorrect; antibiotics are for infection, which is not the primary issue here. Warm compresses might be used for vasospasm but are insufficient for complete arterial occlusion.
Option D is incorrect; medicinal leeches are used for venous congestion, not arterial occlusion. They would be ineffective and potentially harmful in this scenario.
Option E is incorrect; aggressive hand therapy is part of rehabilitation, not an immediate treatment for acute flap vascular compromise. Early mobilization could even worsen the situation if the pedicle is compromised.
Question 11
The reverse radial forearm flap (RRFF) relies on retrograde venous drainage to survive. Which of the following anatomic mechanisms primarily allows the paired venae comitantes to effectively drain the flap against the natural orientation of venous valves?
Explanation
Question 12
During preoperative evaluation for a reverse radial forearm flap, a modified Allen's test is performed. Upon release of the ulnar artery with continued radial artery compression, the hand regains its normal color in 14 seconds. What is the most appropriate management regarding the planned flap?
Explanation
Question 13
During the elevation of a reverse radial forearm flap, the dissection must proceed in the correct anatomic plane to ensure flap viability. Which of the following describes the most appropriate dissection plane for the skin paddle?
Explanation
Question 14
A surgeon is elevating a reverse radial forearm flap.
The critical septocutaneous vessels supplying this flap travel within the lateral intermuscular septum. This septum is located between which two muscles?

Explanation
Question 15
To minimize donor site morbidity and optimize the take of a full-thickness skin graft following harvest of a radial forearm flap, which of the following technical steps is most critical?
Explanation
Question 16
Two weeks after undergoing a reverse radial forearm flap with split-thickness skin grafting to the donor site, a patient presents with graft loss over the distal forearm. The flexor carpi radialis tendon is exposed and devoid of paratenon. What is the most appropriate management to prevent tendon rupture?
Explanation
Question 17
Which of the following is the most frequent long-term complication leading to patient dissatisfaction at the donor site following a radial forearm flap harvest?
Explanation
Question 18
In a reverse radial forearm flap, what is the primary physiological mechanism that permits adequate retrograde venous drainage despite the anatomical presence of venous valves?
Explanation
Question 19
During the elevation of a reverse radial forearm flap, the surgeon must be meticulous when dissecting the flap off the flexor carpi radialis (FCR) and brachioradialis tendons. What is the primary reason for this careful dissection?
Explanation
Question 20
Following the inset of a reverse radial forearm flap for a dorsal hand defect, the flap appears cyanotic with dark, rapid bleeding from pinpricks. Which of the following is the most appropriate intraoperative maneuver to salvage the flap?
Explanation
Question 21
A sensate reverse radial forearm flap is planned for a patient with a massive first web space defect. To provide protective sensation to the reconstructed area, which nerve should be included in the flap harvest for coaptation?
Explanation
Question 22
A reverse radial forearm osteocutaneous flap is being harvested to reconstruct a composite first metacarpal defect. To minimize the risk of a postoperative radius fracture, the bone harvest should not exceed what maximum percentage of the radial cross-sectional diameter?
Explanation
Question 23
To further mitigate the risk of a pathologic fracture of the radius following an osteocutaneous reverse radial forearm flap harvest, what specific technical modification should be applied to the osteotomy design?
Explanation
Question 24
A 45-year-old patient who underwent a reverse radial forearm flap 6 months ago presents with shooting pain radiating to the dorsoradial aspect of the hand when the donor site is tapped. Which nerve is most likely implicated in this complication?
Explanation
Question 25
The extended reach of the reverse radial forearm flap is determined by its pivot point. Anatomically, this pivot point relies on the anastomosis of the radial artery with which of the following structures?
Explanation
Question 26
A patient requires coverage for a dorsal hand defect. The modified Allen test is performed, and the ulnar artery refill time to the entire hand is noted to be 14 seconds. What is the most appropriate next step in management?
Explanation
Question 27
A surgeon opts to perform a reverse adipofascial radial forearm flap instead of a standard fasciocutaneous flap for a dorsal wrist defect. What is the primary advantage of this modification?
Explanation
Question 28
During the elevation of a reverse radial forearm flap, the surgeon prepares to divide the proximal radial artery. Prior to this division, what is the most critical intraoperative step to ensure flap viability?
Explanation
Question 29
A 60-year-old male smoker with peripheral vascular disease undergoes a reverse radial forearm flap. Postoperatively, he develops severe digital ischemia in the affected hand. Which underlying anatomic factor most likely precipitated this complication?
Explanation
Question 30
A patient presents with a soft tissue defect over the distal interphalangeal joint of the middle finger. A reverse radial forearm flap is considered. What limits the utility of this flap for this specific defect?

Explanation
Question 31
A 42-year-old male undergoes a reverse radial forearm flap for a dorsal hand defect. Intraoperatively, the cephalic vein is not anastomosed to a local hand vein. How does venous blood primarily drain from this distally based pedicled flap?
Explanation
Question 32
To achieve maximum distal reach for a reverse radial forearm flap without compromising its primary vascular supply, what is the most distal anatomical landmark for the flap's pivot point?
Explanation
Question 33
Venous drainage in a standard reverse radial forearm flap is primarily facilitated by which of the following mechanisms?
Explanation
Question 34
A surgeon plans to harvest a sensate reverse radial forearm flap to reconstruct a palmar hand defect. Which nerve should be co-apted to a recipient digital nerve to restore protective sensation to the flap?
Explanation
Question 35
During preoperative assessment for a reverse radial forearm flap, a patient demonstrates a capillary refill time of 18 seconds in the digits during the ulnar artery release phase of the Allen test. What is the most appropriate next step in management?
Explanation
Question 36
To minimize the most common postoperative complication at the donor site of a radial forearm fasciocutaneous flap, which technical step is critical before applying a split-thickness skin graft?
Explanation
Question 37
Intraoperatively, following the transfer of a reverse radial forearm flap to the dorsal hand, the flap appears excessively blue and engorged with a brisk, dark capillary bleed. The arterial anastomosis is patent. What is the most reliable surgical method to salvage the flap?
Explanation
Question 38
A reverse radial forearm osteocutaneous flap is planned for a patient with a first metacarpal bone and soft tissue defect. To prevent a late iatrogenic radius fracture, what is the maximum recommended cross-sectional diameter of the radius that can be safely harvested?
Explanation
Question 39
What anatomical structure primarily dictates the distal-most safe pivot point for a reverse radial forearm flap?
Explanation
Question 40
When dissecting a radial forearm flap, the vascular pedicle lies within the intermuscular septum located precisely between which two muscles?
Explanation
Question 41
During the elevation of a standard reverse radial forearm flap, the surgeon must ensure that the deep antebrachial fascia is included with the skin paddle. What is the primary anatomical rationale for this step?
Explanation
Question 42
When harvesting the reverse radial forearm flap, what is the correct handling of the proximal radial artery to ensure mobility and survival of the flap?
Explanation
Question 43
A patient requires soft tissue coverage for a dorsal hand defect. The surgeon opts against a reverse radial forearm flap to avoid sacrificing a major artery and instead chooses a posterior interosseous artery (PIA) flap. The PIA flap relies on retrograde flow from which of the following vessels?
Explanation
Question 44
Several hours after a successful reverse radial forearm flap transfer, the patient exhibits an acutely ischemic hand with absent capillary refill in the digits. The flap itself remains pink with brisk capillary refill. What is the most likely cause of this presentation?
Explanation
Question 45
A 42-year-old female presents with severe, radiating neuropathic pain on the dorsoradial aspect of her hand 6 months after undergoing a reverse radial forearm flap. Tinel's sign is strongly positive over the mid-forearm at the donor site. Which structure was most likely injured during flap harvest?
Explanation
Question 46
A patient requires a reverse radial forearm flap, but pre-operative angiography demonstrates a complete, co-dominant superficial palmar arch with a hypoplastic deep palmar arch. How does this finding affect the surgical plan?
Explanation
Question 47
A resident asks about the pathophysiology of venous congestion in a reverse radial forearm flap. What is the primary mechanism that allows retrograde venous drainage in this distally based flap despite the presence of venous valves?
Explanation
Question 48
During the elevation of a reverse radial forearm flap, the surgeon dissects deep to the deep fascia. Which of the following neurological structures is most at risk of injury and must be carefully preserved along the deep surface of the brachioradialis?
Explanation
Question 49
A 42-year-old male undergoes a reverse radial forearm flap for a first web space defect. A split-thickness skin graft is used to close the donor site. To maximize graft take and prevent tendon desiccation, the surgeon must ensure preservation of the paratenon over which of the following tendons?
Explanation
Question 50
The ultimate distal reach of a reverse radial forearm flap is determined by its pivot point. Anatomically, this pivot point is primarily dictated by the patency and location of the anastomosis between the radial artery and the:
Explanation
Question 51
A 30-year-old trauma patient requires soft tissue coverage for a dorsal hand defect. An Allen test shows a capillary refill time of 15 seconds in the hand when the radial artery is compressed and the ulnar artery is released. What is the most appropriate next step in management?
Explanation
Question 52
Postoperatively, a reverse radial forearm flap used for a dorsal hand defect develops severe venous congestion, characterized by a bluish hue and rapid capillary refill. To salvage the flap intraoperatively or during early re-exploration, what is the most effective surgical maneuver?
Explanation
Question 53
A surgeon plans to reconstruct a dorsal hand defect using a reverse radial forearm flap but wishes to minimize donor site morbidity and avoid a conspicuous contour defect or a split-thickness skin graft over the volar forearm. Which of the following flap modifications is most appropriate?
Explanation
Question 54
The blood supply to the skin paddle of a reverse radial forearm flap travels through septocutaneous perforators. During dissection, these critical perforators are located within the intermuscular septum between which two muscles?

Explanation
Question 55
A 45-year-old male undergoes a reverse radial forearm flap. Preoperative Allen test and Doppler examination were normal. Intraoperatively, immediately after dividing the proximal radial artery, the hand becomes pale and pulseless. What is the most appropriate initial management step?
Explanation
Question 56
A reverse radial forearm flap is planned to reconstruct a combined soft tissue and 3 cm bony defect of the first metacarpal. An osteocutaneous flap is designed. To prevent an iatrogenic radius fracture, what is the maximum recommended cross-sectional area of the radius that can be safely harvested with the pedicle?
Explanation
None
